Author Interviews, COVID -19 Coronavirus, Race/Ethnic Diversity, Vaccine Studies / 10.02.2023
Factors Influencing COVID-19 Vaccine Hesitancy in Eastern Pennsylvania
MedicalResearch.com Interview with:
[caption id="attachment_60007" align="alignleft" width="125"] Kenya Colvin[/caption]
Kenya Colvin, MBS
Department of Medical Education
Scranton, PA
MedicalResearch.com: What is the background for this study?
Response: Vaccine hesitancy is a major driver of COVID-19 vaccination disparities between minority and non-Hispanic White communities. Our goal was to understand what factors influenced vaccine hesitancy among individuals in Eastern Pennsylvania to identify more effective ways to promote vaccine uptake within minority communities.
Kenya Colvin[/caption]
Kenya Colvin, MBS
Department of Medical Education
Scranton, PA
MedicalResearch.com: What is the background for this study?
Response: Vaccine hesitancy is a major driver of COVID-19 vaccination disparities between minority and non-Hispanic White communities. Our goal was to understand what factors influenced vaccine hesitancy among individuals in Eastern Pennsylvania to identify more effective ways to promote vaccine uptake within minority communities.
 Kenya Colvin[/caption]
Kenya Colvin, MBS
Department of Medical Education
Scranton, PA
MedicalResearch.com: What is the background for this study?
Response: Vaccine hesitancy is a major driver of COVID-19 vaccination disparities between minority and non-Hispanic White communities. Our goal was to understand what factors influenced vaccine hesitancy among individuals in Eastern Pennsylvania to identify more effective ways to promote vaccine uptake within minority communities.
Kenya Colvin[/caption]
Kenya Colvin, MBS
Department of Medical Education
Scranton, PA
MedicalResearch.com: What is the background for this study?
Response: Vaccine hesitancy is a major driver of COVID-19 vaccination disparities between minority and non-Hispanic White communities. Our goal was to understand what factors influenced vaccine hesitancy among individuals in Eastern Pennsylvania to identify more effective ways to promote vaccine uptake within minority communities.




 Dr. Blumenthal[/caption]
Kimberly G. Blumenthal, MD, MSc
Massachusetts General Hospital
The Mongan Institute
Boston, MA 02114
[caption id="attachment_57828" align="alignleft" width="100"]
Dr. Blumenthal[/caption]
Kimberly G. Blumenthal, MD, MSc
Massachusetts General Hospital
The Mongan Institute
Boston, MA 02114
[caption id="attachment_57828" align="alignleft" width="100"] Dr. Krantz[/caption]
Matthew S. Krantz, MD
Division of Allergy, Pulmonary and Critical Care Medicine
Department of Medicine,
Vanderbilt University Medical Center,
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: During the initial COVID-19 vaccine campaign with healthcare workers in December 2020, there was an unexpected higher than anticipated rate of immediate allergic reactions after Pfizer and Moderna mRNA vaccines. This prompted both patient and provider concerns, particularly in those with underlying allergic histories, on the associated risks for immediate allergic reactions with the mRNA vaccines.
Because of the significantly improved effectiveness of two doses of an mRNA vaccine compared to one dose, it was important to determine if those who experienced immediate allergic reaction symptoms after their first dose could go on to tolerate a second dose safely.
Dr. Krantz[/caption]
Matthew S. Krantz, MD
Division of Allergy, Pulmonary and Critical Care Medicine
Department of Medicine,
Vanderbilt University Medical Center,
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: During the initial COVID-19 vaccine campaign with healthcare workers in December 2020, there was an unexpected higher than anticipated rate of immediate allergic reactions after Pfizer and Moderna mRNA vaccines. This prompted both patient and provider concerns, particularly in those with underlying allergic histories, on the associated risks for immediate allergic reactions with the mRNA vaccines.
Because of the significantly improved effectiveness of two doses of an mRNA vaccine compared to one dose, it was important to determine if those who experienced immediate allergic reaction symptoms after their first dose could go on to tolerate a second dose safely. 
 Laura M. Bogart, PhD
Senior Behavioral Scientist
RAND Corporation
Santa Monica, CA 90407-2138
MedicalResearch.com: What is the background for this study?
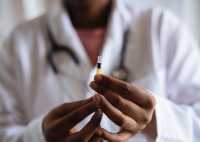
Response: Recent media polls continue to show that Black Americans are less likely to intend to get the COVID-19 vaccine than White Americans, and initial state data show a similar racial/ethnic disparity in vaccination rates. Initial uptake of the vaccine has been significantly affected by inequities in vaccine access and supply. In addition to these challenges, other factors contribute to hesitancy around vaccination, including self-perceived risk of infection, trust in the vaccine itself, trust in healthcare systems, healthcare providers, and policymakers who support the vaccine, and trust in the pharmaceutical industry and clinical research. In this study, we conducted a survey of a nationally representative sample of 207 Black Americans in late 2020, after initial COVID-19 vaccine effectiveness and safety data were released to the public. We also did in-depth interviews with a subsample of those surveyed who said that they would not get vaccinated. In addition, we engaged with a stakeholder advisory committee comprised of individuals who represent different subgroups and organizations in Black communities in the U.S., in order to discuss the results and make recommendations for policies to increase COVID-19 vaccination among Black Americans.
