Author Interviews, Dermatology, JAMA, Salt-Sodium / 12.06.2024
UCSF Study Finds Salt Intake May Be Associated with Eczema Severity
MedicalResearch.com Interview with:
[caption id="attachment_61942" align="alignleft" width="200"] Dr. Abuabar[/caption]
Katrina Abuabara, MD, MA, MSCE
Associate Professor of Dermatology, UCSF
Associate Adjunct Professor of Epidemiology
UC Berkeley School of Public Health
MedicalResearch.com: What is the background for this study?
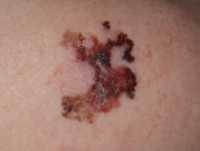
Response: Eczema (also known as atopic dermatitis) has become increasingly common over recent decades, especially in industrialized countries, suggesting that environmental or lifestyle factors like diet could impact rates of disease. It is well established that sodium, consumed primarily in the form of salt, increases the risk of hypertension and heart disease through pro-inflammatory mechanisms. The role of sodium on other chronic inflammatory conditions like eczema has been less well-studied.
Dr. Abuabar[/caption]
Katrina Abuabara, MD, MA, MSCE
Associate Professor of Dermatology, UCSF
Associate Adjunct Professor of Epidemiology
UC Berkeley School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Eczema (also known as atopic dermatitis) has become increasingly common over recent decades, especially in industrialized countries, suggesting that environmental or lifestyle factors like diet could impact rates of disease. It is well established that sodium, consumed primarily in the form of salt, increases the risk of hypertension and heart disease through pro-inflammatory mechanisms. The role of sodium on other chronic inflammatory conditions like eczema has been less well-studied.
 Dr. Abuabar[/caption]
Katrina Abuabara, MD, MA, MSCE
Associate Professor of Dermatology, UCSF
Associate Adjunct Professor of Epidemiology
UC Berkeley School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Eczema (also known as atopic dermatitis) has become increasingly common over recent decades, especially in industrialized countries, suggesting that environmental or lifestyle factors like diet could impact rates of disease. It is well established that sodium, consumed primarily in the form of salt, increases the risk of hypertension and heart disease through pro-inflammatory mechanisms. The role of sodium on other chronic inflammatory conditions like eczema has been less well-studied.
Dr. Abuabar[/caption]
Katrina Abuabara, MD, MA, MSCE
Associate Professor of Dermatology, UCSF
Associate Adjunct Professor of Epidemiology
UC Berkeley School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Eczema (also known as atopic dermatitis) has become increasingly common over recent decades, especially in industrialized countries, suggesting that environmental or lifestyle factors like diet could impact rates of disease. It is well established that sodium, consumed primarily in the form of salt, increases the risk of hypertension and heart disease through pro-inflammatory mechanisms. The role of sodium on other chronic inflammatory conditions like eczema has been less well-studied.
Author Interviews, Dermatology, Immunotherapy / 18.07.2023
Atopic Dermatitis: Mount Sinai Study Finds Lebrikizumab May Allow Longer Intervals Between Treatments
MedicalResearch.com Interview with:
[caption id="attachment_60633" align="alignleft" width="150"] Dr. Guttman-Yassky[/caption]
Emma Guttman-Yassky, M.D., PhD,
Lead investigator of this study
Waldman Professor and
System Chair
Kimberly and Eric J. Waldman Department of Dermatology
Icahn School of Medicine at Mount Sinai, NY
MedicalResearch.com: What is the background for this study?
Response: The idea to test how spacing out treatment or even stopping it affects treatment responses once patients are well controlled. Lebrikizumab it is a potent biologic agent with a relatively long-lasting effect.
Dr. Guttman-Yassky[/caption]
Emma Guttman-Yassky, M.D., PhD,
Lead investigator of this study
Waldman Professor and
System Chair
Kimberly and Eric J. Waldman Department of Dermatology
Icahn School of Medicine at Mount Sinai, NY
MedicalResearch.com: What is the background for this study?
Response: The idea to test how spacing out treatment or even stopping it affects treatment responses once patients are well controlled. Lebrikizumab it is a potent biologic agent with a relatively long-lasting effect.
 Dr. Guttman-Yassky[/caption]
Emma Guttman-Yassky, M.D., PhD,
Lead investigator of this study
Waldman Professor and
System Chair
Kimberly and Eric J. Waldman Department of Dermatology
Icahn School of Medicine at Mount Sinai, NY
MedicalResearch.com: What is the background for this study?
Response: The idea to test how spacing out treatment or even stopping it affects treatment responses once patients are well controlled. Lebrikizumab it is a potent biologic agent with a relatively long-lasting effect.
Dr. Guttman-Yassky[/caption]
Emma Guttman-Yassky, M.D., PhD,
Lead investigator of this study
Waldman Professor and
System Chair
Kimberly and Eric J. Waldman Department of Dermatology
Icahn School of Medicine at Mount Sinai, NY
MedicalResearch.com: What is the background for this study?
Response: The idea to test how spacing out treatment or even stopping it affects treatment responses once patients are well controlled. Lebrikizumab it is a potent biologic agent with a relatively long-lasting effect.
Author Interviews, Dermatology, Eli Lilly, NEJM / 26.03.2023
NEJM: Two Phase 3 Trials Find Lebrikizumab Safe and Highly Effective for Atopic Dermatitis
MedicalResearch.com Interview with:
[caption id="attachment_24142" align="alignleft" width="128"] Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Lebrikizumab was previously shown to be safe and effective as a treatment for moderate-severe atopic dermatitis in a phase 2 study. These Phase 3 randomized placebo-controlled trials are the largest studies to date of lebrikizumab in AD. They showed that lebrikizumab was safe and highly effective for the treatment of moderate-severe atopic dermatitis. These studies will hopefully support the approval of lebrikizumab in the United States later this year.
Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Lebrikizumab was previously shown to be safe and effective as a treatment for moderate-severe atopic dermatitis in a phase 2 study. These Phase 3 randomized placebo-controlled trials are the largest studies to date of lebrikizumab in AD. They showed that lebrikizumab was safe and highly effective for the treatment of moderate-severe atopic dermatitis. These studies will hopefully support the approval of lebrikizumab in the United States later this year.
 Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Lebrikizumab was previously shown to be safe and effective as a treatment for moderate-severe atopic dermatitis in a phase 2 study. These Phase 3 randomized placebo-controlled trials are the largest studies to date of lebrikizumab in AD. They showed that lebrikizumab was safe and highly effective for the treatment of moderate-severe atopic dermatitis. These studies will hopefully support the approval of lebrikizumab in the United States later this year.
Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Lebrikizumab was previously shown to be safe and effective as a treatment for moderate-severe atopic dermatitis in a phase 2 study. These Phase 3 randomized placebo-controlled trials are the largest studies to date of lebrikizumab in AD. They showed that lebrikizumab was safe and highly effective for the treatment of moderate-severe atopic dermatitis. These studies will hopefully support the approval of lebrikizumab in the United States later this year.
Allergies, Author Interviews, Cancer Research, Dermatology, Melanoma / 17.03.2023
Study Finds Lower Risk of Melanoma in Patients with Atopic History
MedicalResearch.com Interview with:
Jenni Komulainen
University of Eastern Finland | UEF
MedicalResearch.com: What is the background for this study?
Response: The background for this study comes from the earlier findings that the skin cancer risk and atopic status have some connection, but the results have been inconsistent. The connection between atopy and skin cancers may be related to the stimulation of protective immune response or the predisposition to carcinogenesis through chronic inflammation. The aim of this study was to investigate if atopic disorders associate with skin cancers.
Allergies, Author Interviews, Dermatology / 09.03.2023
Eczema: Mount Sinai Study Finds No Increase Risk of Cancer in 5 Year Study of Dupilumab
MedicalResearch.com Interview with:
[caption id="attachment_60156" align="alignleft" width="150"] Dr. Gulati[/caption]
Nicholas Gulati, MD, PhD
Director, Early Detection of Skin Cancer and Oncodermatology Clinic
The Kimberly and Eric J. Waldman
Department of Dermatology
Mount Sinai Health System
New York, New York
MedicalResearch.com: What is the background for this study? What is dupilumab primarily used for?
Response: Dupilumab is a monoclonal antibody that inhibits a specific part of the immune system known as Th2 cells, which are important in the development of various diseases including atopic dermatitis (eczema) and asthma. Therefore, dupilumab has become one of the major treatments for these conditions. Given the increasing use of this drug, it is important to understand the safety of it in terms of cancer development, as that is currently largely unknown.
Dr. Gulati[/caption]
Nicholas Gulati, MD, PhD
Director, Early Detection of Skin Cancer and Oncodermatology Clinic
The Kimberly and Eric J. Waldman
Department of Dermatology
Mount Sinai Health System
New York, New York
MedicalResearch.com: What is the background for this study? What is dupilumab primarily used for?
Response: Dupilumab is a monoclonal antibody that inhibits a specific part of the immune system known as Th2 cells, which are important in the development of various diseases including atopic dermatitis (eczema) and asthma. Therefore, dupilumab has become one of the major treatments for these conditions. Given the increasing use of this drug, it is important to understand the safety of it in terms of cancer development, as that is currently largely unknown.
 Dr. Gulati[/caption]
Nicholas Gulati, MD, PhD
Director, Early Detection of Skin Cancer and Oncodermatology Clinic
The Kimberly and Eric J. Waldman
Department of Dermatology
Mount Sinai Health System
New York, New York
MedicalResearch.com: What is the background for this study? What is dupilumab primarily used for?
Response: Dupilumab is a monoclonal antibody that inhibits a specific part of the immune system known as Th2 cells, which are important in the development of various diseases including atopic dermatitis (eczema) and asthma. Therefore, dupilumab has become one of the major treatments for these conditions. Given the increasing use of this drug, it is important to understand the safety of it in terms of cancer development, as that is currently largely unknown.
Dr. Gulati[/caption]
Nicholas Gulati, MD, PhD
Director, Early Detection of Skin Cancer and Oncodermatology Clinic
The Kimberly and Eric J. Waldman
Department of Dermatology
Mount Sinai Health System
New York, New York
MedicalResearch.com: What is the background for this study? What is dupilumab primarily used for?
Response: Dupilumab is a monoclonal antibody that inhibits a specific part of the immune system known as Th2 cells, which are important in the development of various diseases including atopic dermatitis (eczema) and asthma. Therefore, dupilumab has become one of the major treatments for these conditions. Given the increasing use of this drug, it is important to understand the safety of it in terms of cancer development, as that is currently largely unknown.
Author Interviews, Dermatology, JAMA, Pediatrics, Rheumatology / 26.02.2023
Atopic Dermatitis – Eczema: Greater Awareness in Black and Hispanic Children
MedicalResearch.com Interview with: Siri Choragudi Medical Student University of Miami Gil Yosipovitch, MD Professor and Stiefel endowed Chair of Medical Dermatology at the Dr Phillip...
Author Interviews, Dermatology, Lancet / 13.12.2022
Atopic Dermatitis- Eczema: New Antibody Therapy Has Potential to Modify Disease Course
MedicalResearch.com Interview with:
[caption id="attachment_59823" align="alignleft" width="130"] Dr. Guttman-Yassky[/caption]
Dr. Emma Guttman-Yassky, MD, PhD
Waldman Professor and System Chair
The Kimberly and Eric J. Waldman Department of Dermatology
Director, Center of Excellence in Eczema
Director, Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study are studies that show that OX40 is a pathway that is upregulated in patients with atopic dermatitis (or eczema). OX40 is involved in activation of immune molecules associated with allergy and atopy, and also with formation of memory immune cells that are required for disease recurrence. The hypothesis to the study was that giving an OX40 antagonist will not only ameliorate the disease but perhaps have a remittive effect in that the disease will not come back.
