Author Interviews, COVID -19 Coronavirus, JAMA, Pediatrics / 05.08.2020
Young Children Have Same or More COVID-19 in Respiratory Tract as Adults
MedicalResearch.com Interview with:
[caption id="attachment_54986" align="alignleft" width="200"] Dr. Heald-Sargent[/caption]
Taylor Heald-Sargent, M.D., Ph.D.
Ann & Robert H. Lurie Children’s Hospital
Chicago
MedicalResearch.com: What is the background for this study?
Response: Given the ongoing debate around the ability of children to transmit SARS-CoV-2, we noticed that our clinical data could address one of the prevalent assumptions. Some people postulated that the reason children have less severe infections with SARS-CoV-2 is because they are not able to replicate virus as much as adults and therefore may not transmit as readily.
Dr. Heald-Sargent[/caption]
Taylor Heald-Sargent, M.D., Ph.D.
Ann & Robert H. Lurie Children’s Hospital
Chicago
MedicalResearch.com: What is the background for this study?
Response: Given the ongoing debate around the ability of children to transmit SARS-CoV-2, we noticed that our clinical data could address one of the prevalent assumptions. Some people postulated that the reason children have less severe infections with SARS-CoV-2 is because they are not able to replicate virus as much as adults and therefore may not transmit as readily.
 Dr. Heald-Sargent[/caption]
Taylor Heald-Sargent, M.D., Ph.D.
Ann & Robert H. Lurie Children’s Hospital
Chicago
MedicalResearch.com: What is the background for this study?
Response: Given the ongoing debate around the ability of children to transmit SARS-CoV-2, we noticed that our clinical data could address one of the prevalent assumptions. Some people postulated that the reason children have less severe infections with SARS-CoV-2 is because they are not able to replicate virus as much as adults and therefore may not transmit as readily.
Dr. Heald-Sargent[/caption]
Taylor Heald-Sargent, M.D., Ph.D.
Ann & Robert H. Lurie Children’s Hospital
Chicago
MedicalResearch.com: What is the background for this study?
Response: Given the ongoing debate around the ability of children to transmit SARS-CoV-2, we noticed that our clinical data could address one of the prevalent assumptions. Some people postulated that the reason children have less severe infections with SARS-CoV-2 is because they are not able to replicate virus as much as adults and therefore may not transmit as readily. 



 Dr. Perrett[/caption]
Kirsten P Perrett MD PhD
Group Leader/Clinician Scientist Fellow
Population Allergy Research Group and
Melbourne Children's Trial Centre
Murdoch Children's Research Institute
Rachel L Peters PhD
Murdoch Children’s Research Institute
Department of Paediatrics
The University of Melbourne
Parkville, Australia
MedicalResearch.com: What is the background for this study?
Dr. Perrett[/caption]
Kirsten P Perrett MD PhD
Group Leader/Clinician Scientist Fellow
Population Allergy Research Group and
Melbourne Children's Trial Centre
Murdoch Children's Research Institute
Rachel L Peters PhD
Murdoch Children’s Research Institute
Department of Paediatrics
The University of Melbourne
Parkville, Australia
MedicalResearch.com: What is the background for this study?


 Dr. Dixon[/caption]
Cinnamon A. Dixon, DO, MPH
Associate Professor of Pediatrics
University of Colorado School of Medicine
Children’s Hospital Colorado
Senior Investigator | Center for Global Health
Colorado School of Public Health
Aurora, CO
MedicalResearch.com: What is the background for this commentary?
Response: Dog bites are a long-standing public health problem. Each year there are approximately 4.5 million dog bites across the Unites States (US),1 and global estimates suggest tens of millions of these injuries worldwide.2 Children are the most vulnerable population with nearly 1 million annual dog bites in the US and more severe injury outcomes.1
National organizations espouse consistent strategies on how to prevent dog bites to children, however studies reveal that most children have never received dog bite prevention education.3,4 Furthermore, children lack critical knowledge of how to prevent dog bites in high-risk “resource guarding” situations (such as when a dog is eating or chewing on toys).4
During the COVID-19 pandemic, millions of US households are experiencing restrictions in activities. Children now spend more time in the home environment and presumably have increased exposure to their pet dogs. Parents and caregivers likely experience greater stress with more potential for competing interests and resultant decreased supervision of their children and dogs. Finally, pet dogs may be affected by the increased tension of their environment and be more likely to mirror the emotions of their human caregivers.
We hypothesized that these combined elements compound the risk of dog bites to children during the COVID-19 pandemic.
Dr. Dixon[/caption]
Cinnamon A. Dixon, DO, MPH
Associate Professor of Pediatrics
University of Colorado School of Medicine
Children’s Hospital Colorado
Senior Investigator | Center for Global Health
Colorado School of Public Health
Aurora, CO
MedicalResearch.com: What is the background for this commentary?
Response: Dog bites are a long-standing public health problem. Each year there are approximately 4.5 million dog bites across the Unites States (US),1 and global estimates suggest tens of millions of these injuries worldwide.2 Children are the most vulnerable population with nearly 1 million annual dog bites in the US and more severe injury outcomes.1
National organizations espouse consistent strategies on how to prevent dog bites to children, however studies reveal that most children have never received dog bite prevention education.3,4 Furthermore, children lack critical knowledge of how to prevent dog bites in high-risk “resource guarding” situations (such as when a dog is eating or chewing on toys).4
During the COVID-19 pandemic, millions of US households are experiencing restrictions in activities. Children now spend more time in the home environment and presumably have increased exposure to their pet dogs. Parents and caregivers likely experience greater stress with more potential for competing interests and resultant decreased supervision of their children and dogs. Finally, pet dogs may be affected by the increased tension of their environment and be more likely to mirror the emotions of their human caregivers.
We hypothesized that these combined elements compound the risk of dog bites to children during the COVID-19 pandemic.

