MedicalResearch.com Interview with:
Vincent Guilamo-Ramos, PhD
MPH, LCSW, RN, ANP-BC, PMHNP-BC, AAHIVS, FAAN
[caption id="attachment_57914" align="alignleft" width="200"]

Dr. Guilamo-Ramos[/caption]
Vincent Guilamo-Ramos is dean and professor at the Duke University School of Nursing, vice chancellor for nursing affairs, Duke University, and director of the Center for Latino Adolescent and Family Health (CLAFH) at Duke.
Dr. Guilamo-Ramos served as a member of the National Academies of Sciences, Engineering, and Medicine (National Academies) Committee on Prevention and Control of STIs in the U.S. that wrote the recent consensus study report. He also serves as a member of the Presidential Advisory Council on HIV/AIDS (PACHA) and the HHS Panel on Antiretroviral Guidelines for Adults and Adolescents.
MedicalResearch.com: What is the background for this study?
Response: The National Academies of Sciences, Engineering, and Medicine (National Academies) recently released a consensus study report on prevention and control of sexually transmitted infections (STIs) in the United States. The report entitled “Sexually Transmitted Infections: Adopting a Sexual Health Paradigm” includes a strong emphasis on adolescents and young adults as an important priority population for the response to record-level STI rates that have reached an all-time high for the sixth year in a row in 2019. The report also highlights the well-supported and crucial role of parents in addressing STIs and promoting sexual health among adolescents and young adults. In
this new Viewpoint article, my co-authors and I, who contributed to the National Academies report as committee members or consultants, discuss the practical implications for health care professionals of engaging parents in adolescent sexual health services.


 Dr. Stevermer [/caption]
James Stevermer, M.D., M.S.P.H.Vice chair for clinical affairs
Professor of family and community medicine
University of Missouri
Medical director of MU Health Care Family Medicine–Callaway Physicians,
Dr. Stevermer joined the U.S. Preventive Service Task Force in January 2021.
MedicalResearch.com: What is the background for this study?
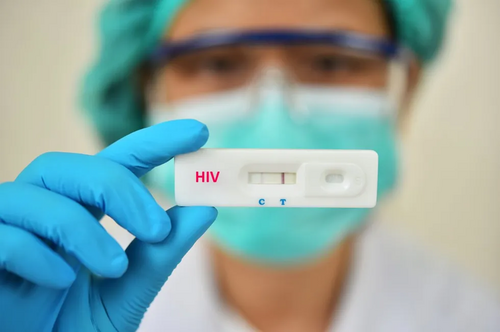
Response: HIV continues to be a significant public health issue. The good news is that PrEP is a safe, highly effective way to help prevent HIV in people at increased risk. There are now two ways people can take PrEP – as a pill or as a shot. We encourage healthcare professionals to have a conversation with their patients about their individual risk for HIV and determine if they should consider taking whichever form of PrEP would work best for them.
Dr. Stevermer [/caption]
James Stevermer, M.D., M.S.P.H.Vice chair for clinical affairs
Professor of family and community medicine
University of Missouri
Medical director of MU Health Care Family Medicine–Callaway Physicians,
Dr. Stevermer joined the U.S. Preventive Service Task Force in January 2021.
MedicalResearch.com: What is the background for this study?
Response: HIV continues to be a significant public health issue. The good news is that PrEP is a safe, highly effective way to help prevent HIV in people at increased risk. There are now two ways people can take PrEP – as a pill or as a shot. We encourage healthcare professionals to have a conversation with their patients about their individual risk for HIV and determine if they should consider taking whichever form of PrEP would work best for them.

 Dr. Gandhi[/caption]
Manoj Gandhi, MD PhD
Senior Medical Director of Genetic Testing Services,
Dr. Gandhi[/caption]
Manoj Gandhi, MD PhD
Senior Medical Director of Genetic Testing Services, 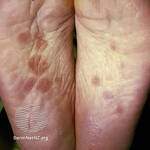
 Dr. Ogedegbe[/caption]
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
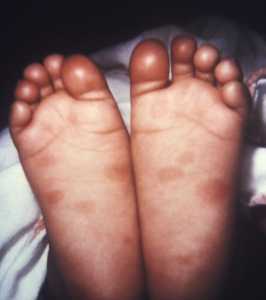
Response: Syphilis has become more common over the past 20 years, after reaching a record low in 2000. The Task Force found that screening people who are at increased risk for syphilis can identify the infection early so it can be treated before problems develop. For that reason, the Task Force recommends screening people who are at increased risk for syphilis infection.
Dr. Ogedegbe[/caption]
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Syphilis has become more common over the past 20 years, after reaching a record low in 2000. The Task Force found that screening people who are at increased risk for syphilis can identify the infection early so it can be treated before problems develop. For that reason, the Task Force recommends screening people who are at increased risk for syphilis infection.



