This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis or treatment. Contact a qualified medical professional before engaging in any physical activity, or making any changes to your diet, medication or lifestyle,
Navigating the broad universe of medicine resembles finding a path in a maze. Picking the right medical specialization is crucial for both professional growth and personal fulfillment. Medicine's field is varied, each having distinct challenges and benefits, thus making this decision crucial.
 Understanding oneself is vital before exploring medical fields. What are your unique interests? Which medical areas spark your enthusiasm? It's common to advise students to reflect on their likes and dislikes in various subjects. To save some time, you might hire an EssayPro to lessen your workload. This could enlighten you about your abilities and preferences.
Each medical field has specific requirements. A surgeon may have unpredictable hours and stressful situations, while a dermatologist may have more set hours. Understanding the work-life balance you desire can affect your choice.
Visualizing your future is essential. Where do you want to be in the next decade or two? Whether in a busy hospital emergency room, a peaceful research laboratory, or a community clinic, your long-term goals can guide your current choices.
Understanding oneself is vital before exploring medical fields. What are your unique interests? Which medical areas spark your enthusiasm? It's common to advise students to reflect on their likes and dislikes in various subjects. To save some time, you might hire an EssayPro to lessen your workload. This could enlighten you about your abilities and preferences.
Each medical field has specific requirements. A surgeon may have unpredictable hours and stressful situations, while a dermatologist may have more set hours. Understanding the work-life balance you desire can affect your choice.
Visualizing your future is essential. Where do you want to be in the next decade or two? Whether in a busy hospital emergency room, a peaceful research laboratory, or a community clinic, your long-term goals can guide your current choices.
Self-Assessment and Introspection
 Understanding oneself is vital before exploring medical fields. What are your unique interests? Which medical areas spark your enthusiasm? It's common to advise students to reflect on their likes and dislikes in various subjects. To save some time, you might hire an EssayPro to lessen your workload. This could enlighten you about your abilities and preferences.
Each medical field has specific requirements. A surgeon may have unpredictable hours and stressful situations, while a dermatologist may have more set hours. Understanding the work-life balance you desire can affect your choice.
Visualizing your future is essential. Where do you want to be in the next decade or two? Whether in a busy hospital emergency room, a peaceful research laboratory, or a community clinic, your long-term goals can guide your current choices.
Understanding oneself is vital before exploring medical fields. What are your unique interests? Which medical areas spark your enthusiasm? It's common to advise students to reflect on their likes and dislikes in various subjects. To save some time, you might hire an EssayPro to lessen your workload. This could enlighten you about your abilities and preferences.
Each medical field has specific requirements. A surgeon may have unpredictable hours and stressful situations, while a dermatologist may have more set hours. Understanding the work-life balance you desire can affect your choice.
Visualizing your future is essential. Where do you want to be in the next decade or two? Whether in a busy hospital emergency room, a peaceful research laboratory, or a community clinic, your long-term goals can guide your current choices.



 Mytien Nguyen[/caption]
Mytien Nguyen, MS
Department of Immunobiology,
Yale School of Medicine
New Haven, Connecticut
MedicalResearch.com: What is the background for this study?
Response: Physician-scientists are critical for innovative translational research.
Mytien Nguyen[/caption]
Mytien Nguyen, MS
Department of Immunobiology,
Yale School of Medicine
New Haven, Connecticut
MedicalResearch.com: What is the background for this study?
Response: Physician-scientists are critical for innovative translational research. 

