MedicalResearch.com Interview with:
[caption id="attachment_55578" align="alignleft" width="150"]

Nathan B. Warren[/caption]
Nathan Warren is a Ph.D.
candidate in marketing at the University of Oregon. His research examines how people respond when social norms, such as masculinity norms, are disrupted by social change. He hopes that his research can empower people who are struggling to adapt to changing norms to live healthier, happier, and more productive lives. For more information on his research, please visit: www.nathanwarrenresearch.com
[caption id="attachment_55579" align="alignleft" width="150"]

Dr. Troy Campbell[/caption]
Dr. Troy Campbell is a behavioral scientist (PhD, Duke University), former marketing professor (University of Oregon), former art, film, and psychology scholar (UC Irvine), professional designer and researcher (Netflix Insights, Disney Imagineering, UnitedHealth) and currently chief scientist at On Your Feet. Troy believes everything can be awesome when you start with the right science and follow with the right creative process, and he hopes his professional services or public guides can help his clients make something awesome and impactful. For more information on Troy Campbell, please visit: www.troy-campbell.com
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In the United States, the average American sleeps less than the minimum seven hours of sleep per night recommended by the Center for Disease Control, and nearly half of Americans report negative consequences from insufficient sleep. This problem appears to be especially prevalent in men, who report getting significantly less sleep, on average, than women.
A cultural complication is the notion that getting less than the recommended amount of sleep signals something positive about an individual. For example, US President Donald Trump has boasted about getting less than four hours of sleep per night and regularly derogates his political opponent Joe Biden as “Sleepy Joe.”
"The Sleep-Deprived Masculinity Stereotype," a new paper in the
Journal of the Association for Consumer Research, examines a possible stereotype connecting sleep and masculinity along with its underlying mechanisms and its social implications.
Authors Nathan B. Warren and Troy H. Campbell conducted 12 experiments involving 2,564 American participants to demonstrate that a sleep-deprived masculinity stereotype exists. In one experiment, participants were asked to imagine seeing a man shopping for a bed. Then, a salesperson asked the man, “How much do you normally sleep?” The results found that the mean masculinity rating for participants in the lots of sleep condition was significantly lower than the mean masculinity rating for participants in the little sleep condition.
In another experiment, participants were asked to ascribe different attributes to a male character, assigned to either a “very masculine and manly” man or a “not very masculine and not very manly” man. Participants in the masculine condition described their character sleeping 33 minutes less sleep per night than the characters described in the not masculine condition. A final experiment showed that participants who imagined stating they sleep more than average felt significantly less masculine than participants who imagined stating they sleep less than average.
Collectively, the experiments found that men who sleep less are seen as more masculine and more positively judged by society. The same patterns were not consistently observed for perceptions of women.




 Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
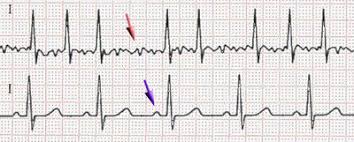
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
 Dr. Jacob[/caption]
Jesse T. Jacob, MD
School of Medicine
Director, Antibiotic Stewardship Program
Emory University, Atlanta, Georgia
MedicalResearch.com: What is the background for this study?
Response: Since coronavirus disease 2019 (COVID-19) was recognized in the United States in January 2020, the risk of infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) attributed to exposures in the health care workplace has been studied with conflicting results, and the role of job functions (such as nurse) or specific workplace activities, including care for individuals with known and unknown SARS-CoV-2 positivity, increase the risk of SARS-CoV-2 infection.
We assessed more than 24,000 healthcare providers between April and August 2020 across four large academic medical systems (Emory, Johns Hopkins, Rush University Medical Center, and University of Maryland) which collaborate in the CDC’s Prevention Epicenter Program and conduct innovative infection prevention research. Each site conducted voluntary COVID-19 antibody testing on its health care workers, as well as offered a questionnaire/survey on the employees’ occupational activities and possible exposures to individuals with COVID-19 infection both inside and outside the workplace. We also looked at three-digit residential zip-code prefixes to determine COVID-19 prevalence in communities.
Dr. Jacob[/caption]
Jesse T. Jacob, MD
School of Medicine
Director, Antibiotic Stewardship Program
Emory University, Atlanta, Georgia
MedicalResearch.com: What is the background for this study?
