Pain Research / 27.02.2026
Sciatica Flare-Ups: 5 Mistakes People Make When They Try to Stretch It Away
Editors' note: Don't self-diagnose sciatica, nerve or back pain. See your health care provider before starting any exercise program to rule out more serious conditions.
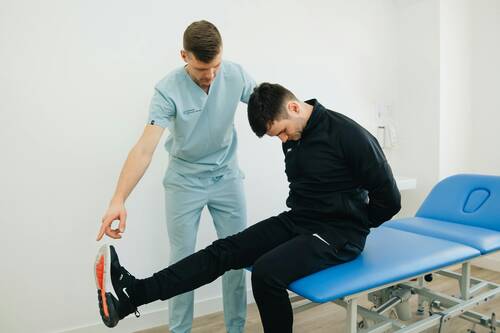
[caption id="attachment_72649" align="aligncenter" width="500"] Image by GMB Fitness on Pexels[/caption]
Sciatica pain has a sneaky way of turning a simple stretch into a full-blown flare. One minute you feel tight, the next you are guarding every step. This is because sciatica is not just a short hamstring or a stiff back. It is often an irritated nerve that hates aggressive guessing. In addition, heat, dehydration, long drives, and hard workouts can all add fuel.
Flare-ups often come from stacking triggers, not one movement. So your goal should be to reduce irritation today and build resilience tomorrow without panicking or pushing through. Here are five mistakes people make when they try to stretch it away.
Image by GMB Fitness on Pexels[/caption]
Sciatica pain has a sneaky way of turning a simple stretch into a full-blown flare. One minute you feel tight, the next you are guarding every step. This is because sciatica is not just a short hamstring or a stiff back. It is often an irritated nerve that hates aggressive guessing. In addition, heat, dehydration, long drives, and hard workouts can all add fuel.
Flare-ups often come from stacking triggers, not one movement. So your goal should be to reduce irritation today and build resilience tomorrow without panicking or pushing through. Here are five mistakes people make when they try to stretch it away.
 Image by GMB Fitness on Pexels[/caption]
Sciatica pain has a sneaky way of turning a simple stretch into a full-blown flare. One minute you feel tight, the next you are guarding every step. This is because sciatica is not just a short hamstring or a stiff back. It is often an irritated nerve that hates aggressive guessing. In addition, heat, dehydration, long drives, and hard workouts can all add fuel.
Flare-ups often come from stacking triggers, not one movement. So your goal should be to reduce irritation today and build resilience tomorrow without panicking or pushing through. Here are five mistakes people make when they try to stretch it away.
Image by GMB Fitness on Pexels[/caption]
Sciatica pain has a sneaky way of turning a simple stretch into a full-blown flare. One minute you feel tight, the next you are guarding every step. This is because sciatica is not just a short hamstring or a stiff back. It is often an irritated nerve that hates aggressive guessing. In addition, heat, dehydration, long drives, and hard workouts can all add fuel.
Flare-ups often come from stacking triggers, not one movement. So your goal should be to reduce irritation today and build resilience tomorrow without panicking or pushing through. Here are five mistakes people make when they try to stretch it away.




 Probe being applied to nerve root.
Probe being applied to nerve root.