Laura M. Bogart, PhD
Senior Behavioral Scientist
RAND Corporation
Santa Monica, CA 90407-2138
MedicalResearch.com: What is the background for this study?
Response: Recent media polls continue to show that Black Americans are less likely to intend to get the COVID-19 vaccine than White Americans, and initial state data show a similar racial/ethnic disparity in vaccination rates. Initial uptake of the vaccine has been significantly affected by inequities in vaccine access and supply. In addition to these challenges, other factors contribute to hesitancy around vaccination, including self-perceived risk of infection, trust in the vaccine itself, trust in healthcare systems, healthcare providers, and policymakers who support the vaccine, and trust in the pharmaceutical industry and clinical research. In this study, we conducted a survey of a nationally representative sample of 207 Black Americans in late 2020, after initial COVID-19 vaccine effectiveness and safety data were released to the public. We also did in-depth interviews with a subsample of those surveyed who said that they would not get vaccinated. In addition, we engaged with a stakeholder advisory committee comprised of individuals who represent different subgroups and organizations in Black communities in the U.S., in order to discuss the results and make recommendations for policies to increase COVID-19 vaccination among Black Americans.
 Dr. Kriner[/caption]
Douglas L. Kriner, PhD
The Clinton Rossiter Professor in American Institutions
Department of Government
Cornell University
MedicalResearch.com: What is the background for this study?
Response: When a safe and effective vaccine for COVID-19 reaches the market, the world will not change overnight. Rather, government and public health individuals will have to develop a comprehensive plan to distribute the vaccine and to convince potentially wary Americans to take it.
Our study examined the influence of both specific vaccine characteristics and the politics surrounding it on public willingness to vaccinate. Both matter in important ways. For example, efficacy is unsurprisingly a major driver of public opinion; Americans are more willing to take a vaccine that is more efficacious.
Dr. Kriner[/caption]
Douglas L. Kriner, PhD
The Clinton Rossiter Professor in American Institutions
Department of Government
Cornell University
MedicalResearch.com: What is the background for this study?
Response: When a safe and effective vaccine for COVID-19 reaches the market, the world will not change overnight. Rather, government and public health individuals will have to develop a comprehensive plan to distribute the vaccine and to convince potentially wary Americans to take it.
Our study examined the influence of both specific vaccine characteristics and the politics surrounding it on public willingness to vaccinate. Both matter in important ways. For example, efficacy is unsurprisingly a major driver of public opinion; Americans are more willing to take a vaccine that is more efficacious.





 Kathryn M. Edwards, M.D.
Sarah H. Sell and Cornelius Vanderbilt Chair in Pediatrics
Professor of Pediatrics
Vanderbilt University School of Medicine
Dr. Edwards discusses the statement from the Infectious Diseases Society of America (IDSA) regarding the Centers for Disease Control and Prevention’s new data on child vaccine rates across the United States.
MedicalResearch.com: What is the background for this study? What are the main findings?
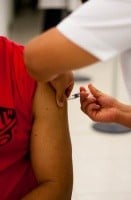
Response: To monitor the uptake of vaccines the CDC conducts a National Immunization Survey each year. This survey is conducted by random-digit dialing (cell phones or landlines) of parents and guardians of children 19-35 months of age. The interviewers ask the families who provides the vaccines for their children and if these providers can be contacted to inquire about the immunizations received. The overall response rate to the telephone survey was 26% and immunization records were provided on 54% of the children where permission was granted. Overall 15, 333 children had their immunization records reviewed.
When comparing immunization rates for 2017 and 2016, the last two years of the study, several new findings were discovered.
First the overall coverage rate for 3 doses of polio vaccine, one dose of MMR, 3 doses of Hepatitis b, and 1 dose of chickenpox vaccine was 90%, a high rate of coverage. Children were less likely to be up to date on the hepatitis A vaccine (70%) and rotavirus vaccine (73%). Coverage was lower for children living in rural areas when compared with urban areas and children living in rural areas had higher percentages of no vaccine receipt at all (1.9%) compared with those living in urban areas (1%).
There were more uninsured children in 2017 at 2.8% and these children had lower immunization rates. In fact 7.1% of the children with no insurance were totally unimmunized when compared with 0.8% unimmunized in those with private insurance. Vaccine coverage varies by state and by vaccine.
Kathryn M. Edwards, M.D.