Response: Since coronavirus disease 2019 (COVID-19) was recognized in the United States in January 2020, the risk of infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) attributed to exposures in the health care workplace has been studied with conflicting results, and the role of job functions (such as nurse) or specific workplace activities, including care for individuals with known and unknown SARS-CoV-2 positivity, increase the risk of SARS-CoV-2 infection.
We assessed more than 24,000 healthcare providers between April and August 2020 across four large academic medical systems (Emory, Johns Hopkins, Rush University Medical Center, and University of Maryland) which collaborate in the CDC’s Prevention Epicenter Program and conduct innovative infection prevention research. Each site conducted voluntary COVID-19 antibody testing on its health care workers, as well as offered a questionnaire/survey on the employees’ occupational activities and possible exposures to individuals with COVID-19 infection both inside and outside the workplace. We also looked at three-digit residential zip-code prefixes to determine COVID-19 prevalence in communities. 

 Dr. Traverso[/caption]
Carlo Giovanni Traverso, MB, BChir, PhD
Associate Physician, Brigham and Women's Hospital
Assistant Professor,
[caption id="attachment_56823" align="alignleft" width="150"]
Dr. Traverso[/caption]
Carlo Giovanni Traverso, MB, BChir, PhD
Associate Physician, Brigham and Women's Hospital
Assistant Professor,
[caption id="attachment_56823" align="alignleft" width="150"] Dr. Chai[/caption]
Peter R. Chai, MD, MMS
Emergency Medicine Physician and Medical Toxicologist
Harvard Medical School
Brigham and Women's Hospital
Department of Medicine
Dr. Chai[/caption]
Peter R. Chai, MD, MMS
Emergency Medicine Physician and Medical Toxicologist
Harvard Medical School
Brigham and Women's Hospital
Department of Medicine
 MedicalResearch.com: What is the background for this study? What are some of the functions that Dr. Spot can facilitate?
Response: During the COVID-19 pandemic, we wanted to consider innovative methods to provide additional social distance for physicians evaluating low acuity individuals who may have COVID-19 disease in the emergency department. While other health systems had instituted processes like evaluating patients from outside of emergency department rooms or calling patients to obtain a history, we considered the use of a mobile robotic system in collaboration with Boston Dynamics to provide telemedicine triage on an agile platform that could be navigated around a busy emergency department. Dr. Spot was built with a camera system to help an operator navigate it through an emergency department into a patient room where an on-board tablet would permit face-to-face triage and assessment of individuals.
MedicalResearch.com: What is the background for this study? What are some of the functions that Dr. Spot can facilitate?
Response: During the COVID-19 pandemic, we wanted to consider innovative methods to provide additional social distance for physicians evaluating low acuity individuals who may have COVID-19 disease in the emergency department. While other health systems had instituted processes like evaluating patients from outside of emergency department rooms or calling patients to obtain a history, we considered the use of a mobile robotic system in collaboration with Boston Dynamics to provide telemedicine triage on an agile platform that could be navigated around a busy emergency department. Dr. Spot was built with a camera system to help an operator navigate it through an emergency department into a patient room where an on-board tablet would permit face-to-face triage and assessment of individuals.

 Dr. Crosbie[/caption]
Eric Crosbie, PhD, MA
Assistant Professor
School of Community Health Sciences
Ozmen Institute for Global Studies
University of Nevada Reno
MedicalResearch.com: What is the background for this study?
Response: My colleague Dr. Laura Schmidt and I established a framework for studying preemption (when a higher level of government limits the authority of lower levels to enact laws) by studying the
Dr. Crosbie[/caption]
Eric Crosbie, PhD, MA
Assistant Professor
School of Community Health Sciences
Ozmen Institute for Global Studies
University of Nevada Reno
MedicalResearch.com: What is the background for this study?
Response: My colleague Dr. Laura Schmidt and I established a framework for studying preemption (when a higher level of government limits the authority of lower levels to enact laws) by studying the 

 Dr. Swerlick[/caption]
Robert A. Swerlick, MD
Professor and Alicia Leizman Stonecipher Chair of Dermatology
Emory University School of Medicine
Atlanta, GA 30322
MedicalResearch.com: What is the background for this study?
