MedicalResearch.com Interview with:
[caption id="attachment_60038" align="alignleft" width="200"]

Dr. Schutz[/caption]
Michael R.
Schutz,
Ph.D.
Professor of Music Cognition/Percussion at McMaster University
Founding director of the
MAPLE Lab and
Core member of the McMaster Institute for Music and the Mind.
Prof. Schutz is also a professional musician and directs McMaster’s percussion ensemble.
MedicalResearch.com: What is the background for this study?
Response: Hospitals around the world are filled with devices generating a
constant stream of tones conveying information to medical staff.
overburdened healthcare professionals, and contributes to burnout in
medical staff. The Emergency Care Research Institute (ECRI) regularly
includes problems with auditory alarms in their list of "Top 10 Health
Technology Hazards" and they are so problematic an FDA survey
implicated them in hundreds of patient deaths.
While there is currently a lot of interest in how to improve alarm
management protocols, this study is different in that it looks at
improving the quality of the alarm sounds themselves. For historical
reasons many default to simplistic "beeps" which are generally
annoying. While annoying is useful for critical alarms requiring
immediate action, the vast majority of these messages are merely
intended to update medical staff of changes (i.e. blood pressure is
rising) or indicate other situations that do not require immediate
action. Unfortunately, many machines use the same simplistic and
annoying "beeps" regardless of whether the messages are urgent or
non-urgent. This constant flood of annoying beeps negatively affects
both patients (extending recovery time due to interrupted rest) and
staff (who can develop "alarm fatigue" from the constant cacophony).





 Dr. Caraballo-Cordovez[/caption]
César Caraballo-Cordovez, MD
Dr. Caraballo-Cordovez[/caption]
César Caraballo-Cordovez, MD




 Dr. Jacob[/caption]
Jesse T. Jacob, MD
School of Medicine
Director, Antibiotic Stewardship Program
Emory University, Atlanta, Georgia
MedicalResearch.com: What is the background for this study?
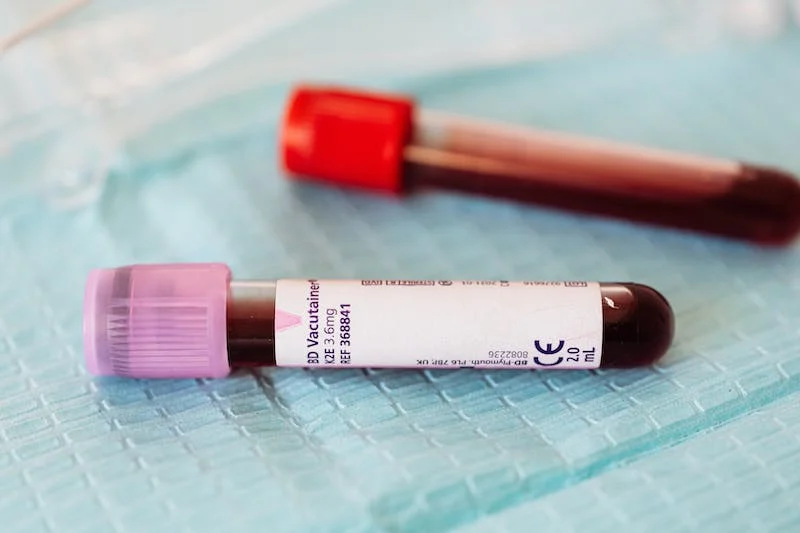
Response: Since coronavirus disease 2019 (COVID-19) was recognized in the United States in January 2020, the risk of infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) attributed to exposures in the health care workplace has been studied with conflicting results, and the role of job functions (such as nurse) or specific workplace activities, including care for individuals with known and unknown SARS-CoV-2 positivity, increase the risk of SARS-CoV-2 infection.
We assessed more than 24,000 healthcare providers between April and August 2020 across four large academic medical systems (Emory, Johns Hopkins, Rush University Medical Center, and University of Maryland) which collaborate in the CDC’s Prevention Epicenter Program and conduct innovative infection prevention research. Each site conducted voluntary COVID-19 antibody testing on its health care workers, as well as offered a questionnaire/survey on the employees’ occupational activities and possible exposures to individuals with COVID-19 infection both inside and outside the workplace. We also looked at three-digit residential zip-code prefixes to determine COVID-19 prevalence in communities.
Dr. Jacob[/caption]
Jesse T. Jacob, MD
School of Medicine
Director, Antibiotic Stewardship Program
Emory University, Atlanta, Georgia
MedicalResearch.com: What is the background for this study?
Response: Since coronavirus disease 2019 (COVID-19) was recognized in the United States in January 2020, the risk of infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) attributed to exposures in the health care workplace has been studied with conflicting results, and the role of job functions (such as nurse) or specific workplace activities, including care for individuals with known and unknown SARS-CoV-2 positivity, increase the risk of SARS-CoV-2 infection.
We assessed more than 24,000 healthcare providers between April and August 2020 across four large academic medical systems (Emory, Johns Hopkins, Rush University Medical Center, and University of Maryland) which collaborate in the CDC’s Prevention Epicenter Program and conduct innovative infection prevention research. Each site conducted voluntary COVID-19 antibody testing on its health care workers, as well as offered a questionnaire/survey on the employees’ occupational activities and possible exposures to individuals with COVID-19 infection both inside and outside the workplace. We also looked at three-digit residential zip-code prefixes to determine COVID-19 prevalence in communities. 
 Dr. Traverso[/caption]
Carlo Giovanni Traverso, MB, BChir, PhD
Associate Physician, Brigham and Women's Hospital
Assistant Professor,
[caption id="attachment_56823" align="alignleft" width="150"]
Dr. Traverso[/caption]
Carlo Giovanni Traverso, MB, BChir, PhD
Associate Physician, Brigham and Women's Hospital
Assistant Professor,
[caption id="attachment_56823" align="alignleft" width="150"] Dr. Chai[/caption]
Peter R. Chai, MD, MMS
Emergency Medicine Physician and Medical Toxicologist
Harvard Medical School
Brigham and Women's Hospital
Department of Medicine
Dr. Chai[/caption]
Peter R. Chai, MD, MMS
Emergency Medicine Physician and Medical Toxicologist
Harvard Medical School
Brigham and Women's Hospital
Department of Medicine
 MedicalResearch.com: What is the background for this study? What are some of the functions that Dr. Spot can facilitate?
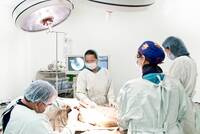
Response: During the COVID-19 pandemic, we wanted to consider innovative methods to provide additional social distance for physicians evaluating low acuity individuals who may have COVID-19 disease in the emergency department. While other health systems had instituted processes like evaluating patients from outside of emergency department rooms or calling patients to obtain a history, we considered the use of a mobile robotic system in collaboration with Boston Dynamics to provide telemedicine triage on an agile platform that could be navigated around a busy emergency department. Dr. Spot was built with a camera system to help an operator navigate it through an emergency department into a patient room where an on-board tablet would permit face-to-face triage and assessment of individuals.
MedicalResearch.com: What is the background for this study? What are some of the functions that Dr. Spot can facilitate?
Response: During the COVID-19 pandemic, we wanted to consider innovative methods to provide additional social distance for physicians evaluating low acuity individuals who may have COVID-19 disease in the emergency department. While other health systems had instituted processes like evaluating patients from outside of emergency department rooms or calling patients to obtain a history, we considered the use of a mobile robotic system in collaboration with Boston Dynamics to provide telemedicine triage on an agile platform that could be navigated around a busy emergency department. Dr. Spot was built with a camera system to help an operator navigate it through an emergency department into a patient room where an on-board tablet would permit face-to-face triage and assessment of individuals.


