Author Interviews, Cleveland Clinic, Infections / 31.10.2020
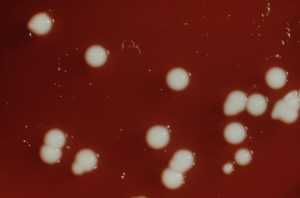
Shoes, Stretchers and Floors May Transmit Pathogens in Hospital Settings
MedicalResearch.com Interview with:
MedicalResearch.com Interview with:
[caption id="attachment_32590" align="alignleft" width="200"] Dr. Curtis J. Donskey[/caption]
Curtis J. Donskey, MD
Professor of Medicine
Case Western Reserve University
Staff Physician, Infectious Diseases Section,
Louis Stokes Cleveland VA Medical Center
MedicalResearch.com: What is the background for this study?
Response: The goal of the study was to obtain a better understanding of how healthcare-associated pathogens are transmitted. Infection control efforts tend to emphasize hand hygiene and cleaning of high-touch surfaces in patient rooms. However, there is evidence that portable equipment and floors could be underappreciated sources of transmission.
We previously found that a nonpathogenic virus inoculated onto floors in patient rooms spread rapidly to the hands of patients and to surfaces in the room and throughout the ward. This raised concern that pathogens could spread by the same route.
Dr. Curtis J. Donskey[/caption]
Curtis J. Donskey, MD
Professor of Medicine
Case Western Reserve University
Staff Physician, Infectious Diseases Section,
Louis Stokes Cleveland VA Medical Center
MedicalResearch.com: What is the background for this study?
Response: The goal of the study was to obtain a better understanding of how healthcare-associated pathogens are transmitted. Infection control efforts tend to emphasize hand hygiene and cleaning of high-touch surfaces in patient rooms. However, there is evidence that portable equipment and floors could be underappreciated sources of transmission.
We previously found that a nonpathogenic virus inoculated onto floors in patient rooms spread rapidly to the hands of patients and to surfaces in the room and throughout the ward. This raised concern that pathogens could spread by the same route.
 Dr. Curtis J. Donskey[/caption]
Curtis J. Donskey, MD
Professor of Medicine
Case Western Reserve University
Staff Physician, Infectious Diseases Section,
Louis Stokes Cleveland VA Medical Center
MedicalResearch.com: What is the background for this study?
Response: The goal of the study was to obtain a better understanding of how healthcare-associated pathogens are transmitted. Infection control efforts tend to emphasize hand hygiene and cleaning of high-touch surfaces in patient rooms. However, there is evidence that portable equipment and floors could be underappreciated sources of transmission.
We previously found that a nonpathogenic virus inoculated onto floors in patient rooms spread rapidly to the hands of patients and to surfaces in the room and throughout the ward. This raised concern that pathogens could spread by the same route.
Dr. Curtis J. Donskey[/caption]
Curtis J. Donskey, MD
Professor of Medicine
Case Western Reserve University
Staff Physician, Infectious Diseases Section,
Louis Stokes Cleveland VA Medical Center
MedicalResearch.com: What is the background for this study?
Response: The goal of the study was to obtain a better understanding of how healthcare-associated pathogens are transmitted. Infection control efforts tend to emphasize hand hygiene and cleaning of high-touch surfaces in patient rooms. However, there is evidence that portable equipment and floors could be underappreciated sources of transmission.
We previously found that a nonpathogenic virus inoculated onto floors in patient rooms spread rapidly to the hands of patients and to surfaces in the room and throughout the ward. This raised concern that pathogens could spread by the same route.


 Dr. Hooker[/caption]
Edmond A. Hooker, MD, DrPH
Professor, Department of Health Services Administration
MHSA Associate Director for Accreditation
Xavier University
Cincinnati, Ohio
MedicalResearch.com: What is the background for this study?