Indeed all drug doses were significantly effective at week 16, the primary endpoint compared to placebo and continued to improve towards week 36, the secondary endpoint. In addition, the responders to treatment maintained their responses for an additional 20 weeks, which is unusual, suggesting a potential for disease modification.
Dr. Guttman-Yassky[/caption]
Dr. Emma Guttman-Yassky, MD, PhD
Waldman Professor and System Chair
The Kimberly and Eric J. Waldman Department of Dermatology
Director, Center of Excellence in Eczema
Director, Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study are studies that show that OX40 is a pathway that is upregulated in patients with atopic dermatitis (or eczema). OX40 is involved in activation of immune molecules associated with allergy and atopy, and also with formation of memory immune cells that are required for disease recurrence. The hypothesis to the study was that giving an OX40 antagonist will not only ameliorate the disease but perhaps have a remittive effect in that the disease will not come back.
Indeed all drug doses were significantly effective at week 16, the primary endpoint compared to placebo and continued to improve towards week 36, the secondary endpoint. In addition, the responders to treatment maintained their responses for an additional 20 weeks, which is unusual, suggesting a potential for disease modification.
 Dr. Guttman-Yassky[/caption]
Dr. Emma Guttman-Yassky, MD, PhD
Waldman Professor and System Chair
The Kimberly and Eric J. Waldman Department of Dermatology
Director, Center of Excellence in Eczema
Director, Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study are studies that show that OX40 is a pathway that is upregulated in patients with atopic dermatitis (or eczema). OX40 is involved in activation of immune molecules associated with allergy and atopy, and also with formation of memory immune cells that are required for disease recurrence. The hypothesis to the study was that giving an OX40 antagonist will not only ameliorate the disease but perhaps have a remittive effect in that the disease will not come back.
Indeed all drug doses were significantly effective at week 16, the primary endpoint compared to placebo and continued to improve towards week 36, the secondary endpoint. In addition, the responders to treatment maintained their responses for an additional 20 weeks, which is unusual, suggesting a potential for disease modification.
Dr. Guttman-Yassky[/caption]
Dr. Emma Guttman-Yassky, MD, PhD
Waldman Professor and System Chair
The Kimberly and Eric J. Waldman Department of Dermatology
Director, Center of Excellence in Eczema
Director, Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study are studies that show that OX40 is a pathway that is upregulated in patients with atopic dermatitis (or eczema). OX40 is involved in activation of immune molecules associated with allergy and atopy, and also with formation of memory immune cells that are required for disease recurrence. The hypothesis to the study was that giving an OX40 antagonist will not only ameliorate the disease but perhaps have a remittive effect in that the disease will not come back.
Indeed all drug doses were significantly effective at week 16, the primary endpoint compared to placebo and continued to improve towards week 36, the secondary endpoint. In addition, the responders to treatment maintained their responses for an additional 20 weeks, which is unusual, suggesting a potential for disease modification.
Abuse and Neglect, Author Interviews, Dermatology, JAMA, Pediatrics / 27.03.2022
Atopic Dermatitis and Growth Parameters in Children
MedicalResearch.com Interview with:
[caption id="attachment_58947" align="alignleft" width="150"] Dr. Drucker[/caption]
Aaron Drucker MD, ScM, FRCPC
Division of Dermatology, Department of Medicine, Women’s College Hospital
Scientist, Women’s College Research Institute
Assistant Professor, Department of Medicin and Institute of Health Policy, Management and Evaluation
University of Toronto
Adjunct Scientist, ICES
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Because atopic dermatitis is a chronic condition that is common in children, parents and physicians often wonder if it will affect overall child well-being, including their growth parameters. Previous studies were mostly cross-sectional, so we conducted a longitudinal study to follow children over time.
We found that although young children with atopic dermatitis were somewhat shorter with higher BMI than children without atopic dermatitis, these differences were small and attenuated as children grew older.
Dr. Drucker[/caption]
Aaron Drucker MD, ScM, FRCPC
Division of Dermatology, Department of Medicine, Women’s College Hospital
Scientist, Women’s College Research Institute
Assistant Professor, Department of Medicin and Institute of Health Policy, Management and Evaluation
University of Toronto
Adjunct Scientist, ICES
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Because atopic dermatitis is a chronic condition that is common in children, parents and physicians often wonder if it will affect overall child well-being, including their growth parameters. Previous studies were mostly cross-sectional, so we conducted a longitudinal study to follow children over time.
We found that although young children with atopic dermatitis were somewhat shorter with higher BMI than children without atopic dermatitis, these differences were small and attenuated as children grew older.
 Dr. Drucker[/caption]
Aaron Drucker MD, ScM, FRCPC
Division of Dermatology, Department of Medicine, Women’s College Hospital
Scientist, Women’s College Research Institute
Assistant Professor, Department of Medicin and Institute of Health Policy, Management and Evaluation
University of Toronto
Adjunct Scientist, ICES
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Because atopic dermatitis is a chronic condition that is common in children, parents and physicians often wonder if it will affect overall child well-being, including their growth parameters. Previous studies were mostly cross-sectional, so we conducted a longitudinal study to follow children over time.
We found that although young children with atopic dermatitis were somewhat shorter with higher BMI than children without atopic dermatitis, these differences were small and attenuated as children grew older.
Dr. Drucker[/caption]
Aaron Drucker MD, ScM, FRCPC
Division of Dermatology, Department of Medicine, Women’s College Hospital
Scientist, Women’s College Research Institute
Assistant Professor, Department of Medicin and Institute of Health Policy, Management and Evaluation
University of Toronto
Adjunct Scientist, ICES
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Because atopic dermatitis is a chronic condition that is common in children, parents and physicians often wonder if it will affect overall child well-being, including their growth parameters. Previous studies were mostly cross-sectional, so we conducted a longitudinal study to follow children over time.
We found that although young children with atopic dermatitis were somewhat shorter with higher BMI than children without atopic dermatitis, these differences were small and attenuated as children grew older.
Author Interviews, Dermatology, Geriatrics, Sleep Disorders / 07.08.2021
Geriatric Patients with Atopic Dermatitis Can Suffer From Sleep Disturbances
MedicalResearch.com Interview with:
[caption id="attachment_24142" align="alignleft" width="128"] Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis affects people of all ages, including geriatric patients. Previous studies found age-related differences in the clinical manifestations of atopic dermatitis between children and adults.
Though, few studies examined whether there are age-related differences of AD severity between geriatric and younger adults. We performed a cross-sectional real-world observational study and found that geriatric age (≥65 years) was not associated with atopic dermatitis severity. However, geriatric age was associated with increased sleep disturbances, delays falling asleep and nighttime awakenings from itch, as well as fatigue.
Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis affects people of all ages, including geriatric patients. Previous studies found age-related differences in the clinical manifestations of atopic dermatitis between children and adults.
Though, few studies examined whether there are age-related differences of AD severity between geriatric and younger adults. We performed a cross-sectional real-world observational study and found that geriatric age (≥65 years) was not associated with atopic dermatitis severity. However, geriatric age was associated with increased sleep disturbances, delays falling asleep and nighttime awakenings from itch, as well as fatigue.
 Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis affects people of all ages, including geriatric patients. Previous studies found age-related differences in the clinical manifestations of atopic dermatitis between children and adults.
Though, few studies examined whether there are age-related differences of AD severity between geriatric and younger adults. We performed a cross-sectional real-world observational study and found that geriatric age (≥65 years) was not associated with atopic dermatitis severity. However, geriatric age was associated with increased sleep disturbances, delays falling asleep and nighttime awakenings from itch, as well as fatigue.
Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis affects people of all ages, including geriatric patients. Previous studies found age-related differences in the clinical manifestations of atopic dermatitis between children and adults.
Though, few studies examined whether there are age-related differences of AD severity between geriatric and younger adults. We performed a cross-sectional real-world observational study and found that geriatric age (≥65 years) was not associated with atopic dermatitis severity. However, geriatric age was associated with increased sleep disturbances, delays falling asleep and nighttime awakenings from itch, as well as fatigue.
Author Interviews, COVID -19 Coronavirus, Dermatology / 11.05.2021
COVID-19: More Hand Scrubbing Linked to Greater Risk of Cracked Dry Hands
MedicalResearch.com Interview with:
Dr Monisha Madhumita
Father Muller Medical College
India
MedicalResearch.com: What is the background for this study?
 Response: The COVID‐19 pandemic requires stringent adoption of hand hygiene practices. Health Care Workers (HCW) and the general population are at increased risk of irritation, dryness, redness and cracked hands (irritant dermatitis) due to frequent hand washing and the use of alcohol-based hand rubs. An effective hand sanitizer contains at least 60% alcohol to kill germs. Thus, it can be very drying to the skin. Transepidermal water loss (TEWL) is a way to measure the water lost from the skin. It is an essential parameter for characterizing skin hydration and protective function. Both of which are disrupted in irritant hand dermatitis.
This research study was conducted on 582 participants: 291 health care workers and 291 healthy individuals of the general population. Measurements of TEWL were made using a noninvasive, closed- chamber system (VapoMeter) in a standardized environment. The study participants were asked to identify the challenges to compliance in hand hygiene practice
Response: The COVID‐19 pandemic requires stringent adoption of hand hygiene practices. Health Care Workers (HCW) and the general population are at increased risk of irritation, dryness, redness and cracked hands (irritant dermatitis) due to frequent hand washing and the use of alcohol-based hand rubs. An effective hand sanitizer contains at least 60% alcohol to kill germs. Thus, it can be very drying to the skin. Transepidermal water loss (TEWL) is a way to measure the water lost from the skin. It is an essential parameter for characterizing skin hydration and protective function. Both of which are disrupted in irritant hand dermatitis.
This research study was conducted on 582 participants: 291 health care workers and 291 healthy individuals of the general population. Measurements of TEWL were made using a noninvasive, closed- chamber system (VapoMeter) in a standardized environment. The study participants were asked to identify the challenges to compliance in hand hygiene practice
 Response: The COVID‐19 pandemic requires stringent adoption of hand hygiene practices. Health Care Workers (HCW) and the general population are at increased risk of irritation, dryness, redness and cracked hands (irritant dermatitis) due to frequent hand washing and the use of alcohol-based hand rubs. An effective hand sanitizer contains at least 60% alcohol to kill germs. Thus, it can be very drying to the skin. Transepidermal water loss (TEWL) is a way to measure the water lost from the skin. It is an essential parameter for characterizing skin hydration and protective function. Both of which are disrupted in irritant hand dermatitis.
This research study was conducted on 582 participants: 291 health care workers and 291 healthy individuals of the general population. Measurements of TEWL were made using a noninvasive, closed- chamber system (VapoMeter) in a standardized environment. The study participants were asked to identify the challenges to compliance in hand hygiene practice
Response: The COVID‐19 pandemic requires stringent adoption of hand hygiene practices. Health Care Workers (HCW) and the general population are at increased risk of irritation, dryness, redness and cracked hands (irritant dermatitis) due to frequent hand washing and the use of alcohol-based hand rubs. An effective hand sanitizer contains at least 60% alcohol to kill germs. Thus, it can be very drying to the skin. Transepidermal water loss (TEWL) is a way to measure the water lost from the skin. It is an essential parameter for characterizing skin hydration and protective function. Both of which are disrupted in irritant hand dermatitis.