 Larissa K. Samuelson, PhD
Professor
Developmental Dynamics Lab
School of Psychology; UK 14th for Research Quality
Psychology, Psychiatry, and Neuroscience
University of East Anglia, United Kingdom
MedicalResearch.com: What is the background for this study?
Response: Words direct the attention of infants, children and adults to mentioned objects in the environment. When someone says “Can you find the candy,” you look to the candy sitting on the counter. This fact is the basis of many tests of infant cognition in laboratories. To find out if a child knows the word “bike” we put a picture of a bike and a truck on a TV screen, say the word “bike” and see if they look at the correct object.
There is also evidence that words can direct attention even if you don’t know what they mean yet. For example, in studies of learning in the lab novel made up words like “modi” can direct children’s attention to specific features of objects. One particular example of this is the “shape bias”. If a two-year-old is shown a novel object and told a novel name, for example “This is my blicket,” and then asked, “Can you get your blicket” and shown one object that matches the named one in shape and another that is made from the same material, they will attend to the one that matches in shape. Researchers think the naming event “This is my…” cues children to look at things that are the same shape because they already know many names for things in sets that are similar in shape; cups are all cup-shaped, keys are all key-shaped, spoons are all spoon-shaped, etc.
Prior research suggests there may be differences in the way children who struggle with language decide what a new word means. For example, children with Developmental Language Disorder do not pay attention to the same things when learning new words as children with typical language development. These children do not look to an object that matches a named exemplar in shape when asked to “get your blicket”. But you can’t diagnose children with DLD until they are 3 or 4. We want to see if we can identify these children earlier, so they can get early support.
Larissa K. Samuelson, PhD
Professor
Developmental Dynamics Lab
School of Psychology; UK 14th for Research Quality
Psychology, Psychiatry, and Neuroscience
University of East Anglia, United Kingdom
MedicalResearch.com: What is the background for this study?
Response: Words direct the attention of infants, children and adults to mentioned objects in the environment. When someone says “Can you find the candy,” you look to the candy sitting on the counter. This fact is the basis of many tests of infant cognition in laboratories. To find out if a child knows the word “bike” we put a picture of a bike and a truck on a TV screen, say the word “bike” and see if they look at the correct object.
There is also evidence that words can direct attention even if you don’t know what they mean yet. For example, in studies of learning in the lab novel made up words like “modi” can direct children’s attention to specific features of objects. One particular example of this is the “shape bias”. If a two-year-old is shown a novel object and told a novel name, for example “This is my blicket,” and then asked, “Can you get your blicket” and shown one object that matches the named one in shape and another that is made from the same material, they will attend to the one that matches in shape. Researchers think the naming event “This is my…” cues children to look at things that are the same shape because they already know many names for things in sets that are similar in shape; cups are all cup-shaped, keys are all key-shaped, spoons are all spoon-shaped, etc.
Prior research suggests there may be differences in the way children who struggle with language decide what a new word means. For example, children with Developmental Language Disorder do not pay attention to the same things when learning new words as children with typical language development. These children do not look to an object that matches a named exemplar in shape when asked to “get your blicket”. But you can’t diagnose children with DLD until they are 3 or 4. We want to see if we can identify these children earlier, so they can get early support.


 Dr. Wong[/caption]
Mitchell Wong, MD PhD
Professor of Medicine
Executive Vice Chair for Research Training
Department of Medicine
Executive Co-Director, Specialty Training and Advanced Research (STAR) Program
Director, UCLA CTSI KL2 Program
UCLA Division of General Internal Medicine and Health Services Research Los Angeles, CA 90024
MedicalResearch.com: What is the background for this study?
Response: It is estimated that social factors like poverty, education, and housing have a large impact on health. Yet, there are few interventions that exist to directly address those issues. Schools are a promising solution since society already invests heavily in education and schools are an everyday part of most children’s lives.
Dr. Wong[/caption]
Mitchell Wong, MD PhD
Professor of Medicine
Executive Vice Chair for Research Training
Department of Medicine
Executive Co-Director, Specialty Training and Advanced Research (STAR) Program
Director, UCLA CTSI KL2 Program
UCLA Division of General Internal Medicine and Health Services Research Los Angeles, CA 90024
MedicalResearch.com: What is the background for this study?
Response: It is estimated that social factors like poverty, education, and housing have a large impact on health. Yet, there are few interventions that exist to directly address those issues. Schools are a promising solution since society already invests heavily in education and schools are an everyday part of most children’s lives.


