In the quest for a perfect smile, many people in Mount Holly, NJ, are turning to Invisalign as a discreet and effective alternative to traditional braces. Invisalign clear aligners offer a modern solution for straightening teeth without the use of wires or brackets. If you’re exploring affordable Invisalign options in Mount Holly, this guide will help you navigate the best choices for orthodontic treatment in your area.
Gaming, Pediatrics, Technology / 23.09.2024
The Influences Shaping Today’s Youth
Today’s youth are growing up in a world that is constantly evolving, shaped by rapid technological advances, shifting social norms, and global connectivity. The influences affecting their lives are more diverse and accessible than ever before, making it both an exciting and complex time to navigate adolescence. Understanding these influences is crucial in shaping the future, as today’s youth are the leaders, thinkers, and innovators of tomorrow.
This article explores the key influences shaping today’s youth, from technology and social media to global movements and shifting cultural landscapes.
- Technology and Digital Connectivity
Complementary Medicine, Prostate, Supplements / 23.09.2024
Natural Supplements for Better Prostate Health: A Comprehensive Guide
Editor's note: This article discusses supplements, which in no way are intended to substitute for professional medical care and regular prostate cancer screening. Supplements are generally not FDA tested or approved. Some supplements can interfere with medications and/or cause side effects. Do not delay seeking medical attention for prostate concerns by taking supplements without medical advice.
Please discuss any and all supplements you take with your health care provider and be sure to follow your provider's recommendations for your prostate and overall health.
As men age, maintaining good prostate health becomes a top priority. The prostate, a small gland located below the bladder, plays a significant role in male reproductive health. However, many men face challenges related to this vital organ, especially as they get older. Fortunately, natural supplements can help support prostate health and overall well-being. In this article, we'll explore the benefits of these supplements, how they work, and how you can incorporate them into your lifestyle. Before we begin, it's essential to remember that supplements like Prostovit are among many that can help, but they should always be used as part of a holistic approach to health.


Why Prostate Health is Important
The prostate is crucial for producing seminal fluid, which helps transport sperm during ejaculation. Over time, the prostate may enlarge, leading to conditions like benign prostatic hyperplasia (BPH), or even develop into more severe conditions like prostate cancer. Prostate health directly impacts urinary function and quality of life, making it a critical aspect of men’s health that shouldn’t be ignored. Symptoms such as frequent urination, especially at night, difficulty starting or stopping urination, and weak urine flow are common indicators of prostate issues. Addressing these symptoms early with lifestyle changes and natural supplements may prevent more serious complications in the future. (more…)
Pain Research, Plastic Surgery / 21.09.2024
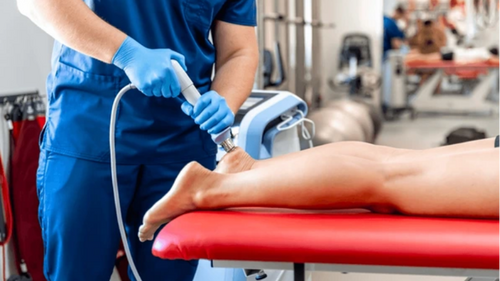
Acoustic Wave Therapy: Transforming Non-Invasive Aesthetic Treatments
Acoustic Wave Therapy (AWT) is capturing attention as a modern, non-invasive treatment option that claims to help with a variety of conditions, including erectile dysfunction and muscle pain. This therapy uses sound waves to stimulate the body's own healing processes, which can improve blood flow and promote tissue repair.
For those considering if this is a treatment worth incorporating into your clinic service, the answer is yes. AWT (Acoustic Wave Therapy) can enhance blood circulation and potentially improve sexual performance for some individuals.
It's particularly noted for helping men with vascular-related erectile dysfunction. Although not yet approved by the FDA, many clinics worldwide offer it as a promising alternative.