Response: Financial incentives have the potential to drive provider behavior, even unintentionally. The aim of this study was to evaluate differences in clinic “productivity” measures that occur in outpatient dermatology encounters. Specifically, we used data from 2016-2020 at one academic dermatology practice to evaluate differences in work relative value units (wRVUs, a measure of clinical productivity) and financial reimbursement by patient race, sex, and age. 66,463 encounters were included in this study, among which 70.1% of encounters were for white patients, 59.6% were for females, and the mean age was 55.9 years old.
Dr. Swerlick[/caption]
Robert A. Swerlick, MD
Professor and Alicia Leizman Stonecipher Chair of Dermatology
Emory University School of Medicine
Atlanta, GA 30322
MedicalResearch.com: What is the background for this study?
Response: Financial incentives have the potential to drive provider behavior, even unintentionally. The aim of this study was to evaluate differences in clinic “productivity” measures that occur in outpatient dermatology encounters. Specifically, we used data from 2016-2020 at one academic dermatology practice to evaluate differences in work relative value units (wRVUs, a measure of clinical productivity) and financial reimbursement by patient race, sex, and age. 66,463 encounters were included in this study, among which 70.1% of encounters were for white patients, 59.6% were for females, and the mean age was 55.9 years old.



![MedicalResearch.com Interview with: Jeffrey D. Kent, M.D., FACG, FACP Executive Vice President, Medical Affairs and Outcomes Research Horizon MedicalResearch.com: What is the background for this study? What is the marker for reduced immunogenicity with Pegloticase? Response: Pegloticase is a recombinant, pegylated uricase that is used for treatment of chronic gout in patients who fail oral urate lowering therapy (uncontrolled gout) and has a demonstrated impact on the serum uric acid (sUA) level. As with other biologics, in some people the body’s immune system develops anti-drug antibodies and reduces the effectiveness of the biologic therapy. Recent case series and open-label trials have suggested that using an immunomodulator with pegloticase has the potential to increase the durability of response so patients can receive a full course of therapy. Researchers in the RECIPE trial sought to examine whether the co-administration of disease-modifying antirheumatic drugs (DMARDs), specifically mycophenolate mofetil, may mitigate this loss of efficacy and increase in response rates for people living with uncontrolled gout MedicalResearch.com: Are symptoms of gout improved as well as reduced infusion reactions? Response Results from this trial indicated that short-term concomitant use of mycophenolate mofetil with pegloticase was generally well tolerated. It was also associated with a statistically significant and clinically meaningful impact on the proportion of patients achieving and maintaining an sUA ≤6 mg/dL at 24 weeks. No infusion reactions were reported in the pegloticase/mycophenolate mofetil arm (0 or 22 patients) compared to 30 percent (3 of 10) of patients reporting infusion reactions in the pegloticase/placebo arm. It’s been well established that in patients receiving pegloticase with persistent urate lowering, they experience relatively rapid resolution of tophi indicating significant reductions in their urate burden. MedicalResearch.com: What are the main findings? Response: This is the first randomized controlled trial evaluating pegloticase co-prescribed with an immunomodulator compared to pegloticase with placebo. Data showed that 86.4 percent of patients (19 of 22) receiving co-therapy of pegloticase with mycophenolate mofetil achieved an sUA ≤ 6 mg/dL through Month 3, the primary study endpoint, compared to 40.0 percent of patients (4 of 10) receiving pegloticase monotherapy. After Month 3, all patients received pegloticase only and at Month 6 a sustained response was shown in 68.2 percent (15 of 22) of patients who had received pegloticase with mycophenolate mofetil versus 30.0 percent (3 of 10) of patients who received pegloticase and placebo. This data adds to the growing body of evidence on the concomitant use of pegloticase with an immunomodulator to ultimately help more patients receive a full course of therapy and improve outcomes and may help shift the treatment paradigm in uncontrolled gout. MedicalResearch.com: What should readers take away from your report? Response: While rheumatologists are familiar with and may use DMARDs for other autoimmune conditions to minimize the development of anti-drug antibodies and increase response to therapies, data shows that the use of an immunomodulating therapy in patients with uncontrolled gout can improve response rates. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: There is a consistent pattern demonstrating that the concomitant use of pegloticase and an immunomodulator can improve patient outcomes without introducing additional toxicities. As clinicians we understand the immense burden gout places on our patients. Future research should continue exploring options to maximize the benefit of effective treatments to improve patient outcomes. MedicalResearch.com: Is there anything else you would like to add? Response: Uncontrolled gout is a chronic, systemic inflammatory condition and we continue to see data linking it to many comorbid conditions. Horizon is evaluating the use of methotrexate to improve response rates for pegloticase. We are committed to exploring various immunotherapy co-treatment options to allow both patients and clinicians to address elevated sUA levels to minimize urate burden and avoid lasting damage to the body. RECIPE is an investigator-initiated trial led by Puja Khanna, M.D., M.P.H. and Kenneth Saag, M.D., M.Sc. Citation: Khanna P, Khanna D, Cutter G, Foster J, Melnick J, Jaafar S, Biggers S, Rahman A, Kuo H, Feese M, Saag K. Reducing Immunogenicity of Pegloticase (RECIPE) with Concomitant Use of Mycophenolate Mofetil in Patients with Refractory Gout—a Phase II Double Blind Randomized Controlled Trial [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/reducing-immunogenicity-of-pegloticase-recipe-with-concomitant-use-of-mycophenolate-mofetil-in-patients-with-refractory-gout-a-phase-ii-double-blind-randomized-controlled-trial/. Accessed November 12, 2020. [subscribe] Last Modified: [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/2020/11/Dr-Jeffrey-Kent.jpg)



 Dr. Sachdev[/caption]
Darpun D. Sachdev, M.D.
