Author Interviews, COVID -19 Coronavirus / 17.07.2020
COVID-19: What Are the Limitations of Social Distancing?
MedicalResearch.com Interview with:
[caption id="attachment_54880" align="alignleft" width="196"] Dr. Chakrabarty[/caption]
Rajan K. Chakrabarty, Ph.D.
Associate Professor,
Department of Energy, Environmental and Chemical Engineering
Washington University in Saint Louis
MedicalResearch.com: What is the background for this study?
Response: At the onset of COVID-19, we developed a state-of-the-art epidemic progression model involving the susceptible, exposed, infected, and recovered (SEIR) dynamics, the age-stratified disease transmissibility, and the possible large-scale undocumented asymptomatic transmission of COVID-19 taking place in the US states. By informing our model with using epidemiological COVID-19 data for the US between March 19 and 28 – a period corresponding to the early stage of the epidemic when the impacts of social distancing on disease progression were yet to manifest – we investigated: “What is the medical cost benefit of implementing social distancing as the “only” non-pharmaceutical intervention policy to combat COVID-19 in the US?”
As part of this study, we investigated three social distancing strategies – indefinite, finite-duration, and intermittent – on age-stratified US population and benchmark its effectiveness in reducing the burden on hospital beds.
Dr. Chakrabarty[/caption]
Rajan K. Chakrabarty, Ph.D.
Associate Professor,
Department of Energy, Environmental and Chemical Engineering
Washington University in Saint Louis
MedicalResearch.com: What is the background for this study?
Response: At the onset of COVID-19, we developed a state-of-the-art epidemic progression model involving the susceptible, exposed, infected, and recovered (SEIR) dynamics, the age-stratified disease transmissibility, and the possible large-scale undocumented asymptomatic transmission of COVID-19 taking place in the US states. By informing our model with using epidemiological COVID-19 data for the US between March 19 and 28 – a period corresponding to the early stage of the epidemic when the impacts of social distancing on disease progression were yet to manifest – we investigated: “What is the medical cost benefit of implementing social distancing as the “only” non-pharmaceutical intervention policy to combat COVID-19 in the US?”
As part of this study, we investigated three social distancing strategies – indefinite, finite-duration, and intermittent – on age-stratified US population and benchmark its effectiveness in reducing the burden on hospital beds.
 Dr. Chakrabarty[/caption]
Rajan K. Chakrabarty, Ph.D.
Associate Professor,
Department of Energy, Environmental and Chemical Engineering
Washington University in Saint Louis
MedicalResearch.com: What is the background for this study?
Response: At the onset of COVID-19, we developed a state-of-the-art epidemic progression model involving the susceptible, exposed, infected, and recovered (SEIR) dynamics, the age-stratified disease transmissibility, and the possible large-scale undocumented asymptomatic transmission of COVID-19 taking place in the US states. By informing our model with using epidemiological COVID-19 data for the US between March 19 and 28 – a period corresponding to the early stage of the epidemic when the impacts of social distancing on disease progression were yet to manifest – we investigated: “What is the medical cost benefit of implementing social distancing as the “only” non-pharmaceutical intervention policy to combat COVID-19 in the US?”
As part of this study, we investigated three social distancing strategies – indefinite, finite-duration, and intermittent – on age-stratified US population and benchmark its effectiveness in reducing the burden on hospital beds.
Dr. Chakrabarty[/caption]
Rajan K. Chakrabarty, Ph.D.
Associate Professor,
Department of Energy, Environmental and Chemical Engineering
Washington University in Saint Louis
MedicalResearch.com: What is the background for this study?
Response: At the onset of COVID-19, we developed a state-of-the-art epidemic progression model involving the susceptible, exposed, infected, and recovered (SEIR) dynamics, the age-stratified disease transmissibility, and the possible large-scale undocumented asymptomatic transmission of COVID-19 taking place in the US states. By informing our model with using epidemiological COVID-19 data for the US between March 19 and 28 – a period corresponding to the early stage of the epidemic when the impacts of social distancing on disease progression were yet to manifest – we investigated: “What is the medical cost benefit of implementing social distancing as the “only” non-pharmaceutical intervention policy to combat COVID-19 in the US?”
