15 Dec Examination of Nailfold Capillaries Can Unmask Systemic Nature of Exfoliation Glaucoma
MedicalResearch.com Interview with:

Dr. Ritch
Robert Ritch, MD, FACS, FARVO
Shelley and Steven Einhorn Distinguished Chair
Professor of Ophthalmology, Surgeon Director Emeritus
Chief, Glaucoma Services Emeritus
The New York Eye and Ear Infirmary of Mount Sinai
New York, NY 10003
Founder, Medical Director and
Chairman, Scientific Advisory Board
The Glaucoma Foundation
MedicalResearch.com: What is the background for this study?
Response: Nailfold capillaroscopy (NFC), long used in rheumatology is a new approach to investigation of glaucoma.
Posterior to the nailbed and just anterior to the proximal nailfold is the cuticle, which has no structural elements visible to the naked eye. NFC is a non-invasive imaging modality that provides a highly magnified view of the capillaries at the nailfold of digits. It has also been used in ophthalmology to show morphological changes at the nailfold capillaries of POAG and XFG/XFS patients, helping to confirm the systemic nature of these diseases.

Nailfold Capillaroscopy / Dr. Ritch
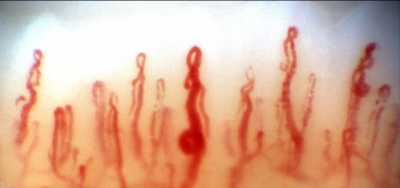
With nailfold capillaroscopy, an extensive array of capillaries can be seen greatly enlarged on a monitor screen. Capillary loops can be imaged, stored, recorded with videoscopy, and blood flow actively imaged and measured..
The first series of papers on glaucoma were written by Prof Josef Flammer’s group at the turn of the 21st century, looking at vasospasm, blood flow in normal-tension and high-tension glaucoma, and relating ocular blood flow alterations to systemic vascular regulation and relating laser Doppler flowmetry to NFC.
Studies from Korea later associated nailbed hemorrhages and loss of nailbed capillaries to the presence of optic disc hemorrhages and investigated correlation of of heart rate variability with visual field defects and nailfold capillaroscopy.
Studies by our group began with the publication in 2015 of a paper by Pasquale et al (Nailfold Capillary Abnormalities in Primary Open-Angle Glaucoma: A Multisite Study. IOVS;56:7021) using NFC video microscopy, associating dilated capillaries, avascular zones, and hemorrhages with primary open-angle glaucoma. Successive manuscripts and presentations at conferences have indicated differences between capillary loop patterns in high-tension and normal-tension POAG and exfoliation syndrome/exfoliation glaucoma.
Our goal in this paper was to compare nailfold peripheral blood flow in XFG, which had not previously been compared to control subjects using NFC. We explored the peripheral blood flow at the nailfold of patients with high-tension glaucoma, normal-tension glaucoma, exfoliation glaucoma (XFG) and compared it to control subjects further evaluate the possible differences between these glaucoma entities. We examined the morphology and extent of nailfold capillary loops, vascular tortuosity, blood flow, and nailfold hemorrhages.
MedicalResearch.com: What are the main findings?
Response: Both primary open-angle glaucoma (POAC) and XFs/XFG involve abnormal blood flow, but XFS/XFG is increasingly known to be associated with cardiovascular and cerebrovascular disorders and more recently, disease of elastic tissue. XFS is a distinct disease with specific genetic, biochemical, cell biological, and pathophysiologic mechanisms leading to trabecular dysfunction. It is the most common recognizable cause of open angle glaucoma worldwide and is not a “type” or form” of glaucoma, but rather glaucoma is the most common manifestation of this systemic disease.
We hypothesized that XFS/XFG would reveal more pronounced differences from primary open-angle glaucoma. We found a significantly lower and limited range of resting peripheral blood flow in XFG. This may represent stiffened vasculature or impaired maximal flow in the peripheral vasculature of XFG patients compared to control subjects. It may also be related to increased tortuosity in XFS patients. XFS has also been reported to show decreased optic nerve head blood flow to the optic nerve head.
Our study is the first to show decreased non-ocular resting peripheral capillary blood flow as measured by nailfold capillaroscopy in XFG compared to control subjects even after correction for multiple co-variables. The vascular hemodynamic alteration at the peripheral nailfold circulation in XFG may represent the systemic nature and etiology of exfoliation glaucoma, which necessitates further studies.
MedicalResearch.com: What should readers take away from your report?
Response: What use can we conceive of to carry this work further? First, assuming that differences in nailfold capillaroscopy morphology and blood flow in different glaucomas reflect the vasculature both systemically and in the eye, this could be the beginning of a new approach to the disease. It might serve as a diagnostic tool to differentiate or substantiate findings in different glaucomas. Studies measuring blood flow might be indicative or predictive of glaucoma severity.
MedicalResearch.com: What recommendations do you have for future research as a result of this work?
Response: Correlations between NFC and ocular blood flow are an additional area of investigation and if these were to bear out, the results of NFC might be predictive of a predisposition to the rate of progression. The effect of drugs given topically or systemically might be reflected in nailfold capillaroscopy and counterintuitively, the effect of drugs on NFC might be reflected in measurement of ocular blood flow, providing an alternative means of assessing or verifying alterations in the ocular circulation. Future studies will hopefully provide the information to gather this information and to determine the value of NFC in glaucoma.
Citation:
Philip S, Najafi A, Tantraworasin A, Pasquale LR, Ritch R. Nailfold Capillaroscopy of Resting Peripheral Blood Flow in Exfoliation Glaucoma and Primary Open-Angle Glaucoma. JAMA Ophthalmol. 2019;137(6):618–625. doi:https://doi.org/10.1001/jamaophthalmol.2019.0434
[subscribe]
Last Modified: [last-modified]
The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.
Last Updated on December 15, 2019 by Marie Benz MD FAAD
