MedicalResearch.com Interview with:
[caption id="attachment_40814" align="alignleft" width="200"]

Trends in calorie availability in Canada and synthetic controls, 1978-2006. Data from the United Nations Food and Agricultural Office (2016). 'Synthetic controls' are constructed from a weighted combination of OECD countries, where weights correspond to the similarity of each country with Canada before CUSFTA.
Credit:
American Journal of Preventive Medicine[/caption]
Pepita Barlow, MSc, Department of Sociology
University of Oxford, Manor Road Building, Manor Road,
Oxford, United Kingdom
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The escalating global prevalence of overweight and obesity, or “globesity,” is often described as a pandemic. Globalization via free trade agreements (FTAs) with the US has been implicated in this pandemic because of its role in spreading high-calorie diets rich in salt, sugar, and fat through the reduction of trade barriers like tariffs in the food and beverage sector.
We used a “natural experiment” design (that mimics a randomized controlled trial as closely as possible) and data from the United Nations Food and Agricultural Office to evaluate the impact of the 1989 Canada-US Free Trade Agreement on caloric availability in Canada (CUSFTA).
We found that CUSFTA was associated with an increase in caloric availability and likely intake of approximately 170 kilocalories per person per day in Canada. Additional models showed that this rise in caloric intake can contribute to weight gain of between 1.8-9.3 kg for men and 2.0-12.2 kg for women aged 40, depending on their physical activity levels and the extent to which availability affects caloric intake.
 Dr. Kooraki[/caption]
Soheil Kooraki MSR MS, MD
on behalf of Dr. Ali Gholamrezanezhad MD and co-authors
Department of Radiological Sciences,
David Geffen School of Medicine, University of California at Los Angeles
Los Angeles, California
MedicalResearch.com: What is the background for this study? What are the main findings?
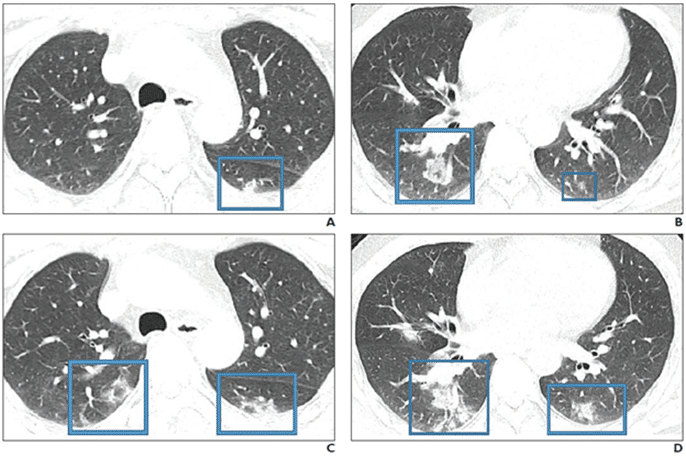
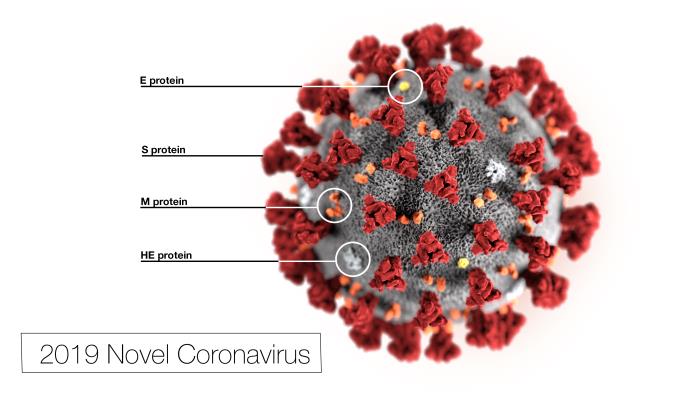
Response: COVID19 is a novel strain of the coronavirus family causing pneumonia. Two similar strains were discovered in 2003 and 2012 to cause the so-called SARS and MERS outbreaks, respectively. Radiologists need to be prepared for the escalating incidence of COVID-19. We reviewed the literature to extract the epidemiologic and imaging features of SARS and MERS in comparison with known imaging features of COVID-19 pneumonia to have a better understanding of the imaging features of the COVID19 pneumonia in acute and post-recovery stages.
Dr. Kooraki[/caption]
Soheil Kooraki MSR MS, MD
on behalf of Dr. Ali Gholamrezanezhad MD and co-authors
Department of Radiological Sciences,
David Geffen School of Medicine, University of California at Los Angeles
Los Angeles, California
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: COVID19 is a novel strain of the coronavirus family causing pneumonia. Two similar strains were discovered in 2003 and 2012 to cause the so-called SARS and MERS outbreaks, respectively. Radiologists need to be prepared for the escalating incidence of COVID-19. We reviewed the literature to extract the epidemiologic and imaging features of SARS and MERS in comparison with known imaging features of COVID-19 pneumonia to have a better understanding of the imaging features of the COVID19 pneumonia in acute and post-recovery stages.














