Author Interviews, Gender Differences, Menopause, Urology / 15.03.2021
Urinary Incontinence Affects Nearly Half of US Women
MedicalResearch.com Interview with:
[caption id="attachment_56949" align="alignleft" width="150"] Dr. Lin Yang[/caption]
Lin Yang, PhD
Research Scientist/Epidemiologist
Department of Cancer Epidemiology and Prevention Research
Cancer Care Alberta | Alberta Health Services | Canada
Adjunct Assistant Professor
Departments of Oncology and Community Health Sciences
University of Calgary | Canada
MedicalResearch.com: What is the background for this study?
Response: Urinary incontinence disproportionately affects women. Urinary incontinence results in significant physical, social, and psychological adverse consequences that impair women’s quality of life and contribute to considerable healthcare costs. At the moment, the contemporary prevalence and recent trends in urinary incontinence in US women are unknown.
More importantly, there is a growing awareness that urinary incontinence is not part of normal aging, but very little information is available to inform prevention strategies. Therefore, we were also interested in exploring correlates of urinary incontinence in a population-based sample of US women.
Dr. Lin Yang[/caption]
Lin Yang, PhD
Research Scientist/Epidemiologist
Department of Cancer Epidemiology and Prevention Research
Cancer Care Alberta | Alberta Health Services | Canada
Adjunct Assistant Professor
Departments of Oncology and Community Health Sciences
University of Calgary | Canada
MedicalResearch.com: What is the background for this study?
Response: Urinary incontinence disproportionately affects women. Urinary incontinence results in significant physical, social, and psychological adverse consequences that impair women’s quality of life and contribute to considerable healthcare costs. At the moment, the contemporary prevalence and recent trends in urinary incontinence in US women are unknown.
More importantly, there is a growing awareness that urinary incontinence is not part of normal aging, but very little information is available to inform prevention strategies. Therefore, we were also interested in exploring correlates of urinary incontinence in a population-based sample of US women.
 Dr. Lin Yang[/caption]
Lin Yang, PhD
Research Scientist/Epidemiologist
Department of Cancer Epidemiology and Prevention Research
Cancer Care Alberta | Alberta Health Services | Canada
Adjunct Assistant Professor
Departments of Oncology and Community Health Sciences
University of Calgary | Canada
MedicalResearch.com: What is the background for this study?
Response: Urinary incontinence disproportionately affects women. Urinary incontinence results in significant physical, social, and psychological adverse consequences that impair women’s quality of life and contribute to considerable healthcare costs. At the moment, the contemporary prevalence and recent trends in urinary incontinence in US women are unknown.
More importantly, there is a growing awareness that urinary incontinence is not part of normal aging, but very little information is available to inform prevention strategies. Therefore, we were also interested in exploring correlates of urinary incontinence in a population-based sample of US women.
Dr. Lin Yang[/caption]
Lin Yang, PhD
Research Scientist/Epidemiologist
Department of Cancer Epidemiology and Prevention Research
Cancer Care Alberta | Alberta Health Services | Canada
Adjunct Assistant Professor
Departments of Oncology and Community Health Sciences
University of Calgary | Canada
MedicalResearch.com: What is the background for this study?
Response: Urinary incontinence disproportionately affects women. Urinary incontinence results in significant physical, social, and psychological adverse consequences that impair women’s quality of life and contribute to considerable healthcare costs. At the moment, the contemporary prevalence and recent trends in urinary incontinence in US women are unknown.
More importantly, there is a growing awareness that urinary incontinence is not part of normal aging, but very little information is available to inform prevention strategies. Therefore, we were also interested in exploring correlates of urinary incontinence in a population-based sample of US women.
















 Dr. Kenneth Iczkowski,[/caption]
Kenneth A. Iczkowski, M.D.
Department of Pathology
Medical College of Wisconsin
Milwaukee, WI 53226
MedicalResearch.com: What is the background for this study?
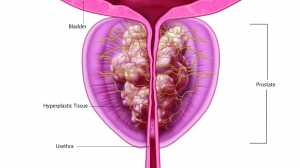
Dr. Iczkowski: The International Society of Urological Pathology (ISUP) in 2014 proposed use of a new 5-tier grade grouping system to supplement traditional Gleason grading to facilitate prognosis stratification and treatment1. The 5 categories subsume: Gleason 3+3=6, Gleason 3+4=7, Gleason 4+3=7, Gleason 8, and Gleason 9-10.
We desired to determine whether men with a highest Gleason score of 3+5=8 or 5+3=8 in their set of prostate biopsy specimens, would have differing outcomes from those with Gleason 4+4=8. Because Gleason 5 cancer has been demonstrated to have a higher biologic potential than Gleason 4, it was expected that Gleason score 8 pattern with any Gleason 5 pattern would have a worse outcome.
Dr. Kenneth Iczkowski,[/caption]
Kenneth A. Iczkowski, M.D.
