MedicalResearch.com Interview with:
Rachel Slayton PhD
National Center for Emerging and Zoonotic Infectious Diseases
CDC
Medical Research: What is the background for this study? What are the main findings?
Dr. Slayton: Antibiotic-resistant bacteria cause more than 2 million illnesses and at least 23,000 deaths each year in the US. Additionally,
Clostridium difficile caused close to half a million illnesses in 2011, and an estimated 15,000 deaths a year are attributable to
C. difficile infections. Antibiotic resistance is a regional problem with inter-facility spread through movement of patients who are colonized or infected with these organisms.
In our first analysis we projected the national incidence of infections and deaths from Carbapenem-resistant
Enterobacteriaceae (CRE),
Clostridium difficile, invasive methicillin-resistant
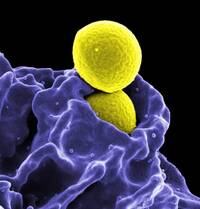
Staphylococcus aureus (MRSA), and multidrug-resistant
Pseudomonas aeruginosa. With immediate implementation of national interventions combining infection control and antibiotic stewardship and, assuming similar effectiveness to that reported in other countries, an estimated 619,000 health care–associated infections and 37,000 deaths could be averted over 5 years.
Using CRE as an exemplar, we also estimated the effect of a coordinated approach in a network for the preventing the spread of antibiotic-resistance organisms among healthcare facilities that share patients. Our Carbapenem-resistant
Enterobacteriaceae modeling was done in collaboration with Johns Hopkins Bloomberg School of Public Health, the University of Utah, and University of California Irvine School of Medicine. Both models clearly show that we could see fewer antibiotic-resistant infections if health care facilities and public health officials work together as a team. For example, five years after
Carbapenem-resistant Enterobacteriaceae enters an area with 10 facilities that share patients, baseline activity alone resulted a prevalence of healthcare-associated CRE infection or colonization of 12.2% with 2,141 patients acquiring CRE. With independent facility-augmented efforts, we estimated that there would be an 8.6% prevalence with 1,590 patients acquiring Carbapenem-resistant
Enterobacteriaceae. With a coordinated augmented approach, we estimated that there would be a 2.1% prevalence with 406 patients acquiring CRE. Using a 102-facility model of Orange County, California, we estimated that over 15 years countywide 19,271 patient acquisitions could be prevented with the coordinated augmented approach compared with independent-facility efforts.




 Dr. Andreas Bäumler[/caption]
Andreas J. Bäumler, Ph.D
Editor, Infection and Immunity
Associate Editor, PLOS Pathogens
Section Editor, EcoSal Plus
Professor, Department of Medical Microbiology and Immunology
Vice Chair of Research
University of California, Davis School of Medicine
Davis, California
MedicalResearch.com: What is the background for this study? What are the main findings?
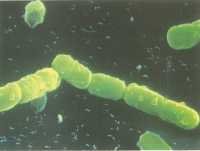
Dr. Bäumler: Antibiotics are generally beneficial for treating bacterial infection, but paradoxically a history of antibiotic therapy is a risk factor for developing Salmonella food poisoning. Our study reveals the mechanism by which antibiotics increase susceptibility to Salmonella infection.
Antibiotics deplete beneficial microbes from the gut, which normally provide nutrition to the cells lining our large bowel, termed epithelial cells. Depletion of microbe-derived nutrients causes our epithelial cells to switch their energy metabolism from respiration to fermentation, which in turn increases the availability of oxygen at the epithelial surface. The resulting increase in oxygen diffusion into the gut lumen drives a luminal expansion of Salmonella by respiration. Through this mechanism, antibiotics help Salmonella to breath in the gut.
Dr. Andreas Bäumler[/caption]
Andreas J. Bäumler, Ph.D
Editor, Infection and Immunity
Associate Editor, PLOS Pathogens
Section Editor, EcoSal Plus
Professor, Department of Medical Microbiology and Immunology
Vice Chair of Research
University of California, Davis School of Medicine
Davis, California
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Bäumler: Antibiotics are generally beneficial for treating bacterial infection, but paradoxically a history of antibiotic therapy is a risk factor for developing Salmonella food poisoning. Our study reveals the mechanism by which antibiotics increase susceptibility to Salmonella infection.
Antibiotics deplete beneficial microbes from the gut, which normally provide nutrition to the cells lining our large bowel, termed epithelial cells. Depletion of microbe-derived nutrients causes our epithelial cells to switch their energy metabolism from respiration to fermentation, which in turn increases the availability of oxygen at the epithelial surface. The resulting increase in oxygen diffusion into the gut lumen drives a luminal expansion of Salmonella by respiration. Through this mechanism, antibiotics help Salmonella to breath in the gut.











