Author Interviews, Brigham & Women's - Harvard, Melatonin, Pediatrics, Sleep Disorders / 28.09.2022
Myths About Teenager Sleep Needs Are Common
MedicalResearch.com Interview with:
[caption id="attachment_59589" align="alignleft" width="150"] Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.
Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.
 Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.
Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.









 Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.
Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.



 Dr. Goyal[/caption]
Dr. Monika K. Goyal, MD
Associate Division Chief, Emergency Medicine
Children’s National Hospital
Department of Pediatrics, School of Medicine and Health Sciences
The George Washington University
Washington, District of Columbia
MedicalResearch.com: What is the background for this study?
Response: There has been growing attention to the disproportionate use of police force in communities of color. Therefore, we sought to investigate whether Black and Hispanic teenagers have higher rates of death due to police shootings when compared to white youth.
Dr. Goyal[/caption]
Dr. Monika K. Goyal, MD
Associate Division Chief, Emergency Medicine
Children’s National Hospital
Department of Pediatrics, School of Medicine and Health Sciences
The George Washington University
Washington, District of Columbia
MedicalResearch.com: What is the background for this study?
Response: There has been growing attention to the disproportionate use of police force in communities of color. Therefore, we sought to investigate whether Black and Hispanic teenagers have higher rates of death due to police shootings when compared to white youth.