 Dr. Paller[/caption]
Amy S Paller, MD
Chair, Department of Dermatology
Director, Skin Biology and Diseases Resource-Based Center
Walter J. Hamlin Professor of Dermatology
Professor of Dermatology and Pediatrics (Dermatology)
Feinberg School of Medicine
Northwestern University
Dr. Paller discusses the FDA approval of Dupixent® (dupilumab) for children aged 6 to 11 years with moderate-to-severe atopic dermatitis (eczema), whose disease is not adequately controlled with topical prescription therapies or when those therapies are not advisable.
MedicalResearch.com: What is the background for this announcement? Would you briefly discuss what is meant by atopic dermatitis and how it affects children?
Response: “Atopic dermatitis, the most common form of eczema, is a chronic inflammatory disease that often appears as a rash on the skin. Moderate-to-severe atopic dermatitis is characterized by rashes that can potentially cover much of the body and can include intense, persistent itching, skin lesions and skin dryness, cracking, redness or darkness, crusting and oozing. Itch is one of the most burdensome symptoms for patients and can be debilitating.
This recent FDA approval expands the use of Dupilumab in the U.S. to include children aged 6 to 11 years with uncontrolled moderate-to-severe atopic dermatitis, making it the only biologic medicine approved for this use in this population. Dupilumab is also approved in the U.S. to treat patients aged 12 years and older with moderate-to-severe atopic dermatitis.
Moderate-to-severe atopic dermatitis can place a particularly substantial burden on young children aged 6 to 11 years and their families. Limited treatment options leave many of these children to cope with intense, unrelenting itch and skin lesions. Families of these children can spend countless hours helping them to manage their disease.”
Dr. Paller[/caption]
Amy S Paller, MD
Chair, Department of Dermatology
Director, Skin Biology and Diseases Resource-Based Center
Walter J. Hamlin Professor of Dermatology
Professor of Dermatology and Pediatrics (Dermatology)
Feinberg School of Medicine
Northwestern University
Dr. Paller discusses the FDA approval of Dupixent® (dupilumab) for children aged 6 to 11 years with moderate-to-severe atopic dermatitis (eczema), whose disease is not adequately controlled with topical prescription therapies or when those therapies are not advisable.
MedicalResearch.com: What is the background for this announcement? Would you briefly discuss what is meant by atopic dermatitis and how it affects children?
Response: “Atopic dermatitis, the most common form of eczema, is a chronic inflammatory disease that often appears as a rash on the skin. Moderate-to-severe atopic dermatitis is characterized by rashes that can potentially cover much of the body and can include intense, persistent itching, skin lesions and skin dryness, cracking, redness or darkness, crusting and oozing. Itch is one of the most burdensome symptoms for patients and can be debilitating.
This recent FDA approval expands the use of Dupilumab in the U.S. to include children aged 6 to 11 years with uncontrolled moderate-to-severe atopic dermatitis, making it the only biologic medicine approved for this use in this population. Dupilumab is also approved in the U.S. to treat patients aged 12 years and older with moderate-to-severe atopic dermatitis.
Moderate-to-severe atopic dermatitis can place a particularly substantial burden on young children aged 6 to 11 years and their families. Limited treatment options leave many of these children to cope with intense, unrelenting itch and skin lesions. Families of these children can spend countless hours helping them to manage their disease.”
 Dr. Garstang[/caption]
Dr Joanna Garstang
Consultant Community Paediatrician / Designated Doctor for Child Death
Allenscroft Children's Centre
Kings Heath, Birmingham UK
MedicalResearch.com: What is the background for this study?
Response: Each year in England and Wales there around 3-400 babies die unexpectedly, in many cases the cause of death remains unexplained and these deaths are called Sudden Infant Death Syndrome (SIDS). Parents are understandably anxious about the risks for future children, the Care of Next Infant (CONI) programme was set up to offer support for families. In this study, we looked at records of families registered with CONI between 2000-2015 to determine the frequency and causes for repeat unexpected infant deaths.
Dr. Garstang[/caption]
Dr Joanna Garstang
Consultant Community Paediatrician / Designated Doctor for Child Death
Allenscroft Children's Centre
Kings Heath, Birmingham UK
MedicalResearch.com: What is the background for this study?
Response: Each year in England and Wales there around 3-400 babies die unexpectedly, in many cases the cause of death remains unexplained and these deaths are called Sudden Infant Death Syndrome (SIDS). Parents are understandably anxious about the risks for future children, the Care of Next Infant (CONI) programme was set up to offer support for families. In this study, we looked at records of families registered with CONI between 2000-2015 to determine the frequency and causes for repeat unexpected infant deaths.