 Dr. Hooker[/caption]
Edmond A. Hooker, MD, DrPH
Professor, Department of Health Services Administration
MHSA Associate Director for Accreditation
Xavier University
Cincinnati, Ohio
MedicalResearch.com: What is the background for this study?
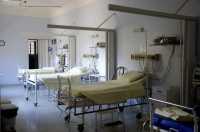
Response: Healthcare acquired infections are still a huge problem in the US. Most hospitals are not following the hospital bed manufacturers guidelines for cleaning these mattresses and bed decks (the metal bed frame). Many use only a single step, when the manufacturers recommend a 5-6 step process (pre-clean any obvious soil, clean, rinse off cleaner, disinfect, rinse off disinfectant, inspect mattress for damage). The problem is that, if done, this takes 45 minutes to 1 hours. Most hospitals turn over a hospital room in less than 30 minutes. The launderable bed cover allows the bed to be cleaned and turned over in minutes, not an hours.
Dr. Hooker[/caption]
Edmond A. Hooker, MD, DrPH
Professor, Department of Health Services Administration
MHSA Associate Director for Accreditation
Xavier University
Cincinnati, Ohio
MedicalResearch.com: What is the background for this study?
Response: Healthcare acquired infections are still a huge problem in the US. Most hospitals are not following the hospital bed manufacturers guidelines for cleaning these mattresses and bed decks (the metal bed frame). Many use only a single step, when the manufacturers recommend a 5-6 step process (pre-clean any obvious soil, clean, rinse off cleaner, disinfect, rinse off disinfectant, inspect mattress for damage). The problem is that, if done, this takes 45 minutes to 1 hours. Most hospitals turn over a hospital room in less than 30 minutes. The launderable bed cover allows the bed to be cleaned and turned over in minutes, not an hours. 