Aside from erectile dysfunction, acoustic wave therapy is researched for its potential benefits in reducing cellulite and chronic pain. It's a quick procedure with minimal discomfort, making it an attractive option for those looking for a less invasive therapy.
With these advantages, AWT is becoming a topic of interest for patients and medical professionals.
(more…)
Sleep is an essential element of health and so people’s claims that they have more difficulty in falling asleep remain very common. Irrespective of whether this is a passing phase or an established and chronic problem, recognizing the reasons can assist individuals in seeking possible solutions. This article discusses possible sources of sleep hindrances and recommends how to fall asleep faster.
What is Difficulty in Falling Asleep?
‘Difficulty in falling asleep’ as it sounds, by definition falls under the category of sleep disturbances that can best be referred to as sleep-onset insomnia. It is the failure to fall asleep after lying down over a period that is reasonable after bed. A person's parents who have this disorder are also more likely to have this disorder. This condition can have a detrimental influence on multiple aspects of health, resulting in low energy levels, high levels of mood swings, and poor concentration during working hours.
(more…)
 Art therapy can be described as a subcategory of psychotherapy in which art-related exercises are used as vehicles of expression. It harnesses the processes of the artistic mind to assist people with their emotional, psychological, and sometimes physical difficulties.
This type of creative art and artistic expression, which takes place under the guidance of an art therapist, is based on the idea that art and creativity contribute to psychological health and facilitate nonverbal communication. What's art therapy, and how can it help you boost your overall lifestyle? Read on to learn how art therapy can be helpful, including its effect on mental health issues, mood modulation, and health overall.
(more…)
Art therapy can be described as a subcategory of psychotherapy in which art-related exercises are used as vehicles of expression. It harnesses the processes of the artistic mind to assist people with their emotional, psychological, and sometimes physical difficulties.
This type of creative art and artistic expression, which takes place under the guidance of an art therapist, is based on the idea that art and creativity contribute to psychological health and facilitate nonverbal communication. What's art therapy, and how can it help you boost your overall lifestyle? Read on to learn how art therapy can be helpful, including its effect on mental health issues, mood modulation, and health overall.
(more…)
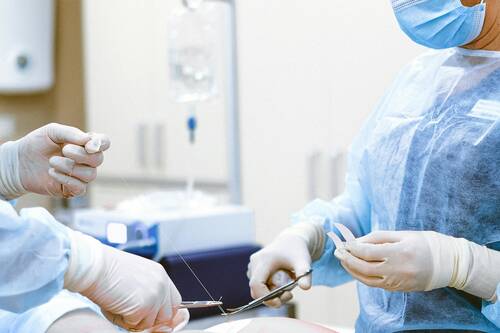
Whether planning a surgery or recovering from one, it is always important to take ample rest and prepare for a smooth experience. Preoperative preparation and post operative home care can, in fact, help minimize potential risks and ensure satisfactory outcomes.
Proactively optimizing physical and emotional well-being can help improve a patient’s overall health and increase their chances of a successful recovery. This may cover pre-surgery guidance and advice based on the patient’s medical history, dietary modifications, level and need of emotional support, and other practical considerations.
This article explores the various aspects of pre-surgery preparation to equip patients with the information and resources they need. The importance of pre-surgery care cannot be overstated, and patients must play an active role in their own healthcare for faster recovery.
(more…)
 Ever thought what are the next steps after launching a product? Once a product is launched, there is much more to do about FDA approval, particularly with health and safety products. The FDA acts as a protector and safeguard of products, be they medications or medical devices, allowed to enter the U.S. market.
Here, understanding the FDA approval process will benefit you to help understand the complex world of product approval and set real expectations of your product for the market. Let’s look at the basic structure of FDA approval and its after-process.
(more…)
Ever thought what are the next steps after launching a product? Once a product is launched, there is much more to do about FDA approval, particularly with health and safety products. The FDA acts as a protector and safeguard of products, be they medications or medical devices, allowed to enter the U.S. market.