 SooYoung VanDeMar[/caption]
SooYoung VanDeMark, MBS
Geisinger Commonwealth School of Medicine
Scranton, Pennsylvania
MedicalResearch.com: What is the background for this study?
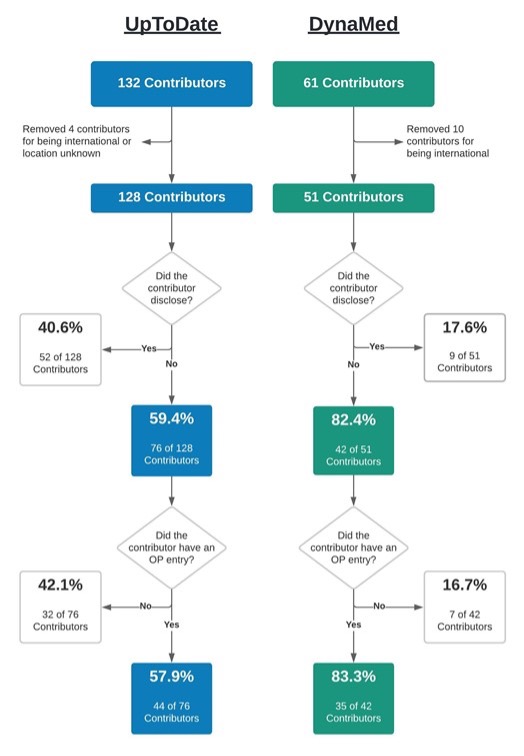
Response: Health care providers utilize subscription-based, point-of-care databases such as DynaMed and UpToDate to provide clinical care guidance and remain current on the latest evidence-based findings. Both of these websites maintain this content through a cadre of physician contributors who write and edit articles for these sites. These physician contributors are required to self-report any conflicts of interest (COI) as outlined by the respective policies on each website. However, prior COI research into similarly self-regulated areas, such as medical and pharmacology textbooks, and clinical practice guidelines, has found both appreciable potential COI and inconsistencies between self-reported and industry mandated disclosures (1-3).
This study (4) explored the accuracy of physician contributors to DynaMed and UpToDate by comparing their self-reported disclosure status with the financial remunerations they received from the healthcare industry (e.g., pharmaceutical companies) as reported to the U.S. Centers for Medicare and Medicaid Services’ Open Payments database. Physician contributors who reported “nothing to disclose” on their respective article topic but had an entry on Open Payments for having received money from industry, were classified as discordant and, thus, as having the potential for a COI. Additionally, total remuneration, gender, and payment category were investigated more in depth for each database.
SooYoung VanDeMar[/caption]
SooYoung VanDeMark, MBS
Geisinger Commonwealth School of Medicine
Scranton, Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: Health care providers utilize subscription-based, point-of-care databases such as DynaMed and UpToDate to provide clinical care guidance and remain current on the latest evidence-based findings. Both of these websites maintain this content through a cadre of physician contributors who write and edit articles for these sites. These physician contributors are required to self-report any conflicts of interest (COI) as outlined by the respective policies on each website. However, prior COI research into similarly self-regulated areas, such as medical and pharmacology textbooks, and clinical practice guidelines, has found both appreciable potential COI and inconsistencies between self-reported and industry mandated disclosures (1-3).
This study (4) explored the accuracy of physician contributors to DynaMed and UpToDate by comparing their self-reported disclosure status with the financial remunerations they received from the healthcare industry (e.g., pharmaceutical companies) as reported to the U.S. Centers for Medicare and Medicaid Services’ Open Payments database. Physician contributors who reported “nothing to disclose” on their respective article topic but had an entry on Open Payments for having received money from industry, were classified as discordant and, thus, as having the potential for a COI. Additionally, total remuneration, gender, and payment category were investigated more in depth for each database.




 Ali M. Fazlollahi[/caption]
Ali M. Fazlollahi, MSc, McGill Medicine Class of 2025
Neurosurgical Simulation and Artificial Intelligence Learning Centre
Department of Neurology and Neurosurgery, Montreal Neurological Institute and Hospital
Faculty of Medicine and Health Sciences
McGill University, Montreal, Canada
MedicalResearch.com: What is the background for this study?
Response: COVID-19 disrupted hands on surgical exposure of medical students and academic centres around the world had to quickly adapt to teaching technical skills remotely. At the same time, advances in artificial intelligence (AI) allowed researchers at the Neurosurgical Simulation and Artificial Intelligence Learning Centre to develop an intelligent tutoring system that evaluates performance and provides high-quality personalized feedback to students. Because this is the first AI system capable of providing surgical instructions in simulation, we sought to evaluate its effectiveness compared with learning from expert human instructors who provided coaching remotely.
Ali M. Fazlollahi[/caption]
Ali M. Fazlollahi, MSc, McGill Medicine Class of 2025
Neurosurgical Simulation and Artificial Intelligence Learning Centre
Department of Neurology and Neurosurgery, Montreal Neurological Institute and Hospital
Faculty of Medicine and Health Sciences
McGill University, Montreal, Canada
MedicalResearch.com: What is the background for this study?
Response: COVID-19 disrupted hands on surgical exposure of medical students and academic centres around the world had to quickly adapt to teaching technical skills remotely. At the same time, advances in artificial intelligence (AI) allowed researchers at the Neurosurgical Simulation and Artificial Intelligence Learning Centre to develop an intelligent tutoring system that evaluates performance and provides high-quality personalized feedback to students. Because this is the first AI system capable of providing surgical instructions in simulation, we sought to evaluate its effectiveness compared with learning from expert human instructors who provided coaching remotely.

