Breast Cancer, Cancer Research, JAMA, Weight Research / 13.05.2026
GLP-1 Medications Associated With Improved Survival and Lower Recurrence Risk in Breast Cancer Patients With Obesity or Diabetes in Observational Study
MedicalResearch.com Interview with:
[caption id="attachment_73639" align="alignleft" width="125"] Dr. Fuemmeler[/caption]
Bernard F. Fuemmeler, PhD, MPH
Professor and Gordon D. Ginder, MD Chair in Cancer Research
Associate Director of Population Science, Massey Comprehensive Cancer Center
Director of Research, Family Medicine and Population Health
[caption id="attachment_73640" align="alignleft" width="125"]
Dr. Fuemmeler[/caption]
Bernard F. Fuemmeler, PhD, MPH
Professor and Gordon D. Ginder, MD Chair in Cancer Research
Associate Director of Population Science, Massey Comprehensive Cancer Center
Director of Research, Family Medicine and Population Health
[caption id="attachment_73640" align="alignleft" width="125"] Dr. Tatum[/caption]
Kristina L. Tatum, PsyD, MS
Instructor
Department of Social and Behavioral Sciences
School of Public Health
A large population-based analysis of more than 841,000 breast cancer patients across the United States examines whether GLP-1 receptor agonist use is associated with improved survival and lower recurrence risk — with findings that researchers describe as very promising.
Dr. Tatum[/caption]
Kristina L. Tatum, PsyD, MS
Instructor
Department of Social and Behavioral Sciences
School of Public Health
A large population-based analysis of more than 841,000 breast cancer patients across the United States examines whether GLP-1 receptor agonist use is associated with improved survival and lower recurrence risk — with findings that researchers describe as very promising.
MedicalResearch.com: What is the background for this study? What are the main findings? Response: Glucagon-like peptide-1 receptor agonists, or GLP-1RAs, have been used since 2005 and as the GLP1RAs treatments and delivery methods have improved, their use has markedly increased. Now it is estimated that nearly 1 in 8 US adults report ever using a GLP-1RA, which includes many people who are using them to treat obesity, diabetes, heart disease, and sleep apnea. There has been some preclinical data from mouse models to suggest that maybe GLP1RAs have an anticancer effect reducing the effects of obesity on tumor growth or progression. We were interested to understand to what extent GLP1RA use among cancer patients might be associated with cancer outcomes, like length of survival after cancer treatment or the chance of recurrence. In our large population-based study using an aggregate of de-identified electronic health record data from more than 841,000 patients with breast cancer across the US, we found that GLP-1 RAs use was associated with significantly improved survival and lower recurrence risk among patients with obesity or type 2 diabetes. Among patients with obesity, GLP-1 RAs use was associated with approximately 65% lower risk of death and a 56% lower risk of recurrence over 10 years compared with nonuse. We also observed substantially improved outcomes among patients with type 2 diabetes compared with insulin or metformin.
 Dr. Fuemmeler[/caption]
Bernard F. Fuemmeler, PhD, MPH
Professor and Gordon D. Ginder, MD Chair in Cancer Research
Associate Director of Population Science, Massey Comprehensive Cancer Center
Director of Research, Family Medicine and Population Health
[caption id="attachment_73640" align="alignleft" width="125"]
Dr. Fuemmeler[/caption]
Bernard F. Fuemmeler, PhD, MPH
Professor and Gordon D. Ginder, MD Chair in Cancer Research
Associate Director of Population Science, Massey Comprehensive Cancer Center
Director of Research, Family Medicine and Population Health
[caption id="attachment_73640" align="alignleft" width="125"] Dr. Tatum[/caption]
Kristina L. Tatum, PsyD, MS
Instructor
Department of Social and Behavioral Sciences
School of Public Health
A large population-based analysis of more than 841,000 breast cancer patients across the United States examines whether GLP-1 receptor agonist use is associated with improved survival and lower recurrence risk — with findings that researchers describe as very promising.