Here, understanding the FDA approval process will benefit you to help understand the complex world of product approval and set real expectations of your product for the market. Let’s look at the basic structure of FDA approval and its after-process.
(more…)
Using Medicare can be quite challenging for those without experience dealing with this system and its numerous programs, plans, and services. Hiring a Medicare insurance agent is one of the best ways to guarantee that you get the right Medicare plan suitable for your needs. However, the problem of choosing the right agent might be even more daunting than the task of comprehending the insurance plans. This guide is designed to help you select the best Medicare insurance agent and make the right decision.
(more…)
 Pharmacovigilance is the strict monitoring process in the drug industry to ensure that drugs are safe to administer. It simply ensures that public health is kept away from harmful drugs by keeping a tab on any safety concerns with the drug once it is on the market.
This blog explains the fundamental characteristics of pharmacovigilance, its significance, and what process is applied.
(more…)
Pharmacovigilance is the strict monitoring process in the drug industry to ensure that drugs are safe to administer. It simply ensures that public health is kept away from harmful drugs by keeping a tab on any safety concerns with the drug once it is on the market.
This blog explains the fundamental characteristics of pharmacovigilance, its significance, and what process is applied.
(more…)Common Issues with Relationships
A relationship can sometimes become overwhelming to maintain. While every couple experiences struggles, certain issues may indicate that professional help could be beneficial. Recognizing these signs early on can provide a couple with a better opportunity to invest in healthier communication and strengthen their relationship with one another. Here are some key indicators that it might be time to seek couples counseling:Communication Breakdown
One of the most common indicators that it's time to arrange couples therapy is communication dysfunction. When partners struggle to communicate without raising their voices, becoming defensive, feeling unheard, or experiencing escalating frustration, these are clear signs that assistance is needed. Strong communication is a vital component of a healthy relationship. If discussions frequently devolve into arguments or silence, couples counseling in Denver can offer techniques to enhance communication skills and foster a better understanding between partners. (more…)
Aging, Nutrition / 20.09.2024
The Science of Aging: Foods That May Boost Your Body’s Natural Defenses
Aging is an inevitable part of life, but the rate and manner in which we age are influenced by several factors, including our diet. As research continues to uncover the relationship between nutrition and longevity, it’s clear that what we eat plays a pivotal role in protecting our body’s natural defenses. By incorporating nutrient-rich foods into your daily routine, you can help mitigate the effects of aging, strengthen your immune system, and improve your overall quality of life.
This article explores some of the most impactful foods to incorporate into your diet to naturally support healthy aging.
Understanding the Aging Process
Aging is a complex biological process that involves the gradual decline of cellular function. As we age, our cells undergo oxidative stress, a condition where free radicals—unstable molecules—cause damage to our DNA, proteins, and lipids. This damage accumulates over time, leading to inflammation, chronic diseases, and a weakened immune system. However, certain foods are rich in antioxidants, which help neutralize free radicals and protect the body’s cells from oxidative damage. Additionally, many foods contain anti-inflammatory properties, essential vitamins, and minerals that support the body’s natural repair mechanisms, helping you stay healthier for longer. (more…)
Supporting a loved one with a disability is not only challenging for the caregiver but can also be incredibly difficult for the person living with the disability. Daily tasks, social interactions, and emotional well-being often become more complicated to manage, leading to frustration and feelings of isolation.
However, with the right approach and practical strategies, you can provide valuable support that makes a real difference for both of you. This guide outlines five key ways to effectively assist a family member with a disability, helping to create a more supportive and understanding environment.
(more…)
Endocrinology, Pharmacology / 20.09.2024
The Science and Benefits Behind Next-Generation Hormone Regulation Treatments
Editor's note: Consult with your medical provider beginner any form of potential hormonal regulation therapy.
The discussion below has not been FDA verified or approved and should not be construed as specific medical advice.
The field of hormone regulation has evolved significantly, offering new treatments that aim to restore balance and improve overall well-being.