This research study was conducted on 582 participants: 291 health care workers and 291 healthy individuals of the general population. Measurements of TEWL were made using a noninvasive, closed- chamber system (VapoMeter) in a standardized environment. The study participants were asked to identify the challenges to compliance in hand hygiene practice
Author Interviews, Microbiome, UCSD / 24.02.2021
Bacteria From Healthy Human Skin Can Be Used to Treat Atopic Dermatitis – Eczema
MedicalResearch.com Interview with:
[caption id="attachment_56783" align="alignleft" width="146"] Dr. Gallo[/caption]
Dr. Richard Gallo, MD, PhD
Ima Gigli Distinguished Professor of Dermatology
Chair of the Department of Dermatology
UC San Diego School of Medicine
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by atopic dermatitis/eczema? How common is it and what are the symptoms.
Response: Atopic Dermatitis is a common inflammatory disease of the skin that appears in up to 20% of children and 3% of the adult population. People suffering from atopic dermatitis have red, itchy skin. In many cases this rash will disrupt sleeping and severely impact quality of life. Also, people with atopic dermatitis are more susceptible to infections of the skin and are more likely to have other allergies and asthma.
Dr. Gallo[/caption]
Dr. Richard Gallo, MD, PhD
Ima Gigli Distinguished Professor of Dermatology
Chair of the Department of Dermatology
UC San Diego School of Medicine
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by atopic dermatitis/eczema? How common is it and what are the symptoms.
Response: Atopic Dermatitis is a common inflammatory disease of the skin that appears in up to 20% of children and 3% of the adult population. People suffering from atopic dermatitis have red, itchy skin. In many cases this rash will disrupt sleeping and severely impact quality of life. Also, people with atopic dermatitis are more susceptible to infections of the skin and are more likely to have other allergies and asthma.
 Dr. Gallo[/caption]
Dr. Richard Gallo, MD, PhD
Ima Gigli Distinguished Professor of Dermatology
Chair of the Department of Dermatology
UC San Diego School of Medicine
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by atopic dermatitis/eczema? How common is it and what are the symptoms.
Response: Atopic Dermatitis is a common inflammatory disease of the skin that appears in up to 20% of children and 3% of the adult population. People suffering from atopic dermatitis have red, itchy skin. In many cases this rash will disrupt sleeping and severely impact quality of life. Also, people with atopic dermatitis are more susceptible to infections of the skin and are more likely to have other allergies and asthma.
Dr. Gallo[/caption]
Dr. Richard Gallo, MD, PhD
Ima Gigli Distinguished Professor of Dermatology
Chair of the Department of Dermatology
UC San Diego School of Medicine
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by atopic dermatitis/eczema? How common is it and what are the symptoms.
Response: Atopic Dermatitis is a common inflammatory disease of the skin that appears in up to 20% of children and 3% of the adult population. People suffering from atopic dermatitis have red, itchy skin. In many cases this rash will disrupt sleeping and severely impact quality of life. Also, people with atopic dermatitis are more susceptible to infections of the skin and are more likely to have other allergies and asthma.
Author Interviews, Dermatology / 15.01.2021
New Itch Pathway Helps Explain Why Antihistamines Don’t Always Work
MedicalResearch.com Interview with:
[caption id="attachment_56427" align="alignleft" width="280"] Dr. Kim[/caption]
Brian Kim, MD
Associate Professor of Dermatology
Co-Director, Center for the Study of Itch & Sensory Disorders
John T. Milliken Department of Internal Medicine
Washington University in St. Louis
MedicalResearch.com: What is the background for this study?
Response: Patients with eczema suffer from chronic itch due to the rashes they have on their body. However, as a physician, I have always noticed that patients with eczema will have sudden flares of their itching all over there body that is often triggered by what appear to be allergens – being around a cat, pollen, mold in a house, etc. Eczema is in the family of allergic diseases such as food allergy, asthma, and hay fever. All of these conditions are noted for patients being reactive to allergens by way of an antibody called IgE that coats a cell called the mast cell. Upon IgE binding an allergen, mast cells produce tons of histamine which can cause symptoms like itching. So we speculated that perhaps because patients with eczema have such misbehaving IgE, that exposure to allergen is what triggers this kind of severe itch flare that we see in patients.
Dr. Kim[/caption]
Brian Kim, MD
Associate Professor of Dermatology
Co-Director, Center for the Study of Itch & Sensory Disorders
John T. Milliken Department of Internal Medicine
Washington University in St. Louis
MedicalResearch.com: What is the background for this study?
Response: Patients with eczema suffer from chronic itch due to the rashes they have on their body. However, as a physician, I have always noticed that patients with eczema will have sudden flares of their itching all over there body that is often triggered by what appear to be allergens – being around a cat, pollen, mold in a house, etc. Eczema is in the family of allergic diseases such as food allergy, asthma, and hay fever. All of these conditions are noted for patients being reactive to allergens by way of an antibody called IgE that coats a cell called the mast cell. Upon IgE binding an allergen, mast cells produce tons of histamine which can cause symptoms like itching. So we speculated that perhaps because patients with eczema have such misbehaving IgE, that exposure to allergen is what triggers this kind of severe itch flare that we see in patients.
 Dr. Kim[/caption]
Brian Kim, MD
Associate Professor of Dermatology
Co-Director, Center for the Study of Itch & Sensory Disorders
John T. Milliken Department of Internal Medicine
Washington University in St. Louis
MedicalResearch.com: What is the background for this study?
Response: Patients with eczema suffer from chronic itch due to the rashes they have on their body. However, as a physician, I have always noticed that patients with eczema will have sudden flares of their itching all over there body that is often triggered by what appear to be allergens – being around a cat, pollen, mold in a house, etc. Eczema is in the family of allergic diseases such as food allergy, asthma, and hay fever. All of these conditions are noted for patients being reactive to allergens by way of an antibody called IgE that coats a cell called the mast cell. Upon IgE binding an allergen, mast cells produce tons of histamine which can cause symptoms like itching. So we speculated that perhaps because patients with eczema have such misbehaving IgE, that exposure to allergen is what triggers this kind of severe itch flare that we see in patients.
Dr. Kim[/caption]
Brian Kim, MD
Associate Professor of Dermatology
Co-Director, Center for the Study of Itch & Sensory Disorders
John T. Milliken Department of Internal Medicine
Washington University in St. Louis
MedicalResearch.com: What is the background for this study?
Response: Patients with eczema suffer from chronic itch due to the rashes they have on their body. However, as a physician, I have always noticed that patients with eczema will have sudden flares of their itching all over there body that is often triggered by what appear to be allergens – being around a cat, pollen, mold in a house, etc. Eczema is in the family of allergic diseases such as food allergy, asthma, and hay fever. All of these conditions are noted for patients being reactive to allergens by way of an antibody called IgE that coats a cell called the mast cell. Upon IgE binding an allergen, mast cells produce tons of histamine which can cause symptoms like itching. So we speculated that perhaps because patients with eczema have such misbehaving IgE, that exposure to allergen is what triggers this kind of severe itch flare that we see in patients.
Allergies, Author Interviews, Dermatology / 06.12.2020
Hand Eczema: Patch Testing Important in Diagnosis of Potential Allergens
MedicalResearch.com Interview with:
[caption id="attachment_24142" align="alignleft" width="128"] Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study
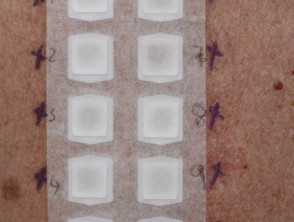
Response: Chronic hand eczema was previously shown to be associated with higher rates of allergic contact dermatitis. Yet, little is known about recent trends in North America with respect to the clinical presentation and allergen profile in chronic hand eczema. This study sought to determine the clinical characteristics and etiologies of hand eczema in a large North American cohort of adults referred for patch testing. The patients in the study were patch tested using the North American Contact Dermatitis Group’s allergen screening series.
Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study
Response: Chronic hand eczema was previously shown to be associated with higher rates of allergic contact dermatitis. Yet, little is known about recent trends in North America with respect to the clinical presentation and allergen profile in chronic hand eczema. This study sought to determine the clinical characteristics and etiologies of hand eczema in a large North American cohort of adults referred for patch testing. The patients in the study were patch tested using the North American Contact Dermatitis Group’s allergen screening series.
 Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study
Response: Chronic hand eczema was previously shown to be associated with higher rates of allergic contact dermatitis. Yet, little is known about recent trends in North America with respect to the clinical presentation and allergen profile in chronic hand eczema. This study sought to determine the clinical characteristics and etiologies of hand eczema in a large North American cohort of adults referred for patch testing. The patients in the study were patch tested using the North American Contact Dermatitis Group’s allergen screening series.
Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study
Response: Chronic hand eczema was previously shown to be associated with higher rates of allergic contact dermatitis. Yet, little is known about recent trends in North America with respect to the clinical presentation and allergen profile in chronic hand eczema. This study sought to determine the clinical characteristics and etiologies of hand eczema in a large North American cohort of adults referred for patch testing. The patients in the study were patch tested using the North American Contact Dermatitis Group’s allergen screening series.
Author Interviews, Brigham & Women's - Harvard, Cancer Research, Dermatology, JAMA / 14.08.2020
Atopic Dermatitis: No Link Found Between Topical Calcineurin Inhibitor Use and Non-Melanoma Skin Cancer
MedicalResearch.com Interview with:
[caption id="attachment_55124" align="alignleft" width="160"] Dr. Asgari[/caption]
Maryam M. Asgari, MD MPH
Professor
Department of Dermatology, Massachusetts General Hospital
Department of Population Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study? What are Topical Calcineurin Inhibitors used for?
Response: Topical calcineurin inhibitors (TCIs) are FDA approved for the treatment of atopic dermatitis (though they are used off-label to treat a wide range of inflammatory conditions of the skin, including psoriasis, seborrheic dermatitis, and contact dermatitis). There are currently two drugs available – tacrolimus and pimecrolimus – both of which carry a black box label warning users about the potential for increased skin cancer risk. The risk associated with keratinocyte carcinoma, the most common cancer (defined as basal cell carcinoma and squamous cell carcinoma), remains poorly defined because findings from large-scale post-marketing surveillance studies are lacking.
Dr. Asgari[/caption]
Maryam M. Asgari, MD MPH
Professor
Department of Dermatology, Massachusetts General Hospital
Department of Population Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study? What are Topical Calcineurin Inhibitors used for?
Response: Topical calcineurin inhibitors (TCIs) are FDA approved for the treatment of atopic dermatitis (though they are used off-label to treat a wide range of inflammatory conditions of the skin, including psoriasis, seborrheic dermatitis, and contact dermatitis). There are currently two drugs available – tacrolimus and pimecrolimus – both of which carry a black box label warning users about the potential for increased skin cancer risk. The risk associated with keratinocyte carcinoma, the most common cancer (defined as basal cell carcinoma and squamous cell carcinoma), remains poorly defined because findings from large-scale post-marketing surveillance studies are lacking.
 Dr. Asgari[/caption]
Maryam M. Asgari, MD MPH
Professor
Department of Dermatology, Massachusetts General Hospital
Department of Population Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study? What are Topical Calcineurin Inhibitors used for?
Response: Topical calcineurin inhibitors (TCIs) are FDA approved for the treatment of atopic dermatitis (though they are used off-label to treat a wide range of inflammatory conditions of the skin, including psoriasis, seborrheic dermatitis, and contact dermatitis). There are currently two drugs available – tacrolimus and pimecrolimus – both of which carry a black box label warning users about the potential for increased skin cancer risk. The risk associated with keratinocyte carcinoma, the most common cancer (defined as basal cell carcinoma and squamous cell carcinoma), remains poorly defined because findings from large-scale post-marketing surveillance studies are lacking.
