If you are a registered nurse, or you are thinking about nursing as a career option, then becoming a nurse practitioner is a great way to prove your experience and expertise.
It allows you more agency when working with patients, as the advanced level of qualification that nurse practitioners have means that they are allowed to make treatment decisions without the supervision of a physician.
Becoming a nurse practitioner also gives you access to higher remuneration, and to specialize in an area of medicine which can be incredibly fulfilling.
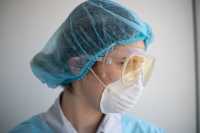 Nurse Practitioners are registered nurses who have carried out extra training, which means that they have more authority than registered nurses and share a similar responsibility level to doctors.
They are able to prescribe medications, order diagnostic tests and provide treatments much as a physician would. Also like a physician, they will have undertaken their training to specialize in a particular area of medicine.
Nurse Practitioners begin their careers as registered nurses, which means that they are used to approaching medicine in a patient-centric way. They will often work with an idea of patient comfort at the forefront of their minds, whereas a doctor can operate with an idea of medical treatment at the forefront of theirs. This means that a combination of doctors and Nurse Practitioners within a healthcare facility can lead to a more rounded care experience.
In some states, Nurse Practitioners are able to operate without the supervision of a doctor. However, in others, they do need to get a sign off for any treatments that they provide. There is a general movement towards allowing Nurse Practitioners more agency as this is helping to relieve strain on the healthcare system.
Nurse Practitioners are registered nurses who have carried out extra training, which means that they have more authority than registered nurses and share a similar responsibility level to doctors.
They are able to prescribe medications, order diagnostic tests and provide treatments much as a physician would. Also like a physician, they will have undertaken their training to specialize in a particular area of medicine.
Nurse Practitioners begin their careers as registered nurses, which means that they are used to approaching medicine in a patient-centric way. They will often work with an idea of patient comfort at the forefront of their minds, whereas a doctor can operate with an idea of medical treatment at the forefront of theirs. This means that a combination of doctors and Nurse Practitioners within a healthcare facility can lead to a more rounded care experience.
In some states, Nurse Practitioners are able to operate without the supervision of a doctor. However, in others, they do need to get a sign off for any treatments that they provide. There is a general movement towards allowing Nurse Practitioners more agency as this is helping to relieve strain on the healthcare system.
What is a nurse practitioner?
 Nurse Practitioners are registered nurses who have carried out extra training, which means that they have more authority than registered nurses and share a similar responsibility level to doctors.
They are able to prescribe medications, order diagnostic tests and provide treatments much as a physician would. Also like a physician, they will have undertaken their training to specialize in a particular area of medicine.
Nurse Practitioners begin their careers as registered nurses, which means that they are used to approaching medicine in a patient-centric way. They will often work with an idea of patient comfort at the forefront of their minds, whereas a doctor can operate with an idea of medical treatment at the forefront of theirs. This means that a combination of doctors and Nurse Practitioners within a healthcare facility can lead to a more rounded care experience.
In some states, Nurse Practitioners are able to operate without the supervision of a doctor. However, in others, they do need to get a sign off for any treatments that they provide. There is a general movement towards allowing Nurse Practitioners more agency as this is helping to relieve strain on the healthcare system.
Nurse Practitioners are registered nurses who have carried out extra training, which means that they have more authority than registered nurses and share a similar responsibility level to doctors.
They are able to prescribe medications, order diagnostic tests and provide treatments much as a physician would. Also like a physician, they will have undertaken their training to specialize in a particular area of medicine.
Nurse Practitioners begin their careers as registered nurses, which means that they are used to approaching medicine in a patient-centric way. They will often work with an idea of patient comfort at the forefront of their minds, whereas a doctor can operate with an idea of medical treatment at the forefront of theirs. This means that a combination of doctors and Nurse Practitioners within a healthcare facility can lead to a more rounded care experience.
In some states, Nurse Practitioners are able to operate without the supervision of a doctor. However, in others, they do need to get a sign off for any treatments that they provide. There is a general movement towards allowing Nurse Practitioners more agency as this is helping to relieve strain on the healthcare system.


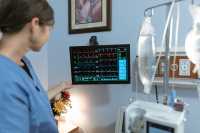 If you’re currently working as a nurse, you are probably well aware of just how rewarding and fulfilling a job role it can be. You get to help patients from all walks of life every single day and make a real difference to not only people’s health but their lives more generally. It’s also a career in which there is a lot of scope for progression. There are so many different spheres within the field of nursing that you can choose to specialize in, whether it’s a particular age group (like pediatrics or gerontology) or a particular health condition (like oncology or emergency care).
Some of these paths involve training on the job, whereas others require you to return to college to study and obtain a postgraduate qualification. Among these, one of the highest possible qualifications you can aim for is the DNP, or Doctor of Nursing Practice.
If you’re currently working as a nurse, you are probably well aware of just how rewarding and fulfilling a job role it can be. You get to help patients from all walks of life every single day and make a real difference to not only people’s health but their lives more generally. It’s also a career in which there is a lot of scope for progression. There are so many different spheres within the field of nursing that you can choose to specialize in, whether it’s a particular age group (like pediatrics or gerontology) or a particular health condition (like oncology or emergency care).
Some of these paths involve training on the job, whereas others require you to return to college to study and obtain a postgraduate qualification. Among these, one of the highest possible qualifications you can aim for is the DNP, or Doctor of Nursing Practice. 








