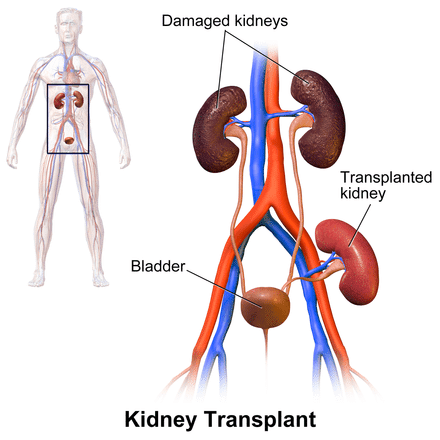
09 Nov Kidney Transplant and Living Kidney Donation: Multicomponent Program to Improve Patient Access
MedicalResearch.com Interview with:
Collective responses from study authors:
MedicalResearch.com: What is the background for this study?
- Patients with advanced chronic kidney disease (CKD) have the best chance for a longer and healthier life if they receive a kidney transplant.
- However, due to many barriers, many eligible patients today will never receive a kidney transplant.
- Advanced CKD care is provided by 26 chronic kidney disease (CKD) programs managed by a government funded provincial renal agency (the Ontario Renal Network)
- Together these 26 programs treat ~ 24,000 patients each year
- This care is provided by over 3400 nurses and 230 nephrologists
- To patients approaching the need for dialysis and those receiving dialysis
- Approximately half are transplant eligible
- ~ 600 kidney transplants done in Ontario each year across 6 transplant centres
- with approximately.30% of kidneys coming from living donors
MedicalResearch.com: Please describe the interventional protocol to address barriers to kidney transplantation from living donors:
The main components of the intervention were:
- Administrative support from a central operations group for each CKD program to establish a local quality improvement team, to drive local performance and share best practices with others,
- Transplant educational resources for healthcare staff, patients, and potential donors,
- A patient-led initiative called the Transplant Ambassador Program where over 85 kidney transplant recipients and living kidney donors shared experiences and provided emotional support,
- Quarterly program-level reports which showed the program how many of their patients were completing different steps towards receiving a transplant.
The group committed to a robust evaluation, and a pragmatic cluster-randomized trial was conducted to determine if CKD program-wide use of the multicomponent intervention is superior to usual care in helping eligible patients complete the following four key steps towards receiving a kidney transplant:
- Referral to a transplant centre for evaluation,
- Having a potential living donor contact a transplant centre for evaluation (only the first potential donor was counted for a patient with multiple potential donors),
- Added to the deceased donor waitlist, and
- Receiving a transplant from a living or deceased donor.
This trial included 20,375 patients with advanced CKD cared for by more than 3600 healthcare staff in Ontario’s 26 CKD programs, over the 4.2-year trial period. Unfortunately, the arrival of the COVID-19 pandemic 2.4 years into the trial negatively affected the implementation of the intervention as CKD programs faced staffing challenges and shifting priorities. The intervention delivery was substantially impacted for at least a year.
MedicalResearch.com: What are the main findings?
Response: Despite evidence of intervention uptake, the rate of completed steps toward receiving a kidney transplant did not significantly differ between the multicomponent intervention versus usual care groups.
MedicalResearch.com: What should readers take away from your report?
Key findings
- It is challenging to improve patient access to kidney transplantation in busy healthcare environments and there is an urgent need for effective solutions. Currently, there is limited evidence on which strategies may be effective in addressing the barriers faced by patients.
- Acknowledging the pandemic complicated intervention delivery, the team failed to show this intervention increased access to kidney transplantation and living kidney donation.
MedicalResearch.com: What recommendations do you have for future research as a results of this study?
Responses:
- The team is not giving up. They along with others are committed to addressing this complex and important problem.
- After much introspection, they believe several aspects of their approach remain sensible.
- Co-designing a solution with diverse stakeholders.
- Connecting health professionals in a community of leading practice.
- Patient and health professional education, multiple times and in multiple formats.
- A volunteer workforce of recipients and living donors, who spend thousands of hours sharing experiences and providing hope.
- Tracking key steps towards receiving a transplant, with accountabilities for system performance.
- Evaluating intervention effects robustly in a learning healthcare system.
- They are also completing a process evaluation to optimize the future approach.
MedicalResearch.com: Is there anything else you would like to add? Any disclosures?
- The trial had several strengths, including the size and scope and systematic approach to designing, implementing, and testing a province-wide multicomponent intervention.
- The intervention was designed and implemented by diverse stakeholders, including administrators, healthcare staff, patients, and nephrologists. These stakeholders created and used new and valuable transplant educational materials.