 Dr. Van der Pol[/caption]
Barbara Van Der Pol, PhD, MPH
President, American STD Association
President-Elect, International Society fo STD Research
Professor of Medicine & Public Health
Director, STD Diagnostics Lab
Director, UAB STD Clinical Research Organization
University of Alabama at Birmingham
Birmingham, AL 35294
MedicalResearch.com: What is the background for this study?
Response: For many decades, public health programs focused on control and prevention of sexually transmitted infections (STI) have relied on lab based tests that required a 1-day to 1-week wait for test results. Efforts to shorten the duration of infection lead to treating at the time of the clinic visit based on the association between certain clinical signs or symptoms and the likelihood of infection.
Unfortunately, more than ½ of infected persons do not have signs or symptoms so they receive no treatment until test results are available. Thus, a test that could be performed at the clinical site with a limited wait time would improve the accuracy of treatment and shorten the duration of infection. Such a strategy will hopefully reduce the number of return clinic visits, the possibility of transmission, and the potential for consequences of untreated infection such as infertility.
Dr. Van der Pol[/caption]
Barbara Van Der Pol, PhD, MPH
President, American STD Association
President-Elect, International Society fo STD Research
Professor of Medicine & Public Health
Director, STD Diagnostics Lab
Director, UAB STD Clinical Research Organization
University of Alabama at Birmingham
Birmingham, AL 35294
MedicalResearch.com: What is the background for this study?
Response: For many decades, public health programs focused on control and prevention of sexually transmitted infections (STI) have relied on lab based tests that required a 1-day to 1-week wait for test results. Efforts to shorten the duration of infection lead to treating at the time of the clinic visit based on the association between certain clinical signs or symptoms and the likelihood of infection.
Unfortunately, more than ½ of infected persons do not have signs or symptoms so they receive no treatment until test results are available. Thus, a test that could be performed at the clinical site with a limited wait time would improve the accuracy of treatment and shorten the duration of infection. Such a strategy will hopefully reduce the number of return clinic visits, the possibility of transmission, and the potential for consequences of untreated infection such as infertility. 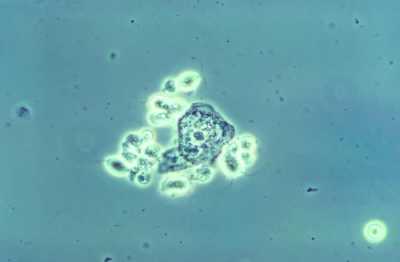
 Dr. Kaufman[/caption]
Gregory Kaufman, M.D.
Senior Vice President
Global Clinical and Medical Affairs
Specialty at Lupin
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by trichomoniasis? How common is this infection?
Response: The Phase 3 trial evaluated the effectiveness and safety of a single oral dose of Solosec® (secnidazole) 2g oral granules for the treatment of trichomoniasis in adult women. Top-line results were positive and showed that Solosec was generally well-tolerated.
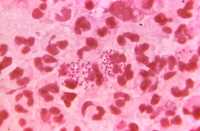
Trichomoniasis is the most common non-viral sexually transmitted infection (STI) in the U.S., and is caused by a protozoan parasite called Trichomonas vaginalis.
Dr. Kaufman[/caption]
Gregory Kaufman, M.D.
Senior Vice President
Global Clinical and Medical Affairs
Specialty at Lupin
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by trichomoniasis? How common is this infection?
Response: The Phase 3 trial evaluated the effectiveness and safety of a single oral dose of Solosec® (secnidazole) 2g oral granules for the treatment of trichomoniasis in adult women. Top-line results were positive and showed that Solosec was generally well-tolerated.
Trichomoniasis is the most common non-viral sexually transmitted infection (STI) in the U.S., and is caused by a protozoan parasite called Trichomonas vaginalis.