 Dr. Flaherty[/caption]
Michael R. Flaherty, DO
Attending, Pediatric Critical Care Medicine
Co-Director, Trauma and Injury Prevention Outreach Program, MGH
Instructor in Pediatrics,
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study was a joint collaboration between Massachusetts General Hospital and Boston Children’s Hospital. The Consumer Product Safety Commission (CPSC) found an increasing incidence of rare earth magnet ingestions by children causing serious injury; Injuries are particularly serious when a child ingests two of these small magnets, or a magnet with another metal object – this can lead to bowel walls becoming attached and kinked, leading to catastrophic bowel injury and/or death.
The Consumer Product Safety Commission initiated campaigns to limit sales in 2012 with voluntary recalls and safety standards, as well as public awareness campaigns, legislative advocacy, and lawsuits. In October 2014, the CPSC published their final rule, “Safety Standard for Magnet Sets,” which prohibited the sale of magnets based on a pre-specified size and power scale, essentially eliminating the ability to sell SREMs. This rule was appealed by largest manufacturer of these magnets, Zen Magnets, LLC., and in November 2016 this rule was legally reversed by the U.S. Court of Appeals Tenth Circuit resulting in a resurgence of these magnets on the market.
Dr. Flaherty[/caption]
Michael R. Flaherty, DO
Attending, Pediatric Critical Care Medicine
Co-Director, Trauma and Injury Prevention Outreach Program, MGH
Instructor in Pediatrics,
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study was a joint collaboration between Massachusetts General Hospital and Boston Children’s Hospital. The Consumer Product Safety Commission (CPSC) found an increasing incidence of rare earth magnet ingestions by children causing serious injury; Injuries are particularly serious when a child ingests two of these small magnets, or a magnet with another metal object – this can lead to bowel walls becoming attached and kinked, leading to catastrophic bowel injury and/or death.
The Consumer Product Safety Commission initiated campaigns to limit sales in 2012 with voluntary recalls and safety standards, as well as public awareness campaigns, legislative advocacy, and lawsuits. In October 2014, the CPSC published their final rule, “Safety Standard for Magnet Sets,” which prohibited the sale of magnets based on a pre-specified size and power scale, essentially eliminating the ability to sell SREMs. This rule was appealed by largest manufacturer of these magnets, Zen Magnets, LLC., and in November 2016 this rule was legally reversed by the U.S. Court of Appeals Tenth Circuit resulting in a resurgence of these magnets on the market.
 Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor and director of the School of Nursing
College of Health and Human Services at George Mason University
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study? What are the main findings? Has the recommendation changed over the last decade?
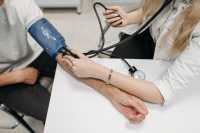
Response: High blood pressure is becoming more common among children and teens in the United States and can have serious negative health effects in childhood and adulthood, such as kidney and heart disease. However, there is not enough research to know whether treating high blood pressure in young people improves cardiovascular health in adulthood.
The Task Force continued to find that there is not enough evidence to recommend for or against screening for high blood pressure in children and teens who do not have signs or symptoms.
Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor and director of the School of Nursing
College of Health and Human Services at George Mason University
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study? What are the main findings? Has the recommendation changed over the last decade?
Response: High blood pressure is becoming more common among children and teens in the United States and can have serious negative health effects in childhood and adulthood, such as kidney and heart disease. However, there is not enough research to know whether treating high blood pressure in young people improves cardiovascular health in adulthood.
The Task Force continued to find that there is not enough evidence to recommend for or against screening for high blood pressure in children and teens who do not have signs or symptoms. Dr. Ganson[/caption]
Kyle T. Ganson, PhD, MSW
Assistant Professor, Factor-Inwentash Faculty of Social Work
University of Toronto
Toronto, Canada
[caption id="attachment_55902" align="alignleft" width="132"]
Dr. Ganson[/caption]
Kyle T. Ganson, PhD, MSW
Assistant Professor, Factor-Inwentash Faculty of Social Work
University of Toronto
Toronto, Canada
[caption id="attachment_55902" align="alignleft" width="132"] Dr. Nagata[/caption]
Jason Nagata, MD, MSc
Assistant Professor of Pediatrics
University of California, San Francisco
San Francisco, California, USA
MedicalResearch.com: What is the background for this study?
Response: A quarter of young adults in the US have reported being unemployed during the COVID-19 pandemic. Young adults may be especially affected by employment loss as they often work in industries most adversely affected by social distancing.
MedicalResearch.com: What are the main findings?
Response: Among a sample of nearly 5,000 young adults age 18 to 26 in the US, we found that since March 2020, young adults who lost their job or were part of a household that experienced employment loss were more likely than those with secure employment to experience four common symptoms of anxiety and depression. This was also true of young adults who expected an employment loss in the next four weeks. The study also found that symptoms of anxiety and depression were common among the sample of young adults. In the seven days prior to the survey, 75% reported being nervous, anxious or on edge, 68% reported not being able to stop or control worrying, 67% reported having little interest or pleasure in doing things, and 64% reported feeling down, depressed, or hopeless.
Dr. Nagata[/caption]
Jason Nagata, MD, MSc
Assistant Professor of Pediatrics
University of California, San Francisco
San Francisco, California, USA
MedicalResearch.com: What is the background for this study?
Response: A quarter of young adults in the US have reported being unemployed during the COVID-19 pandemic. Young adults may be especially affected by employment loss as they often work in industries most adversely affected by social distancing.
MedicalResearch.com: What are the main findings?
Response: Among a sample of nearly 5,000 young adults age 18 to 26 in the US, we found that since March 2020, young adults who lost their job or were part of a household that experienced employment loss were more likely than those with secure employment to experience four common symptoms of anxiety and depression. This was also true of young adults who expected an employment loss in the next four weeks. The study also found that symptoms of anxiety and depression were common among the sample of young adults. In the seven days prior to the survey, 75% reported being nervous, anxious or on edge, 68% reported not being able to stop or control worrying, 67% reported having little interest or pleasure in doing things, and 64% reported feeling down, depressed, or hopeless.