As part of this study, we investigated three social distancing strategies – indefinite, finite-duration, and intermittent – on age-stratified US population and benchmark its effectiveness in reducing the burden on hospital beds.


 Dr. Dixon[/caption]
Cinnamon A. Dixon, DO, MPH
Associate Professor of Pediatrics
University of Colorado School of Medicine
Children’s Hospital Colorado
Senior Investigator | Center for Global Health
Colorado School of Public Health
Aurora, CO
MedicalResearch.com: What is the background for this commentary?
Response: Dog bites are a long-standing public health problem. Each year there are approximately 4.5 million dog bites across the Unites States (US),1 and global estimates suggest tens of millions of these injuries worldwide.2 Children are the most vulnerable population with nearly 1 million annual dog bites in the US and more severe injury outcomes.1
National organizations espouse consistent strategies on how to prevent dog bites to children, however studies reveal that most children have never received dog bite prevention education.3,4 Furthermore, children lack critical knowledge of how to prevent dog bites in high-risk “resource guarding” situations (such as when a dog is eating or chewing on toys).4
During the COVID-19 pandemic, millions of US households are experiencing restrictions in activities. Children now spend more time in the home environment and presumably have increased exposure to their pet dogs. Parents and caregivers likely experience greater stress with more potential for competing interests and resultant decreased supervision of their children and dogs. Finally, pet dogs may be affected by the increased tension of their environment and be more likely to mirror the emotions of their human caregivers.
We hypothesized that these combined elements compound the risk of dog bites to children during the COVID-19 pandemic.
Dr. Dixon[/caption]
Cinnamon A. Dixon, DO, MPH
Associate Professor of Pediatrics
University of Colorado School of Medicine
Children’s Hospital Colorado
Senior Investigator | Center for Global Health
Colorado School of Public Health
Aurora, CO
MedicalResearch.com: What is the background for this commentary?
Response: Dog bites are a long-standing public health problem. Each year there are approximately 4.5 million dog bites across the Unites States (US),1 and global estimates suggest tens of millions of these injuries worldwide.2 Children are the most vulnerable population with nearly 1 million annual dog bites in the US and more severe injury outcomes.1
National organizations espouse consistent strategies on how to prevent dog bites to children, however studies reveal that most children have never received dog bite prevention education.3,4 Furthermore, children lack critical knowledge of how to prevent dog bites in high-risk “resource guarding” situations (such as when a dog is eating or chewing on toys).4
During the COVID-19 pandemic, millions of US households are experiencing restrictions in activities. Children now spend more time in the home environment and presumably have increased exposure to their pet dogs. Parents and caregivers likely experience greater stress with more potential for competing interests and resultant decreased supervision of their children and dogs. Finally, pet dogs may be affected by the increased tension of their environment and be more likely to mirror the emotions of their human caregivers.
We hypothesized that these combined elements compound the risk of dog bites to children during the COVID-19 pandemic.


 Samia Arshad[/caption]
Samia Arshad, MPH
Epidemiologist II
Infectious Disease
Henry Ford Hospital, Detroit, MI
I would like to start off by saying: We need to keep partisanship out of science. During this pandemic, we hope we can stick to science and help save lives with purposeful data driven facts.
MedicalResearch.com: What is the background for this study?
Response: Hydroxychloroquine, an antimalarial and immunomodulatory agent has demonstrated antiviral activity against SARS-CoV-2. We are in an acceleration phase of the COVID-19 pandemic, with 25% of the world’s cases occurring in the United States. Currently there is no known therapy or vaccine for treatment of SARS-CoV-2, highlighting the urgency around identifying effective therapies. The purpose of this study was to evaluate the role of hydroxychloroquine therapy alone and in combination with azithromycin in hospitalized patients positive for COVID-19.
Samia Arshad[/caption]
Samia Arshad, MPH
Epidemiologist II
Infectious Disease
Henry Ford Hospital, Detroit, MI
I would like to start off by saying: We need to keep partisanship out of science. During this pandemic, we hope we can stick to science and help save lives with purposeful data driven facts.
MedicalResearch.com: What is the background for this study?
