AHA Journals, Author Interviews, Heart Disease, Stroke / 12.03.2021
Stroke Risk: AI Can Help Predict Who Might Develop Atrial Fibrillation
MedicalResearch.com Interview with:
[caption id="attachment_56932" align="alignleft" width="200"] Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
 Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
 Dr. Kistler[/caption]
Professor Peter M Kistler MBBS, PhD, FRACP
Head of Clinical Electrophysiology Research
Baker Heart and Diabetes Institute
Head of Electrophysiology at The Alfred hospital
Professor of Medicine
University of Melbourne.
MedicalResearch.com: What is the background for this study?
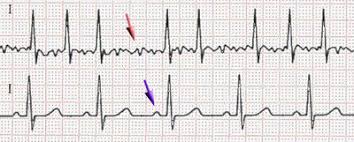
Response: There is a well known association between alcohol intake and atrial fibrillation form population based studies which demonstrate that for every 1 standard drink the incidence of AFib increases by 8%.
This is the first randomised study to determine of alcohol reduction/abstinence leads to a reduction in AFib episodes and time to recurrence.
Dr. Kistler[/caption]
Professor Peter M Kistler MBBS, PhD, FRACP
Head of Clinical Electrophysiology Research
Baker Heart and Diabetes Institute
Head of Electrophysiology at The Alfred hospital
Professor of Medicine
University of Melbourne.
MedicalResearch.com: What is the background for this study?
Response: There is a well known association between alcohol intake and atrial fibrillation form population based studies which demonstrate that for every 1 standard drink the incidence of AFib increases by 8%.
This is the first randomised study to determine of alcohol reduction/abstinence leads to a reduction in AFib episodes and time to recurrence.




 Dr. Phelan[/caption]
Dermot Phelan, MD, PhD
Director of the Sports Cardiology Center
Cleveland Clinic in Cleveland, Ohio
MedicalResearch.com: What is the background for this study?
Response: It is well recognized that long-term elite endurance athletes are at higher risk of atrial fibrillation. We wished to evaluate whether this held true for primarily strength-type athletes. We had the opportunity to screen almost 500 former NFL athletes. It became clear that we were seeing more atrial fibrillation than one would expect during the screenings.
Dr. Phelan[/caption]
Dermot Phelan, MD, PhD
Director of the Sports Cardiology Center
Cleveland Clinic in Cleveland, Ohio
MedicalResearch.com: What is the background for this study?
Response: It is well recognized that long-term elite endurance athletes are at higher risk of atrial fibrillation. We wished to evaluate whether this held true for primarily strength-type athletes. We had the opportunity to screen almost 500 former NFL athletes. It became clear that we were seeing more atrial fibrillation than one would expect during the screenings.






 Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
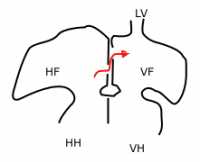
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.
Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.