Author Interviews, CMAJ, Race/Ethnic Diversity / 23.03.2026
Canadian Black Adults Less Likely to Have Prescription Drug Coverage and More Likely to Skip Meds Due to Costs
MedicalResearch.com Interview with:
[caption id="attachment_72842" align="alignleft" width="200"] Bukola Salami, Ph.D.[/caption]
Bukola Salami, RN, BScN, MN, PhD, FCAN, FAAN (She/Her)
Full Professor
Canada Research Chair (Tier 1) in Black and Racialized Peoples Health
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study?
Response: Black people experience disproportionately poor health outcomes, with access to healthcare recognized as a key determinant of health. Although prior research has examined factors influencing healthcare access among Black populations, there is limited evidence on medication access and use. This gap is particularly important in the context of emerging Pharmacare policy in Canada. In this study, we aimed to assess the prevalence of cost-related prescription nonadherence among Black adults in Canada and to examine racial disparities in comparison to White adults, while accounting for demographic, socioeconomic, and insurance-related factors as potential mediators.
Bukola Salami, Ph.D.[/caption]
Bukola Salami, RN, BScN, MN, PhD, FCAN, FAAN (She/Her)
Full Professor
Canada Research Chair (Tier 1) in Black and Racialized Peoples Health
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study?
Response: Black people experience disproportionately poor health outcomes, with access to healthcare recognized as a key determinant of health. Although prior research has examined factors influencing healthcare access among Black populations, there is limited evidence on medication access and use. This gap is particularly important in the context of emerging Pharmacare policy in Canada. In this study, we aimed to assess the prevalence of cost-related prescription nonadherence among Black adults in Canada and to examine racial disparities in comparison to White adults, while accounting for demographic, socioeconomic, and insurance-related factors as potential mediators.
 Bukola Salami, Ph.D.[/caption]
Bukola Salami, RN, BScN, MN, PhD, FCAN, FAAN (She/Her)
Full Professor
Canada Research Chair (Tier 1) in Black and Racialized Peoples Health
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study?
Response: Black people experience disproportionately poor health outcomes, with access to healthcare recognized as a key determinant of health. Although prior research has examined factors influencing healthcare access among Black populations, there is limited evidence on medication access and use. This gap is particularly important in the context of emerging Pharmacare policy in Canada. In this study, we aimed to assess the prevalence of cost-related prescription nonadherence among Black adults in Canada and to examine racial disparities in comparison to White adults, while accounting for demographic, socioeconomic, and insurance-related factors as potential mediators.
Bukola Salami, Ph.D.[/caption]
Bukola Salami, RN, BScN, MN, PhD, FCAN, FAAN (She/Her)
Full Professor
Canada Research Chair (Tier 1) in Black and Racialized Peoples Health
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study?
Response: Black people experience disproportionately poor health outcomes, with access to healthcare recognized as a key determinant of health. Although prior research has examined factors influencing healthcare access among Black populations, there is limited evidence on medication access and use. This gap is particularly important in the context of emerging Pharmacare policy in Canada. In this study, we aimed to assess the prevalence of cost-related prescription nonadherence among Black adults in Canada and to examine racial disparities in comparison to White adults, while accounting for demographic, socioeconomic, and insurance-related factors as potential mediators.


 Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.
Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.