Dr. Asgari[/caption]
Maryam M. Asgari, MD MPH
Professor
Department of Dermatology, Massachusetts General Hospital
Department of Population Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study? What are Topical Calcineurin Inhibitors used for?
Response: Topical calcineurin inhibitors (TCIs) are FDA approved for the treatment of atopic dermatitis (though they are used off-label to treat a wide range of inflammatory conditions of the skin, including psoriasis, seborrheic dermatitis, and contact dermatitis). There are currently two drugs available – tacrolimus and pimecrolimus – both of which carry a black box label warning users about the potential for increased skin cancer risk. The risk associated with keratinocyte carcinoma, the most common cancer (defined as basal cell carcinoma and squamous cell carcinoma), remains poorly defined because findings from large-scale post-marketing surveillance studies are lacking.
Author Interviews, Dermatology, FDA, Regeneron, Sanofi / 31.07.2020
FDA Approves Dupixent® (dupilumab) Pre-Filled Pen For All Indications in Patients Aged 12 Years and Older
MedicalResearch.com Interview with:
Elizabeth Laws, PhD
Vice President and Global Project Head for Dupilumab/Dupixent
Sanofi
Marcie Ruddy, MD, MA
Strategic Program Direction, Immunology and Inflammation
Regeneron
Dr. Laws and Dr. Ruddy discuss the FDA approval of a 300 mg single-dose pre-filled pen for Dupixent® (dupilumab) for all indications in patients aged 12 years and older.
[caption id="attachment_54997" align="alignleft" width="200"] Dupixent is a biologic therapy that works differently from existing therapies that treat atopic diseases[/caption]
MedicalResearch.com: What is the background for this announcement? What are the main indications for Dupixent?
Response: Until now, Dupixent 300 mg dose was available only in pre-filled syringe for administration. The approval of the pre-filled pen provides an additional, easy-to-use option for patients to self-administer Dupixent.
Dupixent is approved to treat patients aged 6 years and older with uncontrolled moderate-to-severe atopic dermatitis (AD) and can be used with or without topical treatments. Dupixent is also approved for use with other medicines for the maintenance treatment of uncontrolled moderate-to-severe eosinophilic or oral steroid dependent asthma in patients aged 12 years and older, and with other medicines for the maintenance treatment of uncontrolled chronic rhinosinusitis with nasal polyposis (CRSwNP) in adults, respectively.
The pre-filled pen is approved for use in patients prescribed Dupixent who are 12 years of age and older across current indications, at the 300 mg dose.
Dupixent is a biologic therapy that works differently from existing therapies that treat atopic diseases[/caption]
MedicalResearch.com: What is the background for this announcement? What are the main indications for Dupixent?
Response: Until now, Dupixent 300 mg dose was available only in pre-filled syringe for administration. The approval of the pre-filled pen provides an additional, easy-to-use option for patients to self-administer Dupixent.
Dupixent is approved to treat patients aged 6 years and older with uncontrolled moderate-to-severe atopic dermatitis (AD) and can be used with or without topical treatments. Dupixent is also approved for use with other medicines for the maintenance treatment of uncontrolled moderate-to-severe eosinophilic or oral steroid dependent asthma in patients aged 12 years and older, and with other medicines for the maintenance treatment of uncontrolled chronic rhinosinusitis with nasal polyposis (CRSwNP) in adults, respectively.
The pre-filled pen is approved for use in patients prescribed Dupixent who are 12 years of age and older across current indications, at the 300 mg dose.
 Dupixent is a biologic therapy that works differently from existing therapies that treat atopic diseases[/caption]
MedicalResearch.com: What is the background for this announcement? What are the main indications for Dupixent?
Response: Until now, Dupixent 300 mg dose was available only in pre-filled syringe for administration. The approval of the pre-filled pen provides an additional, easy-to-use option for patients to self-administer Dupixent.
Dupixent is approved to treat patients aged 6 years and older with uncontrolled moderate-to-severe atopic dermatitis (AD) and can be used with or without topical treatments. Dupixent is also approved for use with other medicines for the maintenance treatment of uncontrolled moderate-to-severe eosinophilic or oral steroid dependent asthma in patients aged 12 years and older, and with other medicines for the maintenance treatment of uncontrolled chronic rhinosinusitis with nasal polyposis (CRSwNP) in adults, respectively.
The pre-filled pen is approved for use in patients prescribed Dupixent who are 12 years of age and older across current indications, at the 300 mg dose.
Dupixent is a biologic therapy that works differently from existing therapies that treat atopic diseases[/caption]
MedicalResearch.com: What is the background for this announcement? What are the main indications for Dupixent?
Response: Until now, Dupixent 300 mg dose was available only in pre-filled syringe for administration. The approval of the pre-filled pen provides an additional, easy-to-use option for patients to self-administer Dupixent.
Dupixent is approved to treat patients aged 6 years and older with uncontrolled moderate-to-severe atopic dermatitis (AD) and can be used with or without topical treatments. Dupixent is also approved for use with other medicines for the maintenance treatment of uncontrolled moderate-to-severe eosinophilic or oral steroid dependent asthma in patients aged 12 years and older, and with other medicines for the maintenance treatment of uncontrolled chronic rhinosinusitis with nasal polyposis (CRSwNP) in adults, respectively.
The pre-filled pen is approved for use in patients prescribed Dupixent who are 12 years of age and older across current indications, at the 300 mg dose.
Allergies, Author Interviews, Dermatology, Pediatrics / 25.07.2020
Allergenic Potential of Eczema Moisturizers
MedicalResearch.com Interview with:
[caption id="attachment_54947" align="alignleft" width="177"] Catherine M. Ludwig[/caption]
Catherine M. Ludwig is a 4th year medical student at the University of Illinois Chicago College of Medicine.
Her interests in dermatology include inflammatory and genetic conditions, especially within pediatric dermatology.
[caption id="attachment_54948" align="alignleft" width="163"]
Catherine M. Ludwig[/caption]
Catherine M. Ludwig is a 4th year medical student at the University of Illinois Chicago College of Medicine.
Her interests in dermatology include inflammatory and genetic conditions, especially within pediatric dermatology.
[caption id="attachment_54948" align="alignleft" width="163"] Alyssa M. Thompson[/caption]
Alyssa M. Thompson is currently a 2nd year medical student at the UA-COM Tucson. She graduated from the University of Arizona, Summa Cum Laude in 2018 as the athletic department's Valedictorian with a degree in Physiology and an Entrepreneurship certificate. Her passion for research and dermatology stems from her innovative and integrative mindset with specific interest in inflammatory skin disease.
MedicalResearch.com: What is the background for this study?
Response: Eczema is very common in children. Prescription medications are important for managing eczema flares, but a lot of the work in treating eczema is preventative, done by consistently moisturizing the skin at home with drug store products. Allergic contact dermatitis occurs more commonly in people with eczema. A previous study was done in characterizing the allergenic potential of drug-store moisturizers and found that 88% of moisturizers contain at least one common allergen. Many moisturizers are marketed specifically to eczema, but the allergen content of these products are unknown.
Alyssa M. Thompson[/caption]
Alyssa M. Thompson is currently a 2nd year medical student at the UA-COM Tucson. She graduated from the University of Arizona, Summa Cum Laude in 2018 as the athletic department's Valedictorian with a degree in Physiology and an Entrepreneurship certificate. Her passion for research and dermatology stems from her innovative and integrative mindset with specific interest in inflammatory skin disease.
MedicalResearch.com: What is the background for this study?
Response: Eczema is very common in children. Prescription medications are important for managing eczema flares, but a lot of the work in treating eczema is preventative, done by consistently moisturizing the skin at home with drug store products. Allergic contact dermatitis occurs more commonly in people with eczema. A previous study was done in characterizing the allergenic potential of drug-store moisturizers and found that 88% of moisturizers contain at least one common allergen. Many moisturizers are marketed specifically to eczema, but the allergen content of these products are unknown.
 Catherine M. Ludwig[/caption]
Catherine M. Ludwig is a 4th year medical student at the University of Illinois Chicago College of Medicine.
Her interests in dermatology include inflammatory and genetic conditions, especially within pediatric dermatology.
[caption id="attachment_54948" align="alignleft" width="163"]
Catherine M. Ludwig[/caption]
Catherine M. Ludwig is a 4th year medical student at the University of Illinois Chicago College of Medicine.
Her interests in dermatology include inflammatory and genetic conditions, especially within pediatric dermatology.
[caption id="attachment_54948" align="alignleft" width="163"] Alyssa M. Thompson[/caption]
Alyssa M. Thompson is currently a 2nd year medical student at the UA-COM Tucson. She graduated from the University of Arizona, Summa Cum Laude in 2018 as the athletic department's Valedictorian with a degree in Physiology and an Entrepreneurship certificate. Her passion for research and dermatology stems from her innovative and integrative mindset with specific interest in inflammatory skin disease.
MedicalResearch.com: What is the background for this study?
Response: Eczema is very common in children. Prescription medications are important for managing eczema flares, but a lot of the work in treating eczema is preventative, done by consistently moisturizing the skin at home with drug store products. Allergic contact dermatitis occurs more commonly in people with eczema. A previous study was done in characterizing the allergenic potential of drug-store moisturizers and found that 88% of moisturizers contain at least one common allergen. Many moisturizers are marketed specifically to eczema, but the allergen content of these products are unknown.
Alyssa M. Thompson[/caption]
Alyssa M. Thompson is currently a 2nd year medical student at the UA-COM Tucson. She graduated from the University of Arizona, Summa Cum Laude in 2018 as the athletic department's Valedictorian with a degree in Physiology and an Entrepreneurship certificate. Her passion for research and dermatology stems from her innovative and integrative mindset with specific interest in inflammatory skin disease.
MedicalResearch.com: What is the background for this study?
Response: Eczema is very common in children. Prescription medications are important for managing eczema flares, but a lot of the work in treating eczema is preventative, done by consistently moisturizing the skin at home with drug store products. Allergic contact dermatitis occurs more commonly in people with eczema. A previous study was done in characterizing the allergenic potential of drug-store moisturizers and found that 88% of moisturizers contain at least one common allergen. Many moisturizers are marketed specifically to eczema, but the allergen content of these products are unknown.
Author Interviews, Dermatology, Pediatrics / 25.07.2020
Race and Atopic Dermatitis During Early Childhood
MedicalResearch.com Interview with:
[caption id="attachment_54941" align="alignleft" width="133"] Dr. Schoch[/caption]
Jennifer Schoch, MD
Dr. Schoch is a pediatric dermatologist and
Associate Professor of Dermatology at the University of Florida.
Her research focuses on the infantile skin microbiome and its role in pediatric skin disease.
She is a member of the Society for Pediatric Dermatology.
[caption id="attachment_54942" align="alignleft" width="144"]
Dr. Schoch[/caption]
Jennifer Schoch, MD
Dr. Schoch is a pediatric dermatologist and
Associate Professor of Dermatology at the University of Florida.
Her research focuses on the infantile skin microbiome and its role in pediatric skin disease.
She is a member of the Society for Pediatric Dermatology.
[caption id="attachment_54942" align="alignleft" width="144"] Dr. Monir[/caption]
Reesa Monir, MD
Dr. Monir is a PGY-3 dermatology resident at the University of Florida.
She plans to pursue a career in pediatric dermatology.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Atopic dermatitis is a common pediatric skin condition that often begins during infancy. Kids and families alike suffer from the itching and demanding care required to manage this condition. While existing studies have examined the impact of race on atopic dermatitis from birth to adulthood, few studies have examined the early childhood period specifically.