![MedicalResearch.com Interview with: Regis Goulart Rosa, MD, PhD Responsabilidade Social - PROADI Hospital Moinhos de Vento MedicalResearch.com: What is the background for this study? Response: The debate about visiting policies in adult ICUs is of broad and current interest in critical care, with strong advocacy in favour of flexible family visitation models in order to promote patient- and family-centred care. However, the proportion of adult ICUs with unrestricted visiting hours is very low. Data from the literature show that 80% of hospitals in the United Kingdom and USA adopt restrictive ICU visiting policies. Among ICUs with restrictive visiting hours, published studies show that the daily visiting time ranges from a median of 1 hour in Italy to a mean of 4.7 hours in France. In agreement with this scenario, most adult ICUs in Brazil follow a restrictive visitation model, in which family members are allowed to visit the critically ill patient from 30 minutes to 1 hour, once or twice a day. These restrictive visitation models have been justified by the theoretical risks associated with unrestricted visiting hours, mainly infectious complications, disorganization of care, and burnout. Controversially, these risks have not been consistently confirmed by the scarce literature on the subject, and flexible ICU visiting hours have been proposed as a means to prevent delirium among patients and improve family satisfaction. MedicalResearch.com: What are the main findings? Response: Disappointingly, studies evaluating the effectiveness and safety of flexible ICU visiting hours are scarce. To date, no large randomized trials have assessed the impact of a flexible visiting model on patients, family members, and ICU staff, and this evidence gap may constitute a barrier to the understanding of the best way to implement and improve ICU visiting policies. In the present pragmatic cluster-randomized crossover trial (The ICU Visits Study), we engaged 1,685 patients, 1,295 family members, and 826 ICU professionals from 36 adult ICUs in Brazil to compare a flexible visitation model (12 hours/day plus family education) vs. the standard restricted visitation model (median 90 minutes per day). We found that the flexible visitation did not significantly reduce the incidence of delirium among patients, but was associated with fewer symptoms of anxiety and depression and higher satisfaction with care among family members in comparison to the usual restricted visitation. Also, the flexible visitation did not increase the incidence of ICU-acquired infections and ICU staff burnout, which are major concerns when adopting this intervention. MedicalResearch.com: What should readers take away from your report? Response: Considering the evidence suggesting that most adult ICUs restrict the presence of family members, our results provide useful and relevant information that may influence the debate about current ICU visitation policies around the world. First, a flexible visitation policy that permits flexible family visitation in ICU (up to 12 hour per day) is feasible, given the high adherence of participant ICUs to implementation in The ICU Visits Study. Second, the flexible family supported by family education is safe regarding the occurrence of infections, disorganization of care or staff burnout. Third, family members - a commonly missing piece of the critical care puzzle - seem to benefit from the flexible visitation model through higher satisfaction with care and less symptoms of anxiety and depression. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: Future research might focus on the following topics: 1) methods of implementation of flexible visiting models in ICUs; 2) Family support interventions in the context of flexible ICU visiting hours (e.g.: psychological and social support, support for shared decision making, peer support, and comfort); and 3) How flexible ICU visiting hours affects patient, family member and staff outcome at long-term. Disclosures: The ICU Visits study was funded by the Brazilian Ministry of Health through the Brazilian Unified Health System Institutional Development Program (PROADI-SUS). Citation: Effect of Flexible Family Visitation on Delirium Among Patients in the Intensive Care Unit [wysija_form id="3"] [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/hospital-ICU-intensive-care.jpg)