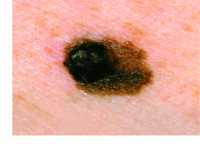
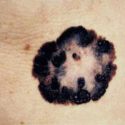 Example of one type of melanoma[/caption]
Dr. Catherine M. Olsen
Associate Professor
Cancer Control Group
QIMR Berghofer Medical Research Institute
MedicalResearch.com: What is the background for this study?
Response: Melanoma incidence and mortality rates are increasing globally. Public health campaigns aiming to reduce sun exposure and use of sunbed have been implemented in many parts of the world, but there is significant variability in terms of the history and reach of these campaigns across countries. We examined melanoma incidence rates in eight different countries with different patterns of sun exposure and varying approaches to melanoma control.
Example of one type of melanoma[/caption]
Dr. Catherine M. Olsen
Associate Professor
Cancer Control Group
QIMR Berghofer Medical Research Institute
MedicalResearch.com: What is the background for this study?
Response: Melanoma incidence and mortality rates are increasing globally. Public health campaigns aiming to reduce sun exposure and use of sunbed have been implemented in many parts of the world, but there is significant variability in terms of the history and reach of these campaigns across countries. We examined melanoma incidence rates in eight different countries with different patterns of sun exposure and varying approaches to melanoma control.



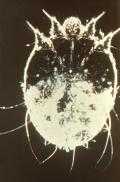
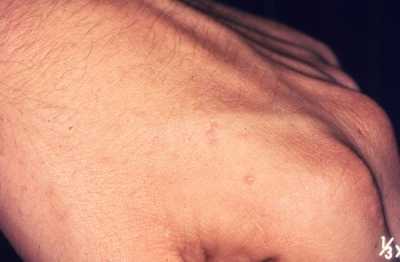 The lateral aspect of the left hand depicted here, reveals the presence of papules due to an infestation of the human itch mite, Sarcoptes scabiei var. hominis, in a case of what is commonly referred to as scabies.CDC image[/caption]
MedicalResearch.com: What is the background for this study?
MM: Scabies is extremely common. Globally in the region of 100-200 million people are believed to be affected by scabies annually.
Recently the WHO has recognised Scabies as a ‘Neglected Tropical Disease’ in response to this burden of disease. There has been increasing interest in using Mass Drug Administration (treating whole communities) as a strategy to control scabies in communities. In order to make this practical countries need an easy mechanism for establishing if scabies is a significant problem in their communities. In general when treating an individual, clinicians would conduct a full body examination to diagnose scabies – however this may not be practical or necessary when making decisions about whether to treat whole communities.
DE: Despite the fact that Scabies is a very common condition that causes a great deal of health problems, it has been largely neglected by health, research and funding agencies – but pleasingly, the WHO has now started to take action on scabies control, starting with the recognition of scabies as a "Neglected Tropical Disease"
The lateral aspect of the left hand depicted here, reveals the presence of papules due to an infestation of the human itch mite, Sarcoptes scabiei var. hominis, in a case of what is commonly referred to as scabies.CDC image[/caption]
MedicalResearch.com: What is the background for this study?
MM: Scabies is extremely common. Globally in the region of 100-200 million people are believed to be affected by scabies annually.
Recently the WHO has recognised Scabies as a ‘Neglected Tropical Disease’ in response to this burden of disease. There has been increasing interest in using Mass Drug Administration (treating whole communities) as a strategy to control scabies in communities. In order to make this practical countries need an easy mechanism for establishing if scabies is a significant problem in their communities. In general when treating an individual, clinicians would conduct a full body examination to diagnose scabies – however this may not be practical or necessary when making decisions about whether to treat whole communities.
DE: Despite the fact that Scabies is a very common condition that causes a great deal of health problems, it has been largely neglected by health, research and funding agencies – but pleasingly, the WHO has now started to take action on scabies control, starting with the recognition of scabies as a "Neglected Tropical Disease"