 Dr. Travers[/caption]
Colm Travers, M.D., MSPH
Assistant Professor
Department of Pediatrics
University of Alabama at Birmingham
MedicalResearch.com: What is the background for this study?
Response: It is known that black mothers are much more likely to deliver preterm and low birth weight infants. The purpose of this study was to determine whether racial/ethnic disparities in care practices and outcomes were decreasing or increasing among extremely preterm infants.
These are infants born from 22 to 27 weeks of gestation who have a high risk of death and major illnesses.
Dr. Travers[/caption]
Colm Travers, M.D., MSPH
Assistant Professor
Department of Pediatrics
University of Alabama at Birmingham
MedicalResearch.com: What is the background for this study?
Response: It is known that black mothers are much more likely to deliver preterm and low birth weight infants. The purpose of this study was to determine whether racial/ethnic disparities in care practices and outcomes were decreasing or increasing among extremely preterm infants.
These are infants born from 22 to 27 weeks of gestation who have a high risk of death and major illnesses. 




 Dr. Tandon[/caption]
Pooja S. Tandon, MD, MPH
Center for Child Health, Behavior and Development
Seattle Children's Research Institute
MedicalResearch.com: What is the background for this study?
Response: Cell phone use is common among middle and high school students, yet we do not have an understanding of school cell phone policies and practices in the U.S. We conducted a survey of public schools serving grades 6-12. The survey sent to over 1,100 school principals, representing a national sample of schools across the U.S., asked questions about the presence of a cell phone policy for students and staff and restrictions on phone use. Additional questions addressed consequences of policy violation, the use of cell phones for curricular activities and principals’ attitudes toward cell phone policies.
Dr. Tandon[/caption]
Pooja S. Tandon, MD, MPH
Center for Child Health, Behavior and Development
Seattle Children's Research Institute
MedicalResearch.com: What is the background for this study?
Response: Cell phone use is common among middle and high school students, yet we do not have an understanding of school cell phone policies and practices in the U.S. We conducted a survey of public schools serving grades 6-12. The survey sent to over 1,100 school principals, representing a national sample of schools across the U.S., asked questions about the presence of a cell phone policy for students and staff and restrictions on phone use. Additional questions addressed consequences of policy violation, the use of cell phones for curricular activities and principals’ attitudes toward cell phone policies.

 Barbara Chaiyachati, MD PhD
SafePlace: The Center for Child Protection and Health
Division of General Pediatrics
The Children’s Hospital of Philadelphia,
Center for Pediatric Clinical Effectiveness
University of Pennsylvania
Philadelphia, Pennsylvania
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Children in foster care have high rates of medical problems including chronic diseases. There is less known about the differences in mortality for children in foster care.
Looking at national data from 2003 to 2016, this study finds that children (ages 1 to 18) in foster care have higher mortality compared to children in the general population and that the difference in mortality has increased over time.
Barbara Chaiyachati, MD PhD
SafePlace: The Center for Child Protection and Health
Division of General Pediatrics
The Children’s Hospital of Philadelphia,
Center for Pediatric Clinical Effectiveness
University of Pennsylvania
Philadelphia, Pennsylvania
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Children in foster care have high rates of medical problems including chronic diseases. There is less known about the differences in mortality for children in foster care.
Looking at national data from 2003 to 2016, this study finds that children (ages 1 to 18) in foster care have higher mortality compared to children in the general population and that the difference in mortality has increased over time. 















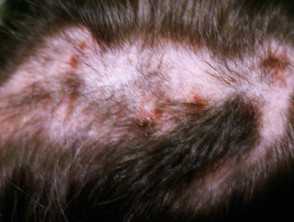
 Dr. Diaz[/caption]
Lucia Diaz, M.D., is chief of pediatric dermatology, dermatology residency associate program director and assistant professor of medicine and pediatrics at Dell Medical School. She is also co-director of the dermatology-rheumatology combined clinic at Dell Children’s Medical Center.
[caption id="attachment_52796" align="alignleft" width="150"]
Dr. Diaz[/caption]
Lucia Diaz, M.D., is chief of pediatric dermatology, dermatology residency associate program director and assistant professor of medicine and pediatrics at Dell Medical School. She is also co-director of the dermatology-rheumatology combined clinic at Dell Children’s Medical Center.
[caption id="attachment_52796" align="alignleft" width="150"] Dr. Jaquez[/caption]
Sasha Jaquez, Ph.D. is a pediatric psychologist at Dell Children's Medical School/Dell Children's Medical Center and specializes in seeing children with chronic medical illness, including skin disorders.
[caption id="attachment_52791" align="alignleft" width="294"]
Dr. Jaquez[/caption]
Sasha Jaquez, Ph.D. is a pediatric psychologist at Dell Children's Medical School/Dell Children's Medical Center and specializes in seeing children with chronic medical illness, including skin disorders.
[caption id="attachment_52791" align="alignleft" width="294"]