Author Interviews, Beth Israel Deaconess, COVID -19 Coronavirus, JAMA, Race/Ethnic Diversity / 01.05.2020
COVID-19: Which NYC Borough Has Highest Rate of Hospitalizations and Deaths?
MedicalResearch.com Interview with:
[caption id="attachment_54070" align="alignleft" width="120"] Dr. Wadhera[/caption]
Rishi Wadhera, MD, MPP, MPhil
Instructor in Medicine at Harvard Medical School
Cardiologist,Beth Israel Deaconess Medical Center
MedicalResearch.com: What is the background for this study?
Response: With more than a million confirmed cases of COVID-19 in the United States, there is growing concern that low-income communities and racial/ethnic minorities may be disproportionately shouldering the burden of the pandemic. New York City, which is comprised of 5 boroughs (Bronx, Brooklyn, Manhattan, Queens, and Staten Island) with unique demographic and socioeconomic characteristics, has emerged as the epicenter of the COVID-19 outbreak.
Dr. Wadhera[/caption]
Rishi Wadhera, MD, MPP, MPhil
Instructor in Medicine at Harvard Medical School
Cardiologist,Beth Israel Deaconess Medical Center
MedicalResearch.com: What is the background for this study?
Response: With more than a million confirmed cases of COVID-19 in the United States, there is growing concern that low-income communities and racial/ethnic minorities may be disproportionately shouldering the burden of the pandemic. New York City, which is comprised of 5 boroughs (Bronx, Brooklyn, Manhattan, Queens, and Staten Island) with unique demographic and socioeconomic characteristics, has emerged as the epicenter of the COVID-19 outbreak.
 Dr. Wadhera[/caption]
Rishi Wadhera, MD, MPP, MPhil
Instructor in Medicine at Harvard Medical School
Cardiologist,Beth Israel Deaconess Medical Center
MedicalResearch.com: What is the background for this study?
Response: With more than a million confirmed cases of COVID-19 in the United States, there is growing concern that low-income communities and racial/ethnic minorities may be disproportionately shouldering the burden of the pandemic. New York City, which is comprised of 5 boroughs (Bronx, Brooklyn, Manhattan, Queens, and Staten Island) with unique demographic and socioeconomic characteristics, has emerged as the epicenter of the COVID-19 outbreak.
Dr. Wadhera[/caption]
Rishi Wadhera, MD, MPP, MPhil
Instructor in Medicine at Harvard Medical School
Cardiologist,Beth Israel Deaconess Medical Center
MedicalResearch.com: What is the background for this study?
Response: With more than a million confirmed cases of COVID-19 in the United States, there is growing concern that low-income communities and racial/ethnic minorities may be disproportionately shouldering the burden of the pandemic. New York City, which is comprised of 5 boroughs (Bronx, Brooklyn, Manhattan, Queens, and Staten Island) with unique demographic and socioeconomic characteristics, has emerged as the epicenter of the COVID-19 outbreak.



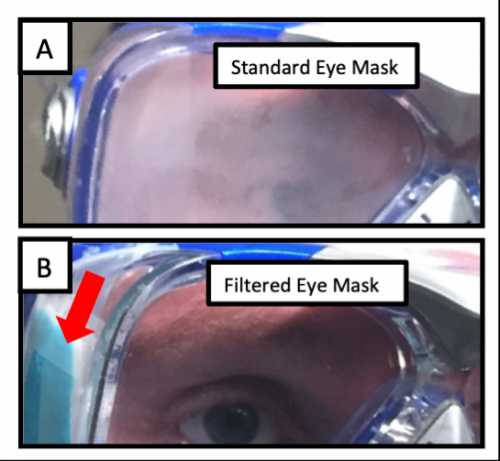

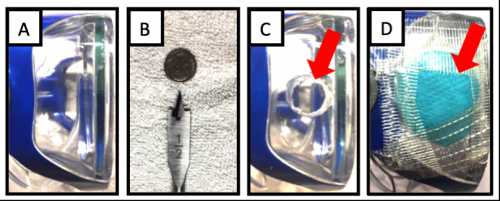 The building of the filtered eye mask prototype.[/caption]
The building of the filtered eye mask prototype.[/caption]




 Vasily Giannakeas[/caption]
Vasily Giannakeas, MPH
Epidemiologist/ Dedicated ICES Analyst
Women's College Hospital
Toronto, Ontario, Canada
MedicalResearch.com: What is the background for this study?
Response: As some health care systems approach collapse, a pressing need exists for tools modeling the capacity of acute and critical care systems during the COVID-19 pandemic.
We developed an online tool to estimate the maximum number of COVID-19 cases that could be managed per day within the catchment area served by a health care system, given acute and critical care resource availability.
The COVID-19 Acute and Intensive Care Resource Tool (CAIC-RT) is open access and available at
Vasily Giannakeas[/caption]
Vasily Giannakeas, MPH
Epidemiologist/ Dedicated ICES Analyst
Women's College Hospital
Toronto, Ontario, Canada
MedicalResearch.com: What is the background for this study?
Response: As some health care systems approach collapse, a pressing need exists for tools modeling the capacity of acute and critical care systems during the COVID-19 pandemic.
We developed an online tool to estimate the maximum number of COVID-19 cases that could be managed per day within the catchment area served by a health care system, given acute and critical care resource availability.
The COVID-19 Acute and Intensive Care Resource Tool (CAIC-RT) is open access and available at 