 Dr. Rattray[/caption]
Nicholas A. Rattray, Ph.D.
Research Scientist/Investigator
VA HSR&D Center for Health Information and Communication
Implementation Core, Precision Monitoring to Transform Care (PRISM) QUERI
Richard L. Roudebush Veterans Affairs Medical Center
Indiana University Center for Health Services & Outcomes Research
Regenstrief Institute, Inc.
Indianapolis, Indiana
on behalf of study co-authors re:
Rattray NA, Flanagan ME, Militello LG, Barach P, Franks Z, Ebright P, Rehman SU,
Gordon HS, Frankel RM
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: End-of-shift handoffs pose a substantial patient safety risk. The transition of care from one doctor to another has been associated with delays in diagnosis and treatment, duplication of tests or treatment and patient discomfort, inappropriate care, medication errors and longer hospital stays with more laboratory testing. Handoff education varies widely in medical schools and residency training programs. Although there have been efforts to improve transfers of care, they have not shown meaningful improvement.
Led for the last decade by Richard Frankel, Ph.D., a senior health scientist at Regenstrief Institute and Indiana University and professor at Indiana University School of Medicine, our team has studied how health practitioners communicate during end-of-shift handoffs. In this current study, funded by VA Health Services and Research Development, we conducted interviews with 35 internal medicine and surgery residents at three VA medical centers about a recent handoff and analyzed the responses. Our team also video-recorded and analyzed more than 150 handoffs.
Published in the Journal of General Internal Medicine, this study explains how the person receiving the handoff can affect the interaction. Medical residents said they changed their delivery based on the doctor or resident who was taking over (i.e., training level, preference for fewer details, day or night shift). We found that handoff communication involves a complex combination of socio-technical information where residents balance relational factors against content and risk. It is not a mechanistic process of merely transferring clinical data but rather is based on learned habits of communication that are context-sensitive and variable, what we refer to as “recipient design”.
In another paper led by Laura Militello, we focus on how residents cognitively prepare for handoffs. In the paper published in The Joint Commission Journal of Quality and Patient Safety®, researchers detailed the tasks involved in cognitively preparing for handoffs. A third paper, published in BMC Medical Education, reports on the limited training that physicians receive during their residency. Residents said they were only partially prepared for enacting handoffs as interns, and clinical experience and enacting handoffs actually taught them the most.
Dr. Rattray[/caption]
Nicholas A. Rattray, Ph.D.
Research Scientist/Investigator
VA HSR&D Center for Health Information and Communication
Implementation Core, Precision Monitoring to Transform Care (PRISM) QUERI
Richard L. Roudebush Veterans Affairs Medical Center
Indiana University Center for Health Services & Outcomes Research
Regenstrief Institute, Inc.
Indianapolis, Indiana
on behalf of study co-authors re:
Rattray NA, Flanagan ME, Militello LG, Barach P, Franks Z, Ebright P, Rehman SU,
Gordon HS, Frankel RM
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: End-of-shift handoffs pose a substantial patient safety risk. The transition of care from one doctor to another has been associated with delays in diagnosis and treatment, duplication of tests or treatment and patient discomfort, inappropriate care, medication errors and longer hospital stays with more laboratory testing. Handoff education varies widely in medical schools and residency training programs. Although there have been efforts to improve transfers of care, they have not shown meaningful improvement.
Led for the last decade by Richard Frankel, Ph.D., a senior health scientist at Regenstrief Institute and Indiana University and professor at Indiana University School of Medicine, our team has studied how health practitioners communicate during end-of-shift handoffs. In this current study, funded by VA Health Services and Research Development, we conducted interviews with 35 internal medicine and surgery residents at three VA medical centers about a recent handoff and analyzed the responses. Our team also video-recorded and analyzed more than 150 handoffs.
Published in the Journal of General Internal Medicine, this study explains how the person receiving the handoff can affect the interaction. Medical residents said they changed their delivery based on the doctor or resident who was taking over (i.e., training level, preference for fewer details, day or night shift). We found that handoff communication involves a complex combination of socio-technical information where residents balance relational factors against content and risk. It is not a mechanistic process of merely transferring clinical data but rather is based on learned habits of communication that are context-sensitive and variable, what we refer to as “recipient design”.
In another paper led by Laura Militello, we focus on how residents cognitively prepare for handoffs. In the paper published in The Joint Commission Journal of Quality and Patient Safety®, researchers detailed the tasks involved in cognitively preparing for handoffs. A third paper, published in BMC Medical Education, reports on the limited training that physicians receive during their residency. Residents said they were only partially prepared for enacting handoffs as interns, and clinical experience and enacting handoffs actually taught them the most.



 Dawn Wiest, PhD
Director, Action Research & Evaluation
Camden Coalition of Healthcare Providers
MedicalResearch.com: What is the background for this study?
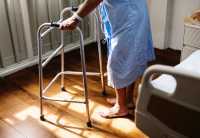
Response: Understanding the role of care transitions after hospitalization in reducing avoidable readmissions, the Camden Coalition launched the 7-Day Pledge in 2014 in partnership with primary care practices in Camden, NJ to address patient and provider barriers to timely post-discharge primary care follow-up. To evaluate whether our program was associated with lower hospital readmissions, we used all-payer hospital claims data from five regional health systems. We compared readmissions for patients who had a primary care follow-up within seven days with similar patients who had a later or no follow-up using propensity score matching.
Dawn Wiest, PhD
Director, Action Research & Evaluation
Camden Coalition of Healthcare Providers
MedicalResearch.com: What is the background for this study?
Response: Understanding the role of care transitions after hospitalization in reducing avoidable readmissions, the Camden Coalition launched the 7-Day Pledge in 2014 in partnership with primary care practices in Camden, NJ to address patient and provider barriers to timely post-discharge primary care follow-up. To evaluate whether our program was associated with lower hospital readmissions, we used all-payer hospital claims data from five regional health systems. We compared readmissions for patients who had a primary care follow-up within seven days with similar patients who had a later or no follow-up using propensity score matching.