Case investigation and Contact tracing Branch Chief
SFDPH Covid Command Center
San Francisco Department of Public Health
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The ultimate goal of contact tracing is to rapidly identify and isolate contacts who are COVID-19 positive before they have time to transmit to others. As mentioned in the published research letter by SFDPH, through JAMA, during early shelter-in-place (from April to June 2020), our contact tracing program successfully reached greater than 80% of cases and contacts within a median timeframe of 6 days from the onset of their case’s symptoms. Approximately 10% of named contacts were newly diagnosed with COVID-19 (compared to 2% positivity during this time period). Household contacts made up approximately 80% of all identified contacts, but 90% of contacts who tested positive lived in the same household as the case. Secondary cases (contacts who were found to be newly diagnosed with COVID-19) were traced and quarantined within 6 days of the case’s symptom onset.
With that said, the 6-day time difference between symptom onset and contact notification raises concern regarding the overall effectiveness of tracing in preventing onward transmission by infected contacts. We are working with community-based organizations to scale up access to testing and culturally competent tracing and wraparound services. Currently, we have now decreased the time difference to 5 days. Moreover, given that the majority of contacts resided in the same household, transmission could have occurred presymptomatically such that by the time infected contacts were identified, they might have already transmitted the virus. Hence, why SFDPH, on May 5, 2020, implemented the recommendation of universal testing for COVID-19 contacts, regardless of symptoms.
We recommend that testing should be offered to all contacts regardless of symptoms and encourage local health departments to adopt novel ways of increasing testing access for contacts.
Dr. Sachdev[/caption]
Darpun D. Sachdev, M.D.
Case investigation and Contact tracing Branch Chief
SFDPH Covid Command Center
San Francisco Department of Public Health
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The ultimate goal of contact tracing is to rapidly identify and isolate contacts who are COVID-19 positive before they have time to transmit to others. As mentioned in the published research letter by SFDPH, through JAMA, during early shelter-in-place (from April to June 2020), our contact tracing program successfully reached greater than 80% of cases and contacts within a median timeframe of 6 days from the onset of their case’s symptoms. Approximately 10% of named contacts were newly diagnosed with COVID-19 (compared to 2% positivity during this time period). Household contacts made up approximately 80% of all identified contacts, but 90% of contacts who tested positive lived in the same household as the case. Secondary cases (contacts who were found to be newly diagnosed with COVID-19) were traced and quarantined within 6 days of the case’s symptom onset.
With that said, the 6-day time difference between symptom onset and contact notification raises concern regarding the overall effectiveness of tracing in preventing onward transmission by infected contacts. We are working with community-based organizations to scale up access to testing and culturally competent tracing and wraparound services. Currently, we have now decreased the time difference to 5 days. Moreover, given that the majority of contacts resided in the same household, transmission could have occurred presymptomatically such that by the time infected contacts were identified, they might have already transmitted the virus. Hence, why SFDPH, on May 5, 2020, implemented the recommendation of universal testing for COVID-19 contacts, regardless of symptoms.
We recommend that testing should be offered to all contacts regardless of symptoms and encourage local health departments to adopt novel ways of increasing testing access for contacts.

