Author Interviews, CMAJ, Cost of Health Care / 25.09.2018
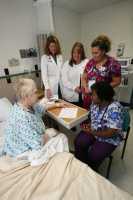
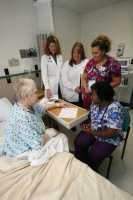
Who Has the Highest Rate of Readmission After Hospital Discharge?
MedicalResearch.com Interview with:
 Andrea Gruneir, PhD
Department of Family Medicine
University of Alberta
Edmonton, AB Canada
MedicalResearch.com: What is the background for this study?
Response: Hospital readmissions – when a patient is discharged from hospital but then returns to hospital in a short period of time – are known to be a problem, both for the patients and for the larger health system. Hospital readmissions have received considerable attention and there have been a number of initiatives to try to reduce them, but with mixed success. Older adults are among the most vulnerable group for hospital readmission. Older adults are also the largest users of continuing care services, such as home care and long-term care homes (also known as nursing homes). Yet, few large studies have really considered how older adults with different pathways through hospital compare on the risk of hospital readmission.
In our study, we take a population-level approach and use health administrative data to create a large cohort of older adults who were hospitalized in Ontario between 2008 and 2015. For each of the 701,527 patients in our study, we identified where they received care before the hospitalization (in the community or in long-term care) and where they received care after discharge (in the community, in the community with home care, or in long-term care).
Andrea Gruneir, PhD
Department of Family Medicine
University of Alberta
Edmonton, AB Canada
MedicalResearch.com: What is the background for this study?
Response: Hospital readmissions – when a patient is discharged from hospital but then returns to hospital in a short period of time – are known to be a problem, both for the patients and for the larger health system. Hospital readmissions have received considerable attention and there have been a number of initiatives to try to reduce them, but with mixed success. Older adults are among the most vulnerable group for hospital readmission. Older adults are also the largest users of continuing care services, such as home care and long-term care homes (also known as nursing homes). Yet, few large studies have really considered how older adults with different pathways through hospital compare on the risk of hospital readmission.
In our study, we take a population-level approach and use health administrative data to create a large cohort of older adults who were hospitalized in Ontario between 2008 and 2015. For each of the 701,527 patients in our study, we identified where they received care before the hospitalization (in the community or in long-term care) and where they received care after discharge (in the community, in the community with home care, or in long-term care).
 Andrea Gruneir, PhD
Department of Family Medicine
University of Alberta
Edmonton, AB Canada
MedicalResearch.com: What is the background for this study?
Response: Hospital readmissions – when a patient is discharged from hospital but then returns to hospital in a short period of time – are known to be a problem, both for the patients and for the larger health system. Hospital readmissions have received considerable attention and there have been a number of initiatives to try to reduce them, but with mixed success. Older adults are among the most vulnerable group for hospital readmission. Older adults are also the largest users of continuing care services, such as home care and long-term care homes (also known as nursing homes). Yet, few large studies have really considered how older adults with different pathways through hospital compare on the risk of hospital readmission.
In our study, we take a population-level approach and use health administrative data to create a large cohort of older adults who were hospitalized in Ontario between 2008 and 2015. For each of the 701,527 patients in our study, we identified where they received care before the hospitalization (in the community or in long-term care) and where they received care after discharge (in the community, in the community with home care, or in long-term care).
Andrea Gruneir, PhD
Department of Family Medicine
University of Alberta
Edmonton, AB Canada
MedicalResearch.com: What is the background for this study?
Response: Hospital readmissions – when a patient is discharged from hospital but then returns to hospital in a short period of time – are known to be a problem, both for the patients and for the larger health system. Hospital readmissions have received considerable attention and there have been a number of initiatives to try to reduce them, but with mixed success. Older adults are among the most vulnerable group for hospital readmission. Older adults are also the largest users of continuing care services, such as home care and long-term care homes (also known as nursing homes). Yet, few large studies have really considered how older adults with different pathways through hospital compare on the risk of hospital readmission.
In our study, we take a population-level approach and use health administrative data to create a large cohort of older adults who were hospitalized in Ontario between 2008 and 2015. For each of the 701,527 patients in our study, we identified where they received care before the hospitalization (in the community or in long-term care) and where they received care after discharge (in the community, in the community with home care, or in long-term care).