Response: Healthcare acquired infections are still a huge problem in the US. Most hospitals are not following the hospital bed manufacturers guidelines for cleaning these mattresses and bed decks (the metal bed frame). Many use only a single step, when the manufacturers recommend a 5-6 step process (pre-clean any obvious soil, clean, rinse off cleaner, disinfect, rinse off disinfectant, inspect mattress for damage). The problem is that, if done, this takes 45 minutes to 1 hours. Most hospitals turn over a hospital room in less than 30 minutes. The launderable bed cover allows the bed to be cleaned and turned over in minutes, not an hours.
Dr. Hooker[/caption]
Edmond A. Hooker, MD, DrPH
Professor, Department of Health Services Administration
MHSA Associate Director for Accreditation
Xavier University
Cincinnati, Ohio
MedicalResearch.com: What is the background for this study?
Response: Healthcare acquired infections are still a huge problem in the US. Most hospitals are not following the hospital bed manufacturers guidelines for cleaning these mattresses and bed decks (the metal bed frame). Many use only a single step, when the manufacturers recommend a 5-6 step process (pre-clean any obvious soil, clean, rinse off cleaner, disinfect, rinse off disinfectant, inspect mattress for damage). The problem is that, if done, this takes 45 minutes to 1 hours. Most hospitals turn over a hospital room in less than 30 minutes. The launderable bed cover allows the bed to be cleaned and turned over in minutes, not an hours. 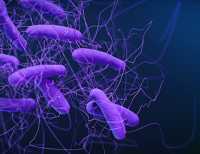
 Dr. Marra[/caption]
Alexandre R. Marra, MD PhD
Iowa Infection Prevention Research Group
University of Iowa Carver College of Medicine
Division of Medical Practice, Hospital Israelita Albert Einstein
São Paulo, Brazil
MedicalResearch.com: What is the background for this study?
Response: This is a comprehensive systematic literature review evaluating the burden of C. difficile infections in the U.S healthcare system. The literature has diverse studies with variable outcomes. Thus, we only included incidence estimates derived from multicenter studies. In our meta-analysis to calculate incidence, data were pooled only with denominators using the same unit (patient-days) to avoid comparisons with different denominators. For length of stay (LOS), we only included studies that used advanced statistical methods (e.g., propensity score matching).
Dr. Marra[/caption]
Alexandre R. Marra, MD PhD
Iowa Infection Prevention Research Group
University of Iowa Carver College of Medicine
Division of Medical Practice, Hospital Israelita Albert Einstein
São Paulo, Brazil
MedicalResearch.com: What is the background for this study?
Response: This is a comprehensive systematic literature review evaluating the burden of C. difficile infections in the U.S healthcare system. The literature has diverse studies with variable outcomes. Thus, we only included incidence estimates derived from multicenter studies. In our meta-analysis to calculate incidence, data were pooled only with denominators using the same unit (patient-days) to avoid comparisons with different denominators. For length of stay (LOS), we only included studies that used advanced statistical methods (e.g., propensity score matching).