 Dr. Bragg[/caption]
Marie Bragg, PhD
Assistant Professor, Department of Population Health on Health Choice
NYU College of Global Public Health
MedicalResearch.com: What is the background for this study?
Response: We know from previous research that children who see food advertisements eat significantly more calories than children who see non-food advertisements. Those studies led the World Health Organization and National Academy of Medicine to issue reports declaring that exposure to food advertising is a major driver of childhood obesity.
What we don’t know is how frequently unhealthy food and beverage brands are appearing in YouTube videos posted by Kid Influencers. Kid influences are children whose parents film videos of the child playing with toys, unwrapping presents, eating food, or engaging in other family-friendly activities. The parents then post the videos to YouTube for other children and parents to view for entertainment.
Dr. Bragg[/caption]
Marie Bragg, PhD
Assistant Professor, Department of Population Health on Health Choice
NYU College of Global Public Health
MedicalResearch.com: What is the background for this study?
Response: We know from previous research that children who see food advertisements eat significantly more calories than children who see non-food advertisements. Those studies led the World Health Organization and National Academy of Medicine to issue reports declaring that exposure to food advertising is a major driver of childhood obesity.
What we don’t know is how frequently unhealthy food and beverage brands are appearing in YouTube videos posted by Kid Influencers. Kid influences are children whose parents film videos of the child playing with toys, unwrapping presents, eating food, or engaging in other family-friendly activities. The parents then post the videos to YouTube for other children and parents to view for entertainment. 


 Melanie Leung[/caption]
Melanie Leung, M.D.,C.M. candidate 2021
4th-year medical student at McGill University
Division of Allergy and Clinical Immunology
Department of Pediatrics, Montreal Children’s Hospital
McGill University Health Centre, Montreal, QC, Canada
Dr. Moshe Ben-Shoshan, MD, MSc
Pediatric allergist and immunologist at the MCH (Montreal Children’s Hospital) and
Scientist at the Research Institute of the MUHC (McGill University Health Center)
MedicalResearch.com: What is the background for this study?
Response: In Canada, up to 9% of children have at least 1 food allergy. Anaphylaxis is the most severe and potential life-threatening manifestation of food allergy. Peanuts and tree nuts are the main culprits in food-induced anaphylaxis and account for most fatal cases in North America.
Public awareness about peanut and nut anaphylaxis can help to prevent and to act promptly, in the case of anaphylactic reaction. However, the best timing for public awareness campaigns remained unknown, as no previous study looked at the potential association between specific times of the year, such as public holidays, and the incidence of peanut and tree nut anaphylaxis. Our aim was to evaluate the risk of peanut and tree nut-induced anaphylaxis on Halloween, Christmas, Easter, Diwali, Chinese New Year, and Eid al-Adha.
Data was collected from 1390 pediatric cases of peanut or nut-induced anaphylaxis across Canada (Newfoundland & Labrador, Quebec, Ontario, and British Columbia), from 2011 to 2020. 62% of children were boys and the median age was 5.4 years. We compared the average daily number of cases during each holiday and compared it to the rest of the year (i.e.: non-holiday period).
Melanie Leung[/caption]
Melanie Leung, M.D.,C.M. candidate 2021
4th-year medical student at McGill University
Division of Allergy and Clinical Immunology
Department of Pediatrics, Montreal Children’s Hospital
McGill University Health Centre, Montreal, QC, Canada
Dr. Moshe Ben-Shoshan, MD, MSc
Pediatric allergist and immunologist at the MCH (Montreal Children’s Hospital) and
Scientist at the Research Institute of the MUHC (McGill University Health Center)
MedicalResearch.com: What is the background for this study?
Response: In Canada, up to 9% of children have at least 1 food allergy. Anaphylaxis is the most severe and potential life-threatening manifestation of food allergy. Peanuts and tree nuts are the main culprits in food-induced anaphylaxis and account for most fatal cases in North America.
Public awareness about peanut and nut anaphylaxis can help to prevent and to act promptly, in the case of anaphylactic reaction. However, the best timing for public awareness campaigns remained unknown, as no previous study looked at the potential association between specific times of the year, such as public holidays, and the incidence of peanut and tree nut anaphylaxis. Our aim was to evaluate the risk of peanut and tree nut-induced anaphylaxis on Halloween, Christmas, Easter, Diwali, Chinese New Year, and Eid al-Adha.
Data was collected from 1390 pediatric cases of peanut or nut-induced anaphylaxis across Canada (Newfoundland & Labrador, Quebec, Ontario, and British Columbia), from 2011 to 2020. 62% of children were boys and the median age was 5.4 years. We compared the average daily number of cases during each holiday and compared it to the rest of the year (i.e.: non-holiday period).