- The trial supports the goal of a learning healthcare system at Ontario’s transplant and kidney agencies, CKD programs and transplant centres. The intervention supported the development of a culture where robust evaluative processes are embedded in quality improvement initiatives.
- Unlike other jurisdictions, Ontario monitors and tracks steps early in the transplant process, including when the individual is referred for a transplant and when a potential donor first contacts the transplant centre to begin their evaluation. This allowed for the trial to evaluate and monitor the patient journey in accessing kidney transplant.
- The creation of data-sharing agreements and data collection allowed CKD programs to receive detailed performance reports on transplant-related metrics for the first time.
The extent of patient-partner involvement in the trial could pave the way for how we think about how patients support future trials. Patient partners played an integral role throughout the trial, including developing the research question and protocols, designing the intervention, participating in ethics concerns, and leading the Transplant Ambassador Program (TAP), a key component of the multicomponent intervention, which continues to provide support to thousands of patients across Ontario and due to its success, is expanding across Canada. There
Citation:
Garg AX, Yohanna S, Naylor KL, et al. Effect of a Novel Multicomponent Intervention to Improve Patient Access to Kidney Transplant and Living Kidney Donation: The EnAKT LKD Cluster Randomized Clinical Trial. JAMA Intern Med. Published online November 03, 2023. doi:10.1001/jamainternmed.2023.5802
Publications
- Partnering with Patients to Enhance Access to Kidney Transplantation and Living Kidney Donation – PubMed (nih.gov)
- Enhance Access to Kidney Transplantation and Living Kidney Donation (EnAKT LKD): Statistical Analysis Plan of a Registry-Based, Cluster-Randomized Clinical Trial – PubMed (nih.gov)
- Protocol for a Process Evaluation of the Quality Improvement Intervention to Enhance Access to Kidney Transplantation and Living Kidney Donation (EnAKT LKD) Cluster-Randomized Clinical Trial – PubMed (nih.gov)
- A Quality Improvement Intervention to Enhance Access to Kidney Transplantation and Living Kidney Donation (EnAKT LKD) in Patients With Chronic Kidney Disease: Clinical Research Protocol of a Cluster-Randomized Clinical Trial – PubMed (nih.gov)
Researcher Quotes:
Dr. Seychelle Yohanna, Provincial Medical Lead for Kidney Transplant at the Ontario Renal Network, QI Lead, Priority Panel
“While the intervention was being implemented, we saw a shift in how the staff at renal programs approached quality improvement work,” said Dr. Seychelle Yohanna. “Throughout its implementation, the trial embedded a complex learning healthcare system across all participating renal programs and transplant centres This system has resulted in an ongoing culture shift among centre staff where they are committed to learning throughout all improvement initiatives, making robust assessments of quality improvement activities the status quo rather than the exception.”
Susan Q. McKenzie, Patient Partner, Co-Founder and Chair of Transplant Ambassador Program
Patient-Focused
“As a kidney patient who experienced dialysis and received a kidney transplant 13 years ago, I know firsthand how a kidney transplant can completely transform someone’s life. But I also know the path to transplant isn’t easy for anyone, and is almost impossible without support, education and hope. This project is an important first step in a series of steps still needed to refocus kidney care in a way that prioritizes a timely kidney transplant as the first and best treatment for all who are eligible.”
TAP-Focused
“We feel incredibly fortunate, as a grassroots patient-led group, to have worked with so many amazing healthcare providers to make thousands of meaningful connections with inspiring kidney patients and potential kidney donors since this project began. Many patients have told us directly that we have made a difference in their lives. That’s what drives us to continue to grow our program and give hope to fellow patients and donors — one patient at a time.”
Dr. Peter Blake, Medical Director of Ontario Renal Network at Ontario Health and Co-Investigator in EnAKT LKD Trial
“This pragmatic cluster randomized controlled trial is wonderful example of a combined initiative between a clinical research group (ICS-KDT) and a government agency (Ontario Renal Network at Ontario Health), both off which are trying to identify how best to increase living kidney donor transplantation in the province of Ontario”
Dr. Amit Garg,
“Acknowledging the pandemic negatively affected intervention delivery, we failed to show this intervention increased access to kidney transplantation and living kidney donation. However, we are not giving up, and we and others are committed to addressing this complex and important problem. After much introspection, several aspects of our approach still seem sensible. We are currently completing a process evaluation to optimize our future approach. Some of the early data suggests more focus to the intervention, more healthcare resources, better re-orientation for personnel who turnover, and making it clear who is responsible for what may lead to future success.”
———————————–
The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition.
Some links may be sponsored. Products are not endorsed.
Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.
Last Updated on November 9, 2023 by Marie Benz
