Fertility, OBGYNE / 29.04.2026
IVF and Emotional Wellbeing: A Couple’s Guide with Millennium IVF Clinic
[caption id="attachment_73525" align="aligncenter" width="333"] Image source[/caption]
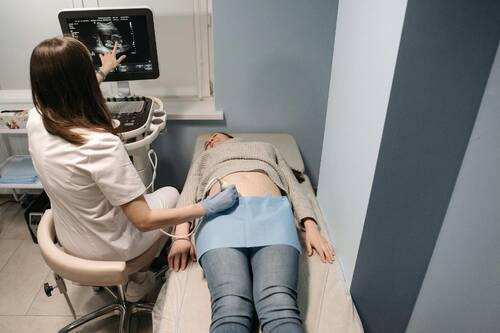
Infertility and IVF treatment can bring a whirlwind of emotions and challenges for couples. As you progress through IVF, it's common to swing between hope, excitement, and moments of worry. The emotional ups and downs are real, and coping well often means finding practical ways to support both your mental and physical health along the way.
Women and men might feel the strain differently. The uncertainty, the persistence needed for multiple treatment cycles, the financial pressure, and the way all of this can affect your relationship—it's a lot to juggle. Yet, it's a journey rooted in hope.
That's why so many turn to clinics where compassionate professionals understand the process. Millennium IVF in Thailand offers experienced infertility support, known for its genuine care that extends beyond just the latest medical treatments; they prioritise emotional wellbeing, too. The team is on hand for every phase, bringing both expertise and encouragement. At Millennium IVF Clinic, looking after how you feel is just as important as the clinical care, so you don't have to face it all alone.
Image source[/caption]
Infertility and IVF treatment can bring a whirlwind of emotions and challenges for couples. As you progress through IVF, it's common to swing between hope, excitement, and moments of worry. The emotional ups and downs are real, and coping well often means finding practical ways to support both your mental and physical health along the way.
Women and men might feel the strain differently. The uncertainty, the persistence needed for multiple treatment cycles, the financial pressure, and the way all of this can affect your relationship—it's a lot to juggle. Yet, it's a journey rooted in hope.
That's why so many turn to clinics where compassionate professionals understand the process. Millennium IVF in Thailand offers experienced infertility support, known for its genuine care that extends beyond just the latest medical treatments; they prioritise emotional wellbeing, too. The team is on hand for every phase, bringing both expertise and encouragement. At Millennium IVF Clinic, looking after how you feel is just as important as the clinical care, so you don't have to face it all alone.
 Image source[/caption]
Infertility and IVF treatment can bring a whirlwind of emotions and challenges for couples. As you progress through IVF, it's common to swing between hope, excitement, and moments of worry. The emotional ups and downs are real, and coping well often means finding practical ways to support both your mental and physical health along the way.
Women and men might feel the strain differently. The uncertainty, the persistence needed for multiple treatment cycles, the financial pressure, and the way all of this can affect your relationship—it's a lot to juggle. Yet, it's a journey rooted in hope.
That's why so many turn to clinics where compassionate professionals understand the process. Millennium IVF in Thailand offers experienced infertility support, known for its genuine care that extends beyond just the latest medical treatments; they prioritise emotional wellbeing, too. The team is on hand for every phase, bringing both expertise and encouragement. At Millennium IVF Clinic, looking after how you feel is just as important as the clinical care, so you don't have to face it all alone.
Image source[/caption]
Infertility and IVF treatment can bring a whirlwind of emotions and challenges for couples. As you progress through IVF, it's common to swing between hope, excitement, and moments of worry. The emotional ups and downs are real, and coping well often means finding practical ways to support both your mental and physical health along the way.
Women and men might feel the strain differently. The uncertainty, the persistence needed for multiple treatment cycles, the financial pressure, and the way all of this can affect your relationship—it's a lot to juggle. Yet, it's a journey rooted in hope.
That's why so many turn to clinics where compassionate professionals understand the process. Millennium IVF in Thailand offers experienced infertility support, known for its genuine care that extends beyond just the latest medical treatments; they prioritise emotional wellbeing, too. The team is on hand for every phase, bringing both expertise and encouragement. At Millennium IVF Clinic, looking after how you feel is just as important as the clinical care, so you don't have to face it all alone.






 Dr. Kaufman[/caption]
Gregory Kaufman, M.D.
Senior Vice President
Global Clinical and Medical Affairs
Specialty at Lupin
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by trichomoniasis? How common is this infection?
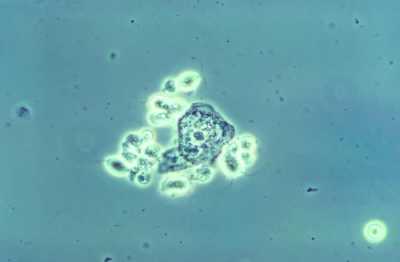
Response: The Phase 3 trial evaluated the effectiveness and safety of a single oral dose of Solosec® (secnidazole) 2g oral granules for the treatment of trichomoniasis in adult women. Top-line results were positive and showed that Solosec was generally well-tolerated.
Trichomoniasis is the most common non-viral sexually transmitted infection (STI) in the U.S., and is caused by a protozoan parasite called Trichomonas vaginalis.
Dr. Kaufman[/caption]
Gregory Kaufman, M.D.
Senior Vice President
Global Clinical and Medical Affairs
Specialty at Lupin
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by trichomoniasis? How common is this infection?
Response: The Phase 3 trial evaluated the effectiveness and safety of a single oral dose of Solosec® (secnidazole) 2g oral granules for the treatment of trichomoniasis in adult women. Top-line results were positive and showed that Solosec was generally well-tolerated.
Trichomoniasis is the most common non-viral sexually transmitted infection (STI) in the U.S., and is caused by a protozoan parasite called Trichomonas vaginalis.