MedicalNewsToday states that most people go through natural hormonal fluctuations at various stages of their lives. However, imbalances can emerge when the endocrine glands, which create and release hormones into the circulation, do not operate properly. These glands are distributed throughout the body, and each of them handles different organs and physical activities.
As more individuals seek solutions for hormone-related issues like fatigue, weight gain, and mood swings, next-generation hormone regulation treatments are becoming increasingly popular.
These innovative therapies, such as hormone pellet therapy, bioidentical hormone replacement therapy (BHRT), and peptide therapy, target specific imbalances to provide personalized solutions. These treatments offer hope for improved health, vitality, and quality of life by addressing the root causes of hormone disruptions.
(more…)
Complementary Medicine / 19.09.2024
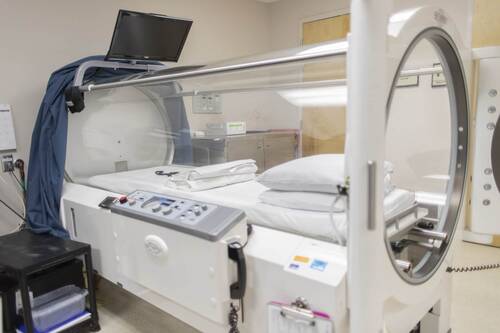
The Evolving Landscape of Oxygen Therapy: Recent Advances and Their Impact on Patient Outcomes
Oxygen therapy has come a long way since its early days. Initially, it was a simple and somewhat limited treatment.
Today, it’s a sophisticated field with a range of innovative technologies improving patient care.
This article explores the latest advancements in oxygen therapy and how they are reshaping patient outcomes.
Historical Context of Oxygen Therapy
Oxygen therapy began as a crucial intervention for treating respiratory conditions. Early on, it was used primarily in hospitals with basic equipment, often involving cumbersome tanks and limited delivery systems. As technology progressed, so did the methods of oxygen delivery. In the past, oxygen was administered mainly through large, stationary tanks. These setups were not always practical for patients needing ongoing therapy at home. The early technologies had significant limitations, including bulkiness and high costs. The evolution from these basic methods to more sophisticated systems marks a significant shift in patient care.] (more…)
Semaglutide, Weight Research / 18.09.2024
What You Need to Know About the Wegovy Pen for Weight Loss
If you’ve been hearing a lot of buzz about the Wegovy pen and are curious about what it can do for weight loss, you're in the right place. There’s a lot to understand, but we’re going to break it down into simple, easy-to-follow information. Whether you're exploring your options or have already made up your mind about giving it a try, here's everything you need to know about the Wegovy pen.
What is the Wegovy Pen?
Let’s start with the basics. The Wegovy pen is a once-weekly injectable medication that’s used to support weight loss in adults. It contains the active ingredient semaglutide, which is designed to help regulate appetite. In simple terms, it helps you feel fuller for longer, so you're less likely to overeat. Semaglutide mimics a hormone called GLP-1 (glucagon-like peptide-1), which plays a role in controlling hunger. By imitating this hormone, Wegovy helps reduce food cravings and manages how much you eat. (more…)
Chiropractic, Pain Research / 18.09.2024
Effective Chiropractic Techniques for Alleviating Lower Back Pain
Editor's note: Be sure to check with your health care provider for new, persistent or changing pain before embarking on any therapeutic maneuvers.
Lower back pain, a common issue affecting millions, can result from flawed posture, injuries, or chronic illnesses. Chiropractic treatment offers an effective, non-invasive method to alleviate this discomfort by concentrating on spinal adjustments and manipulations to restore alignment and improve mobility. Through targeted techniques, chiropractors help reduce pain and promote healing.
In this article, we will analyze effective chiropractic methods for relieving lower back pain and improving overall spinal health.
