Author Interviews, End of Life Care, Hearing Loss / 09.07.2020
Dying Unconscious Patients May Still Be Able to Hear
MedicalResearch.com Interview with:
[caption id="attachment_54792" align="alignleft" width="128"] Dr. Blundon[/caption]
Elizabeth Blundon PhD
Department of Psychology
University of British Columbia – Vancouver
MedicalResearch.com: What is the background for this study?
Response: Many healthcare workers have noticed that dying patients appear to be comforted by the words of their loved ones, even when patients appear to be unconscious and are no longer able to communicate. There is a persistent belief, therefore, that hearing may persist into the last hours of someone's life. Our study attempts to detect evidence of hearing among a small group of unresponsive hospice patients at the end of life.
To do this, we compared the brain activity of young, healthy control participants, with the brain activity of hospice patients, both when the patients were awake and responsive, and again when they became unresponsive. The brain activity we measured was in response to a complex series of tone-patterns, where participants were asked to identify by pressing a button (control participants) or by counting (hospice patients) every time they heard a tone-pattern that was different from the rest of the series.
Dr. Blundon[/caption]
Elizabeth Blundon PhD
Department of Psychology
University of British Columbia – Vancouver
MedicalResearch.com: What is the background for this study?
Response: Many healthcare workers have noticed that dying patients appear to be comforted by the words of their loved ones, even when patients appear to be unconscious and are no longer able to communicate. There is a persistent belief, therefore, that hearing may persist into the last hours of someone's life. Our study attempts to detect evidence of hearing among a small group of unresponsive hospice patients at the end of life.
To do this, we compared the brain activity of young, healthy control participants, with the brain activity of hospice patients, both when the patients were awake and responsive, and again when they became unresponsive. The brain activity we measured was in response to a complex series of tone-patterns, where participants were asked to identify by pressing a button (control participants) or by counting (hospice patients) every time they heard a tone-pattern that was different from the rest of the series.
 Dr. Blundon[/caption]
Elizabeth Blundon PhD
Department of Psychology
University of British Columbia – Vancouver
MedicalResearch.com: What is the background for this study?
Response: Many healthcare workers have noticed that dying patients appear to be comforted by the words of their loved ones, even when patients appear to be unconscious and are no longer able to communicate. There is a persistent belief, therefore, that hearing may persist into the last hours of someone's life. Our study attempts to detect evidence of hearing among a small group of unresponsive hospice patients at the end of life.
To do this, we compared the brain activity of young, healthy control participants, with the brain activity of hospice patients, both when the patients were awake and responsive, and again when they became unresponsive. The brain activity we measured was in response to a complex series of tone-patterns, where participants were asked to identify by pressing a button (control participants) or by counting (hospice patients) every time they heard a tone-pattern that was different from the rest of the series.
Dr. Blundon[/caption]
Elizabeth Blundon PhD
Department of Psychology
University of British Columbia – Vancouver
MedicalResearch.com: What is the background for this study?
Response: Many healthcare workers have noticed that dying patients appear to be comforted by the words of their loved ones, even when patients appear to be unconscious and are no longer able to communicate. There is a persistent belief, therefore, that hearing may persist into the last hours of someone's life. Our study attempts to detect evidence of hearing among a small group of unresponsive hospice patients at the end of life.
To do this, we compared the brain activity of young, healthy control participants, with the brain activity of hospice patients, both when the patients were awake and responsive, and again when they became unresponsive. The brain activity we measured was in response to a complex series of tone-patterns, where participants were asked to identify by pressing a button (control participants) or by counting (hospice patients) every time they heard a tone-pattern that was different from the rest of the series. 















 Dr. Jill Cameron[/caption]
Jill Cameron, PhD
Canadian Institutes of Health Research New Investigator
Associate Professor,
Department of Occupational Science and Occupational Therapy
Rehabilitation Sciences Institute
Faculty of Medicine,
University of Toronto
MedicalResearch.com: What is the background for this study? What are the main findings?
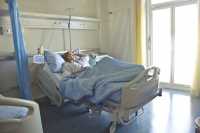
Dr. Cameron: In the world of critical illness, a lot of research has focused on helping people to survive – and now that more people are surviving, we need to ask ourselves, what does quality of life and wellbeing look like afterwards for both patients and caregivers? The aim of our research was to identify factors associated with family caregiver health and wellbeing during the first year after patients were discharged from the Intensive Care Unit. We examined factors related to the patient and their functional wellbeing, the caregiving situation including the impact it has on caregivers everyday lives, and caregiver including their sense of control over their lives and available social support. We used Pearlin’s Caregiving Stress Process model to guide this research.
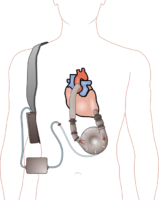
From 2007-2014, caregivers of patients who received seven or more days of mechanical ventilation in an ICU across 10 Canadian university-affiliated hospitals were given self-administered questionnaires to assess caregiver and patient characteristics, caregiver depression symptoms, psychological wellbeing, and health-related quality of life. Assessments occurred seven days and three, six and 12-months after ICU discharge.