As this time is the peak period for diagnosis, we sought to examine the impact of race on disease prevalence during early childhood.
Dr. Monir[/caption]
Reesa Monir, MD
Dr. Monir is a PGY-3 dermatology resident at the University of Florida.
She plans to pursue a career in pediatric dermatology.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Atopic dermatitis is a common pediatric skin condition that often begins during infancy. Kids and families alike suffer from the itching and demanding care required to manage this condition. While existing studies have examined the impact of race on atopic dermatitis from birth to adulthood, few studies have examined the early childhood period specifically.
As this time is the peak period for diagnosis, we sought to examine the impact of race on disease prevalence during early childhood.
 Dr. Schoch[/caption]
Jennifer Schoch, MD
Dr. Schoch is a pediatric dermatologist and
Associate Professor of Dermatology at the University of Florida.
Her research focuses on the infantile skin microbiome and its role in pediatric skin disease.
She is a member of the Society for Pediatric Dermatology.
[caption id="attachment_54942" align="alignleft" width="144"]
Dr. Schoch[/caption]
Jennifer Schoch, MD
Dr. Schoch is a pediatric dermatologist and
Associate Professor of Dermatology at the University of Florida.
Her research focuses on the infantile skin microbiome and its role in pediatric skin disease.
She is a member of the Society for Pediatric Dermatology.
[caption id="attachment_54942" align="alignleft" width="144"] Dr. Monir[/caption]
Reesa Monir, MD
Dr. Monir is a PGY-3 dermatology resident at the University of Florida.
She plans to pursue a career in pediatric dermatology.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Atopic dermatitis is a common pediatric skin condition that often begins during infancy. Kids and families alike suffer from the itching and demanding care required to manage this condition. While existing studies have examined the impact of race on atopic dermatitis from birth to adulthood, few studies have examined the early childhood period specifically.
As this time is the peak period for diagnosis, we sought to examine the impact of race on disease prevalence during early childhood.
Dr. Monir[/caption]
Reesa Monir, MD
Dr. Monir is a PGY-3 dermatology resident at the University of Florida.
She plans to pursue a career in pediatric dermatology.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Atopic dermatitis is a common pediatric skin condition that often begins during infancy. Kids and families alike suffer from the itching and demanding care required to manage this condition. While existing studies have examined the impact of race on atopic dermatitis from birth to adulthood, few studies have examined the early childhood period specifically.
As this time is the peak period for diagnosis, we sought to examine the impact of race on disease prevalence during early childhood.
Allergies, Author Interviews, Dermatology / 22.07.2020
Non-Invasive Skin Biopsy Can Distinguish Eczema from Psoriasis
MedicalResearch.com Interview with:
[caption id="attachment_13209" align="alignleft" width="130"] Dr. Guttman-Yassky[/caption]
Emma Guttman-Yassky, MD, PhD
Professor of Dermatology and Immunology
Vice Chair of the Department of Dermatology
Icahn School of Medicine
MedicalResearch.com: What is the background for this study? What is the importance of differentiating these two skin conditions?
Response: The background is that up to now skin biopsies were considered the gold standard for obtaining skin biomarkers of atopic dermatitis/AD and psoriasis that are linked to disease activity in skin and for obtaining the cutaneous gene and protein expression fingerprint of each individual disease. Biopsies are also used in clinical trials to obtain the skin phenotype. However biopsies are invasive, painful and scarring. Thus we need less invasive means to profile diseases and obtain biomarkers. Tape strips is a minimally invasive approach to sample and study the skin. However, prior studies using tape strips could not fully capture the phenotype of the diseases and also sampling the recovery rate was less than optimal, not allowing this approach to be widely used. Psoriasis and AD are the most common inflammatory skin diseases, but these diseases are treated very differently and in some cases are very difficult to differentiate between them clinically and even in biopsies.
Dr. Guttman-Yassky[/caption]
Emma Guttman-Yassky, MD, PhD
Professor of Dermatology and Immunology
Vice Chair of the Department of Dermatology
Icahn School of Medicine
MedicalResearch.com: What is the background for this study? What is the importance of differentiating these two skin conditions?
Response: The background is that up to now skin biopsies were considered the gold standard for obtaining skin biomarkers of atopic dermatitis/AD and psoriasis that are linked to disease activity in skin and for obtaining the cutaneous gene and protein expression fingerprint of each individual disease. Biopsies are also used in clinical trials to obtain the skin phenotype. However biopsies are invasive, painful and scarring. Thus we need less invasive means to profile diseases and obtain biomarkers. Tape strips is a minimally invasive approach to sample and study the skin. However, prior studies using tape strips could not fully capture the phenotype of the diseases and also sampling the recovery rate was less than optimal, not allowing this approach to be widely used. Psoriasis and AD are the most common inflammatory skin diseases, but these diseases are treated very differently and in some cases are very difficult to differentiate between them clinically and even in biopsies.
 Dr. Guttman-Yassky[/caption]
Emma Guttman-Yassky, MD, PhD
Professor of Dermatology and Immunology
Vice Chair of the Department of Dermatology
Icahn School of Medicine
MedicalResearch.com: What is the background for this study? What is the importance of differentiating these two skin conditions?
Response: The background is that up to now skin biopsies were considered the gold standard for obtaining skin biomarkers of atopic dermatitis/AD and psoriasis that are linked to disease activity in skin and for obtaining the cutaneous gene and protein expression fingerprint of each individual disease. Biopsies are also used in clinical trials to obtain the skin phenotype. However biopsies are invasive, painful and scarring. Thus we need less invasive means to profile diseases and obtain biomarkers. Tape strips is a minimally invasive approach to sample and study the skin. However, prior studies using tape strips could not fully capture the phenotype of the diseases and also sampling the recovery rate was less than optimal, not allowing this approach to be widely used. Psoriasis and AD are the most common inflammatory skin diseases, but these diseases are treated very differently and in some cases are very difficult to differentiate between them clinically and even in biopsies.
Dr. Guttman-Yassky[/caption]
Emma Guttman-Yassky, MD, PhD
Professor of Dermatology and Immunology
Vice Chair of the Department of Dermatology
Icahn School of Medicine
MedicalResearch.com: What is the background for this study? What is the importance of differentiating these two skin conditions?
Response: The background is that up to now skin biopsies were considered the gold standard for obtaining skin biomarkers of atopic dermatitis/AD and psoriasis that are linked to disease activity in skin and for obtaining the cutaneous gene and protein expression fingerprint of each individual disease. Biopsies are also used in clinical trials to obtain the skin phenotype. However biopsies are invasive, painful and scarring. Thus we need less invasive means to profile diseases and obtain biomarkers. Tape strips is a minimally invasive approach to sample and study the skin. However, prior studies using tape strips could not fully capture the phenotype of the diseases and also sampling the recovery rate was less than optimal, not allowing this approach to be widely used. Psoriasis and AD are the most common inflammatory skin diseases, but these diseases are treated very differently and in some cases are very difficult to differentiate between them clinically and even in biopsies.
Author Interviews, Dermatology / 25.06.2020
Atopic Dermatitis: Study Finds Monoclonal Antibody Tralokinumab + Topical Steroids Effective for Moderate to Severe Disease
MedicalResearch.com Interview with:
[caption id="attachment_24142" align="alignleft" width="128"] Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Assistant Professor in Dermatology
Medical Social Sciences and Preventive Medicine
Northwestern, Chicago, Illinois
MedicalResearch.com: What is the background for this study?
Response: Topical anti-inflammatory therapy is often inadequate to achieve disease control in patients with moderate-to-severe atopic dermatitis (AD), and systemic therapy is often warranted. Tralokinumab is a fully human immunoglobulin G4 monoclonal antibody that specifically binds to the IL-13 cytokine with high affinity and inhibits downstream IL-13 pro-inflammatory signaling.
Tralokinumab was previously studied as a monotherapy in moderate-severe AD in the ECZTRA1 and ECZTRA2 studies. In this Phase 3 randomized controlled study, ECZTRA3, tralokinumab was studies in combination with topical corticosteroids compared to placebo with topical corticosteroids. The use of topical anti-inflammatory therapy is more akin to the way in which systemic and biologic therapies are typically used in the real-world.
Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Assistant Professor in Dermatology
Medical Social Sciences and Preventive Medicine
Northwestern, Chicago, Illinois
MedicalResearch.com: What is the background for this study?
Response: Topical anti-inflammatory therapy is often inadequate to achieve disease control in patients with moderate-to-severe atopic dermatitis (AD), and systemic therapy is often warranted. Tralokinumab is a fully human immunoglobulin G4 monoclonal antibody that specifically binds to the IL-13 cytokine with high affinity and inhibits downstream IL-13 pro-inflammatory signaling.
Tralokinumab was previously studied as a monotherapy in moderate-severe AD in the ECZTRA1 and ECZTRA2 studies. In this Phase 3 randomized controlled study, ECZTRA3, tralokinumab was studies in combination with topical corticosteroids compared to placebo with topical corticosteroids. The use of topical anti-inflammatory therapy is more akin to the way in which systemic and biologic therapies are typically used in the real-world.
 Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Assistant Professor in Dermatology
Medical Social Sciences and Preventive Medicine
Northwestern, Chicago, Illinois
MedicalResearch.com: What is the background for this study?
Response: Topical anti-inflammatory therapy is often inadequate to achieve disease control in patients with moderate-to-severe atopic dermatitis (AD), and systemic therapy is often warranted. Tralokinumab is a fully human immunoglobulin G4 monoclonal antibody that specifically binds to the IL-13 cytokine with high affinity and inhibits downstream IL-13 pro-inflammatory signaling.
Tralokinumab was previously studied as a monotherapy in moderate-severe AD in the ECZTRA1 and ECZTRA2 studies. In this Phase 3 randomized controlled study, ECZTRA3, tralokinumab was studies in combination with topical corticosteroids compared to placebo with topical corticosteroids. The use of topical anti-inflammatory therapy is more akin to the way in which systemic and biologic therapies are typically used in the real-world.
Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Assistant Professor in Dermatology
Medical Social Sciences and Preventive Medicine
Northwestern, Chicago, Illinois
MedicalResearch.com: What is the background for this study?
Response: Topical anti-inflammatory therapy is often inadequate to achieve disease control in patients with moderate-to-severe atopic dermatitis (AD), and systemic therapy is often warranted. Tralokinumab is a fully human immunoglobulin G4 monoclonal antibody that specifically binds to the IL-13 cytokine with high affinity and inhibits downstream IL-13 pro-inflammatory signaling.
Tralokinumab was previously studied as a monotherapy in moderate-severe AD in the ECZTRA1 and ECZTRA2 studies. In this Phase 3 randomized controlled study, ECZTRA3, tralokinumab was studies in combination with topical corticosteroids compared to placebo with topical corticosteroids. The use of topical anti-inflammatory therapy is more akin to the way in which systemic and biologic therapies are typically used in the real-world.
Author Interviews, Dermatology, Regeneron / 23.06.2020
Atopic Dermatitis – Eczema: Dupilumab plus Topical Corticosteroids Improved Symptoms and Quality of Life in Children with Severe Disease
MedicalResearch.com Interview with:
[caption id="attachment_54684" align="alignleft" width="125"] Dr. Shumel[/caption]
Brad Shumel, MD
Senior Director of Medical Affairs, Immunology
Regeneron
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis is a chronic inflammatory disease and one of the most common skin disorders in children. Severe atopic dermatitis is characterized by skin lesions that often cover a large body surface area and can include intense, persistent itch. Uncontrolled moderate-to-severe atopic dermatitis can have a physical, emotional and psychosocial impact on children, resulting in sleep deprivation, activity restriction, poor school performance, depression and anxiety that can have a greater impact on quality-of-life.