 Jiawen Liu[/caption]
Jiawen Liu, PhD student
Department of Civil & Environmental Engineering
University of Washington
MedicalResearch.com: What is the background for this study?
Response: As previous literature has documented, racial/ethnic minority populations and lower-income populations in the US often experience higher-than-average burdens of air pollution and its associated health impacts.
The disparities vary by pollutant, location, and time. In 2014, Clark et al. found higher average NO2 exposure for nonwhites than for whites and for below-poverty-level than for above-poverty-level. Clark et al. (2017) expanded research for NO2 exposure by race-ethnicity and socioeconomic status to 2000 and 2010 and found that absolute racial-ethnic disparities decreased over time while relative racial-ethnic disparities persisted.
Jiawen Liu[/caption]
Jiawen Liu, PhD student
Department of Civil & Environmental Engineering
University of Washington
MedicalResearch.com: What is the background for this study?
Response: As previous literature has documented, racial/ethnic minority populations and lower-income populations in the US often experience higher-than-average burdens of air pollution and its associated health impacts.
The disparities vary by pollutant, location, and time. In 2014, Clark et al. found higher average NO2 exposure for nonwhites than for whites and for below-poverty-level than for above-poverty-level. Clark et al. (2017) expanded research for NO2 exposure by race-ethnicity and socioeconomic status to 2000 and 2010 and found that absolute racial-ethnic disparities decreased over time while relative racial-ethnic disparities persisted. 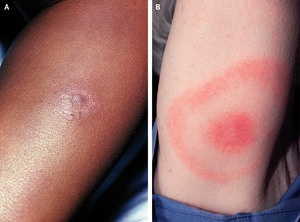
 Dr. Dan P. Ly[/caption]
Division of General Internal Medicine and Health Services Research
David Geffen School of Medicine at UCLA
Los Angeles, CA
MedicalResearch.com: What is the background for this study?
Response: Lyme disease presents first on the skin with the classic “bull’s-eye” rash. But such rashes in Black patients aren’t well-represented in medical textbooks. This may lead to physicians not recognizing such rashes in Black patients.
As a result, Black patients are more likely to present with later complications of Lyme disease when first diagnosed such as neurologic complications.
Dr. Dan P. Ly[/caption]
Division of General Internal Medicine and Health Services Research
David Geffen School of Medicine at UCLA
Los Angeles, CA
MedicalResearch.com: What is the background for this study?
Response: Lyme disease presents first on the skin with the classic “bull’s-eye” rash. But such rashes in Black patients aren’t well-represented in medical textbooks. This may lead to physicians not recognizing such rashes in Black patients.
As a result, Black patients are more likely to present with later complications of Lyme disease when first diagnosed such as neurologic complications. 

 Dr. Correa[/caption]
Andres F. Correa, MD
Assistant Professor
Department of Surgical Oncology, and
[caption id="attachment_57815" align="alignleft" width="150"]
Dr. Correa[/caption]
Andres F. Correa, MD
Assistant Professor
Department of Surgical Oncology, and
[caption id="attachment_57815" align="alignleft" width="150"] Dr. Bernstein[/caption]
Adrien Bernstein, MD
Second Year Urologic Oncology Fellow
Fox Chase Cancer Center
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, it has been well-established that historically Black Americans experience increased cancer specific mortality compared to white patients. In prostate cancer specifically studies have shown that when access to care is equitable this gap resolves. This suggests that biological factors are not driving these differences but rather the result of the complex interplay of social determinants and systemic inequities in our healthcare system.
Early in the pandemic, multiple studies demonstrated that minority communities disproportionately shouldered poor COVID-19 outcomes. On March 13th 2020, the American College of Surgeons recommended against elective procedures; however, the definition of an elective oncologic case was left to the discretion of the provider. As prostate cancer treatment can be safely deferred up to a year follow diagnosis, management of prostate cancer during the initial lockdown period of the COVID-19 Pandemic provided a useful analysis of the differential restrictions placed on non-emergent health care during the Pandemic.
Dr. Bernstein[/caption]
Adrien Bernstein, MD
Second Year Urologic Oncology Fellow
Fox Chase Cancer Center
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, it has been well-established that historically Black Americans experience increased cancer specific mortality compared to white patients. In prostate cancer specifically studies have shown that when access to care is equitable this gap resolves. This suggests that biological factors are not driving these differences but rather the result of the complex interplay of social determinants and systemic inequities in our healthcare system.
Early in the pandemic, multiple studies demonstrated that minority communities disproportionately shouldered poor COVID-19 outcomes. On March 13th 2020, the American College of Surgeons recommended against elective procedures; however, the definition of an elective oncologic case was left to the discretion of the provider. As prostate cancer treatment can be safely deferred up to a year follow diagnosis, management of prostate cancer during the initial lockdown period of the COVID-19 Pandemic provided a useful analysis of the differential restrictions placed on non-emergent health care during the Pandemic.