 Arman A. Shahriar
Medical Student, University of Minnesota Medical School Research
Consultant, HealthPartners Institute
Minneapolis, Minnesota
Arman A. Shahriar
Medical Student, University of Minnesota Medical School Research
Consultant, HealthPartners Institute
Minneapolis, Minnesota
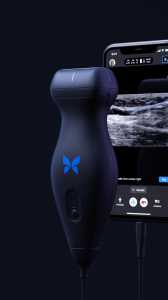 Response: Point-of-care ultrasound is one of the most significant advances in bedside patient care, and its use is expanding across nearly all fields of medicine. In order to best prepare medical students for residency and beyond, it is imperative to begin POCUS training as early as possible. At the Lewis Katz School of Medicine at Temple University, we introduced POCUS education over a decade ago and have expanded it since then.
By providing each student with a Butterfly iQ device, we can augment our curriculum significantly. In addition to our robust pre-clinical sessions, now we will expand into the clinical years highlighting the utility of POCUS with actual patients.
This gift was made possible by the incredible generosity of Dr. Ronald Salvitti, MD ’63.
Response: Point-of-care ultrasound is one of the most significant advances in bedside patient care, and its use is expanding across nearly all fields of medicine. In order to best prepare medical students for residency and beyond, it is imperative to begin POCUS training as early as possible. At the Lewis Katz School of Medicine at Temple University, we introduced POCUS education over a decade ago and have expanded it since then.
By providing each student with a Butterfly iQ device, we can augment our curriculum significantly. In addition to our robust pre-clinical sessions, now we will expand into the clinical years highlighting the utility of POCUS with actual patients.
This gift was made possible by the incredible generosity of Dr. Ronald Salvitti, MD ’63. 


 Dr. Forbes[/caption]
Lisa Forbes, Ph.D, LPC, NCC
Clinical Assistant Professor
Counseling Program
University of Colorado Denver
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The most common mode of learning in tertiary education is lecture-based learning despite the knowledge that more active, engaged, and flexible approaches to teaching may better support the learning process. This study aimed to understand graduate students’ experiences with a playful pedagogy as an alternative approach to learning.
Dr. Forbes[/caption]
Lisa Forbes, Ph.D, LPC, NCC
Clinical Assistant Professor
Counseling Program
University of Colorado Denver
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The most common mode of learning in tertiary education is lecture-based learning despite the knowledge that more active, engaged, and flexible approaches to teaching may better support the learning process. This study aimed to understand graduate students’ experiences with a playful pedagogy as an alternative approach to learning.

 As a specialized healthcare position where you will be responsible for the health and wellbeing of patients, nurses are required to hold a degree and a license before they can begin work. To qualify as a registered nurse, you will need to obtain a BSN degree, which typically takes around four years when studying full-time. However, if you already have a bachelor’s degree in another subject, there is an option that will allow you to become a nurse in half the time; accelerated nursing programs are designed for those who already have a bachelor’s degree and want a quick career change into nursing. The
As a specialized healthcare position where you will be responsible for the health and wellbeing of patients, nurses are required to hold a degree and a license before they can begin work. To qualify as a registered nurse, you will need to obtain a BSN degree, which typically takes around four years when studying full-time. However, if you already have a bachelor’s degree in another subject, there is an option that will allow you to become a nurse in half the time; accelerated nursing programs are designed for those who already have a bachelor’s degree and want a quick career change into nursing. The 
 Dr. Bullard[/caption]
Jared Bullard MD FRCPC
Associate Professor, Departments of Pediatrics & Child Health and Medical Microbiology & Infectious Diseases
Max Rady College of Medicine
Rady Faculty of Health Sciences
Cadham Provincial Laboratory
Children’s Hospital Research Institute of Manitoba
MedicalResearch.com: What is the background for this study?
Response: Children are well known to transmit epidemic/endemic respiratory viruses like influenza. Initial public health policy was based on that children were likely to transmit SARS-CoV-2 effectively within a community and subsequently in-person school and extracurricular activities were suspended.
Initial research did not show a clear association with children driving transmission. The purpose of our study was to take respiratory samples from both children and adults with COVID-19 (all had SARS-CoV-2 detected by RT-PCR) and compare those samples by their ability to grow in cell culture and amount of virus in samples.
We took 175 samples from children (97 younger than 10 years of age and 78 between 11-17 years) and compared them to 130 adult samples from the same communities in Manitoba experiencing outbreaks of COVID-19.
Dr. Bullard[/caption]
Jared Bullard MD FRCPC
Associate Professor, Departments of Pediatrics & Child Health and Medical Microbiology & Infectious Diseases
Max Rady College of Medicine
Rady Faculty of Health Sciences
Cadham Provincial Laboratory
Children’s Hospital Research Institute of Manitoba
MedicalResearch.com: What is the background for this study?
Response: Children are well known to transmit epidemic/endemic respiratory viruses like influenza. Initial public health policy was based on that children were likely to transmit SARS-CoV-2 effectively within a community and subsequently in-person school and extracurricular activities were suspended.
Initial research did not show a clear association with children driving transmission. The purpose of our study was to take respiratory samples from both children and adults with COVID-19 (all had SARS-CoV-2 detected by RT-PCR) and compare those samples by their ability to grow in cell culture and amount of virus in samples.
We took 175 samples from children (97 younger than 10 years of age and 78 between 11-17 years) and compared them to 130 adult samples from the same communities in Manitoba experiencing outbreaks of COVID-19. 

