MedicalResearch.com Interview with:
[caption id="attachment_56251" align="alignleft" width="200"] Dr. Magnusson[/caption]
Karin Magnusson PT, PhD
Associate Researcher
Lund University and
Norwegian Institute of Public Health
MedicalResearch.com: What is the background for this study?
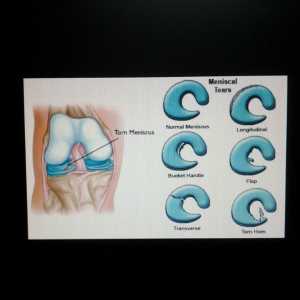
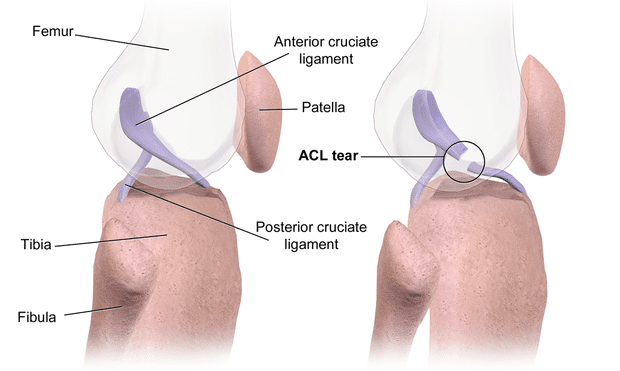
Response: Anterior cruciate ligament (ACL) injury is one of the most common knee injuries, for which very limited data has been presented on the genetic contribution. Based on our knowledge of the role of genetics in the development of ACL-rupture related traits, such as joint hypermobility and knee osteoarthritis, we hypothesized that heritability might play a role also in ACL injury.
Using the Swedish Twin Registry, which is the world's largest twin registry and in this study including more than 88.000 twins, we had unique data to for the first time reliably estimate the heritability for this common knee injury.
Dr. Magnusson[/caption]
Karin Magnusson PT, PhD
Associate Researcher
Lund University and
Norwegian Institute of Public Health
MedicalResearch.com: What is the background for this study?
Response: Anterior cruciate ligament (ACL) injury is one of the most common knee injuries, for which very limited data has been presented on the genetic contribution. Based on our knowledge of the role of genetics in the development of ACL-rupture related traits, such as joint hypermobility and knee osteoarthritis, we hypothesized that heritability might play a role also in ACL injury.
Using the Swedish Twin Registry, which is the world's largest twin registry and in this study including more than 88.000 twins, we had unique data to for the first time reliably estimate the heritability for this common knee injury.
 Dr. Magnusson[/caption]
Karin Magnusson PT, PhD
Associate Researcher
Lund University and
Norwegian Institute of Public Health
MedicalResearch.com: What is the background for this study?
Response: Anterior cruciate ligament (ACL) injury is one of the most common knee injuries, for which very limited data has been presented on the genetic contribution. Based on our knowledge of the role of genetics in the development of ACL-rupture related traits, such as joint hypermobility and knee osteoarthritis, we hypothesized that heritability might play a role also in ACL injury.
Using the Swedish Twin Registry, which is the world's largest twin registry and in this study including more than 88.000 twins, we had unique data to for the first time reliably estimate the heritability for this common knee injury.
Dr. Magnusson[/caption]
Karin Magnusson PT, PhD
Associate Researcher
Lund University and
Norwegian Institute of Public Health
MedicalResearch.com: What is the background for this study?
Response: Anterior cruciate ligament (ACL) injury is one of the most common knee injuries, for which very limited data has been presented on the genetic contribution. Based on our knowledge of the role of genetics in the development of ACL-rupture related traits, such as joint hypermobility and knee osteoarthritis, we hypothesized that heritability might play a role also in ACL injury.
Using the Swedish Twin Registry, which is the world's largest twin registry and in this study including more than 88.000 twins, we had unique data to for the first time reliably estimate the heritability for this common knee injury. 

 Dr. Cavanaugh[/caption]
Alyson Cavanaugh, PT, PhD
Joint Doctoral Program in Epidemiology
University of California, San Diego/ San Diego State University
MedicalResearch.com: What is the background for this study?
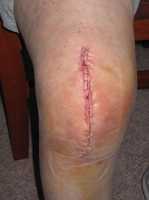
Response: More than 700,000 total knee replacements are performed annually in the United States, but there is a racial disparity in outcomes after the surgery. If the knee replacement procedure is considered a highly effective treatment, why don't black women present with the same outcomes as whites?
Physical function when going into surgery has a large impact on the potential functional outcomes after surgery. Our hypothesis was that black women were presenting to surgery with poorer physical function, which was contributing to poorer functional outcomes after surgery.
Dr. Cavanaugh[/caption]
Alyson Cavanaugh, PT, PhD
Joint Doctoral Program in Epidemiology
University of California, San Diego/ San Diego State University
MedicalResearch.com: What is the background for this study?
Response: More than 700,000 total knee replacements are performed annually in the United States, but there is a racial disparity in outcomes after the surgery. If the knee replacement procedure is considered a highly effective treatment, why don't black women present with the same outcomes as whites?
Physical function when going into surgery has a large impact on the potential functional outcomes after surgery. Our hypothesis was that black women were presenting to surgery with poorer physical function, which was contributing to poorer functional outcomes after surgery.


 Dr. Schneider[/caption]
Dr. Michael Schneider DC, PhD
Associate Professor
School of Health and Rehabilitation Sciences
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
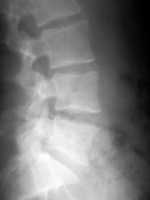
Response: Lumbar spinal stenosis (LSS) is one of the fastest growing problems in the country due to its aging population. One third of Medicare users have the condition, and it is the number one reason for spine surgery in this population. Existing research evaluates the benefits of nonsurgical treatment options compared to surgery, but there was no existing research that compared the available nonsurgical options to each other to determine the best course of treatment for each patient.
We studied three nonsurgical treatments for LSS: medical management with medications and/or epidural injections, individualized care with a physical therapist or chiropractor, and group exercise. We assessed each of these treatment methods with a questionnaire, a walking distance test, and a physical activity monitor.
Dr. Schneider[/caption]
Dr. Michael Schneider DC, PhD
Associate Professor
School of Health and Rehabilitation Sciences
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
Response: Lumbar spinal stenosis (LSS) is one of the fastest growing problems in the country due to its aging population. One third of Medicare users have the condition, and it is the number one reason for spine surgery in this population. Existing research evaluates the benefits of nonsurgical treatment options compared to surgery, but there was no existing research that compared the available nonsurgical options to each other to determine the best course of treatment for each patient.
We studied three nonsurgical treatments for LSS: medical management with medications and/or epidural injections, individualized care with a physical therapist or chiropractor, and group exercise. We assessed each of these treatment methods with a questionnaire, a walking distance test, and a physical activity monitor.