The standard of care for this pediatric population has been topical corticosteroids. Children with severe atopic dermatitis who remain uncontrolled with topical therapies have limited treatment options.
This Phase 3 trial was conducted to evaluate the safety and efficacy of dupilumab plus topical corticosteroids (TCS) compared with TCS alone in children with uncontrolled severe atopic dermatitis across two treatment arms – every four weeks and every two weeks (Q4W and Q2W).
Dr. Shumel[/caption]
Brad Shumel, MD
Senior Director of Medical Affairs, Immunology
Regeneron
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis is a chronic inflammatory disease and one of the most common skin disorders in children. Severe atopic dermatitis is characterized by skin lesions that often cover a large body surface area and can include intense, persistent itch. Uncontrolled moderate-to-severe atopic dermatitis can have a physical, emotional and psychosocial impact on children, resulting in sleep deprivation, activity restriction, poor school performance, depression and anxiety that can have a greater impact on quality-of-life.
The standard of care for this pediatric population has been topical corticosteroids. Children with severe atopic dermatitis who remain uncontrolled with topical therapies have limited treatment options.
This Phase 3 trial was conducted to evaluate the safety and efficacy of dupilumab plus topical corticosteroids (TCS) compared with TCS alone in children with uncontrolled severe atopic dermatitis across two treatment arms – every four weeks and every two weeks (Q4W and Q2W).
 Dr. Shumel[/caption]
Brad Shumel, MD
Senior Director of Medical Affairs, Immunology
Regeneron
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis is a chronic inflammatory disease and one of the most common skin disorders in children. Severe atopic dermatitis is characterized by skin lesions that often cover a large body surface area and can include intense, persistent itch. Uncontrolled moderate-to-severe atopic dermatitis can have a physical, emotional and psychosocial impact on children, resulting in sleep deprivation, activity restriction, poor school performance, depression and anxiety that can have a greater impact on quality-of-life.
The standard of care for this pediatric population has been topical corticosteroids. Children with severe atopic dermatitis who remain uncontrolled with topical therapies have limited treatment options.
This Phase 3 trial was conducted to evaluate the safety and efficacy of dupilumab plus topical corticosteroids (TCS) compared with TCS alone in children with uncontrolled severe atopic dermatitis across two treatment arms – every four weeks and every two weeks (Q4W and Q2W).
Dr. Shumel[/caption]
Brad Shumel, MD
Senior Director of Medical Affairs, Immunology
Regeneron
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis is a chronic inflammatory disease and one of the most common skin disorders in children. Severe atopic dermatitis is characterized by skin lesions that often cover a large body surface area and can include intense, persistent itch. Uncontrolled moderate-to-severe atopic dermatitis can have a physical, emotional and psychosocial impact on children, resulting in sleep deprivation, activity restriction, poor school performance, depression and anxiety that can have a greater impact on quality-of-life.
The standard of care for this pediatric population has been topical corticosteroids. Children with severe atopic dermatitis who remain uncontrolled with topical therapies have limited treatment options.
This Phase 3 trial was conducted to evaluate the safety and efficacy of dupilumab plus topical corticosteroids (TCS) compared with TCS alone in children with uncontrolled severe atopic dermatitis across two treatment arms – every four weeks and every two weeks (Q4W and Q2W).
Author Interviews, Dermatology / 23.06.2020
Gladskin Treats Atopic Dermatitis – Eczema – by Repairing Skin Microbiome
MedicalResearch.com Interview with:
 Skyler Stein, MBA
President of Gladskin USA
Mr. Stein discusses Gladskin , a new category of non-prescription eczema treatment, utilizing “Micreobalance™ is a smart protein that defends against flare-causing bacteria and creates a healthy environment for good bacteria to thrive”.
Skyler Stein, MBA
President of Gladskin USA
Mr. Stein discusses Gladskin , a new category of non-prescription eczema treatment, utilizing “Micreobalance™ is a smart protein that defends against flare-causing bacteria and creates a healthy environment for good bacteria to thrive”.
 Skyler Stein, MBA
President of Gladskin USA
Mr. Stein discusses Gladskin , a new category of non-prescription eczema treatment, utilizing “Micreobalance™ is a smart protein that defends against flare-causing bacteria and creates a healthy environment for good bacteria to thrive”.
Skyler Stein, MBA
President of Gladskin USA
Mr. Stein discusses Gladskin , a new category of non-prescription eczema treatment, utilizing “Micreobalance™ is a smart protein that defends against flare-causing bacteria and creates a healthy environment for good bacteria to thrive”.
Author Interviews, Dermatology, Pediatrics, Pharmaceutical Companies, Regeneron / 15.06.2020
Biologic Dupixent® Approved for Children with Severe Atopic Dermatitis – Eczema
MedicalResearch.com Interview with:
[caption id="attachment_54575" align="alignleft" width="200"] Dr. Paller[/caption]
Amy S Paller, MD
Chair, Department of Dermatology
Director, Skin Biology and Diseases Resource-Based Center
Walter J. Hamlin Professor of Dermatology
Professor of Dermatology and Pediatrics (Dermatology)
Feinberg School of Medicine
Northwestern University
Dr. Paller discusses the FDA approval of Dupixent® (dupilumab) for children aged 6 to 11 years with moderate-to-severe atopic dermatitis (eczema), whose disease is not adequately controlled with topical prescription therapies or when those therapies are not advisable.
MedicalResearch.com: What is the background for this announcement? Would you briefly discuss what is meant by atopic dermatitis and how it affects children?
Response: “Atopic dermatitis, the most common form of eczema, is a chronic inflammatory disease that often appears as a rash on the skin. Moderate-to-severe atopic dermatitis is characterized by rashes that can potentially cover much of the body and can include intense, persistent itching, skin lesions and skin dryness, cracking, redness or darkness, crusting and oozing. Itch is one of the most burdensome symptoms for patients and can be debilitating.
This recent FDA approval expands the use of Dupilumab in the U.S. to include children aged 6 to 11 years with uncontrolled moderate-to-severe atopic dermatitis, making it the only biologic medicine approved for this use in this population. Dupilumab is also approved in the U.S. to treat patients aged 12 years and older with moderate-to-severe atopic dermatitis.
Moderate-to-severe atopic dermatitis can place a particularly substantial burden on young children aged 6 to 11 years and their families. Limited treatment options leave many of these children to cope with intense, unrelenting itch and skin lesions. Families of these children can spend countless hours helping them to manage their disease.”
Dr. Paller[/caption]
Amy S Paller, MD
Chair, Department of Dermatology
Director, Skin Biology and Diseases Resource-Based Center
Walter J. Hamlin Professor of Dermatology
Professor of Dermatology and Pediatrics (Dermatology)
Feinberg School of Medicine
Northwestern University
Dr. Paller discusses the FDA approval of Dupixent® (dupilumab) for children aged 6 to 11 years with moderate-to-severe atopic dermatitis (eczema), whose disease is not adequately controlled with topical prescription therapies or when those therapies are not advisable.
MedicalResearch.com: What is the background for this announcement? Would you briefly discuss what is meant by atopic dermatitis and how it affects children?
Response: “Atopic dermatitis, the most common form of eczema, is a chronic inflammatory disease that often appears as a rash on the skin. Moderate-to-severe atopic dermatitis is characterized by rashes that can potentially cover much of the body and can include intense, persistent itching, skin lesions and skin dryness, cracking, redness or darkness, crusting and oozing. Itch is one of the most burdensome symptoms for patients and can be debilitating.
This recent FDA approval expands the use of Dupilumab in the U.S. to include children aged 6 to 11 years with uncontrolled moderate-to-severe atopic dermatitis, making it the only biologic medicine approved for this use in this population. Dupilumab is also approved in the U.S. to treat patients aged 12 years and older with moderate-to-severe atopic dermatitis.
Moderate-to-severe atopic dermatitis can place a particularly substantial burden on young children aged 6 to 11 years and their families. Limited treatment options leave many of these children to cope with intense, unrelenting itch and skin lesions. Families of these children can spend countless hours helping them to manage their disease.”
 Dr. Paller[/caption]
Amy S Paller, MD
Chair, Department of Dermatology
Director, Skin Biology and Diseases Resource-Based Center
Walter J. Hamlin Professor of Dermatology
Professor of Dermatology and Pediatrics (Dermatology)
Feinberg School of Medicine
Northwestern University
Dr. Paller discusses the FDA approval of Dupixent® (dupilumab) for children aged 6 to 11 years with moderate-to-severe atopic dermatitis (eczema), whose disease is not adequately controlled with topical prescription therapies or when those therapies are not advisable.
MedicalResearch.com: What is the background for this announcement? Would you briefly discuss what is meant by atopic dermatitis and how it affects children?
Response: “Atopic dermatitis, the most common form of eczema, is a chronic inflammatory disease that often appears as a rash on the skin. Moderate-to-severe atopic dermatitis is characterized by rashes that can potentially cover much of the body and can include intense, persistent itching, skin lesions and skin dryness, cracking, redness or darkness, crusting and oozing. Itch is one of the most burdensome symptoms for patients and can be debilitating.
This recent FDA approval expands the use of Dupilumab in the U.S. to include children aged 6 to 11 years with uncontrolled moderate-to-severe atopic dermatitis, making it the only biologic medicine approved for this use in this population. Dupilumab is also approved in the U.S. to treat patients aged 12 years and older with moderate-to-severe atopic dermatitis.
Moderate-to-severe atopic dermatitis can place a particularly substantial burden on young children aged 6 to 11 years and their families. Limited treatment options leave many of these children to cope with intense, unrelenting itch and skin lesions. Families of these children can spend countless hours helping them to manage their disease.”
Dr. Paller[/caption]
Amy S Paller, MD
Chair, Department of Dermatology
Director, Skin Biology and Diseases Resource-Based Center
Walter J. Hamlin Professor of Dermatology
Professor of Dermatology and Pediatrics (Dermatology)
Feinberg School of Medicine
Northwestern University
Dr. Paller discusses the FDA approval of Dupixent® (dupilumab) for children aged 6 to 11 years with moderate-to-severe atopic dermatitis (eczema), whose disease is not adequately controlled with topical prescription therapies or when those therapies are not advisable.
MedicalResearch.com: What is the background for this announcement? Would you briefly discuss what is meant by atopic dermatitis and how it affects children?
Response: “Atopic dermatitis, the most common form of eczema, is a chronic inflammatory disease that often appears as a rash on the skin. Moderate-to-severe atopic dermatitis is characterized by rashes that can potentially cover much of the body and can include intense, persistent itching, skin lesions and skin dryness, cracking, redness or darkness, crusting and oozing. Itch is one of the most burdensome symptoms for patients and can be debilitating.
This recent FDA approval expands the use of Dupilumab in the U.S. to include children aged 6 to 11 years with uncontrolled moderate-to-severe atopic dermatitis, making it the only biologic medicine approved for this use in this population. Dupilumab is also approved in the U.S. to treat patients aged 12 years and older with moderate-to-severe atopic dermatitis.
Moderate-to-severe atopic dermatitis can place a particularly substantial burden on young children aged 6 to 11 years and their families. Limited treatment options leave many of these children to cope with intense, unrelenting itch and skin lesions. Families of these children can spend countless hours helping them to manage their disease.”
