27 Feb Decision Aids Can Help Heart Failure Patients Determine If They Want an LVAD
MedicalResearch.com Interview with:
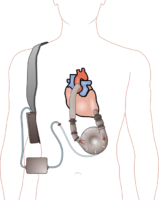
A left ventricular assist device (LVAD) pumping blood from the left ventricle to the aorta, connected to an externally worn control unit and battery pack.
Wikipedia image
Larry A. Allen, MD, MHS
Associate Professor, Medicine
Associate Head for Clinical Affairs, Cardiology
Medical Director, Advanced Heart Failure
Aurora, CO 80045
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Deciding whether or not to get a left ventricular assist device (LVAD) is one of the most challenging medical decisions created by modern medicine.
LVADs improve overall survival but also come with serious risks and lifestyle changes. Particularly for older patients with multiple medical problems, this is a complex choice.
Our research group at the University of Colorado spent years systematically developing unbiased pamphlet and video decision aids for patients and caregivers. We also developed a clinician-directed decision support training for LVAD program staff. The DECIDE-LVAD trial studied the implementation and effectiveness of this decision support intervention with patients and their caregivers in 6 hospitals in the U.S. When compared to previously used education materials, the decision aids appeared to improve patients’ decision quality and lowered the total number of patients getting LVADs.
MedicalResearch.com: What should readers take away from your report?
Response: The results of the DECIDE-LVAD trial show that implementation of formal unbiased decision aids for LVADs can help patients dying from heart failure improve the quality of decision making, and it may change the rate at which patients decide to proceed with such high-risk, high-reward treatment. This suggests that institutional culture and processes can influence medical decisions in life-threatening illness. Additionally, with the rate of 94.7% of patients in the intervention receiving the decision aids from clinical staff, this study shows that use of decision support tools can successfully occur within this medical setting.
MedicalResearch.com: What recommendations do you have for future research as a result of this work?
Response: We are now working to broadly implement the decision aids in hospitals across the world.
Additionally, further research on messaging in this setting is needed. As opposed to many decision support studies, the DECIDE-LVAD trial found no difference in decisional conflict between control and intervention patients at follow-up, which we predicted ahead of time. Nudging patients with life-threatening illness to address their fear and overcome denial—rather than providing them with false reassurances (“don’t worry, everything will be fine”)—may increase feelings of conflict, anxiety, and regret in the short term. However, according to our results, it may also improve the quality of decision making. Further research into this may be beneficial for learning how we present information to patients in these end-of-life decision making scenarios.
Given the importance of widespread adoption of shared decision making for all kinds of medical issues, practical studies such as this one are needed to address the challenges of using patient decision aids in routine practice.
MedicalResearch.com: Is there anything else you would like to add?
Response: This trial was supported through a Patient Centered Outcomes Research Institute Program Award (CDR-1310-06998). I have done consulting work for Abbott, ACI clinical, Amgen, Boston Scientific, Janssen, and Novartis.
Citations:
[wysija_form id=”3″]
The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.
Last Updated on February 27, 2018 by Marie Benz MD FAAD