 Dr. Charu Kaushic[/caption]
Charu Kaushic. PhD.
Professor
OHTN Applied HIV Research Chair
Department of Pathology and Mol. Medicine
McMaster Immunology Research Center,
McMaster University
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Kaushic: Female sex hormones, estradiol and progesterone have been shown to regulate immune responses in many experimental and clinical studies. We and others have shown previously that these hormones also regulate susceptibility to and outcome of sexually transmitted infections (STIs), including Chlamydia, HSV-2, SIV and HIV-1. Most studies show that progesterone generally increases susceptibility while estradiol generally confers protection against STIs. This has recently gained much more widespread attention because of the controversy surrounding use of injectable hormonal contraceptives in geographical areas where there is high prevalence of HIV-1. The most frequently used injectable contraceptive uses a progestin-based formulation which has been correlated with 2-fold increase in HIV acquisition and transmission in epidemiological studies. Oral contraceptives that contain a combination of estradiol and progesterone do not show similar correlation with increased infection. This is currently a very important women’s health issue, which is being carefully monitored by many public health agencies, including WHO. Many researchers are focusing efforts in understanding how sex hormones can increase or decrease susceptibility of women to STIs.
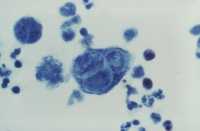
We have published in this area for more than a decade, including a series of papers showing that in a mouse model, the outcome of genital herpes (HSV-2) infection can depend on which hormone we treat the mice with. A few years ago, we showed for the first time that mice that received an HSV-2 vaccine under the influence of estradiol were much better protected and showed less disease pathology (Bhavanam et al, Vaccine 2008). These results were reproduced a year later by another group, using an actual HSV-2 vaccine formulation. Since then, we have been working to understand at a cellular level, the underlying mechanism of estradiol-mediated enhanced protection. In this PLOS Pathogens paper, we report for the first time a cellular mechanism by which estradiol was seen to enhance immune protection against HSV-2 infection in mice.
The main findings are that estradiol primes dendritic cells in the vaginal tract to induce enhanced anti-viral T cell responses. Dendritic cells are key immune cells that decide what type of immune responses will be mounted against an infection. Under the influence of estradiol, the dendritic cells in the vaginal tract of mice induced Th17 cells which in turn helped enhance anti-viral T cell responses (Th1), resulting in better protection against genital HSV-2. This regulation of anti-viral immunity was seen only in the reproductive tract.
Dr. Charu Kaushic[/caption]
Charu Kaushic. PhD.
Professor
OHTN Applied HIV Research Chair
Department of Pathology and Mol. Medicine
McMaster Immunology Research Center,
McMaster University
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Kaushic: Female sex hormones, estradiol and progesterone have been shown to regulate immune responses in many experimental and clinical studies. We and others have shown previously that these hormones also regulate susceptibility to and outcome of sexually transmitted infections (STIs), including Chlamydia, HSV-2, SIV and HIV-1. Most studies show that progesterone generally increases susceptibility while estradiol generally confers protection against STIs. This has recently gained much more widespread attention because of the controversy surrounding use of injectable hormonal contraceptives in geographical areas where there is high prevalence of HIV-1. The most frequently used injectable contraceptive uses a progestin-based formulation which has been correlated with 2-fold increase in HIV acquisition and transmission in epidemiological studies. Oral contraceptives that contain a combination of estradiol and progesterone do not show similar correlation with increased infection. This is currently a very important women’s health issue, which is being carefully monitored by many public health agencies, including WHO. Many researchers are focusing efforts in understanding how sex hormones can increase or decrease susceptibility of women to STIs.
We have published in this area for more than a decade, including a series of papers showing that in a mouse model, the outcome of genital herpes (HSV-2) infection can depend on which hormone we treat the mice with. A few years ago, we showed for the first time that mice that received an HSV-2 vaccine under the influence of estradiol were much better protected and showed less disease pathology (Bhavanam et al, Vaccine 2008). These results were reproduced a year later by another group, using an actual HSV-2 vaccine formulation. Since then, we have been working to understand at a cellular level, the underlying mechanism of estradiol-mediated enhanced protection. In this PLOS Pathogens paper, we report for the first time a cellular mechanism by which estradiol was seen to enhance immune protection against HSV-2 infection in mice.
The main findings are that estradiol primes dendritic cells in the vaginal tract to induce enhanced anti-viral T cell responses. Dendritic cells are key immune cells that decide what type of immune responses will be mounted against an infection. Under the influence of estradiol, the dendritic cells in the vaginal tract of mice induced Th17 cells which in turn helped enhance anti-viral T cell responses (Th1), resulting in better protection against genital HSV-2. This regulation of anti-viral immunity was seen only in the reproductive tract.