Dr. Tatum[/caption]
Kristina L. Tatum, PsyD, MS
Instructor
Department of Social and Behavioral Sciences
School of Public Health
A large population-based analysis of more than 841,000 breast cancer patients across the United States examines whether GLP-1 receptor agonist use is associated with improved survival and lower recurrence risk — with findings that researchers describe as very promising.
MedicalResearch.com: What is the background for this study? What are the main findings? Response: Glucagon-like peptide-1 receptor agonists, or GLP-1RAs, have been used since 2005 and as the GLP1RAs treatments and delivery methods have improved, their use has markedly increased. Now it is estimated that nearly 1 in 8 US adults report ever using a GLP-1RA, which includes many people who are using them to treat obesity, diabetes, heart disease, and sleep apnea. There has been some preclinical data from mouse models to suggest that maybe GLP1RAs have an anticancer effect reducing the effects of obesity on tumor growth or progression. We were interested to understand to what extent GLP1RA use among cancer patients might be associated with cancer outcomes, like length of survival after cancer treatment or the chance of recurrence. In our large population-based study using an aggregate of de-identified electronic health record data from more than 841,000 patients with breast cancer across the US, we found that GLP-1 RAs use was associated with significantly improved survival and lower recurrence risk among patients with obesity or type 2 diabetes. Among patients with obesity, GLP-1 RAs use was associated with approximately 65% lower risk of death and a 56% lower risk of recurrence over 10 years compared with nonuse. We also observed substantially improved outcomes among patients with type 2 diabetes compared with insulin or metformin.






 Dr. Donofry[/caption]
Shannon D. Donofry Ph.D.
Behavioral Scientist
B.A.Sc. in psychology/neuroscience
University of Pittsburgh-Pittsburgh Campus;
Ph.D, University of Pittsburgh-Pittsburgh Campus
[caption id="attachment_70207" align="alignleft" width="125"]
Dr. Donofry[/caption]
Shannon D. Donofry Ph.D.
Behavioral Scientist
B.A.Sc. in psychology/neuroscience
University of Pittsburgh-Pittsburgh Campus;
Ph.D, University of Pittsburgh-Pittsburgh Campus
[caption id="attachment_70207" align="alignleft" width="125"] Dr. Rancaño[/caption]
Katherine M. Rancaño, Ph.D
Associate Policy Researcher
RAND
MedicalResearch.com: What is the background for this study?
Response: GLP-1 medications were first used to help people with diabetes manage their blood sugar. Lately, they’ve become popular for helping people lose weight, too. Because of this, a lot more people have started using them. In our study, we asked over 8,000 adults from across the country about their use of GLP-1 medications and any side effects they had.
Dr. Rancaño[/caption]
Katherine M. Rancaño, Ph.D
Associate Policy Researcher
RAND
MedicalResearch.com: What is the background for this study?
Response: GLP-1 medications were first used to help people with diabetes manage their blood sugar. Lately, they’ve become popular for helping people lose weight, too. Because of this, a lot more people have started using them. In our study, we asked over 8,000 adults from across the country about their use of GLP-1 medications and any side effects they had.







 Prof. El GHOCH[/caption]
MedicalResearch.com Interview with:
Prof. Marwan EL GHOCH
Prof. El GHOCH[/caption]
MedicalResearch.com Interview with:
Prof. Marwan EL GHOCH













 Dr. Dolatshahi[/caption]
Mahsa Dolatshahi, M.D., M.P.H.
Post-doctoral research fellow
Mallinckrodt Institute of Radiology (MIR)
Washington University School of Medicine
St. Louis
MedicalResearch.com: What is the background for this study?