![MedicalResearch.com Interview with: Melissa Bondy, PhD Chair, Department of Epidemiology and Population Health Stanford University MedicalResearch.com: What is the background for this study? Response: Faculty researchers in Stanford’s Department of Epidemiology & Population Health and collaborators from Baylor College of Medicine and Stanford’s Department of Dermatology developed an online survey aimed at rapidly assessing public concerns about the COVID-19 crisis. This survey, which was posted on 3 social media platforms (Twitter, Facebook, and Nextdoor) on March 14, 2020, collected invaluable data about COVID-19, including symptoms, concerns, and individual actions taken by respondents. Twitter and Facebook posts were sharable to facilitate snowball sampling. The survey was comprised of 21 (multiple-choice, single-choice, numeric, and open-ended) questions, which were designed to collect data concerning respondent demographics and recent cold and flu-like illnesses (if any), as well as information about participants’ concerns and any lifestyle changes that occurred as a result of the COVID-19 crisis. All questions were optional, so response rates were variable. MedicalResearch.com: What are the main findings? Response: 9009 surveys were completed within a 48 hour period, between March 14 and 16. A majority were very or extremely concerns about COVID-19, though concern varied by age. Most respondents reported making lifestyle changes in response to COVID-19. The most common changes were more hand washing, avoiding social gatherings, and stockpiling food and supplies. About half of respondents were self-isolating most of the time before shelter-in-place orders, and leaving the house only to buy food and essentials. Respondents who were not self-isolating all of the time, before the shelter-in-place order, most commonly listed not being able to afford missing work as the reason. The top concerns reported by survey participants were getting sick because of COVID-19 and not being able to get medical care. The most common difficulties reported were obtaining hand sanitizer, food, and childcare. MedicalResearch.com: What should readers take away from your report? Response: This convenience sample survey distributed in mid-March 2020 across 3 social media platforms reflect respondents’ serious concerns about COVID-19. They were preparing for the crisis by washing hands, isolating at home, and practicing social distancing to the best of their abilities. Levels of concern about COVID-19 varied by age groups. Participants expressed the most common difficulties included getting sanitizer or food, arranging childcare, and lost wages or reduced working hours. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: Groups who are generally known to be underrepresented in social media, particularly men and older individuals, were underrepresented among survey participants. Few respondents reported concerns about their employment, but the study did not collect information about participants’ socioeconomic status (and was likely high). Our future work will expand geographic representation among survey respondents, with greater focus on longitudinal trends on the health, financial, and social concerns in the United States regarding the COVID-19 pandemic. No disclosures or conflicts of interest. Citation: Nelson LM, Simard JF, Oluyomi A, et al. US Public Concerns About the COVID-19 Pandemic From Results of a Survey Given via Social Media. JAMA Intern Med. Published online April 07, 2020. doi:10.1001/jamainternmed.2020.1369 https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2764368?guestAccessKey=cd7f419d-b177-44d2-86b2-c3e0254b3152&utm_source=For_The_Media&utm_medium=referral&utm_campaign=ftm_links&utm_content=tfl&utm_term=040720 [subscribe] Last Modified: [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/2020/04/Melissa-Bondy.jpg)

 Aurika Savickaite[/caption]
Aurika Savickaite RN
Adult Gerontology Acute Care Nurse Practitioner
Bulletproof Coach
University of Chicago Medicine
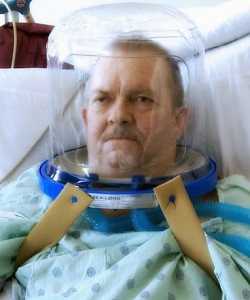
MedicalResearch.com: Would you briefly explain what is meant by helmet-based ventilation? How does it work?
Response: For patients in respiratory failure, noninvasive positive pressure ventilation (NIPPV) is usually delivered through a nasal mask or facemask. Many patients develop pain, discomfort – even claustrophobia -- from using NIPPV systems. The transparent helmet was developed to improve the tolerance of noninvasive ventilation. It allows the patient to see, read, speak and drink without interrupting noninvasive positive-pressure ventilation (NPPV).
The helmet has a sealed connection and a soft collar that adheres to the neck which helps prevent the air leaks that are very common with nasal- or face masks. High positive end-expiratory pressure (PEEP) is vital in treating patients in respiratory failure and thanks to helmets “none to minimum air leak” system, PEEP can be set high (up to 25). NIPPV via a nasal- or full-face mask typically begins to show air leaks when the required pressure exceeds 15-20cm H2O.
Aurika Savickaite[/caption]
Aurika Savickaite RN
Adult Gerontology Acute Care Nurse Practitioner
Bulletproof Coach
University of Chicago Medicine
MedicalResearch.com: Would you briefly explain what is meant by helmet-based ventilation? How does it work?
Response: For patients in respiratory failure, noninvasive positive pressure ventilation (NIPPV) is usually delivered through a nasal mask or facemask. Many patients develop pain, discomfort – even claustrophobia -- from using NIPPV systems. The transparent helmet was developed to improve the tolerance of noninvasive ventilation. It allows the patient to see, read, speak and drink without interrupting noninvasive positive-pressure ventilation (NPPV).
The helmet has a sealed connection and a soft collar that adheres to the neck which helps prevent the air leaks that are very common with nasal- or face masks. High positive end-expiratory pressure (PEEP) is vital in treating patients in respiratory failure and thanks to helmets “none to minimum air leak” system, PEEP can be set high (up to 25). NIPPV via a nasal- or full-face mask typically begins to show air leaks when the required pressure exceeds 15-20cm H2O.