15 Oct MRI Detects Brain Structure Linked to Increased Weight Gain in Children
MedicalResearch.com Interview with:
Kristina M. Rapuano PhD, Postdoctoral Research Fellow
BJ Casey, PhD, Professor of Psychology at Yale University
Richard Watts PhD Technical Consultant
Department of Psychology
Yale University, New Haven, CT
MedicalResearch.com: What is the background for this study?
Response: Around 35% of children and adolescents in the US are overweight or obese, dramatically increasing their likelihood of obesity as adults and the associated health risks. In our paper we use a novel MRI technique to investigate links between obesity and neurobiology in a large group of typically developing 9-10 year-olds. The data were acquired as part of the NIH-funded Adolescent Brain Cognitive DevelopmentSM (ABCD) study, which enrolled more than 11,000 children from across the US.

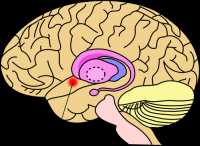
Approximate location of the nucleus accumbens in the brain
We looked specifically at a reward-related region of the brain called the nucleus accumbens. Previous human studies have shown that healthy weight and obese children display different responses to food cues, for example adverts for unhealthy foods, in this region. Animal studies have also found that a high saturated fat (unhealthy) diet induces inflammation in the nucleus accumbens, and changes in behavior including sucrose-seeking. We wanted to investigate if we could use advanced MRI techniques to provide evidence of a similar effect in humans.
MedicalResearch.com: What are the main findings?
Response: We found a very strong association between the microscopic structure of the nucleus accumbens (assessed with MRI) and waist size or BMI in 9-10 year-olds. Importantly, when we looked at the same children a year later we found that this MRI measure of microstructure was predictive of future weight gain
MedicalResearch.com: What should readers take away from your report?
Response: Our study shows neurobiological differences that may make some individuals more susceptible to weight gain than others. We hypothesize that this could be part of a vicious cycle in which poor diet causes brain changes that impact behavior and increase the likelihood of future weight gain. If we can understand this mechanism, we may be able to identify individuals at high risk of obesity early in life and develop interventions to reduce this risk.
MedicalResearch.com: What recommendations do you have for future research as a result of this work?
Response: This study only looked at weight gain over a period of a year. As a longitudinal study, we will also be able to look at both physiological and brain changes over the next 10 years. Changes related to puberty will be particularly interesting. Additionally, we will be able to combine imaging with genetics, environment, diet, and physical activity data. As we follow these children, we may be able to determine imaging biomarkers of future risk of obesity and other factors that may be protective.
MedicalResearch.com: Is there anything else you would like to add?
Response: Data used in the preparation of this article were obtained from the ABCD study® (https://abcdstudy.org), held in the National Institute of Mental Health (NIMH) Data Archive (NDA). The ABCD Study is supported by the NIH and additional federal partners.
Citation:
Kristina M. Rapuano, Jennifer S. Laurent, Donald J. Hagler, Sean N. Hatton, Wesley K. Thompson, Terry L. Jernigan, Anders M. Dale, B. J. Casey, Richard Watts. Nucleus accumbens cytoarchitecture predicts weight gain in children. Proceedings of the National Academy of Sciences, 2020; 202007918 DOI: 10.1073/pnas.2007918117
[subscribe]
Last Modified: [last-modified]
The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.
Last Updated on October 15, 2020 by Marie Benz MD FAAD