 Dr. Maslin[/caption]
Dr. Douglas Maslin, MPhil, MB BCHir
Dermatologist and Pharmacologist
Addenbrooke's Hospital
Cambridge, UK
MedicalResearch.com: What is the background for this study?
Response: I’d like to answer this question in three parts:
Dr. Maslin[/caption]
Dr. Douglas Maslin, MPhil, MB BCHir
Dermatologist and Pharmacologist
Addenbrooke's Hospital
Cambridge, UK
MedicalResearch.com: What is the background for this study?
Response: I’d like to answer this question in three parts:

 Mr. Olin[/caption]
Steve Olin
Chief Product Officer
Rally Health, Inc., part of the Optum business of UnitedHealth Grou
MedicalResearch.com: Can you please elaborate on Rally Health’s mission?
Mr. Olin: Our founding mission 10 years ago and still to this day is to put health in the hands of the individual. As a digital health company, we live this mission through our focus in three key areas:
1) Providing digital-first access to care by giving individuals easy-to-use digital tools and support to navigate their health care and take full advantage of their health benefits;
2) Engaging people in their daily health by creating experiences that people enjoy and that inspire them to perform healthy actions, and by giving them access to resources that help them achieve their health goals;
3) Saving people time and money by providing digital tools that help them understand health care costs and guide them to lower-cost, high-quality care options.
Mr. Olin[/caption]
Steve Olin
Chief Product Officer
Rally Health, Inc., part of the Optum business of UnitedHealth Grou
MedicalResearch.com: Can you please elaborate on Rally Health’s mission?
Mr. Olin: Our founding mission 10 years ago and still to this day is to put health in the hands of the individual. As a digital health company, we live this mission through our focus in three key areas:
1) Providing digital-first access to care by giving individuals easy-to-use digital tools and support to navigate their health care and take full advantage of their health benefits;
2) Engaging people in their daily health by creating experiences that people enjoy and that inspire them to perform healthy actions, and by giving them access to resources that help them achieve their health goals;
3) Saving people time and money by providing digital tools that help them understand health care costs and guide them to lower-cost, high-quality care options.

 Dr. Mazzeffi[/caption]
Michael Mazzeffi MD MPH MSc
Associate Professor of Anesthesiology
Division Chief Anesthesiology Critical Care Medicine
Medical Director Rapid Response Team
MedicalResearch.com: What is the background for this study?
Response: We have known for some time that COVID19 is characterized by hypercoagulability or excess blood clotting. In fact, the incidence of blood clots in the lungs (pulmonary emboli) is as high 20% and is two to three times more common in COVID19 than in severe influenza. Further, autopsies of patients who died from COVID19 have shown that endothelial cells (cells that line the blood vessels) are damaged and that "micro clots" form in multiple organs. Together, these findings strongly suggest that excess blood clotting and endothelial cell dysfunction are defining features of severe COVID19.
For several months, my colleagues and I have been interested in whether aspirin might improve outcomes in patients with severe COVID19. In prior observational research studies, aspirin was found to be protective in patients with severe lung injury. The general idea is that aspirin reduces platelet aggregates in the lung and this improves outcome. Unfortunately, in a prior randomized controlled study (LIPS-A) aspirin was not shown to reduce the incidence of acute respiratory distress syndrome. Nevertheless, COVID19 has unique features that make aspirin more likely to be effective. Mainly COVID19 is associated with hypercoagulability to a greater degree than in other viral illnesses.
Dr. Mazzeffi[/caption]
Michael Mazzeffi MD MPH MSc
Associate Professor of Anesthesiology
Division Chief Anesthesiology Critical Care Medicine
Medical Director Rapid Response Team
MedicalResearch.com: What is the background for this study?
Response: We have known for some time that COVID19 is characterized by hypercoagulability or excess blood clotting. In fact, the incidence of blood clots in the lungs (pulmonary emboli) is as high 20% and is two to three times more common in COVID19 than in severe influenza. Further, autopsies of patients who died from COVID19 have shown that endothelial cells (cells that line the blood vessels) are damaged and that "micro clots" form in multiple organs. Together, these findings strongly suggest that excess blood clotting and endothelial cell dysfunction are defining features of severe COVID19.