 Dr. Huang[/caption]
Jennifer Huang, MD
Dr. Huang is a pediatric dermatologist at Boston Children’s Hospital and Dana-Farber Cancer Institute.
She is an Associate Professor of Dermatology at Harvard Medical School.
Dr. Huang is a member of the
Dr. Huang[/caption]
Jennifer Huang, MD
Dr. Huang is a pediatric dermatologist at Boston Children’s Hospital and Dana-Farber Cancer Institute.
She is an Associate Professor of Dermatology at Harvard Medical School.
Dr. Huang is a member of the 

 Dr. Auger[/caption]
Katherine A. S. Auger, MD, MSc
Division of Hospital Medicine
James M. Anderson Center for Health Systems Excellence,
Cincinnati Children’s Hospital Medical Center
Department of Pediatrics, University of Cincinnati College of Medicine
Pediatric Research in Inpatient Settings Network
Cincinnati, Ohio
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: All states closed schools in the spring of 2020 to try to mitigate the spread of COVID-19. Our study demonstrated a large, significant association between school closure and fewer COVID-19 cases and deaths even when accounting for other state policies.
Dr. Auger[/caption]
Katherine A. S. Auger, MD, MSc
Division of Hospital Medicine
James M. Anderson Center for Health Systems Excellence,
Cincinnati Children’s Hospital Medical Center
Department of Pediatrics, University of Cincinnati College of Medicine
Pediatric Research in Inpatient Settings Network
Cincinnati, Ohio
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: All states closed schools in the spring of 2020 to try to mitigate the spread of COVID-19. Our study demonstrated a large, significant association between school closure and fewer COVID-19 cases and deaths even when accounting for other state policies.


 Dr. Yonker[/caption]
Lael Yonker, MD
Pediatric Pulmonology
Director, MGH Cystic Fibrosis Center
Principal Investigator, Pediatric COVID biorepository
Mucosal Immunology and Biology Research Center
Massachusetts General Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Children were initially felt to be spared from the COVID-19 pandemic. Here, we show that children can become sick from SARS-CoV-2 infection, and even if the initial illness is mild, some go on to develop a severe inflammatory illness after the initial illness. We also show that children can carry very high levels of virus early in the course of infection, suggesting they may play a larger role in spreading the virus than previously thought.
Dr. Yonker[/caption]
Lael Yonker, MD
Pediatric Pulmonology
Director, MGH Cystic Fibrosis Center
Principal Investigator, Pediatric COVID biorepository
Mucosal Immunology and Biology Research Center
Massachusetts General Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Children were initially felt to be spared from the COVID-19 pandemic. Here, we show that children can become sick from SARS-CoV-2 infection, and even if the initial illness is mild, some go on to develop a severe inflammatory illness after the initial illness. We also show that children can carry very high levels of virus early in the course of infection, suggesting they may play a larger role in spreading the virus than previously thought.
 Dr. Walline[/caption]
Jeffrey J. Walline, OD PhD
Associate Dean for Research
The Ohio State University
Columbus, OH 43210-1240
MedicalResearch.com: What is the background for this study?
Response: Greater amounts of nearsightedness are related to higher risks of sight-threatening complications in adulthood, so anything we can do to slow the progression of nearsightedness in childhood can have meaningful benefits in the future.
As the prevalence of nearsightedness increases worldwide and affects approximately 1/3 of the people in the United States, a treatment that provides clear vision AND slows the progression of nearsightedness can have a profound effect.
Dr. Walline[/caption]
Jeffrey J. Walline, OD PhD
Associate Dean for Research
The Ohio State University
Columbus, OH 43210-1240
MedicalResearch.com: What is the background for this study?
Response: Greater amounts of nearsightedness are related to higher risks of sight-threatening complications in adulthood, so anything we can do to slow the progression of nearsightedness in childhood can have meaningful benefits in the future.
As the prevalence of nearsightedness increases worldwide and affects approximately 1/3 of the people in the United States, a treatment that provides clear vision AND slows the progression of nearsightedness can have a profound effect.