Department of Pathology
Medical College of Wisconsin
Milwaukee, WI 53226
MedicalResearch.com: What is the background for this study?
Dr. Iczkowski: The International Society of Urological Pathology (ISUP) in 2014 proposed use of a new 5-tier grade grouping system to supplement traditional Gleason grading to facilitate prognosis stratification and treatment1. The 5 categories subsume: Gleason 3+3=6, Gleason 3+4=7, Gleason 4+3=7, Gleason 8, and Gleason 9-10.
We desired to determine whether men with a highest Gleason score of 3+5=8 or 5+3=8 in their set of prostate biopsy specimens, would have differing outcomes from those with Gleason 4+4=8. Because Gleason 5 cancer has been demonstrated to have a higher biologic potential than Gleason 4, it was expected that Gleason score 8 pattern with any Gleason 5 pattern would have a worse outcome.
 Dr. Alejandro Sousa[/caption]
Alejandro Sousa, MD, PhD
Department of Urology, Comarcal Hospital
Monforte, Spain
MedicalResearch.com: What is the background for this study?
Dr. Sousa: Bladder Cancer management has remained stable over the past 25 years, with very little in the way of new therapies or approaches being developed. Traditional treatment using intravesical Mitomycin C for Non Muscle Invasive Bladder Cancer (NMIBC) patients is limited due it's low absorption levels. Device assisted therapies that deliver Chemo-hyperthermia offer a new hope, with the potential for improved outcomes and better disease management due the the increased drug activity and better efficacy. We wanted to investigate the optimal treatment regime for this new therapy and whether it provides a safe and effective alternative to current standard treatment.
Dr. Alejandro Sousa[/caption]
Alejandro Sousa, MD, PhD
Department of Urology, Comarcal Hospital
Monforte, Spain
MedicalResearch.com: What is the background for this study?
Dr. Sousa: Bladder Cancer management has remained stable over the past 25 years, with very little in the way of new therapies or approaches being developed. Traditional treatment using intravesical Mitomycin C for Non Muscle Invasive Bladder Cancer (NMIBC) patients is limited due it's low absorption levels. Device assisted therapies that deliver Chemo-hyperthermia offer a new hope, with the potential for improved outcomes and better disease management due the the increased drug activity and better efficacy. We wanted to investigate the optimal treatment regime for this new therapy and whether it provides a safe and effective alternative to current standard treatment. Dr. Jed Kaminetsky[/caption]
Dr. Jed Kaminetsky MD
Clinical Assistant Professor
Department of Urology
NYU Langone Medical Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Kaminetsky: Nocturia is a voiding disorder not well treated by available drugs for overactive bladder and benign prostatic hypertrophy. Desmopressin stimulates the kidneys to concentrate the urine which results in a greatly reduced volume of urine formation for a period of time. Serenity Pharmaceuticals has spent many years developing a low dose nasal spray version of desmopressin called Noctiva specifically for nocturia. The study reported now is a large, placebo controlled phase 3 trial to confirm the statistical efficacy and clinical benefit of this treatment for nocturia.
Dr. Jed Kaminetsky[/caption]
Dr. Jed Kaminetsky MD
Clinical Assistant Professor
Department of Urology
NYU Langone Medical Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Kaminetsky: Nocturia is a voiding disorder not well treated by available drugs for overactive bladder and benign prostatic hypertrophy. Desmopressin stimulates the kidneys to concentrate the urine which results in a greatly reduced volume of urine formation for a period of time. Serenity Pharmaceuticals has spent many years developing a low dose nasal spray version of desmopressin called Noctiva specifically for nocturia. The study reported now is a large, placebo controlled phase 3 trial to confirm the statistical efficacy and clinical benefit of this treatment for nocturia.
 Dr. Hiten Patel[/caption]
Hiten D. Patel, MD, MPH
Resident, Urological Surgery
James Buchanan Brady Urological Institute
The Johns Hopkins Medical Institutions
Baltimore, Maryland 21287
MedicalResearch.com: What is the background for this study?
Dr. Patel: The study reports results of a systematic review contracted by the Agency for Healthcare Research and Quality based on input from stakeholders. Part of the motivation was due to the American Urological Association's desire to use the results as a basis to update relevant clinical guidelines.
There are four major management options for clinically localized small renal masses diagnosed on imaging including active surveillance, thermal ablation, partial nephrectomy, and radical nephrectomy. The body of research evaluating these management options is broad, but many of the studies performing comparative analyses have limitations. Therefore, the systematic review aimed to evaluate a number of outcomes (e.g. overall survival, cancer specific survival, local recurrence, metastasis, renal function, complications, and perioperative outcomes) based on available comparative studies in the literature.
Dr. Hiten Patel[/caption]
Hiten D. Patel, MD, MPH
Resident, Urological Surgery
James Buchanan Brady Urological Institute
The Johns Hopkins Medical Institutions
Baltimore, Maryland 21287
MedicalResearch.com: What is the background for this study?