For several months, my colleagues and I have been interested in whether aspirin might improve outcomes in patients with severe COVID19. In prior observational research studies, aspirin was found to be protective in patients with severe lung injury. The general idea is that aspirin reduces platelet aggregates in the lung and this improves outcome. Unfortunately, in a prior randomized controlled study (LIPS-A) aspirin was not shown to reduce the incidence of acute respiratory distress syndrome. Nevertheless, COVID19 has unique features that make aspirin more likely to be effective. Mainly COVID19 is associated with hypercoagulability to a greater degree than in other viral illnesses. 
 Dr. Love you to the moon and back![/caption]
Susan Lu PhD
Gerald Lyles Rising Star Associate Professor of Management
Krannert School of Management
Purdue University
MedicalResearch.com: What is the background for this study?
Response: We started this project in 2016. Overcrowding in emergency rooms (ERs) is a common yet nagging problem. It not only is costly for hospitals but also compromises care quality and patient experience. Hence, finding effective ways to improve ER care delivery is of great importance. Meanwhile, the advancement of healthcare technologies including electronic medical records, online doctor ratings and 4G mobile network motivates us to think about the impact of telemedicine on ER operations in the near future.
Dr. Love you to the moon and back![/caption]
Susan Lu PhD
Gerald Lyles Rising Star Associate Professor of Management
Krannert School of Management
Purdue University
MedicalResearch.com: What is the background for this study?
Response: We started this project in 2016. Overcrowding in emergency rooms (ERs) is a common yet nagging problem. It not only is costly for hospitals but also compromises care quality and patient experience. Hence, finding effective ways to improve ER care delivery is of great importance. Meanwhile, the advancement of healthcare technologies including electronic medical records, online doctor ratings and 4G mobile network motivates us to think about the impact of telemedicine on ER operations in the near future. 



 Nathan B. Warren[/caption]
Nathan Warren is a Ph.D. candidate in marketing at the University of Oregon. His research examines how people respond when social norms, such as masculinity norms, are disrupted by social change. He hopes that his research can empower people who are struggling to adapt to changing norms to live healthier, happier, and more productive lives. For more information on his research, please visit: www.nathanwarrenresearch.com
[caption id="attachment_55579" align="alignleft" width="150"]
Nathan B. Warren[/caption]
Nathan Warren is a Ph.D. candidate in marketing at the University of Oregon. His research examines how people respond when social norms, such as masculinity norms, are disrupted by social change. He hopes that his research can empower people who are struggling to adapt to changing norms to live healthier, happier, and more productive lives. For more information on his research, please visit: www.nathanwarrenresearch.com
[caption id="attachment_55579" align="alignleft" width="150"] Dr. Troy Campbell[/caption]
Dr. Troy Campbell is a behavioral scientist (PhD, Duke University), former marketing professor (University of Oregon), former art, film, and psychology scholar (UC Irvine), professional designer and researcher (Netflix Insights, Disney Imagineering, UnitedHealth) and currently chief scientist at On Your Feet. Troy believes everything can be awesome when you start with the right science and follow with the right creative process, and he hopes his professional services or public guides can help his clients make something awesome and impactful. For more information on Troy Campbell, please visit: www.troy-campbell.com
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In the United States, the average American sleeps less than the minimum seven hours of sleep per night recommended by the Center for Disease Control, and nearly half of Americans report negative consequences from insufficient sleep. This problem appears to be especially prevalent in men, who report getting significantly less sleep, on average, than women.
A cultural complication is the notion that getting less than the recommended amount of sleep signals something positive about an individual. For example, US President Donald Trump has boasted about getting less than four hours of sleep per night and regularly derogates his political opponent Joe Biden as “Sleepy Joe.”
"The Sleep-Deprived Masculinity Stereotype," a new paper in the Journal of the Association for Consumer Research, examines a possible stereotype connecting sleep and masculinity along with its underlying mechanisms and its social implications.
Authors Nathan B. Warren and Troy H. Campbell conducted 12 experiments involving 2,564 American participants to demonstrate that a sleep-deprived masculinity stereotype exists. In one experiment, participants were asked to imagine seeing a man shopping for a bed. Then, a salesperson asked the man, “How much do you normally sleep?” The results found that the mean masculinity rating for participants in the lots of sleep condition was significantly lower than the mean masculinity rating for participants in the little sleep condition.
In another experiment, participants were asked to ascribe different attributes to a male character, assigned to either a “very masculine and manly” man or a “not very masculine and not very manly” man. Participants in the masculine condition described their character sleeping 33 minutes less sleep per night than the characters described in the not masculine condition. A final experiment showed that participants who imagined stating they sleep more than average felt significantly less masculine than participants who imagined stating they sleep less than average.