 Dr. Salciccioli[/caption]
Justin Salciccioli, MBBS, MA
Research Fellow in Medicine
[caption id="attachment_57392" align="alignleft" width="150"]
Dr. Salciccioli[/caption]
Justin Salciccioli, MBBS, MA
Research Fellow in Medicine
[caption id="attachment_57392" align="alignleft" width="150"] Dr. Israel[/caption]
Elliot Israel, MD
Professor of Medicine, Harvard Medical School
Pulmonary and Critical Care, Rheumatology, Medicine
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Asthma attacks account for almost 50% of the cost of asthma care, which costs $80 billion each year in the United States. Asthma is more severe in African-American/Black and Hispanic/Latinx patients, with these groups having double the rates of attacks and hospitalizations as the general population. The PREPARE study is an ongoing national clinical trial for African American/Black and Hispanic/Latinx adults with moderate-to-severe asthma from different U.S. cities in which reporting of asthma control and asthma exacerbations was monitored entirely remotely.
With the arrival of the Covid19 pandemic, several studies suggested that asthma exacerbations may have decreased during the pandemic. However, multiple reports have suggested people were avoiding health services because of the pandemic, making it difficult to tell whether exacerbations truly decreased or whether people were simply avoiding their doctors. This is the first study done to assess asthma exacerbations before and during the pandemic that is unlikely to be impacted by patient healthcare avoidance.
Dr. Israel[/caption]
Elliot Israel, MD
Professor of Medicine, Harvard Medical School
Pulmonary and Critical Care, Rheumatology, Medicine
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Asthma attacks account for almost 50% of the cost of asthma care, which costs $80 billion each year in the United States. Asthma is more severe in African-American/Black and Hispanic/Latinx patients, with these groups having double the rates of attacks and hospitalizations as the general population. The PREPARE study is an ongoing national clinical trial for African American/Black and Hispanic/Latinx adults with moderate-to-severe asthma from different U.S. cities in which reporting of asthma control and asthma exacerbations was monitored entirely remotely.
With the arrival of the Covid19 pandemic, several studies suggested that asthma exacerbations may have decreased during the pandemic. However, multiple reports have suggested people were avoiding health services because of the pandemic, making it difficult to tell whether exacerbations truly decreased or whether people were simply avoiding their doctors. This is the first study done to assess asthma exacerbations before and during the pandemic that is unlikely to be impacted by patient healthcare avoidance.

 Laura M. Bogart, PhD
Senior Behavioral Scientist
RAND Corporation
Santa Monica, CA 90407-2138
MedicalResearch.com: What is the background for this study?
Response: Recent media polls continue to show that Black Americans are less likely to intend to get the COVID-19 vaccine than White Americans, and initial state data show a similar racial/ethnic disparity in vaccination rates. Initial uptake of the vaccine has been significantly affected by inequities in vaccine access and supply. In addition to these challenges, other factors contribute to hesitancy around vaccination, including self-perceived risk of infection, trust in the vaccine itself, trust in healthcare systems, healthcare providers, and policymakers who support the vaccine, and trust in the pharmaceutical industry and clinical research. In this study, we conducted a survey of a nationally representative sample of 207 Black Americans in late 2020, after initial COVID-19 vaccine effectiveness and safety data were released to the public. We also did in-depth interviews with a subsample of those surveyed who said that they would not get vaccinated. In addition, we engaged with a stakeholder advisory committee comprised of individuals who represent different subgroups and organizations in Black communities in the U.S., in order to discuss the results and make recommendations for policies to increase COVID-19 vaccination among Black Americans.
Laura M. Bogart, PhD
Senior Behavioral Scientist
RAND Corporation
Santa Monica, CA 90407-2138
MedicalResearch.com: What is the background for this study?
Response: Recent media polls continue to show that Black Americans are less likely to intend to get the COVID-19 vaccine than White Americans, and initial state data show a similar racial/ethnic disparity in vaccination rates. Initial uptake of the vaccine has been significantly affected by inequities in vaccine access and supply. In addition to these challenges, other factors contribute to hesitancy around vaccination, including self-perceived risk of infection, trust in the vaccine itself, trust in healthcare systems, healthcare providers, and policymakers who support the vaccine, and trust in the pharmaceutical industry and clinical research. In this study, we conducted a survey of a nationally representative sample of 207 Black Americans in late 2020, after initial COVID-19 vaccine effectiveness and safety data were released to the public. We also did in-depth interviews with a subsample of those surveyed who said that they would not get vaccinated. In addition, we engaged with a stakeholder advisory committee comprised of individuals who represent different subgroups and organizations in Black communities in the U.S., in order to discuss the results and make recommendations for policies to increase COVID-19 vaccination among Black Americans.