Response: Hydroxychloroquine, an antimalarial and immunomodulatory agent has demonstrated antiviral activity against SARS-CoV-2. We are in an acceleration phase of the COVID-19 pandemic, with 25% of the world’s cases occurring in the United States. Currently there is no known therapy or vaccine for treatment of SARS-CoV-2, highlighting the urgency around identifying effective therapies. The purpose of this study was to evaluate the role of hydroxychloroquine therapy alone and in combination with azithromycin in hospitalized patients positive for COVID-19. ![MedicalResearch.com Interview with: Dr Herman Anne Service de Dermatologie Cliniques Universitaires Saint-Luc Avenue Hippocrate, 10 1200 Bruxelle MedicalResearch.com: What is the background for this study? Response: In the context of the COVID-19 pandemic, several cases of acro-located lesions (on foot or hands) suggestive of chilblains have been reported and were possibly related to COVID-19. We wanted to determine if chilblains, observed in many patients recently referred to our department, are indicative of COVID-19. MedicalResearch.com: Would you briefly explain what is meant by chilblains? Response: Chilblains are frequent cold induced inflammatory lesions. Chilblains are typically seen in winter and occur after repeated exposure to cold temperatures. Clinical presentation includes erythema and swelling on toes and/or digits followed by red-purple macules or patches. However, given the large number of patients affected, and the exceptionally high outdoor temperatures for the spring season over the past month and at the time of case-observation, cold-exposure seemed unlikely. These lesions were, therefore, suspected to be associated with COVID-19. However, to date, no study has proven a pathological link between these lesions and COVID-19. MedicalResearch.com: What are the main findings? Response: In our series of 31 patients who recently developed chilblains, negative nasopharyngeal swabs and the absence of anti-SARS-CoV-2 blood immunoglobulin (Ig)M and IgG antibodies in all patients included in your study suggested that these patients had not been infected with COVID-19. These lesions appeared not to be directly related to COVID-19. MedicalResearch.com: What should readers take away from your report? Response: One hypothesis points to an indirect consequence of the COVID-19 pandemic due to imposed community containment and lockdown measures. Indeed, all patients in this study had either been working from home or were home-schooled since the beginning of containment measures in Belgium (March 11, 2020) or were temporarily unemployed. As a result of containment measures, the majority (64.5%) of patients reported a decrease in their physical activity and significantly more time spent in sedentary positions in front of screens. Most of the patients declared that they remained barefoot or in socks most of the day. All these lifestyle changes can be considered as risk factors for developing chilblains. Therefore, it seems plausible that containment, through its collateral effects, may induce chilblains. Interestingly also, the mean BMI of the patients included was relatively low, suggesting that thin people may be more at risk of developing chilblains. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: During the current pandemic, several reports have suggested a possible link between cutaneous manifestations including aural lesions such as chilblains, and COVID-19, however, only few patients were tested for SARS-CoV-2 by RT-PCR and no serologic tests were performed. Therefore, reliable testings (RT-PCR and serologic testing) are essential to confirm a potential association with COVID-19. Citation: Herman A, Peeters C, Verroken A, et al. Evaluation of Chilblains as a Manifestation of the COVID-19 Pandemic. JAMA Dermatol. Published online June 25, 2020. doi:10.1001/jamadermatol.2020.2368 https://jamanetwork.com/journals/jamadermatology/fullarticle/2767774 [subscribe] Last Modified: [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/2020/06/chilblain-example-dermnet-nz.jpg)


 Dr. Blume[/caption]
Dr. Christine Blume PhD
Centre for Chronobiology
Psychiatric Hospital of the University of Basel
Transfaculty Research Platform Molecular and Cognitive Neurosciences
Basel
MedicalResearch.com: What is the background for this study?
Response: In modern societies, human rest-activity rhythms and sleep are between the often-conflicting poles of external social time (e.g., work hours and leisure activities) and an individual’s internal biological time. This can lead to so-called “social jetlag”, which has repeatedly been associated with detrimental health effects. With the restrictions to control the pandemic, social timing relaxed as people many started working from home and public life came to a standstill. In an online survey with 435 respondents, we investigated the effects of the phase with the strictest COVID-19 restrictions on the relationship between social and biological rhythms as well as sleep during a six-week period (mid-March until end of April 2020) in three European societies (Austria, Germany, Switzerland).