 Dr. Rettew[/caption]
David C. Rettew, MD
Child & Adolescent Psychiatrist
Associate Professor of Psychiatry and Pediatrics
University of Vermont Larner College of Medicine
MedicalResearch.com: What is the background for this study?
Response: Our group, the Wellness Environment Scientific Team at the University of Vermont, hadn’t planned to look at COVID at the outset of this study and instead were going to look at mental health and engagement in wellness activities in college students across a semester. The pandemic disrupted that plan when students were abruptly sent home but fortunately, they continued to do their daily app-based ratings of their mood, stress levels, and engagement in healthy activities. We then realized we had some interesting pre-COVID to COVID data that was worth exploring.
Dr. Rettew[/caption]
David C. Rettew, MD
Child & Adolescent Psychiatrist
Associate Professor of Psychiatry and Pediatrics
University of Vermont Larner College of Medicine
MedicalResearch.com: What is the background for this study?
Response: Our group, the Wellness Environment Scientific Team at the University of Vermont, hadn’t planned to look at COVID at the outset of this study and instead were going to look at mental health and engagement in wellness activities in college students across a semester. The pandemic disrupted that plan when students were abruptly sent home but fortunately, they continued to do their daily app-based ratings of their mood, stress levels, and engagement in healthy activities. We then realized we had some interesting pre-COVID to COVID data that was worth exploring. 


 Dr. Zimmerman[/caption]
Frederick Zimmerman, PhD
Professor, Department of Health Policy and Management
Fielding School of Public Health
UCLA
MedicalResearch.com: What is the background for this study?
Response: The science on school transmissions of COVID is becoming clearer all the time in its conclusion that there is little to no transmission in school environments as long as reasonable precautions are taken. Yet one recent study got a lot of attention for claiming that states that allowed their schools to remain open in the early days of the pandemic saw more cases. That study did not control for several important factors that might explain this association, so our study aimed to correct that work.
Dr. Zimmerman[/caption]
Frederick Zimmerman, PhD
Professor, Department of Health Policy and Management
Fielding School of Public Health
UCLA
MedicalResearch.com: What is the background for this study?
Response: The science on school transmissions of COVID is becoming clearer all the time in its conclusion that there is little to no transmission in school environments as long as reasonable precautions are taken. Yet one recent study got a lot of attention for claiming that states that allowed their schools to remain open in the early days of the pandemic saw more cases. That study did not control for several important factors that might explain this association, so our study aimed to correct that work.


 If you’re currently working as a nurse, you are probably well aware of just how rewarding and fulfilling a job role it can be. You get to help patients from all walks of life every single day and make a real difference to not only people’s health but their lives more generally. It’s also a career in which there is a lot of scope for progression. There are so many different spheres within the field of nursing that you can choose to specialize in, whether it’s a particular age group (like pediatrics or gerontology) or a particular health condition (like oncology or emergency care).
Some of these paths involve training on the job, whereas others require you to return to college to study and obtain a postgraduate qualification. Among these, one of the highest possible qualifications you can aim for is the DNP, or Doctor of Nursing Practice.
If you’re currently working as a nurse, you are probably well aware of just how rewarding and fulfilling a job role it can be. You get to help patients from all walks of life every single day and make a real difference to not only people’s health but their lives more generally. It’s also a career in which there is a lot of scope for progression. There are so many different spheres within the field of nursing that you can choose to specialize in, whether it’s a particular age group (like pediatrics or gerontology) or a particular health condition (like oncology or emergency care).
Some of these paths involve training on the job, whereas others require you to return to college to study and obtain a postgraduate qualification. Among these, one of the highest possible qualifications you can aim for is the DNP, or Doctor of Nursing Practice.