![MedicalResearch.com Interview with: Gili Regev-Yochay, MD, Lead author Director of the Infection Prevention & Control Unit Sheba Medical Center Tel HaShomer, Israel. MedicalResearch.com: What is the background for this study? Response: CPE (Carbapenemase producing Enterobacteriaceae) is endemic in Israel. In our ICU we had a prolonged CPE outbreak with one particular bacteria, which is not that common (OXA-48 producing-Serratia marcescens). Enhancing our regular control measures (hand hygiene, increased cleaning etc..) did not contain the outbreak. MedicalResearch.com: What are the main findings? Response: The outbreak source were the sink-traps in nearly all the patient rooms, which were contaminated with this same bacteria. Once we understood that this was the source we took two measures: 1) Sink decontamination efforts, including intensive chlorine washes of the drainage and water system, replacement of all sink-traps, acetic acid treatment and more, all these efforts were only partially and only temporarily successful. So that even today, after a year of such efforts and a period in which we didn't have any patients with this infection, the drainage system is still contaminated with these bugs and they grow in the sink-traps and can be found in the sink outlets. 2) The second measure we took was an educational intervention, where we engaged the ICU team through workshops to the issue of the contaminated sinks and together enforced strict "sink-use guidelines" (sinks are to be used ONLY for hand washing, prohibiting placement of any materials near the sinks, etc.). Using these two measure the outbreak was fully contained. To date, nearly 1.5 years since the last outbreak case, we did not have any further infections in our ICU patients with this bug. MedicalResearch.com: What should readers take away from your report? Response: Sink-traps and drainage systems can be a major source of CPE transmission. While traditionally CPE outbreaks were attributed to patient-to patient transmission, the environment and particularly water and drainage system appears to play a major role. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: There is urgent need to find a technological solution for drainage system contaminations. While some have suggested to get rid of sinks in ICU this is probably not realistic in the era of emerging Clostridium infections (where washing hands, and not only alcohol rubs are needed). Citation: Gili Regev-Yochay, Gill Smollan, Ilana Tal, Nani Pinas Zade, Yael Haviv, Valery Nudelman, Ohad Gal-Mor, Hanaa Jaber, Eyal Zimlichman, Nati Keller, Galia Rahav. Sink traps as the source of transmission of OXA-48–producing Serratia marcescens in an intensive care unit. Infection Control & Hospital Epidemiology, 2018; 1 DOI: 1017/ice.2018.235 [wysija_form id="3"] [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/sink.jpg)
![MedicalResearch.com Interview with: Gili Regev-Yochay, MD, Lead author Director of the Infection Prevention & Control Unit Sheba Medical Center Tel HaShomer, Israel. MedicalResearch.com: What is the background for this study? Response: CPE (Carbapenemase producing Enterobacteriaceae) is endemic in Israel. In our ICU we had a prolonged CPE outbreak with one particular bacteria, which is not that common (OXA-48 producing-Serratia marcescens). Enhancing our regular control measures (hand hygiene, increased cleaning etc..) did not contain the outbreak. MedicalResearch.com: What are the main findings? Response: The outbreak source were the sink-traps in nearly all the patient rooms, which were contaminated with this same bacteria. Once we understood that this was the source we took two measures: 1) Sink decontamination efforts, including intensive chlorine washes of the drainage and water system, replacement of all sink-traps, acetic acid treatment and more, all these efforts were only partially and only temporarily successful. So that even today, after a year of such efforts and a period in which we didn't have any patients with this infection, the drainage system is still contaminated with these bugs and they grow in the sink-traps and can be found in the sink outlets. 2) The second measure we took was an educational intervention, where we engaged the ICU team through workshops to the issue of the contaminated sinks and together enforced strict "sink-use guidelines" (sinks are to be used ONLY for hand washing, prohibiting placement of any materials near the sinks, etc.). Using these two measure the outbreak was fully contained. To date, nearly 1.5 years since the last outbreak case, we did not have any further infections in our ICU patients with this bug. MedicalResearch.com: What should readers take away from your report? Response: Sink-traps and drainage systems can be a major source of CPE transmission. While traditionally CPE outbreaks were attributed to patient-to patient transmission, the environment and particularly water and drainage system appears to play a major role. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: There is urgent need to find a technological solution for drainage system contaminations. While some have suggested to get rid of sinks in ICU this is probably not realistic in the era of emerging Clostridium infections (where washing hands, and not only alcohol rubs are needed). Citation: Gili Regev-Yochay, Gill Smollan, Ilana Tal, Nani Pinas Zade, Yael Haviv, Valery Nudelman, Ohad Gal-Mor, Hanaa Jaber, Eyal Zimlichman, Nati Keller, Galia Rahav. Sink traps as the source of transmission of OXA-48–producing Serratia marcescens in an intensive care unit. Infection Control & Hospital Epidemiology, 2018; 1 DOI: 1017/ice.2018.235 [wysija_form id="3"] [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/sink-200x150.jpg)