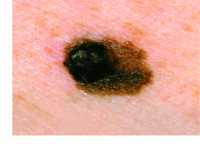
11 Aug Nanovaccine Opens New Approach to Melanoma Treatment
MedicalResearch.com Interview with:

Prof. Satchi-Fainaro
Prof. Ronit Satchi-Fainaro, PhD
Head, Cancer Research and Nanomedicine Laboratory
Department of Physiology and Pharmacology,
Sackler Faculty of Medicine,
Tel Aviv University,
Tel-Aviv 69978, Israel

Prof. Florindo
Prof. Helena Florindo, PhD
Head, BioNanoSciences – iMed.ULisboa
Faculty of Pharmacy,
University of Lisbon
Lisbon, Portugal
MedicalResearch.com: What are the main findings?
Response: The war against cancer in general, and melanoma in particular, has advanced over the years through a variety of treatment modalities, such as surgery, chemotherapy, radiation therapy and immunotherapy. The immune checkpoint inhibitors brought a breakthrough solution for advanced melanoma patients, but only a low percentage of those respond to this therapy, developing resistance and being affected by severe side effects. Despite the success of several vaccines against viral diseases, this success has not been materialized yet against cancer.
This study led by my lab at Tel Aviv University, and Helena Florindo’s lab at the University of Lisbon, describes the development of an effective nano-vaccine against melanoma, that also sensitizes the immune system to immunotherapies.
This nano-vaccine prevented melanoma, and also led to remarkable tumor inhibition and prolonged survival in mice already affected by this disease.
MedicalResearch.com: What is the background for this study?
Response: Our nano-vaccine, containing two peptides (short sequences of amino acids) expressed by melanoma cells, stimulated the immune system of the mice, and their immune cells learned to identify and attack cells containing those peptides – that is, the melanoma cells. This meant that, from now on, the immune system of the immunized mice would attack melanoma cells if and when they appear in the body.
We then examined the effectiveness of this nano-vaccine under three different conditions:
First, the nano-vaccine proved to have prophylactic effects. The nano-vaccine was injected into healthy mice, and an injection of melanoma cells followed. The mice did not get sick, meaning that the nano-vaccine prevented the disease.
Second, we combined the innovative nano-vaccine with immunotherapy to treat mice already bearing melanoma. Besides enabling the expansion of T cells, this combination did not result in a strong control of tumor growth. We found an extensive infiltration of immune suppressor cells derived from bone marrow in the tumor and we discovered that, when these cells were inhibited by a drug (ibrutinib), the full potential of our strategy was unveiled. The growth of melanoma was strongly reduced and the survival rates of these animals increased from 20%, when treated with immunotherapy and the drug, to 70% at day 65, when the nano-vaccine was combined with the immunotherapy-drug regimen. None of the non-treated melanoma mice survived after day 28.
Third, we tested our strategy in tissues taken from human patients in which the melanoma cancer cells had spread to the brain. We found that these same peptides exist in human brain tissues. This suggests that our nano-vaccine “packed” with those two peptides is likely to trigger a similar reaction in the brain, suggesting that the nano-vaccine may be used to treat brain metastases in humans as well.
MedicalResearch.com: What should readers take away from your report?
Response: Our research opens the door to a completely new approach – the vaccine approach – for effective treatment of melanoma, even in the most advanced stages of the disease.
Cancer is a very complex and multifactorial disease. The most aggressive forms do require the combination of different therapeutic strategies as an effort to increase the life expectancy of the patients. We believe that vaccination will play an important role in cancer therapies in the future, particularly in modulating the patients’ own immune system, turning it into its functional state. This nano-vaccine does not target directly the tumor cells, but rather uses our own immune system to achieve the selective destruction of cancer cells. This is important for cancer patients who suffer from severe side effects caused by anticancer agents in normal tissues and organs, due to the lack of tumor selectivity. These not only limit patient quality of life, but also often prevent treatment continuation.
We expect that our nano-vaccine will also improve the outcomes and safety of treatments already in clinical use, but that heavily limit the lives of patients affected by such aggressive diseases.
MedicalResearch.com: What recommendations do you have for future research as a result of this work?
Response: The next step will be to show that we can control the growth of metastasis to prolong overall survival. We have already data that shows that our platform may also be suitable for other types of cancer, namely triple negative breast cancer, colorectal cancer and pancreatic cancer. Therefore, our work is a solid foundation for the development of other cancer nano-vaccines. Nevertheless, it may take at least 5 to 10 years before a product could reach the market, if all the clinical trials are successful.
MedicalResearch.com: Is there anything else you would like to add?
Response: We want to acknowledge the fantastic work done by the first authors of this study- João Conniot and Anna Scomparin- and all the co-authors of this paper. We would like to thank the support received from EuroNanoMed-II, the Israeli Health Ministry, the Portuguese Foundation for Science and Technology (FCT), the Israel Science Foundation (ISF), the European Research Council (ERC), the Saban Family Foundation – Melanoma Research Alliance (MRA) Team Science Award, and the Israel Cancer Research Fund (ICRF).
Citation:
João Conniot, Anna Scomparin, Carina Peres, Eilam Yeini, Sabina Pozzi, Ana I. Matos, Ron Kleiner, Liane I. F. Moura, Eva Zupančič, Ana S. Viana, Hila Doron, Pedro M. P. Gois, Neta Erez, Steffen Jung, Ronit Satchi-Fainaro, Helena F. Florindo. Immunization with mannosylated nanovaccines and inhibition of the immune-suppressing microenvironment sensitizes melanoma to immune checkpoint modulators. Nature Nanotechnology, 2019; DOI: 10.1038/s41565-019-0512-0
[wysija_form id=”3″]
[last-modified]
The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.
Last Updated on August 11, 2019 by Marie Benz MD FAAD