 Dr. Rattray[/caption]
Nicholas A. Rattray, Ph.D.
Research Scientist/Investigator
VA HSR&D Center for Health Information and Communication
Implementation Core, Precision Monitoring to Transform Care (PRISM) QUERI
Richard L. Roudebush Veterans Affairs Medical Center
Indiana University Center for Health Services & Outcomes Research
Regenstrief Institute, Inc.
Indianapolis, Indiana
on behalf of study co-authors re:
Rattray NA, Flanagan ME, Militello LG, Barach P, Franks Z, Ebright P, Rehman SU,
Gordon HS, Frankel RM
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: End-of-shift handoffs pose a substantial patient safety risk. The transition of care from one doctor to another has been associated with delays in diagnosis and treatment, duplication of tests or treatment and patient discomfort, inappropriate care, medication errors and longer hospital stays with more laboratory testing. Handoff education varies widely in medical schools and residency training programs. Although there have been efforts to improve transfers of care, they have not shown meaningful improvement.
Led for the last decade by Richard Frankel, Ph.D., a senior health scientist at Regenstrief Institute and Indiana University and professor at Indiana University School of Medicine, our team has studied how health practitioners communicate during end-of-shift handoffs. In this current study, funded by VA Health Services and Research Development, we conducted interviews with 35 internal medicine and surgery residents at three VA medical centers about a recent handoff and analyzed the responses. Our team also video-recorded and analyzed more than 150 handoffs.
Published in the Journal of General Internal Medicine, this study explains how the person receiving the handoff can affect the interaction. Medical residents said they changed their delivery based on the doctor or resident who was taking over (i.e., training level, preference for fewer details, day or night shift). We found that handoff communication involves a complex combination of socio-technical information where residents balance relational factors against content and risk. It is not a mechanistic process of merely transferring clinical data but rather is based on learned habits of communication that are context-sensitive and variable, what we refer to as “recipient design”.
In another paper led by Laura Militello, we focus on how residents cognitively prepare for handoffs. In the paper published in The Joint Commission Journal of Quality and Patient Safety®, researchers detailed the tasks involved in cognitively preparing for handoffs. A third paper, published in BMC Medical Education, reports on the limited training that physicians receive during their residency. Residents said they were only partially prepared for enacting handoffs as interns, and clinical experience and enacting handoffs actually taught them the most.
Dr. Rattray[/caption]
Nicholas A. Rattray, Ph.D.
Research Scientist/Investigator
VA HSR&D Center for Health Information and Communication
Implementation Core, Precision Monitoring to Transform Care (PRISM) QUERI
Richard L. Roudebush Veterans Affairs Medical Center
Indiana University Center for Health Services & Outcomes Research
Regenstrief Institute, Inc.
Indianapolis, Indiana
on behalf of study co-authors re:
Rattray NA, Flanagan ME, Militello LG, Barach P, Franks Z, Ebright P, Rehman SU,
Gordon HS, Frankel RM
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: End-of-shift handoffs pose a substantial patient safety risk. The transition of care from one doctor to another has been associated with delays in diagnosis and treatment, duplication of tests or treatment and patient discomfort, inappropriate care, medication errors and longer hospital stays with more laboratory testing. Handoff education varies widely in medical schools and residency training programs. Although there have been efforts to improve transfers of care, they have not shown meaningful improvement.
Led for the last decade by Richard Frankel, Ph.D., a senior health scientist at Regenstrief Institute and Indiana University and professor at Indiana University School of Medicine, our team has studied how health practitioners communicate during end-of-shift handoffs. In this current study, funded by VA Health Services and Research Development, we conducted interviews with 35 internal medicine and surgery residents at three VA medical centers about a recent handoff and analyzed the responses. Our team also video-recorded and analyzed more than 150 handoffs.
Published in the Journal of General Internal Medicine, this study explains how the person receiving the handoff can affect the interaction. Medical residents said they changed their delivery based on the doctor or resident who was taking over (i.e., training level, preference for fewer details, day or night shift). We found that handoff communication involves a complex combination of socio-technical information where residents balance relational factors against content and risk. It is not a mechanistic process of merely transferring clinical data but rather is based on learned habits of communication that are context-sensitive and variable, what we refer to as “recipient design”.
In another paper led by Laura Militello, we focus on how residents cognitively prepare for handoffs. In the paper published in The Joint Commission Journal of Quality and Patient Safety®, researchers detailed the tasks involved in cognitively preparing for handoffs. A third paper, published in BMC Medical Education, reports on the limited training that physicians receive during their residency. Residents said they were only partially prepared for enacting handoffs as interns, and clinical experience and enacting handoffs actually taught them the most.














 Dr. Gayer[/caption]
Gregory Gayer, PhD
Associate Professor
Chair of Basic Science Department
TUCOM California
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The prevalence of obesity in the United States continues to be a growing and remains a major health concern. Closely associated with obesity is an extensive list of chronic diseases, including hypertension, dyslipidemia, and type 2 diabetes. Unfortunately, physician bias against obese people may create a self-defeating environment that can produce less effective communication in a manner that could reduce the patient’s willingness to participate in their own health. Our overall goal is to prepare future physicians to appropriately engage the obese patient in order to optimize health care delivery.
This study was initiated in response to the ever increasing demand on the medical profession to properly care for the
Dr. Gayer[/caption]
Gregory Gayer, PhD
Associate Professor
Chair of Basic Science Department
TUCOM California
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The prevalence of obesity in the United States continues to be a growing and remains a major health concern. Closely associated with obesity is an extensive list of chronic diseases, including hypertension, dyslipidemia, and type 2 diabetes. Unfortunately, physician bias against obese people may create a self-defeating environment that can produce less effective communication in a manner that could reduce the patient’s willingness to participate in their own health. Our overall goal is to prepare future physicians to appropriately engage the obese patient in order to optimize health care delivery.
This study was initiated in response to the ever increasing demand on the medical profession to properly care for the 