Author Interviews, Dermatology / 12.06.2020
Atopic Dermatitis- Eczema: New Therapeutic Approach Blocks Protein That Breaks Down Skin Barrier
MedicalResearch.com Interview with:
[caption id="attachment_54528" align="alignleft" width="150"] Dr. Granville[/caption]
David Granville PhD, FAHA
Professor, Pathology and Laboratory Medicine, UBC
Associate Director, Vancouver Coastal Health Research Institute, VGH-UBC
Associate Director, BC Professional Firefighters Burn & Wound Healing Group, Department of Surgery, UBC
Principal Investigator, iCORD and UBC Centre for Heart Lung Innovation
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis (aka. eczema) is a chronic inflammatory skin condition characterized by patches of dry, red, itchy skin. These patches can come and go - a process often referred to as 'flare ups'. Often when these flare ups occur, people avoid going out, or to work, resulting in lost productivity and reduced quality of life. While the cause of these flare-ups is not completely understood, a loss of the skin's protective barrier function is believed to be a triggering event. This is because the outer layer of skin (epidermis) acts as a barrier to allergens and other foreign entities from getting into the skin. When this outer barrier is lost, allergens are able to cross and penetrate the deeper layers of skin. This triggers an inflammatory response. The inflammatory response, in turn, can release factors that cause further disruption of the barrier thereby exacerbating the flare up.
The outer skin barrier can be thought of in terms of a brick wall in which the 'bricks', or skin cells in this case, are held together by a molecular 'grout' known as adhesion proteins. If these adhesion proteins, which tightly anchor the skin cells together, are lost, the skin becomes more permeable to the outer environment, allowing foreign antigens to enter in, and conversely, moisture to escape out resulting in skin dryness and shedding
Dr. Granville[/caption]
David Granville PhD, FAHA
Professor, Pathology and Laboratory Medicine, UBC
Associate Director, Vancouver Coastal Health Research Institute, VGH-UBC
Associate Director, BC Professional Firefighters Burn & Wound Healing Group, Department of Surgery, UBC
Principal Investigator, iCORD and UBC Centre for Heart Lung Innovation
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis (aka. eczema) is a chronic inflammatory skin condition characterized by patches of dry, red, itchy skin. These patches can come and go - a process often referred to as 'flare ups'. Often when these flare ups occur, people avoid going out, or to work, resulting in lost productivity and reduced quality of life. While the cause of these flare-ups is not completely understood, a loss of the skin's protective barrier function is believed to be a triggering event. This is because the outer layer of skin (epidermis) acts as a barrier to allergens and other foreign entities from getting into the skin. When this outer barrier is lost, allergens are able to cross and penetrate the deeper layers of skin. This triggers an inflammatory response. The inflammatory response, in turn, can release factors that cause further disruption of the barrier thereby exacerbating the flare up.
The outer skin barrier can be thought of in terms of a brick wall in which the 'bricks', or skin cells in this case, are held together by a molecular 'grout' known as adhesion proteins. If these adhesion proteins, which tightly anchor the skin cells together, are lost, the skin becomes more permeable to the outer environment, allowing foreign antigens to enter in, and conversely, moisture to escape out resulting in skin dryness and shedding
 Dr. Granville[/caption]
David Granville PhD, FAHA
Professor, Pathology and Laboratory Medicine, UBC
Associate Director, Vancouver Coastal Health Research Institute, VGH-UBC
Associate Director, BC Professional Firefighters Burn & Wound Healing Group, Department of Surgery, UBC
Principal Investigator, iCORD and UBC Centre for Heart Lung Innovation
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis (aka. eczema) is a chronic inflammatory skin condition characterized by patches of dry, red, itchy skin. These patches can come and go - a process often referred to as 'flare ups'. Often when these flare ups occur, people avoid going out, or to work, resulting in lost productivity and reduced quality of life. While the cause of these flare-ups is not completely understood, a loss of the skin's protective barrier function is believed to be a triggering event. This is because the outer layer of skin (epidermis) acts as a barrier to allergens and other foreign entities from getting into the skin. When this outer barrier is lost, allergens are able to cross and penetrate the deeper layers of skin. This triggers an inflammatory response. The inflammatory response, in turn, can release factors that cause further disruption of the barrier thereby exacerbating the flare up.
The outer skin barrier can be thought of in terms of a brick wall in which the 'bricks', or skin cells in this case, are held together by a molecular 'grout' known as adhesion proteins. If these adhesion proteins, which tightly anchor the skin cells together, are lost, the skin becomes more permeable to the outer environment, allowing foreign antigens to enter in, and conversely, moisture to escape out resulting in skin dryness and shedding
Dr. Granville[/caption]
David Granville PhD, FAHA
Professor, Pathology and Laboratory Medicine, UBC
Associate Director, Vancouver Coastal Health Research Institute, VGH-UBC
Associate Director, BC Professional Firefighters Burn & Wound Healing Group, Department of Surgery, UBC
Principal Investigator, iCORD and UBC Centre for Heart Lung Innovation
MedicalResearch.com: What is the background for this study?
Response: Atopic dermatitis (aka. eczema) is a chronic inflammatory skin condition characterized by patches of dry, red, itchy skin. These patches can come and go - a process often referred to as 'flare ups'. Often when these flare ups occur, people avoid going out, or to work, resulting in lost productivity and reduced quality of life. While the cause of these flare-ups is not completely understood, a loss of the skin's protective barrier function is believed to be a triggering event. This is because the outer layer of skin (epidermis) acts as a barrier to allergens and other foreign entities from getting into the skin. When this outer barrier is lost, allergens are able to cross and penetrate the deeper layers of skin. This triggers an inflammatory response. The inflammatory response, in turn, can release factors that cause further disruption of the barrier thereby exacerbating the flare up.
The outer skin barrier can be thought of in terms of a brick wall in which the 'bricks', or skin cells in this case, are held together by a molecular 'grout' known as adhesion proteins. If these adhesion proteins, which tightly anchor the skin cells together, are lost, the skin becomes more permeable to the outer environment, allowing foreign antigens to enter in, and conversely, moisture to escape out resulting in skin dryness and shedding
Author Interviews, Dermatology / 13.05.2020
Atopic Dermatitis – Eczema: Jakafi® (ruxolitinib) Found to Reduce Itch and Improve Quality of Life
MedicalResearch.com Interview with:
[caption id="attachment_54196" align="alignleft" width="145"] Dr. Kim[/caption]
Brian S. Kim, MD, MTR, FAAD
Associate Professor of Medicine (Dermatology)
Co-Director, Center for the Study of Itch and Sensory Disorders
Division of Dermatology, Department of Medicine
Washington University School of Medicine
St. Louis, MO
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Itch is the central and most debilitating symptom of atopic dermatitis. However, surprisingly, measuring itch or quality of life in clinical trials is not often a primary endpoint. Therefore, this study focuses in very detailed fashion on how ruxolitinib cream improves pruritus in a clinically meaningful way and its ultimate impact on quality of life.
What patients want to know at the end of the day is how much will this drug change my life? Not, whether it statistically beat out a placebo group. Indeed, what this study shows is that ruxolitinib cream has a major impact on itch in a meaningful way that is also tied to improvements in quality of life.
Dr. Kim[/caption]
Brian S. Kim, MD, MTR, FAAD
Associate Professor of Medicine (Dermatology)
Co-Director, Center for the Study of Itch and Sensory Disorders
Division of Dermatology, Department of Medicine
Washington University School of Medicine
St. Louis, MO
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Itch is the central and most debilitating symptom of atopic dermatitis. However, surprisingly, measuring itch or quality of life in clinical trials is not often a primary endpoint. Therefore, this study focuses in very detailed fashion on how ruxolitinib cream improves pruritus in a clinically meaningful way and its ultimate impact on quality of life.
What patients want to know at the end of the day is how much will this drug change my life? Not, whether it statistically beat out a placebo group. Indeed, what this study shows is that ruxolitinib cream has a major impact on itch in a meaningful way that is also tied to improvements in quality of life.
 Dr. Kim[/caption]
Brian S. Kim, MD, MTR, FAAD
Associate Professor of Medicine (Dermatology)
Co-Director, Center for the Study of Itch and Sensory Disorders
Division of Dermatology, Department of Medicine
Washington University School of Medicine
St. Louis, MO
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Itch is the central and most debilitating symptom of atopic dermatitis. However, surprisingly, measuring itch or quality of life in clinical trials is not often a primary endpoint. Therefore, this study focuses in very detailed fashion on how ruxolitinib cream improves pruritus in a clinically meaningful way and its ultimate impact on quality of life.
What patients want to know at the end of the day is how much will this drug change my life? Not, whether it statistically beat out a placebo group. Indeed, what this study shows is that ruxolitinib cream has a major impact on itch in a meaningful way that is also tied to improvements in quality of life.
Dr. Kim[/caption]
Brian S. Kim, MD, MTR, FAAD
Associate Professor of Medicine (Dermatology)
Co-Director, Center for the Study of Itch and Sensory Disorders
Division of Dermatology, Department of Medicine
Washington University School of Medicine
St. Louis, MO
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Itch is the central and most debilitating symptom of atopic dermatitis. However, surprisingly, measuring itch or quality of life in clinical trials is not often a primary endpoint. Therefore, this study focuses in very detailed fashion on how ruxolitinib cream improves pruritus in a clinically meaningful way and its ultimate impact on quality of life.
What patients want to know at the end of the day is how much will this drug change my life? Not, whether it statistically beat out a placebo group. Indeed, what this study shows is that ruxolitinib cream has a major impact on itch in a meaningful way that is also tied to improvements in quality of life.
Author Interviews, Dermatology, Neurology / 28.04.2020
Eczema and Psoriasis: Itch Linked to Specific Protein in Skin
MedicalResearch.com Interview with:
[caption id="attachment_54040" align="alignleft" width="200"] Dr. Mishra[/caption]
Santosh K. Mishra M.Tech., PhD
Assistant Professor of Neuroscience
Department of Molecular Biomedical Sciences
NC State Veterinary Medicine
Raleigh, NC 2760
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by atopic dermatitis?
Response: Chronic allergic itch is a worldwide problem that leads to substantial health expenses,but what causes this universal urge to scratch remains elusive in chronic allergic itch. Atopic dermatitis is a common allergic skin disease that often associated with extremely itchy and inflamed skin.
In our study, we showed, for the first time, a molecular pathway that is involved in chronic allergic itch as we identified an endogenous mediator (periostin) and a new role for its sensory neuron receptor, the integrin αVβ3, which drives the excitability and transmission of itch signal to the spinal cord.
Dr. Mishra[/caption]
Santosh K. Mishra M.Tech., PhD
Assistant Professor of Neuroscience
Department of Molecular Biomedical Sciences
NC State Veterinary Medicine
Raleigh, NC 2760
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by atopic dermatitis?
Response: Chronic allergic itch is a worldwide problem that leads to substantial health expenses,but what causes this universal urge to scratch remains elusive in chronic allergic itch. Atopic dermatitis is a common allergic skin disease that often associated with extremely itchy and inflamed skin.
In our study, we showed, for the first time, a molecular pathway that is involved in chronic allergic itch as we identified an endogenous mediator (periostin) and a new role for its sensory neuron receptor, the integrin αVβ3, which drives the excitability and transmission of itch signal to the spinal cord.
 Dr. Mishra[/caption]
Santosh K. Mishra M.Tech., PhD
Assistant Professor of Neuroscience
Department of Molecular Biomedical Sciences
NC State Veterinary Medicine
Raleigh, NC 2760
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by atopic dermatitis?
Response: Chronic allergic itch is a worldwide problem that leads to substantial health expenses,but what causes this universal urge to scratch remains elusive in chronic allergic itch. Atopic dermatitis is a common allergic skin disease that often associated with extremely itchy and inflamed skin.