Dr. Blume[/caption]
Dr. Christine Blume PhD
Centre for Chronobiology
Psychiatric Hospital of the University of Basel
Transfaculty Research Platform Molecular and Cognitive Neurosciences
Basel
MedicalResearch.com: What is the background for this study?
Response: In modern societies, human rest-activity rhythms and sleep are between the often-conflicting poles of external social time (e.g., work hours and leisure activities) and an individual’s internal biological time. This can lead to so-called “social jetlag”, which has repeatedly been associated with detrimental health effects. With the restrictions to control the pandemic, social timing relaxed as people many started working from home and public life came to a standstill. In an online survey with 435 respondents, we investigated the effects of the phase with the strictest COVID-19 restrictions on the relationship between social and biological rhythms as well as sleep during a six-week period (mid-March until end of April 2020) in three European societies (Austria, Germany, Switzerland).
 Dr. Hooker[/caption]
Edmond A. Hooker, MD, DrPH
Professor, Department of Health Services Administration
MHSA Associate Director for Accreditation
Xavier University
Cincinnati, Ohio
MedicalResearch.com: What is the background for this study?
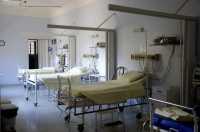
Response: Healthcare acquired infections are still a huge problem in the US. Most hospitals are not following the hospital bed manufacturers guidelines for cleaning these mattresses and bed decks (the metal bed frame). Many use only a single step, when the manufacturers recommend a 5-6 step process (pre-clean any obvious soil, clean, rinse off cleaner, disinfect, rinse off disinfectant, inspect mattress for damage). The problem is that, if done, this takes 45 minutes to 1 hours. Most hospitals turn over a hospital room in less than 30 minutes. The launderable bed cover allows the bed to be cleaned and turned over in minutes, not an hours.
Dr. Hooker[/caption]
Edmond A. Hooker, MD, DrPH
Professor, Department of Health Services Administration
MHSA Associate Director for Accreditation
Xavier University
Cincinnati, Ohio
MedicalResearch.com: What is the background for this study?
Response: Healthcare acquired infections are still a huge problem in the US. Most hospitals are not following the hospital bed manufacturers guidelines for cleaning these mattresses and bed decks (the metal bed frame). Many use only a single step, when the manufacturers recommend a 5-6 step process (pre-clean any obvious soil, clean, rinse off cleaner, disinfect, rinse off disinfectant, inspect mattress for damage). The problem is that, if done, this takes 45 minutes to 1 hours. Most hospitals turn over a hospital room in less than 30 minutes. The launderable bed cover allows the bed to be cleaned and turned over in minutes, not an hours. 


 Dr. Schünemann[/caption]
Holger Schünemann, MD, PhD, FRCPC
Professor of Clinical Epidemiology and of Medicine
Co-Director, WHO Collaborating Centre for Infectious Diseases,
Research Methods and Recommendations
Director, Cochrane Canada and McMaster GRADE Centre
Department of Health Research Methods, Evidence, and Impact
Canada
MedicalResearch.com: What is the background for this study?
Response: Many countries and regions have issued conflicting advice about physical distancing to reduce transmission of COVID-19, based on limited information. In addition, the questions of whether masks and eye coverings might reduce transmission of COVID-19 in the general population, and what the optimum use of masks in healthcare settings is, have been debated during the pandemic.
Dr. Schünemann[/caption]
Holger Schünemann, MD, PhD, FRCPC
Professor of Clinical Epidemiology and of Medicine
Co-Director, WHO Collaborating Centre for Infectious Diseases,
Research Methods and Recommendations
Director, Cochrane Canada and McMaster GRADE Centre
Department of Health Research Methods, Evidence, and Impact
Canada
MedicalResearch.com: What is the background for this study?
Response: Many countries and regions have issued conflicting advice about physical distancing to reduce transmission of COVID-19, based on limited information. In addition, the questions of whether masks and eye coverings might reduce transmission of COVID-19 in the general population, and what the optimum use of masks in healthcare settings is, have been debated during the pandemic.










 Dr. Alladina[/caption]
Jehan Alladina MD
Massachusetts General Hospital
Pulmonary and Critical Care Medicine
Boston, Massachusetts
MedicalResearch.com: What is the background for this study?
