MedicalResearch.com Interview with:
[caption id="attachment_39890" align="alignleft" width="130"]
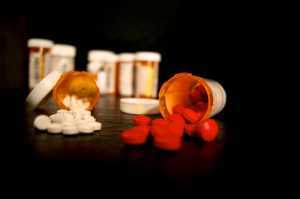
 michigan dispensaries
michigan dispensaries and other dispensaries across America are critical to reduce opioid-related overdoses and substance abuse. We also found evidence that more recently-adopting states have experienced smaller reductions in overdoses and opioid substance abuse, potentially because the more recent adopters tend to enforce more stringent guidelines for dispensaries than the early adopters. MedicalResearch.com: What should readers take away from your report? Response: We find that the introduction of medical marijuana dispensaries has the potential to reduce opioid-related harms quite significantly. More broadly, it also suggests that, when we think about the opioid crisis, improving access to pain management alternatives may be a useful mechanism for reducing dependence on opioids. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: During most of the time period that we studied, prescription opioids were driving the opioid crisis, but it has recently transitioned to the point where heroin and illicit synthetic opioids are playing more prominent roles. We are hesitant to suggest that medical marijuana access will have the same scope in a climate in which synthetic opioids and heroin are the primary substances of abuse. Future work could do more to explore the potential of different types of medical marijuana laws to reduce overdoses related to these substances. Citations: Do medical marijuana laws reduce addictions and deaths related to pain killers? ? •David Powella, , , • Rosalie Liccardo Paculaa, b, Mireille Jacobsonb RAND, Santa Monica, United States NBER Cambridge, MA, United StatesUniversity of California, Irvine, United States Received 14 November 2015, Revised 15 August 2017, Accepted 30 December 2017, Available online 3 February 2018 Journal of Health Economics Volume 58, March 2018, Pages 29–42 https://doi.org/10.1016/j.jhealeco.2017.12.007 [wysija_form id="3"] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website." width="130" height="150" /> Dr. Powell[/caption]
David Powell PhD
Economist; Core Faculty, Pardee RAND Graduate School
RAND, Santa Monica
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There has been some research suggesting that the adoption of state medical marijuana laws leads to reductions in prescriptions for opioid analgesics among certain populations and opioid-related overdoses overall. However, medical marijuana laws are very different across states and they have changed over time as well. We wanted to understand what components of a medical marijuana law could potentially lead to reductions in overdoses and substance abuse. We focused specifically on the role of dispensaries, given their importance in providing access to medical marijuana, and tested for different effects in states with and without legally-protected and operational dispensaries.
We found that dispensaries are critical to reduce opioid-related overdoses and substance abuse. We also found evidence that more recently-adopting states have experienced smaller reductions in overdoses and opioid substance abuse, potentially because the more recent adopters tend to enforce more stringent guidelines for dispensaries than the early adopters.
 Fentanyl addiction and overdose rates are mounting public health challenges linked to opioid use disorder across the United States. Effective treatment programs for recovery are essential to address these concerns, especially as access to both in-person and virtual options improves. Renew Health Addiction Recovery Services delivers evidence-based care and supports individuals seeking help for substance abuse addiction throughout New Mexico.
Fentanyl is a potent synthetic opioid responsible for rising overdose deaths and severe complications among people with substance use disorder. Reaching effective recovery remains difficult for many due to barriers such as stigma, provider shortages, and the geographic spread of rural populations. Organizations like Renew Health Addiction Recovery Services are working to overcome these obstacles by offering accessible, evidence-based addiction care through various treatment options. Renew Health Addiction Recovery Services is a leading drug and alcohol addiction treatment center in New Mexico, providing in-person and online outpatient rehab, plus local clinics in Roswell, Alamogordo, and Clovis. Their programs address opioid, alcohol, methamphetamine, and cocaine addiction, offering medical detoxification, medication-assisted treatment (MAT), mental health services, and ongoing recovery support.
Fentanyl addiction and overdose rates are mounting public health challenges linked to opioid use disorder across the United States. Effective treatment programs for recovery are essential to address these concerns, especially as access to both in-person and virtual options improves. Renew Health Addiction Recovery Services delivers evidence-based care and supports individuals seeking help for substance abuse addiction throughout New Mexico.
Fentanyl is a potent synthetic opioid responsible for rising overdose deaths and severe complications among people with substance use disorder. Reaching effective recovery remains difficult for many due to barriers such as stigma, provider shortages, and the geographic spread of rural populations. Organizations like Renew Health Addiction Recovery Services are working to overcome these obstacles by offering accessible, evidence-based addiction care through various treatment options. Renew Health Addiction Recovery Services is a leading drug and alcohol addiction treatment center in New Mexico, providing in-person and online outpatient rehab, plus local clinics in Roswell, Alamogordo, and Clovis. Their programs address opioid, alcohol, methamphetamine, and cocaine addiction, offering medical detoxification, medication-assisted treatment (MAT), mental health services, and ongoing recovery support.