In our study, we showed, for the first time, a molecular pathway that is involved in chronic allergic itch as we identified an endogenous mediator (periostin) and a new role for its sensory neuron receptor, the integrin αVβ3, which drives the excitability and transmission of itch signal to the spinal cord.
Dr. Mishra[/caption]
Santosh K. Mishra M.Tech., PhD
Assistant Professor of Neuroscience
Department of Molecular Biomedical Sciences
NC State Veterinary Medicine
Raleigh, NC 2760
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by atopic dermatitis?
Response: Chronic allergic itch is a worldwide problem that leads to substantial health expenses,but what causes this universal urge to scratch remains elusive in chronic allergic itch. Atopic dermatitis is a common allergic skin disease that often associated with extremely itchy and inflamed skin.
In our study, we showed, for the first time, a molecular pathway that is involved in chronic allergic itch as we identified an endogenous mediator (periostin) and a new role for its sensory neuron receptor, the integrin αVβ3, which drives the excitability and transmission of itch signal to the spinal cord.
Allergies, Asthma, Author Interviews, Dermatology, Pediatrics / 10.03.2020
Poor Sleep Quality in Asthmatic Children With Atopic Dermatitis
MedicalResearch.com Interview with:
[caption id="attachment_53396" align="alignleft" width="121"] Dr. Aquino[/caption]
Marcella Aquino, M.D.
Hasbro Children's Hospital
Department of Pediatrics
Division of Allergy & Immunology
Associate Professor of Pediatrics
[caption id="attachment_53397" align="alignleft" width="107"]
Dr. Aquino[/caption]
Marcella Aquino, M.D.
Hasbro Children's Hospital
Department of Pediatrics
Division of Allergy & Immunology
Associate Professor of Pediatrics
[caption id="attachment_53397" align="alignleft" width="107"] Dr. Koinis-Mitchell[/caption]
Daphne Koinis-Mitchell PhD
Professor (Research) in the Departments of Psychiatry and
Human Behavior and Pediatrics
Warren Alpert Medical School of Brown University
Providence, Rhode Island 02903
MedicalResearch.com: What is the background for this study?
Response: Urban minority children with asthma are at increased risk for sleep loss and poorer sleep quality secondary to socio-contextual stressors (poverty, stressors of urban living) and the underlying challenges related to following possibly complex asthma treatment regimens. Atopic dermatitis (AD) is very frequently seen in children with asthma and increases the risk for poor quality sleep, for example difficulty falling asleep, awakenings during the night, difficulty awakening in the morning, and/or daytime sleepiness.
Dr. Koinis-Mitchell[/caption]
Daphne Koinis-Mitchell PhD
Professor (Research) in the Departments of Psychiatry and
Human Behavior and Pediatrics
Warren Alpert Medical School of Brown University
Providence, Rhode Island 02903
MedicalResearch.com: What is the background for this study?
Response: Urban minority children with asthma are at increased risk for sleep loss and poorer sleep quality secondary to socio-contextual stressors (poverty, stressors of urban living) and the underlying challenges related to following possibly complex asthma treatment regimens. Atopic dermatitis (AD) is very frequently seen in children with asthma and increases the risk for poor quality sleep, for example difficulty falling asleep, awakenings during the night, difficulty awakening in the morning, and/or daytime sleepiness.
 Dr. Aquino[/caption]
Marcella Aquino, M.D.
Hasbro Children's Hospital
Department of Pediatrics
Division of Allergy & Immunology
Associate Professor of Pediatrics
[caption id="attachment_53397" align="alignleft" width="107"]
Dr. Aquino[/caption]
Marcella Aquino, M.D.
Hasbro Children's Hospital
Department of Pediatrics
Division of Allergy & Immunology
Associate Professor of Pediatrics
[caption id="attachment_53397" align="alignleft" width="107"] Dr. Koinis-Mitchell[/caption]
Daphne Koinis-Mitchell PhD
Professor (Research) in the Departments of Psychiatry and
Human Behavior and Pediatrics
Warren Alpert Medical School of Brown University
Providence, Rhode Island 02903
MedicalResearch.com: What is the background for this study?
Response: Urban minority children with asthma are at increased risk for sleep loss and poorer sleep quality secondary to socio-contextual stressors (poverty, stressors of urban living) and the underlying challenges related to following possibly complex asthma treatment regimens. Atopic dermatitis (AD) is very frequently seen in children with asthma and increases the risk for poor quality sleep, for example difficulty falling asleep, awakenings during the night, difficulty awakening in the morning, and/or daytime sleepiness.
Dr. Koinis-Mitchell[/caption]
Daphne Koinis-Mitchell PhD
Professor (Research) in the Departments of Psychiatry and
Human Behavior and Pediatrics
Warren Alpert Medical School of Brown University
Providence, Rhode Island 02903
MedicalResearch.com: What is the background for this study?
Response: Urban minority children with asthma are at increased risk for sleep loss and poorer sleep quality secondary to socio-contextual stressors (poverty, stressors of urban living) and the underlying challenges related to following possibly complex asthma treatment regimens. Atopic dermatitis (AD) is very frequently seen in children with asthma and increases the risk for poor quality sleep, for example difficulty falling asleep, awakenings during the night, difficulty awakening in the morning, and/or daytime sleepiness.
Author Interviews, Dermatology, Immunotherapy, Science / 27.02.2020
Rebalancing Immune System May Help Bring Atopic Dermatitis – Eczema – Under Control
MedicalResearch.com Interview with:
[caption id="attachment_53319" align="alignleft" width="145"] Dr. Kim[/caption]
Brian S. Kim, MD, MTR, FAAD
Associate Professor of Medicine (Dermatology)
Co-Director, Center for the Study of Itch and Sensory Disorders
Division of Dermatology, Department of Medicine
Washington University School of Medicine
St. Louis, MO 63110
MedicalResearch.com: What is the background for this study?
Response: It has been known well for decades that a specific part of your immune system called the “type 2 immune response” is overactive in atopic disease. Indeed, that is what new drugs like dupilumab block so effectively and thus revolutionized the treatment of atopic disorders just in the last few years. In fact, our lab focuses predominantly on this part of the immune system.
However, increasingly it is becoming recognized that the immune system is not just about whether it is “on or off” but rather a balance like yin and yang. Along these lines, we noticed that a cell that could theoretically counterbalance atopic inflammation was significantly deficient in many patients with eczema. This cell is the natural killer (NK) cell.
Dr. Kim[/caption]
Brian S. Kim, MD, MTR, FAAD
Associate Professor of Medicine (Dermatology)
Co-Director, Center for the Study of Itch and Sensory Disorders
Division of Dermatology, Department of Medicine
Washington University School of Medicine
St. Louis, MO 63110
MedicalResearch.com: What is the background for this study?
Response: It has been known well for decades that a specific part of your immune system called the “type 2 immune response” is overactive in atopic disease. Indeed, that is what new drugs like dupilumab block so effectively and thus revolutionized the treatment of atopic disorders just in the last few years. In fact, our lab focuses predominantly on this part of the immune system.
However, increasingly it is becoming recognized that the immune system is not just about whether it is “on or off” but rather a balance like yin and yang. Along these lines, we noticed that a cell that could theoretically counterbalance atopic inflammation was significantly deficient in many patients with eczema. This cell is the natural killer (NK) cell.
 Dr. Kim[/caption]
Brian S. Kim, MD, MTR, FAAD
Associate Professor of Medicine (Dermatology)
Co-Director, Center for the Study of Itch and Sensory Disorders
Division of Dermatology, Department of Medicine
Washington University School of Medicine
St. Louis, MO 63110
MedicalResearch.com: What is the background for this study?
Response: It has been known well for decades that a specific part of your immune system called the “type 2 immune response” is overactive in atopic disease. Indeed, that is what new drugs like dupilumab block so effectively and thus revolutionized the treatment of atopic disorders just in the last few years. In fact, our lab focuses predominantly on this part of the immune system.
However, increasingly it is becoming recognized that the immune system is not just about whether it is “on or off” but rather a balance like yin and yang. Along these lines, we noticed that a cell that could theoretically counterbalance atopic inflammation was significantly deficient in many patients with eczema. This cell is the natural killer (NK) cell.
Dr. Kim[/caption]
Brian S. Kim, MD, MTR, FAAD
Associate Professor of Medicine (Dermatology)
Co-Director, Center for the Study of Itch and Sensory Disorders
Division of Dermatology, Department of Medicine
Washington University School of Medicine
St. Louis, MO 63110
MedicalResearch.com: What is the background for this study?
Response: It has been known well for decades that a specific part of your immune system called the “type 2 immune response” is overactive in atopic disease. Indeed, that is what new drugs like dupilumab block so effectively and thus revolutionized the treatment of atopic disorders just in the last few years. In fact, our lab focuses predominantly on this part of the immune system.
However, increasingly it is becoming recognized that the immune system is not just about whether it is “on or off” but rather a balance like yin and yang. Along these lines, we noticed that a cell that could theoretically counterbalance atopic inflammation was significantly deficient in many patients with eczema. This cell is the natural killer (NK) cell.
Allergies, Author Interviews, CMAJ, Environmental Risks, Pediatrics / 20.02.2020
Cleaning Products May Raise Risk of Wheezing and Asthma in Young Children
MedicalResearch.com Interview with:
Jaclyn Parks, B.Sc. Health Sciences
M.Sc. Health Sciences Candidate | Faculty of Health Sciences
Simon Fraser University
Burnaby, B.C
MedicalResearch.com: What is the background for this study?
Response: Childhood asthma is a major public health concern, and many researchers are interested in determining environmental and modifiable exposures in early life so that we can recommend preventative measures. The findings of our study add to the understanding of which exposures in early life may be important to the development of childhood asthma and allergies and allows us to identify specific areas of intervention for parents and other stakeholders involved in protecting children’s health.
Author Interviews, Depression, Dermatology, Pediatrics / 21.01.2020
Post-Partum Depression Linked to Atopic Dermatitis – Eczema – in Children
MedicalResearch.com Interview with:
[caption id="attachment_24142" align="alignleft" width="128"] Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Director of Clinical Research and Contact Dermatitis
Associate Professor of Dermatology
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: We previously found that children from single parent families, and unsafe or unsupportive neighborhoods are more likely to have atopic dermatitis. Parents in these settings may experience greater psychosocial distress and higher rates of depression in the post-partum period and beyond.
As such, we sought to understand the relationship of maternal depression with atopic dermatitis in their children.
Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Director of Clinical Research and Contact Dermatitis
Associate Professor of Dermatology
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: We previously found that children from single parent families, and unsafe or unsupportive neighborhoods are more likely to have atopic dermatitis. Parents in these settings may experience greater psychosocial distress and higher rates of depression in the post-partum period and beyond.
As such, we sought to understand the relationship of maternal depression with atopic dermatitis in their children.
 Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Director of Clinical Research and Contact Dermatitis
Associate Professor of Dermatology
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: We previously found that children from single parent families, and unsafe or unsupportive neighborhoods are more likely to have atopic dermatitis. Parents in these settings may experience greater psychosocial distress and higher rates of depression in the post-partum period and beyond.
As such, we sought to understand the relationship of maternal depression with atopic dermatitis in their children.
Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Director of Clinical Research and Contact Dermatitis
Associate Professor of Dermatology
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: We previously found that children from single parent families, and unsafe or unsupportive neighborhoods are more likely to have atopic dermatitis. Parents in these settings may experience greater psychosocial distress and higher rates of depression in the post-partum period and beyond.
As such, we sought to understand the relationship of maternal depression with atopic dermatitis in their children.
- 1
- 2