Dr. Patel: The study reports results of a systematic review contracted by the Agency for Healthcare Research and Quality based on input from stakeholders. Part of the motivation was due to the American Urological Association's desire to use the results as a basis to update relevant clinical guidelines.
There are four major management options for clinically localized small renal masses diagnosed on imaging including active surveillance, thermal ablation, partial nephrectomy, and radical nephrectomy. The body of research evaluating these management options is broad, but many of the studies performing comparative analyses have limitations. Therefore, the systematic review aimed to evaluate a number of outcomes (e.g. overall survival, cancer specific survival, local recurrence, metastasis, renal function, complications, and perioperative outcomes) based on available comparative studies in the literature.
 Dr. Errol Singh[/caption]
Errol Singh, M.D.
Urologist and CEO of PercuVision
MedicalResearch.com: What is the background for this study?
Dr. Singh: We set out to better understand the American public’s fears around Foley catheters and hopefully bring attention to the fact that hospitalizations due to infections from urinary catheters are on the rise. Interestingly enough, 20 percent of hospital patients undergo a urinary catheterization, which is the second most common procedure following intravenous therapy. The procedure, however, often leads to complications including infections mostly caused by trauma.
MedicalResearch.com: What are the main findings?
Dr. Singh: The main findings of the 2016 Urinary Catheter Fear Survey revealed that three out of five men (58 percent) are fearful of urinary catheterizations, while one out of every four men is very fearful of the procedure. Younger men also seem to be more fearful than their older counterparts. More than two-thirds (68 percent) of men ages 18-34 surveyed are fearful of urinary catheterizations, compared to 43 percent of males 65 and over.
Clearly, females are less fearful, with 46 percent of women saying they are not fearful of urinary catheterizations, compared to 37 percent of men. It’s also important to note that half of all women surveyed say they fear the procedure, and 25 percent reporting they are very fearful. You can find more of the 2016 Urinary Catheter Fear Survey results on our website at
Dr. Errol Singh[/caption]
Errol Singh, M.D.
Urologist and CEO of PercuVision
MedicalResearch.com: What is the background for this study?
Dr. Singh: We set out to better understand the American public’s fears around Foley catheters and hopefully bring attention to the fact that hospitalizations due to infections from urinary catheters are on the rise. Interestingly enough, 20 percent of hospital patients undergo a urinary catheterization, which is the second most common procedure following intravenous therapy. The procedure, however, often leads to complications including infections mostly caused by trauma.
MedicalResearch.com: What are the main findings?
Dr. Singh: The main findings of the 2016 Urinary Catheter Fear Survey revealed that three out of five men (58 percent) are fearful of urinary catheterizations, while one out of every four men is very fearful of the procedure. Younger men also seem to be more fearful than their older counterparts. More than two-thirds (68 percent) of men ages 18-34 surveyed are fearful of urinary catheterizations, compared to 43 percent of males 65 and over.
Clearly, females are less fearful, with 46 percent of women saying they are not fearful of urinary catheterizations, compared to 37 percent of men. It’s also important to note that half of all women surveyed say they fear the procedure, and 25 percent reporting they are very fearful. You can find more of the 2016 Urinary Catheter Fear Survey results on our website at

 Dr. R. Jeffrey Karnes[/caption]
MedicalResearch.com Interview with:
R. Jeffrey Karnes MD
Department of Urology, Mayo Clinic,
Rochester, MN 55905
MedicalResearch: What is the background for this study? What are the main findings?
Dr. Karnes: Cancer recurrence following radical prostatectomy is a concern for men undergoing definitive surgical treatment for prostate cancer. Approximately 20-35% of patients develop a rising prostate specific antigen following radical prostatectomy for clinically localized prostate cancer. PSA monitoring is an important tool for cancer surveillance; however, a standard PSA cutpoint to indicate biochemical recurrence has yet to be established. Over 60 different definitions have been described in literature. This variation creates confusion for the patients and clinicians. By studying a large group of patients who underwent radical prostatectomy at Mayo Clinic, we found that a PSA cutpoint of 0.4 ng/mL is the optimal definition for biochemical recurrence.
Dr. R. Jeffrey Karnes[/caption]
MedicalResearch.com Interview with:
R. Jeffrey Karnes MD
Department of Urology, Mayo Clinic,
Rochester, MN 55905
MedicalResearch: What is the background for this study? What are the main findings?
Dr. Karnes: Cancer recurrence following radical prostatectomy is a concern for men undergoing definitive surgical treatment for prostate cancer. Approximately 20-35% of patients develop a rising prostate specific antigen following radical prostatectomy for clinically localized prostate cancer. PSA monitoring is an important tool for cancer surveillance; however, a standard PSA cutpoint to indicate biochemical recurrence has yet to be established. Over 60 different definitions have been described in literature. This variation creates confusion for the patients and clinicians. By studying a large group of patients who underwent radical prostatectomy at Mayo Clinic, we found that a PSA cutpoint of 0.4 ng/mL is the optimal definition for biochemical recurrence.