Collectively, the experiments found that men who sleep less are seen as more masculine and more positively judged by society. The same patterns were not consistently observed for perceptions of women.
Dr. Troy Campbell[/caption]
Dr. Troy Campbell is a behavioral scientist (PhD, Duke University), former marketing professor (University of Oregon), former art, film, and psychology scholar (UC Irvine), professional designer and researcher (Netflix Insights, Disney Imagineering, UnitedHealth) and currently chief scientist at On Your Feet. Troy believes everything can be awesome when you start with the right science and follow with the right creative process, and he hopes his professional services or public guides can help his clients make something awesome and impactful. For more information on Troy Campbell, please visit: www.troy-campbell.com
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In the United States, the average American sleeps less than the minimum seven hours of sleep per night recommended by the Center for Disease Control, and nearly half of Americans report negative consequences from insufficient sleep. This problem appears to be especially prevalent in men, who report getting significantly less sleep, on average, than women.
A cultural complication is the notion that getting less than the recommended amount of sleep signals something positive about an individual. For example, US President Donald Trump has boasted about getting less than four hours of sleep per night and regularly derogates his political opponent Joe Biden as “Sleepy Joe.”
"The Sleep-Deprived Masculinity Stereotype," a new paper in the Journal of the Association for Consumer Research, examines a possible stereotype connecting sleep and masculinity along with its underlying mechanisms and its social implications.
Authors Nathan B. Warren and Troy H. Campbell conducted 12 experiments involving 2,564 American participants to demonstrate that a sleep-deprived masculinity stereotype exists. In one experiment, participants were asked to imagine seeing a man shopping for a bed. Then, a salesperson asked the man, “How much do you normally sleep?” The results found that the mean masculinity rating for participants in the lots of sleep condition was significantly lower than the mean masculinity rating for participants in the little sleep condition.
In another experiment, participants were asked to ascribe different attributes to a male character, assigned to either a “very masculine and manly” man or a “not very masculine and not very manly” man. Participants in the masculine condition described their character sleeping 33 minutes less sleep per night than the characters described in the not masculine condition. A final experiment showed that participants who imagined stating they sleep more than average felt significantly less masculine than participants who imagined stating they sleep less than average.
Collectively, the experiments found that men who sleep less are seen as more masculine and more positively judged by society. The same patterns were not consistently observed for perceptions of women. 
 Dr. Bandi[/caption]
Priti Bandi PhD
Principal Scientist, Risk Factors Surveillance Research
American Cancer Society, Inc.
Atlanta, GA 30303
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Trends in e-cigarette prevalence and population count of users according to cigarette smoking histories are unknown. These data are needed to inform public health actions against a rapidly changing U.S. e-cigarette market.
Dr. Bandi[/caption]
Priti Bandi PhD
Principal Scientist, Risk Factors Surveillance Research
American Cancer Society, Inc.
Atlanta, GA 30303
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Trends in e-cigarette prevalence and population count of users according to cigarette smoking histories are unknown. These data are needed to inform public health actions against a rapidly changing U.S. e-cigarette market.
 Dr. Garg[/caption]
Dr. Madhur Garg, MD MBA
Clinical director, Radiation Oncology
Montefiore Health System and Professor
Departments of Otorhinolaryngology - Head & Neck Surgery - and Urology
Albert Einstein College of Medicine
MedicalResearch.com: What is the background for this study?
Response: The Bronx was hit particularly hard with Covid-19 - making up one of the highest per capita cases and deaths in the country. Montefiore Health System and Albert Einstein College of Medicine, care for a large population of ethnic minorities (non-Hispanic Black and Hispanic individuals make up 65% of our patient population).
Dr. Garg[/caption]
Dr. Madhur Garg, MD MBA
Clinical director, Radiation Oncology
Montefiore Health System and Professor
Departments of Otorhinolaryngology - Head & Neck Surgery - and Urology
Albert Einstein College of Medicine
MedicalResearch.com: What is the background for this study?
Response: The Bronx was hit particularly hard with Covid-19 - making up one of the highest per capita cases and deaths in the country. Montefiore Health System and Albert Einstein College of Medicine, care for a large population of ethnic minorities (non-Hispanic Black and Hispanic individuals make up 65% of our patient population).