MedicalResearch.com Interview with:
Justine M. Naylor, PhD
Braeside Hospital, HammondCare, Australia
South West Sydney Clinical School, University of New South Wales, Liverpool Hospital
South West Sydney Local Health District, Liverpool 2170, NSW, Australia
MedicalResearch.com: What is the background for this study?
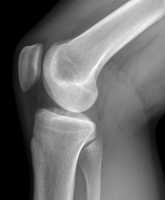
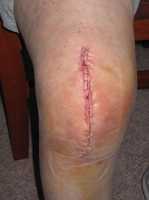
Response: Total knee arthroplasty (replacement) for end-stage arthritis is a very successful procedure for relieving the associated pain and functional impairments. Formalized rehabilitation following the surgery is also considered an essential adjunct to optimise recovery. World-wide, the volume of knee arthroplasty surgeries is increasing each year. In the US, for example, the prevalence of this surgery increased 11-fold from 1980 to 2010. The costs of the procedures (including the acute and rehabilitation costs) are also increasing. Because of these trends, there is concern for the future sustainability of these procedures. Research devoted to identifying the most cost-effective strategies in this field is required.
Our group conducted a randomized trial comparing 10-days of inpatient rehabilitation to a simple, clinician-monitored home program in people who underwent total knee arthroplasty for end-stage osteoarthritis. Inpatient rehabilitation in a rehabilitation facility is commonly provided after knee arthroplasty in various countries including Australia, the US and Switzerland, and is comparatively expensive. In particular, it is a commonly available option for people with private healthcare insurance. Essentially, we wanted to compare 2 extremes – a resource-intensive program to one with far less resource requirements. Because patients who experience complications immediately after surgery may require
inpatient rehabilitation to aid their recovery, we only included patients who did not experience a significant complication while in hospital, thus, were otherwise deemed able to be discharged directly home.

 Dr. Cavanaugh[/caption]
Alyson Cavanaugh, PT, PhD
Joint Doctoral Program in Epidemiology
University of California, San Diego/ San Diego State University
MedicalResearch.com: What is the background for this study?
Response: More than 700,000 total knee replacements are performed annually in the United States, but there is a racial disparity in outcomes after the surgery. If the knee replacement procedure is considered a highly effective treatment, why don't black women present with the same outcomes as whites?
Physical function when going into surgery has a large impact on the potential functional outcomes after surgery. Our hypothesis was that black women were presenting to surgery with poorer physical function, which was contributing to poorer functional outcomes after surgery.
Dr. Cavanaugh[/caption]
Alyson Cavanaugh, PT, PhD
Joint Doctoral Program in Epidemiology
University of California, San Diego/ San Diego State University
MedicalResearch.com: What is the background for this study?
Response: More than 700,000 total knee replacements are performed annually in the United States, but there is a racial disparity in outcomes after the surgery. If the knee replacement procedure is considered a highly effective treatment, why don't black women present with the same outcomes as whites?
Physical function when going into surgery has a large impact on the potential functional outcomes after surgery. Our hypothesis was that black women were presenting to surgery with poorer physical function, which was contributing to poorer functional outcomes after surgery.