The study found that most caregivers reported high levels of depression symptoms, which commonly persisted up to one year and did not improve in some. Caregiver sense of control, impact on caregivers’ everyday lives, and social support had the largest relationships with the outcomes. Caregivers’ experienced better health outcomes when they were older, caring for a spouse, had higher income, better social support, sense of control, and caregiving had less of a negative impact on their everyday lives. No patient characteristics or indicators of illness severity were associated with caregiver outcomes.
Poor caregiver outcomes may compromise patients’ rehabilitation potential and sustainability of home care. Identifying risk factors for caregiver distress is an important first step to prevent more suffering and allow ICU survivors and caregivers to regain active and fulfilling lives.
Dr. Jill Cameron[/caption]
Jill Cameron, PhD
Canadian Institutes of Health Research New Investigator
Associate Professor,
Department of Occupational Science and Occupational Therapy
Rehabilitation Sciences Institute
Faculty of Medicine,
University of Toronto
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Cameron: In the world of critical illness, a lot of research has focused on helping people to survive – and now that more people are surviving, we need to ask ourselves, what does quality of life and wellbeing look like afterwards for both patients and caregivers? The aim of our research was to identify factors associated with family caregiver health and wellbeing during the first year after patients were discharged from the Intensive Care Unit. We examined factors related to the patient and their functional wellbeing, the caregiving situation including the impact it has on caregivers everyday lives, and caregiver including their sense of control over their lives and available social support. We used Pearlin’s Caregiving Stress Process model to guide this research.
From 2007-2014, caregivers of patients who received seven or more days of mechanical ventilation in an ICU across 10 Canadian university-affiliated hospitals were given self-administered questionnaires to assess caregiver and patient characteristics, caregiver depression symptoms, psychological wellbeing, and health-related quality of life. Assessments occurred seven days and three, six and 12-months after ICU discharge.
The study found that most caregivers reported high levels of depression symptoms, which commonly persisted up to one year and did not improve in some. Caregiver sense of control, impact on caregivers’ everyday lives, and social support had the largest relationships with the outcomes. Caregivers’ experienced better health outcomes when they were older, caring for a spouse, had higher income, better social support, sense of control, and caregiving had less of a negative impact on their everyday lives. No patient characteristics or indicators of illness severity were associated with caregiver outcomes.
Poor caregiver outcomes may compromise patients’ rehabilitation potential and sustainability of home care. Identifying risk factors for caregiver distress is an important first step to prevent more suffering and allow ICU survivors and caregivers to regain active and fulfilling lives.


 Dr. Odejide[/caption]
MedicalResearch.com Interview with:
Oreofe O. Odejide, MD
Instructor in Medicine, Harvard Medical School
Dana-Farber Cancer Institute
Medical Research: What is the background for this study? What are the main findings?
Dr. Odejide: The care that patients with hematologic cancers receive near the end of life is distinct from patients with solid tumors. For instance, previous research has shown that patients with blood cancers are more likely to receive intensive care at the end of life such as chemotherapy within 14 days of death, intensive care unit admission within 30 days of death, and they are less likely to enroll in hospice. My colleagues and I hypothesized that timing of discussions regarding end-of-life preferences with patients may contribute to these findings, and we wanted to examine hematologic oncologists’ perspectives regarding end-of-life discussions with this patient population.
We conducted a survey of a national sample of hematologic oncologists obtained from the publicly available clinical directory of the American Society of Hematology. We received responses from 349 hematologic oncologists, giving us a response rate of 57.3%. In our survey, we asked hematologic oncologists about the typical timing of EOL discussions in general, and also about the timing of the first discussion regarding resuscitation status, hospice care, and preferred site of death for patients. Three main findings emerged:
Dr. Odejide[/caption]
MedicalResearch.com Interview with:
Oreofe O. Odejide, MD
Instructor in Medicine, Harvard Medical School
Dana-Farber Cancer Institute
Medical Research: What is the background for this study? What are the main findings?
Dr. Odejide: The care that patients with hematologic cancers receive near the end of life is distinct from patients with solid tumors. For instance, previous research has shown that patients with blood cancers are more likely to receive intensive care at the end of life such as chemotherapy within 14 days of death, intensive care unit admission within 30 days of death, and they are less likely to enroll in hospice. My colleagues and I hypothesized that timing of discussions regarding end-of-life preferences with patients may contribute to these findings, and we wanted to examine hematologic oncologists’ perspectives regarding end-of-life discussions with this patient population.
We conducted a survey of a national sample of hematologic oncologists obtained from the publicly available clinical directory of the American Society of Hematology. We received responses from 349 hematologic oncologists, giving us a response rate of 57.3%. In our survey, we asked hematologic oncologists about the typical timing of EOL discussions in general, and also about the timing of the first discussion regarding resuscitation status, hospice care, and preferred site of death for patients. Three main findings emerged:




