Allergies, Author Interviews, OBGYNE, Pediatrics / 22.12.2020
Drinking MilK During Breast Feeding May Protect Children From Food Allergy
MedicalResearch.com Interview with:
Mia Stråvik
PhD-student | Doktorand
Department of Biology and Biological Engineering
Division of Food and Nutrition Science
Chalmers University of Technology
MedicalResearch.com: What is the background for this study?
Response: There is a need of research investigating the role of maternal diet during pregnancy and lactation on the baby’s allergy risk. Allergy is one of the most common chronic diseases of childhood, causing great suffering for the allergic child but also the entire family. Yet, the possibilities to cure and prevent this, in many cases life long, suffering are very limited. Previous research have indicated that maternal diet during pregnancy and lactation may affect the propensity of the child to develop an allergy, and diet is a factor you as a parent really can influence.


 Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study
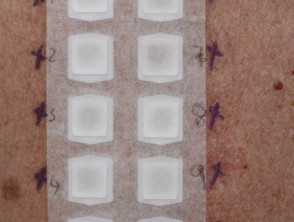
Response: Chronic hand eczema was previously shown to be associated with higher rates of allergic contact dermatitis. Yet, little is known about recent trends in North America with respect to the clinical presentation and allergen profile in chronic hand eczema. This study sought to determine the clinical characteristics and etiologies of hand eczema in a large North American cohort of adults referred for patch testing. The patients in the study were patch tested using the North American Contact Dermatitis Group’s allergen screening series.
Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study
Response: Chronic hand eczema was previously shown to be associated with higher rates of allergic contact dermatitis. Yet, little is known about recent trends in North America with respect to the clinical presentation and allergen profile in chronic hand eczema. This study sought to determine the clinical characteristics and etiologies of hand eczema in a large North American cohort of adults referred for patch testing. The patients in the study were patch tested using the North American Contact Dermatitis Group’s allergen screening series.
 Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.
Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.


 Melanie Leung[/caption]
Melanie Leung, M.D.,C.M. candidate 2021
4th-year medical student at McGill University
Division of Allergy and Clinical Immunology
Department of Pediatrics, Montreal Children’s Hospital
McGill University Health Centre, Montreal, QC, Canada
Dr. Moshe Ben-Shoshan, MD, MSc
Pediatric allergist and immunologist at the MCH (Montreal Children’s Hospital) and
Scientist at the Research Institute of the MUHC (McGill University Health Center)
MedicalResearch.com: What is the background for this study?
Response: In Canada, up to 9% of children have at least 1 food allergy. Anaphylaxis is the most severe and potential life-threatening manifestation of food allergy. Peanuts and tree nuts are the main culprits in food-induced anaphylaxis and account for most fatal cases in North America.
Public awareness about peanut and nut anaphylaxis can help to prevent and to act promptly, in the case of anaphylactic reaction. However, the best timing for public awareness campaigns remained unknown, as no previous study looked at the potential association between specific times of the year, such as public holidays, and the incidence of peanut and tree nut anaphylaxis. Our aim was to evaluate the risk of peanut and tree nut-induced anaphylaxis on Halloween, Christmas, Easter, Diwali, Chinese New Year, and Eid al-Adha.
Data was collected from 1390 pediatric cases of peanut or nut-induced anaphylaxis across Canada (Newfoundland & Labrador, Quebec, Ontario, and British Columbia), from 2011 to 2020. 62% of children were boys and the median age was 5.4 years. We compared the average daily number of cases during each holiday and compared it to the rest of the year (i.e.: non-holiday period).
Melanie Leung[/caption]
Melanie Leung, M.D.,C.M. candidate 2021
4th-year medical student at McGill University
Division of Allergy and Clinical Immunology
Department of Pediatrics, Montreal Children’s Hospital
McGill University Health Centre, Montreal, QC, Canada
Dr. Moshe Ben-Shoshan, MD, MSc
Pediatric allergist and immunologist at the MCH (Montreal Children’s Hospital) and
Scientist at the Research Institute of the MUHC (McGill University Health Center)
MedicalResearch.com: What is the background for this study?
Response: In Canada, up to 9% of children have at least 1 food allergy. Anaphylaxis is the most severe and potential life-threatening manifestation of food allergy. Peanuts and tree nuts are the main culprits in food-induced anaphylaxis and account for most fatal cases in North America.
Public awareness about peanut and nut anaphylaxis can help to prevent and to act promptly, in the case of anaphylactic reaction. However, the best timing for public awareness campaigns remained unknown, as no previous study looked at the potential association between specific times of the year, such as public holidays, and the incidence of peanut and tree nut anaphylaxis. Our aim was to evaluate the risk of peanut and tree nut-induced anaphylaxis on Halloween, Christmas, Easter, Diwali, Chinese New Year, and Eid al-Adha.
Data was collected from 1390 pediatric cases of peanut or nut-induced anaphylaxis across Canada (Newfoundland & Labrador, Quebec, Ontario, and British Columbia), from 2011 to 2020. 62% of children were boys and the median age was 5.4 years. We compared the average daily number of cases during each holiday and compared it to the rest of the year (i.e.: non-holiday period).
 Alyssa M. Thompson[/caption]
Alyssa M. Thompson is currently a 2nd year medical student at the UA-COM Tucson. She graduated from the University of Arizona, Summa Cum Laude in 2018 as the athletic department's Valedictorian with a degree in Physiology and an Entrepreneurship certificate. Her passion for research and dermatology stems from her innovative and integrative mindset with specific interest in inflammatory skin disease.
MedicalResearch.com: What is the background for this study?
Response: Eczema is very common in children. Prescription medications are important for managing eczema flares, but a lot of the work in treating eczema is preventative, done by consistently moisturizing the skin at home with drug store products. Allergic contact dermatitis occurs more commonly in people with eczema. A previous study was done in characterizing the allergenic potential of drug-store moisturizers and found that 88% of moisturizers contain at least one common allergen. Many moisturizers are marketed specifically to eczema, but the allergen content of these products are unknown.
Alyssa M. Thompson[/caption]
Alyssa M. Thompson is currently a 2nd year medical student at the UA-COM Tucson. She graduated from the University of Arizona, Summa Cum Laude in 2018 as the athletic department's Valedictorian with a degree in Physiology and an Entrepreneurship certificate. Her passion for research and dermatology stems from her innovative and integrative mindset with specific interest in inflammatory skin disease.
MedicalResearch.com: What is the background for this study?
Response: Eczema is very common in children. Prescription medications are important for managing eczema flares, but a lot of the work in treating eczema is preventative, done by consistently moisturizing the skin at home with drug store products. Allergic contact dermatitis occurs more commonly in people with eczema. A previous study was done in characterizing the allergenic potential of drug-store moisturizers and found that 88% of moisturizers contain at least one common allergen. Many moisturizers are marketed specifically to eczema, but the allergen content of these products are unknown.

 Dr. Perrett[/caption]
Kirsten P Perrett MD PhD
Group Leader/Clinician Scientist Fellow
Population Allergy Research Group and
Melbourne Children's Trial Centre
Murdoch Children's Research Institute
Rachel L Peters PhD
Murdoch Children’s Research Institute
Department of Paediatrics
The University of Melbourne
Parkville, Australia
MedicalResearch.com: What is the background for this study?
Dr. Perrett[/caption]
Kirsten P Perrett MD PhD
Group Leader/Clinician Scientist Fellow
Population Allergy Research Group and
Melbourne Children's Trial Centre
Murdoch Children's Research Institute
Rachel L Peters PhD
Murdoch Children’s Research Institute
Department of Paediatrics
The University of Melbourne
Parkville, Australia
MedicalResearch.com: What is the background for this study?











 Dr. Shaker[/caption]
Marcus S. Shaker, MD
Associate Professor of Pediatrics
Associate Professor of Community and Family Medicine
Dartmouth-Hitchcock Medical Center
MedicalResearch.com: What is the background for this study?
Response: There are two peanut allergy treatments that are being evaluated for potential FDA approval—an orally administered treatment and an epicutaneous (skin based) treatment. Both have tremendous potential benefit. The focus of our study was to explore the range of health and economic benefits in terms of establishing pathways for how each therapy could be cost effective.
We want to be clear that our purpose was not to suggest one therapy is or is not cost effective at present. That would be a ridiculous statement to make regarding two treatments that not only lack FDA approval, but do not have established pricing. Rather, we used preliminary inputs that are presently available to create as robust a model as we could to better determine the individual paths that would make them more or less cost-effective.
Dr. Shaker[/caption]
Marcus S. Shaker, MD
Associate Professor of Pediatrics
Associate Professor of Community and Family Medicine
Dartmouth-Hitchcock Medical Center
MedicalResearch.com: What is the background for this study?
Response: There are two peanut allergy treatments that are being evaluated for potential FDA approval—an orally administered treatment and an epicutaneous (skin based) treatment. Both have tremendous potential benefit. The focus of our study was to explore the range of health and economic benefits in terms of establishing pathways for how each therapy could be cost effective.
We want to be clear that our purpose was not to suggest one therapy is or is not cost effective at present. That would be a ridiculous statement to make regarding two treatments that not only lack FDA approval, but do not have established pricing. Rather, we used preliminary inputs that are presently available to create as robust a model as we could to better determine the individual paths that would make them more or less cost-effective.



 Dr. Reker[/caption]
Daniel Reker, PhD
Koch Institute for Integrative Cancer Research
Massachusetts Institute of Technology
MedicalResearch.com: What is the background for this study?
Response: We started thinking more about this topic following a clinical experience five years ago that Dr. Traverso was involved in where a patient suffering form Celiac disease received a prescription of a drug which potentially had gluten. This experience really opened our eyes for how little we knew about the inactive ingredients and how clinical workflows do not currently accommodate for such scenarios.
We therefore set up a large scale analysis to better understand the complexity of the inactive ingredient portion in a medication as well as how frequently critical ingredients are included that could potential affect sensitive patients.
Dr. Reker[/caption]
Daniel Reker, PhD
Koch Institute for Integrative Cancer Research
Massachusetts Institute of Technology
MedicalResearch.com: What is the background for this study?
Response: We started thinking more about this topic following a clinical experience five years ago that Dr. Traverso was involved in where a patient suffering form Celiac disease received a prescription of a drug which potentially had gluten. This experience really opened our eyes for how little we knew about the inactive ingredients and how clinical workflows do not currently accommodate for such scenarios.
We therefore set up a large scale analysis to better understand the complexity of the inactive ingredient portion in a medication as well as how frequently critical ingredients are included that could potential affect sensitive patients.




 Dr. Shenoy[/caption]
ESS= Erica S. Shenoy, MD, PhD
Harvard Medical School
Division of Infectious Diseases, Department of Medicine
Massachusetts General Hospital, Boston
[caption id="attachment_47011" align="alignleft" width="150"]
Dr. Shenoy[/caption]
ESS= Erica S. Shenoy, MD, PhD
Harvard Medical School
Division of Infectious Diseases, Department of Medicine
Massachusetts General Hospital, Boston
[caption id="attachment_47011" align="alignleft" width="150"] Dr. Blumenthal[/caption]
KGB= Kimberly G. Blumenthal MD, MSc
Division of Rheumatology, Allergy and Immunology
Department of Medicine, Massachusetts General Hospital,Boston
[caption id="attachment_47012" align="alignleft" width="100"]
Dr. Blumenthal[/caption]
KGB= Kimberly G. Blumenthal MD, MSc
Division of Rheumatology, Allergy and Immunology
Department of Medicine, Massachusetts General Hospital,Boston
[caption id="attachment_47012" align="alignleft" width="100"] Dr. Macy[/caption]
EMM= Eric M. Macy MD, MS
Department of Allergy
Southern California Permanente Medical Group
San Diego Medical Center
[caption id="attachment_47013" align="alignleft" width="150"]
Dr. Macy[/caption]
EMM= Eric M. Macy MD, MS
Department of Allergy
Southern California Permanente Medical Group
San Diego Medical Center
[caption id="attachment_47013" align="alignleft" width="150"] Dr. Rowe[/caption]
TR= Theresa Rowe, DO, MS
General Internal Medicine and Geriatrics
Feinberg School of Medicine
Northwestern University, Chicago, Illinois
MedicalResearch.com: What is the background for this review?
ESS: A key component of reducing antimicrobial resistance is improving how antimicrobials are prescribed—both reducing inappropriate use (i.e., not prescribing when not needed) and favoring the use of narrow-spectrum agents that are less likely to contribute to the development of antimicrobial resistance.
KGB: Because unverified penicillin allergy labels are so prevalent with greater than 32 million Americans affected, and these labels lead to the use of alternative antibiotics that are often more broad-spectrum, we now know that penicillin allergy evaluations are an emerging important component of antibiotic stewardship. When patients with a reported penicillin allergy are tested, more than 95% of them are not allergic, and thus could (and should) receive penicillins, and often related drugs, when appropriate.
Dr. Rowe[/caption]
TR= Theresa Rowe, DO, MS
General Internal Medicine and Geriatrics
Feinberg School of Medicine
Northwestern University, Chicago, Illinois
MedicalResearch.com: What is the background for this review?
ESS: A key component of reducing antimicrobial resistance is improving how antimicrobials are prescribed—both reducing inappropriate use (i.e., not prescribing when not needed) and favoring the use of narrow-spectrum agents that are less likely to contribute to the development of antimicrobial resistance.
KGB: Because unverified penicillin allergy labels are so prevalent with greater than 32 million Americans affected, and these labels lead to the use of alternative antibiotics that are often more broad-spectrum, we now know that penicillin allergy evaluations are an emerging important component of antibiotic stewardship. When patients with a reported penicillin allergy are tested, more than 95% of them are not allergic, and thus could (and should) receive penicillins, and often related drugs, when appropriate.



 Eliane Abou-Jaoude, MD
Allergy and Immunology Fellow
Henry Ford Health System
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Early life exposure to diverse types of microbes is necessary for healthy immune development and may impact the risk for developing allergic disorders.
Theoretically the transfer of parental microbes to their offspring during infancy can influence a child’s developing gut microbiome and subsequent immune response patterns.
We wished to investigate whether parental pacifier cleaning methods, reported at 6-months of age, were associated with altered serum IgE trajectory over the first 18 months of life.
Eliane Abou-Jaoude, MD
Allergy and Immunology Fellow
Henry Ford Health System
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Early life exposure to diverse types of microbes is necessary for healthy immune development and may impact the risk for developing allergic disorders.
Theoretically the transfer of parental microbes to their offspring during infancy can influence a child’s developing gut microbiome and subsequent immune response patterns.
We wished to investigate whether parental pacifier cleaning methods, reported at 6-months of age, were associated with altered serum IgE trajectory over the first 18 months of life.