Response: During the pandemic, clinicians around the world have shared anecdotal experiences to help inform care of patients with COVID-19. However, these anecdotes and observations, without careful analysis, can bias clinicians; many clinicians have even recommended experimental therapies based on this information alone.
To that end, the goal of our study was to rigorously examine the respiratory failure experienced by critically ill patients with COVID-19 and understand their response to the standards of care for respiratory failure.
Dr. Alladina[/caption]
Jehan Alladina MD
Massachusetts General Hospital
Pulmonary and Critical Care Medicine
Boston, Massachusetts
MedicalResearch.com: What is the background for this study?
Response: During the pandemic, clinicians around the world have shared anecdotal experiences to help inform care of patients with COVID-19. However, these anecdotes and observations, without careful analysis, can bias clinicians; many clinicians have even recommended experimental therapies based on this information alone.
To that end, the goal of our study was to rigorously examine the respiratory failure experienced by critically ill patients with COVID-19 and understand their response to the standards of care for respiratory failure.

 Prof. Dagna[/caption]
Prof. Lorenzo Dagna MD FACP
Ospedale San Raffaele and
Vita-Salute San Raffaele University
Milan, Italy
MedicalResearch.com: What is the background for this study?
Response: Upon encountering pathogens, our immune system produces pro-inflammatory mediators, called cytokines. Cytokines activate cells from the immune system. In most people, production of cytokines is an appropriate and protective response to infection. However, some individuals develop excessive and detrimental inflammatory responses, which are even more harmful than the pathogen itself to the host organism.
We hypothesized that some patients with COVID-19 might develop excessive and detrimental inflammation, and that treatment with anti-inflammatory agents might be beneficial in this population.
Anakinra is an inhibitor of the pro-inflammatory molecule interleukin 1 (IL-1). It was originally marketed for the treatment of rheumatoid arthritis, but is now mostly used to treat a variety of pediatric inflammatory diseases.
Prof. Dagna[/caption]
Prof. Lorenzo Dagna MD FACP
Ospedale San Raffaele and
Vita-Salute San Raffaele University
Milan, Italy
MedicalResearch.com: What is the background for this study?
Response: Upon encountering pathogens, our immune system produces pro-inflammatory mediators, called cytokines. Cytokines activate cells from the immune system. In most people, production of cytokines is an appropriate and protective response to infection. However, some individuals develop excessive and detrimental inflammatory responses, which are even more harmful than the pathogen itself to the host organism.
We hypothesized that some patients with COVID-19 might develop excessive and detrimental inflammation, and that treatment with anti-inflammatory agents might be beneficial in this population.
Anakinra is an inhibitor of the pro-inflammatory molecule interleukin 1 (IL-1). It was originally marketed for the treatment of rheumatoid arthritis, but is now mostly used to treat a variety of pediatric inflammatory diseases.



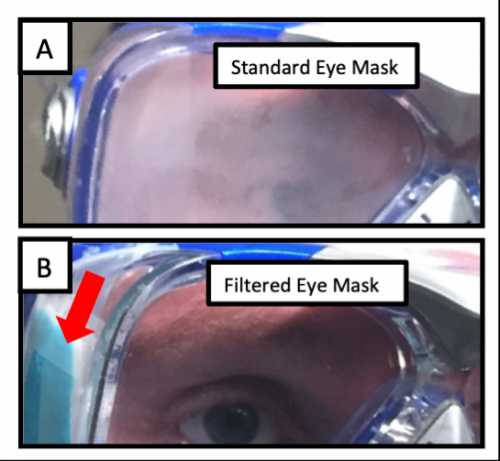

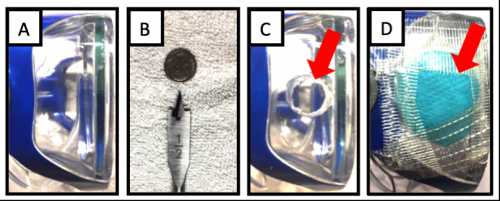 The building of the filtered eye mask prototype.[/caption]
The building of the filtered eye mask prototype.[/caption]