[caption id="attachment_64007" align="aligncenter" width="500"]

Photo by l
uis gomes[/caption]
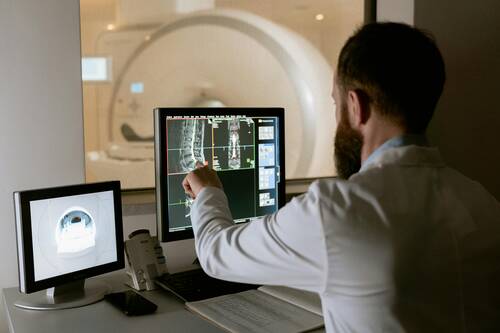
With medical needs escalating and technology advancing at an incredible pace, the speed of patient care is about to become much faster and more effective. Healthcare organizations are under pressure to do more with less. Businesses are finally able to leave their tech logjam behind when they plug into lean IT project services. Suddenly, the thorny vines of procedure fall away, and genuine innovation gets a second wind. Low costs don't mean low-quality care.. What if healthcare operations could run like a well-oiled machine? For that to happen, they need to corral their IT projects, but that's a tall order given the specific challenges they face.
Streamlining Operations Through Digital Transformation
Hospitals and clinics are constantly faced with the challenge of reducing costs without sacrificing the level of care their patients receive. Efficient
IT project services facilitate the implementation of digital tools and technologies that improve operational workflows and processes.
One area where IT project services provide critical support is electronic health record (EHR) integration. Healthcare goes high-tech when EHR systems are properly set up. It's like having a bird’s-eye view of a patient's entire journey, allowing doctors to spot connections and make swift, informed decisions. Under the watchful eye of regulatory authorities like HIPAA, IT project managers expertly integrate these systems, implementing checks and balances to prevent malfunctions and mishaps.
When automation technologies are properly integrated, they morph administrative tasks into background noise, allowing healthcare professionals to redirect their attention to the ones who need it most: their patients. Think of automation as a behind-the-scenes team player. By handing over the routine tasks, healthcare pros can refocus on what matters most: providing top-notch care.



























 Effective RCM is particularly important in today’s changing healthcare environment, where reimbursement is a critical issue for hospital finances. Development in RCM staffing is vital in addressing the needs that modern health organizations face. This blog post will outline the following most recent trends and methods associated with RCM staffing and why these approaches can be used to improve the performances of healthcare institutions.
Effective RCM is particularly important in today’s changing healthcare environment, where reimbursement is a critical issue for hospital finances. Development in RCM staffing is vital in addressing the needs that modern health organizations face. This blog post will outline the following most recent trends and methods associated with RCM staffing and why these approaches can be used to improve the performances of healthcare institutions.



 As technology continues to evolve within the healthcare sector, creating new opportunities for enhancing patient care, it's crucial that empathy doesn't get lost in the shuffle. Innovative tools and systems should be seen as avenues to deepen our understanding and connection with patients, rather than as barriers to the human touch. Embracing technology with empathetic intention can lead to an even greater level of personalized care.
One specific area where empathy can play a transformative role is in addressing
As technology continues to evolve within the healthcare sector, creating new opportunities for enhancing patient care, it's crucial that empathy doesn't get lost in the shuffle. Innovative tools and systems should be seen as avenues to deepen our understanding and connection with patients, rather than as barriers to the human touch. Embracing technology with empathetic intention can lead to an even greater level of personalized care.
One specific area where empathy can play a transformative role is in addressing