 Dr. D'Orsogna[/caption]
Maria-Rita D'Orsogna Ph.D.
Professor, Mathematics
California State University, Northridge
Adjunct Associate Professor
Department of Computational Medicine at UCLA
MedicalResearch.com: What is the background for this study?
Response: Drug overdose deaths have been increasing in the USA for the past two decades. A ‘third wave’ of overdose fatalities started in 2013, with a shift from prescription opioids towards synthetic ones, in particular illicit fentanyl.
To examine trends in drug overdose deaths by gender, race and geography in the United States during the period 2013-2020, we used an epidemiological database provided by the Centers for Disease Control and Prevention, extracting rates by race and gender in all 50 states plus the District of Columbia. We considered the impact of four main drug categories psychostimulants with addiction potential such as methamphetamines; heroin; prescription opioids and synthetic opioids such as fentanyl and its derivatives.
Dr. D'Orsogna[/caption]
Maria-Rita D'Orsogna Ph.D.
Professor, Mathematics
California State University, Northridge
Adjunct Associate Professor
Department of Computational Medicine at UCLA
MedicalResearch.com: What is the background for this study?
Response: Drug overdose deaths have been increasing in the USA for the past two decades. A ‘third wave’ of overdose fatalities started in 2013, with a shift from prescription opioids towards synthetic ones, in particular illicit fentanyl.
To examine trends in drug overdose deaths by gender, race and geography in the United States during the period 2013-2020, we used an epidemiological database provided by the Centers for Disease Control and Prevention, extracting rates by race and gender in all 50 states plus the District of Columbia. We considered the impact of four main drug categories psychostimulants with addiction potential such as methamphetamines; heroin; prescription opioids and synthetic opioids such as fentanyl and its derivatives.


 Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.
Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.
 Dr. O'Donnell[/caption]
Julie O’Donnell, PhD MPH
Division of Overdose Prevention
National Center for Injury Prevention and Control
CDC
National Network of Public Health Institutes
New Orleans, Louisiana
MedicalResearch.com: What is the background for this study?
Response: The estimated number of drug overdose deaths in the US surpassed 100,000 over a 12-month period for the first time during May 2020-April 2021, driven by the involvement of synthetic opioids other than methadone (mainly illicitly manufactured fentanyl (IMF)), according to data from the National Vital Statistics System.
The State Unintentional Drug Overdose Reporting System (SUDORS) is a CDC-funded surveillance program that has collected detailed data on unintentional and undetermined intent drug overdose deaths since 2016 from death certificates, medical examiner and coroner reports, and full postmortem toxicology reports. SUDORS data allow for the analysis specifically of deaths involving fentanyl (rather than the larger category of synthetic opioids), and contain information about decedent demographics and other characteristics, as well as circumstances surrounding the overdose that might help inform prevention.
Dr. O'Donnell[/caption]
Julie O’Donnell, PhD MPH
Division of Overdose Prevention
National Center for Injury Prevention and Control
CDC
National Network of Public Health Institutes
New Orleans, Louisiana
MedicalResearch.com: What is the background for this study?
Response: The estimated number of drug overdose deaths in the US surpassed 100,000 over a 12-month period for the first time during May 2020-April 2021, driven by the involvement of synthetic opioids other than methadone (mainly illicitly manufactured fentanyl (IMF)), according to data from the National Vital Statistics System.
The State Unintentional Drug Overdose Reporting System (SUDORS) is a CDC-funded surveillance program that has collected detailed data on unintentional and undetermined intent drug overdose deaths since 2016 from death certificates, medical examiner and coroner reports, and full postmortem toxicology reports. SUDORS data allow for the analysis specifically of deaths involving fentanyl (rather than the larger category of synthetic opioids), and contain information about decedent demographics and other characteristics, as well as circumstances surrounding the overdose that might help inform prevention.








 michigan dispensaries
michigan dispensaries