Author Interviews, Breast Cancer, Mammograms / 22.05.2025
Family History of Breast Cancer: Study Compares Tomosynthesis vs Mammography
MedicalResearch.com Interview with:
[caption id="attachment_68644" align="alignleft" width="200"] Dr Tong Li[/caption]
Dr Tong Li PhD | Cancer Institute NSW Early Career Fellow
Breast Cancer Clinical and Population Health Stream
The Daffodil Centre, Faculty of Medicine and Health, The University of Sydney
Moore Theological College | The University of Sydney | NSW | 2042
MedicalResearch.com: What is the background for this study?
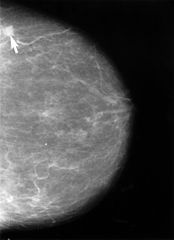
Response: Having a family history of breast cancer is one of the most common risk factors for women. About 8% to 11% of women in the U.S. report having a close relative diagnosed with breast cancer. These women often have dense breasts. Dense breast tissue can make standard digital mammography (DM, also known as 2D mammography) less effective in detecting cancer. Digital breast tomosynthesis (DBT), a 3D imaging technology, has become increasingly used in breast cancer screening because it improves the visibility of lesions and reduces unnecessary callbacks. However, until now, it has been unclear whether DBT offers the same benefits in women with a family history of breast cancer, especially across different family risk levels and breast density types.
Dr Tong Li[/caption]
Dr Tong Li PhD | Cancer Institute NSW Early Career Fellow
Breast Cancer Clinical and Population Health Stream
The Daffodil Centre, Faculty of Medicine and Health, The University of Sydney
Moore Theological College | The University of Sydney | NSW | 2042
MedicalResearch.com: What is the background for this study?
Response: Having a family history of breast cancer is one of the most common risk factors for women. About 8% to 11% of women in the U.S. report having a close relative diagnosed with breast cancer. These women often have dense breasts. Dense breast tissue can make standard digital mammography (DM, also known as 2D mammography) less effective in detecting cancer. Digital breast tomosynthesis (DBT), a 3D imaging technology, has become increasingly used in breast cancer screening because it improves the visibility of lesions and reduces unnecessary callbacks. However, until now, it has been unclear whether DBT offers the same benefits in women with a family history of breast cancer, especially across different family risk levels and breast density types.
 Dr Tong Li[/caption]
Dr Tong Li PhD | Cancer Institute NSW Early Career Fellow
Breast Cancer Clinical and Population Health Stream
The Daffodil Centre, Faculty of Medicine and Health, The University of Sydney
Moore Theological College | The University of Sydney | NSW | 2042
MedicalResearch.com: What is the background for this study?
Response: Having a family history of breast cancer is one of the most common risk factors for women. About 8% to 11% of women in the U.S. report having a close relative diagnosed with breast cancer. These women often have dense breasts. Dense breast tissue can make standard digital mammography (DM, also known as 2D mammography) less effective in detecting cancer. Digital breast tomosynthesis (DBT), a 3D imaging technology, has become increasingly used in breast cancer screening because it improves the visibility of lesions and reduces unnecessary callbacks. However, until now, it has been unclear whether DBT offers the same benefits in women with a family history of breast cancer, especially across different family risk levels and breast density types.
Dr Tong Li[/caption]
Dr Tong Li PhD | Cancer Institute NSW Early Career Fellow
Breast Cancer Clinical and Population Health Stream
The Daffodil Centre, Faculty of Medicine and Health, The University of Sydney
Moore Theological College | The University of Sydney | NSW | 2042
MedicalResearch.com: What is the background for this study?
Response: Having a family history of breast cancer is one of the most common risk factors for women. About 8% to 11% of women in the U.S. report having a close relative diagnosed with breast cancer. These women often have dense breasts. Dense breast tissue can make standard digital mammography (DM, also known as 2D mammography) less effective in detecting cancer. Digital breast tomosynthesis (DBT), a 3D imaging technology, has become increasingly used in breast cancer screening because it improves the visibility of lesions and reduces unnecessary callbacks. However, until now, it has been unclear whether DBT offers the same benefits in women with a family history of breast cancer, especially across different family risk levels and breast density types.


 Anne Cust[/caption]
Anne Cust | PhD, Professor of Cancer Epidemiology
The University of Sydney
Faculty of Medicine and Health
Sydney School of Public Health
MedicalResearch.com: What is the background for this study? Are the screeners specially trained, use full body photographs, dermoscopy etc?
Response: The Melanoma High-risk Clinic Study was developed to optimise the early detection of new melanomas in people at high risk of developing melanoma. A previous single-centre study observed fewer excisions and healthcare costs, thinner melanomas and better quality of life when surveillance of high risk patients was conducted in a melanoma dermatology clinic with a structured surveillance protocol involving 6-monthly full body examinations aided by total body photography (TBP) and sequential digital dermoscopy imaging (SDDI). The initial pilot study was performed in a single tertiary referral specialist centre using trained dermatologists who routinely used the diagnostic interventions.
Our objective was to examine longer-term sustainability and expansion of the program to multiple practices including a primary care skin cancer clinic setting. The hypothesis was that the outcomes would be similar if using the same protocol and diagnostic tools. The participating doctors were trained to follow the protocol, which included instruction on how to respond and interpret changing lesions, but not in use of dermoscopy or skin examinations, which were routinely and consistently used in all clinics prior to the study commencing. There were 593 participants assessed as very high risk of melanoma who participated in the Melanoma High-risk Clinic Study from 2012-2018. Nearly all of the participants had had a previous melanoma and had additional melanoma risk factors. 57% were male and the median age at study entry was 58 years.
Anne Cust[/caption]
Anne Cust | PhD, Professor of Cancer Epidemiology
The University of Sydney
Faculty of Medicine and Health
Sydney School of Public Health
MedicalResearch.com: What is the background for this study? Are the screeners specially trained, use full body photographs, dermoscopy etc?
Response: The Melanoma High-risk Clinic Study was developed to optimise the early detection of new melanomas in people at high risk of developing melanoma. A previous single-centre study observed fewer excisions and healthcare costs, thinner melanomas and better quality of life when surveillance of high risk patients was conducted in a melanoma dermatology clinic with a structured surveillance protocol involving 6-monthly full body examinations aided by total body photography (TBP) and sequential digital dermoscopy imaging (SDDI). The initial pilot study was performed in a single tertiary referral specialist centre using trained dermatologists who routinely used the diagnostic interventions.
Our objective was to examine longer-term sustainability and expansion of the program to multiple practices including a primary care skin cancer clinic setting. The hypothesis was that the outcomes would be similar if using the same protocol and diagnostic tools. The participating doctors were trained to follow the protocol, which included instruction on how to respond and interpret changing lesions, but not in use of dermoscopy or skin examinations, which were routinely and consistently used in all clinics prior to the study commencing. There were 593 participants assessed as very high risk of melanoma who participated in the Melanoma High-risk Clinic Study from 2012-2018. Nearly all of the participants had had a previous melanoma and had additional melanoma risk factors. 57% were male and the median age at study entry was 58 years.