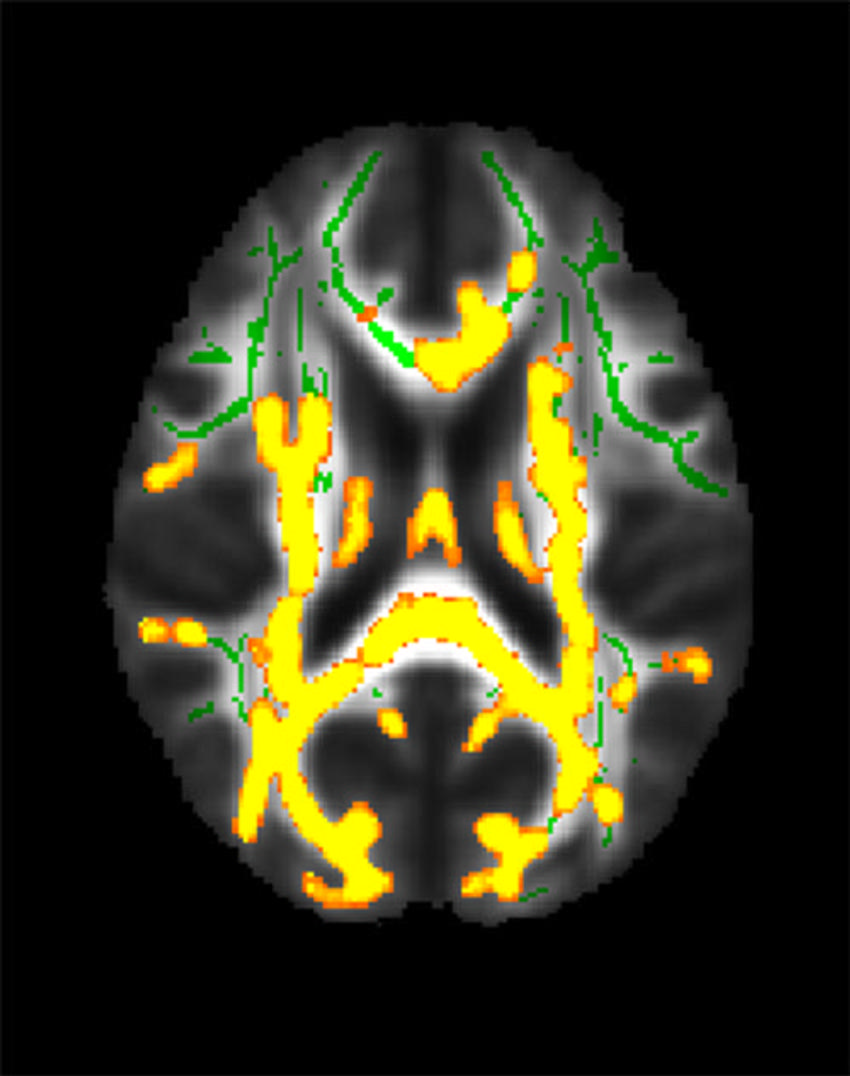
Response: Obesity at midlife is recognized as a risk factor for developing Alzheimer disease decades afterwards. However, body mass index on its own does not adequately represent the risks associated with obesity.
In this study, we went beyond BMI and considered anatomical distribution of body fat, including the metabolically active visceral fat in the belly, and showed its association with Alzheimer pathology in the form of amyloid proteins. In addition, visceral fat along with obesity and insulin resistance were associated with thinning of brain cortex, as early as midlife.
Dr. Dolatshahi[/caption]
Mahsa Dolatshahi, M.D., M.P.H.
Post-doctoral research fellow
Mallinckrodt Institute of Radiology (MIR)
Washington University School of Medicine
St. Louis
MedicalResearch.com: What is the background for this study?
Response: Obesity at midlife is recognized as a risk factor for developing Alzheimer disease decades afterwards. However, body mass index on its own does not adequately represent the risks associated with obesity.
In this study, we went beyond BMI and considered anatomical distribution of body fat, including the metabolically active visceral fat in the belly, and showed its association with Alzheimer pathology in the form of amyloid proteins. In addition, visceral fat along with obesity and insulin resistance were associated with thinning of brain cortex, as early as midlife.