Sarah H. Sell and Cornelius Vanderbilt Chair in Pediatrics
Professor of Pediatrics
Vanderbilt University School of Medicine
Dr. Edwards discusses the statement from the Infectious Diseases Society of America (IDSA) regarding the Centers for Disease Control and Prevention’s new data on child vaccine rates across the United States.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: To monitor the uptake of vaccines the CDC conducts a National Immunization Survey each year. This survey is conducted by random-digit dialing (cell phones or landlines) of parents and guardians of children 19-35 months of age. The interviewers ask the families who provides the vaccines for their children and if these providers can be contacted to inquire about the immunizations received. The overall response rate to the telephone survey was 26% and immunization records were provided on 54% of the children where permission was granted. Overall 15, 333 children had their immunization records reviewed.
When comparing immunization rates for 2017 and 2016, the last two years of the study, several new findings were discovered.
First the overall coverage rate for 3 doses of polio vaccine, one dose of MMR, 3 doses of Hepatitis b, and 1 dose of chickenpox vaccine was 90%, a high rate of coverage. Children were less likely to be up to date on the hepatitis A vaccine (70%) and rotavirus vaccine (73%). Coverage was lower for children living in rural areas when compared with urban areas and children living in rural areas had higher percentages of no vaccine receipt at all (1.9%) compared with those living in urban areas (1%).
There were more uninsured children in 2017 at 2.8% and these children had lower immunization rates. In fact 7.1% of the children with no insurance were totally unimmunized when compared with 0.8% unimmunized in those with private insurance. Vaccine coverage varies by state and by vaccine.

 Dr. Mubdiul Ali Imtiaz[/caption]
MedicalResearch.com Interview with:
Mubdiul Ali Imtiaz, MD
Department of Internal Medicine
Rutgers University, New Jersey Medical School
Newark, NJ 07103
Medical Research: What is the background for this study?
Response: Resident physicians (RPs) were defined to be all individuals enrolled in a graduate medical education training program in a healthcare setting. There were 611 resident physicians enrolled in 47 post-graduate residency and fellowship programs at RU-NJMS during the 2013-2014 academic year. Influenza immunization was strongly recommended, but not mandatory for Resident physicians during 2013-2014. A link to the online survey using a standardized, anonymous, self-administered questionnaire was emailed by the program-chiefs to their respective RPs to collect demographic characteristics, influenza immunization status during the 2013-2014 and the previous season, and reasons for non-vaccination.
Medical Research: What are the main findings?
Response: The overall self-reported immunization rate of Resident physicians in 2013-2014 was 76.7%. The immunization rate did not differ by the location of medical school attended (P= 0.55) or sex (P= 0.69). Among the respondents, 95.8% had influenza vaccination in the past and 83.1% received influenza vaccine during 2012-2013 flu season. History of influenza vaccination ever and in 2012-2013 were both significantly associated with receiving the vaccine during the 2013-2014 season (P<0.01 for both). The most common reason for not being vaccinated (38.6%) was “lack of time to get immunized” (see Figure 1). The most common cited motivating factors to be vaccinated during the next influenza season among the NVRPs were “making vaccinations in the workplace at convenient locations and times” (43.2%), “availability of mobile flu vaccination carts in hospital floors” (40.9%), and “establishing mandatory flu vaccination for employment” (36.4%).
Dr. Mubdiul Ali Imtiaz[/caption]
MedicalResearch.com Interview with:
Mubdiul Ali Imtiaz, MD
Department of Internal Medicine
Rutgers University, New Jersey Medical School
Newark, NJ 07103
Medical Research: What is the background for this study?
Response: Resident physicians (RPs) were defined to be all individuals enrolled in a graduate medical education training program in a healthcare setting. There were 611 resident physicians enrolled in 47 post-graduate residency and fellowship programs at RU-NJMS during the 2013-2014 academic year. Influenza immunization was strongly recommended, but not mandatory for Resident physicians during 2013-2014. A link to the online survey using a standardized, anonymous, self-administered questionnaire was emailed by the program-chiefs to their respective RPs to collect demographic characteristics, influenza immunization status during the 2013-2014 and the previous season, and reasons for non-vaccination.
Medical Research: What are the main findings?
Response: The overall self-reported immunization rate of Resident physicians in 2013-2014 was 76.7%. The immunization rate did not differ by the location of medical school attended (P= 0.55) or sex (P= 0.69). Among the respondents, 95.8% had influenza vaccination in the past and 83.1% received influenza vaccine during 2012-2013 flu season. History of influenza vaccination ever and in 2012-2013 were both significantly associated with receiving the vaccine during the 2013-2014 season (P<0.01 for both). The most common reason for not being vaccinated (38.6%) was “lack of time to get immunized” (see Figure 1). The most common cited motivating factors to be vaccinated during the next influenza season among the NVRPs were “making vaccinations in the workplace at convenient locations and times” (43.2%), “availability of mobile flu vaccination carts in hospital floors” (40.9%), and “establishing mandatory flu vaccination for employment” (36.4%).





