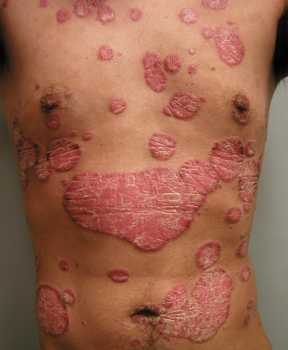
04 Dec Psoriasis: Experimental Use of Lipid Molecule to Supress Inflammation
MedicalResearch.com Interview with:

Dr. Bollag
Wendy Bollag, PhD, FAHA
Professor of Physiology
VA Research Career Scientist
Augusta University, Georgia
MedicalResearch.com: What is the background for this study?
Response: We have previously shown that the lipid (fat) phosphatidylglycerol (PG) is able to inhibit rapidly growing keratinocytes (skin cells) and promote their maturation. We also found that PG can suppress skin inflammation.
Since the common skin disease psoriasis is characterized by inflammation and excessive growth and abnormal maturation of skin cells, we believed that PG might be useful as a treatment. However, the mechanism of its anti-inflammatory effect was unknown. PG in the lung has been found to inhibit inflammation induced by microbes or their components, which work by activating the innate immune system via binding to proteins called toll-like receptors (TLRs); however, psoriasis is not considered to be an infectious disease.
We hypothesized that PG would also inhibit inflammation induced by anti-microbial peptides that activate TLRs. Anti-microbial peptides, produced normally by the skin to protect against infection, are known to be excessively up-regulated in psoriatic skin.
MedicalResearch.com: What are the main findings?
Response: We found that indeed, phosphatidylglycerol could inhibit inflammatory processes induced by representative anti-microbial peptides in skin cells and immune cells.
We also found that PG could improve skin lesions and inflammation in a mouse model of psoriasis.
MedicalResearch.com: What should readers take away from your report?
Response: Phosphatidylglycerol may be appropriate to develop for use as a treatment for psoriasis. PG, a natural lipid in cells, is also already used as an inactive ingredient in several drugs and in cosmetics, so it should have a good safety profile.
MedicalResearch.com: What recommendations do you have for future research as a result of this work?
Response: Although in our studies PG inhibited skin lesion development in a mouse model of psoriasis, it was only partially effective. This may be because the skin tends to prevent molecules above a certain size (about 600 daltons) from entering the skin (one of the skin’s key functions); PG surpasses this size cutoff (it is about 800 daltons). Permeation into the skin can be enhanced by certain lotions (vehicles) so one area of future research is to develop and test a lotion to assist PG’s entry into the skin.
In addition, PG has only been tested in one mouse model of psoriasis, and additional models should be investigated prior to testing in humans. In addition, the exact molecular mechanism by which PG inhibits the inflammatory response to anti-microbial peptides should be determined. Also unknown is the mechanism by which PG is synthesized and released in the skin and how skin PG levels are regulated normally and in disease.
Finally, it is still unclear why psoriatic individuals produce excessive amounts of anti-microbial peptides. Clearly, additional investigation is required.
Dr. Bollag is an inventor on an Augusta University for the use of phosphatidylglycerol to modulate skin function.
Citation:
Choudhary V, Uaratanawong R, Patel RR, Patel H, Bao W, Hartney B, Cohen E, Chen X, Zhong Q, Isales CM, Bollag WB.
J Invest Dermatol. 2018 Oct 31. pii: S0022-202X(18)32774-X. doi: 10.1016/j.jid.2018.10.021. [Epub ahead of print]
PMID:
30391260
[wysija_form id=”3″]
[last-modified]
The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.
Last Updated on December 4, 2018 by Marie Benz MD FAAD
