[caption id="attachment_20847" align="alignleft" width="130"]

Dr. Marita Teng[/caption]
MedicalResearch.com Interview with:
Marita Teng, MD
Associate Professor of Otolaryngology
Head and Neck Institute
Icahn School of Medicine at Mount Sinai
MedicalResearch.com Editor's note: January is Thyroid Awareness Month. In recognition, Dr. Teng discusses the thyroid gland's important role in the production of hormones that help the body regulate its metabolism. Dr. Teng also discusses the recognition of thyroid nodules and cancer.
MedicalResearch: What does the thyroid gland do? Why is it important for health?
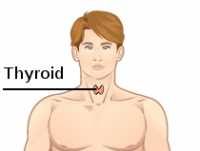
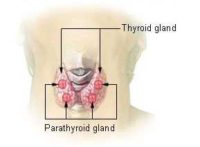
Dr. Teng: The thyroid gland produces thyroid hormone, which is carried through the circulation to the other organs in the body. Thyroid hormone is responsible for the body’s metabolism, and therefore maintains functions such as keeping the body warm, and properly use the energy we derive from food.
MedicalResearch: What is are some signs or symptoms of an underactive or overactive thyroid?
Dr. Teng: Thyroid overactivity (hyperactivity) results in heat intolerance, weight loss, rapid heartbeat, nervousness, increased appetite, difficulty sleeping, skin thinning, and hair loss, among other symptoms. Thyroid underactivity (hypothyroidism) causes fatigue, weight gain, cold sensitivity, slowed heart rate, depression, memory impairment, and weakness, among other symptoms. It should be noted that these symptoms are all nonspecific and can certainly be caused by other medical conditions as well.





















 Dr. Marita Teng[/caption]
MedicalResearch.com Interview with:
Marita Teng, MD
Associate Professor of Otolaryngology
Head and Neck Institute
Icahn School of Medicine at Mount Sinai
MedicalResearch.com Editor's note: January is Thyroid Awareness Month. In recognition, Dr. Teng discusses the thyroid gland's important role in the production of hormones that help the body regulate its metabolism. Dr. Teng also discusses the recognition of thyroid nodules and cancer.
MedicalResearch: What does the thyroid gland do? Why is it important for health?
Dr. Teng: The thyroid gland produces thyroid hormone, which is carried through the circulation to the other organs in the body. Thyroid hormone is responsible for the body’s metabolism, and therefore maintains functions such as keeping the body warm, and properly use the energy we derive from food.
MedicalResearch: What is are some signs or symptoms of an underactive or overactive thyroid?
Dr. Teng: Thyroid overactivity (hyperactivity) results in heat intolerance, weight loss, rapid heartbeat, nervousness, increased appetite, difficulty sleeping, skin thinning, and hair loss, among other symptoms. Thyroid underactivity (hypothyroidism) causes fatigue, weight gain, cold sensitivity, slowed heart rate, depression, memory impairment, and weakness, among other symptoms. It should be noted that these symptoms are all nonspecific and can certainly be caused by other medical conditions as well.
Dr. Marita Teng[/caption]
MedicalResearch.com Interview with:
Marita Teng, MD
Associate Professor of Otolaryngology
Head and Neck Institute
Icahn School of Medicine at Mount Sinai
MedicalResearch.com Editor's note: January is Thyroid Awareness Month. In recognition, Dr. Teng discusses the thyroid gland's important role in the production of hormones that help the body regulate its metabolism. Dr. Teng also discusses the recognition of thyroid nodules and cancer.
MedicalResearch: What does the thyroid gland do? Why is it important for health?
Dr. Teng: The thyroid gland produces thyroid hormone, which is carried through the circulation to the other organs in the body. Thyroid hormone is responsible for the body’s metabolism, and therefore maintains functions such as keeping the body warm, and properly use the energy we derive from food.
MedicalResearch: What is are some signs or symptoms of an underactive or overactive thyroid?
Dr. Teng: Thyroid overactivity (hyperactivity) results in heat intolerance, weight loss, rapid heartbeat, nervousness, increased appetite, difficulty sleeping, skin thinning, and hair loss, among other symptoms. Thyroid underactivity (hypothyroidism) causes fatigue, weight gain, cold sensitivity, slowed heart rate, depression, memory impairment, and weakness, among other symptoms. It should be noted that these symptoms are all nonspecific and can certainly be caused by other medical conditions as well.