Understanding Lower Back Pain(LBP)
Lower back pain is a widespread condition caused by muscle strain, poor posture, herniated discs, or underlying medical ailments like arthritis. It can occur due to sudden movements, prolonged sitting, heavy lifting, or age-related wear and tear on the spine. While common in older adults due to degenerative changes, lower back pain can affect people of any age, including young adults, athletes, etc. According to Statista, around 28% of American adults were found to have chronic lower back pain in 2022. More than 44% of adults having chronic back pain have been suffering for 5 years or more. The pain has deteriorated their quality of life. Risk factors that may cause back pain include obesity, sedentary lifestyles, lack of exercise, and certain occupations. Regardless of age, lower back pain can disrupt daily actions, limiting movement and quality of life for many individuals. Lower back pain (LBP) has impacted around 619 million people worldwide in 2020. The WHO estimates that this number will go up to 843 million by 2050. (more…)
Overcoming drug addiction is a profound transformation, marking the start of a new chapter in an individual’s life. It's not just about abstaining from substances, but also about rebuilding a life that was once overshadowed by dependency. Achieving lasting sobriety requires dedication, the right support systems, and an assortment of strategies tailored to maintain wellness and purpose. This journey is unique for everyone, but there are commonalities in the experience that can guide those looking to create a fresh start. Keep reading to explore the facets of recovery and rebuild a fulfilling life after addiction.
 Recovery from drug addiction is a complex, non-linear process that extends beyond just stopping substance use. It involves a comprehensive lifestyle change, addressing both psychological and physiological aspects of addiction. Therapy and counseling are crucial for uncovering and tackling the underlying issues that contributed to substance use, helping individuals develop healthy coping strategies and avoid relapse.
The journey often begins with detoxification, where the body cleanses itself of substances. A luxury rehab in Hawaii can provide a supportive, serene environment during this challenging phase. Recovery requires patience and self-compassion, with each day of sobriety representing progress towards a healthier, more fulfilling life. Celebrating small victories and staying resilient are key to navigating the path to recovery.
Recovery from drug addiction is often described as a journey rather than a destination. It involves several stages, including:
Recovery from drug addiction is a complex, non-linear process that extends beyond just stopping substance use. It involves a comprehensive lifestyle change, addressing both psychological and physiological aspects of addiction. Therapy and counseling are crucial for uncovering and tackling the underlying issues that contributed to substance use, helping individuals develop healthy coping strategies and avoid relapse.
The journey often begins with detoxification, where the body cleanses itself of substances. A luxury rehab in Hawaii can provide a supportive, serene environment during this challenging phase. Recovery requires patience and self-compassion, with each day of sobriety representing progress towards a healthier, more fulfilling life. Celebrating small victories and staying resilient are key to navigating the path to recovery.
Recovery from drug addiction is often described as a journey rather than a destination. It involves several stages, including:
Understanding the Journey of Recovery from Drug Addiction
 Recovery from drug addiction is a complex, non-linear process that extends beyond just stopping substance use. It involves a comprehensive lifestyle change, addressing both psychological and physiological aspects of addiction. Therapy and counseling are crucial for uncovering and tackling the underlying issues that contributed to substance use, helping individuals develop healthy coping strategies and avoid relapse.
The journey often begins with detoxification, where the body cleanses itself of substances. A luxury rehab in Hawaii can provide a supportive, serene environment during this challenging phase. Recovery requires patience and self-compassion, with each day of sobriety representing progress towards a healthier, more fulfilling life. Celebrating small victories and staying resilient are key to navigating the path to recovery.
Recovery from drug addiction is often described as a journey rather than a destination. It involves several stages, including:
Recovery from drug addiction is a complex, non-linear process that extends beyond just stopping substance use. It involves a comprehensive lifestyle change, addressing both psychological and physiological aspects of addiction. Therapy and counseling are crucial for uncovering and tackling the underlying issues that contributed to substance use, helping individuals develop healthy coping strategies and avoid relapse.
The journey often begins with detoxification, where the body cleanses itself of substances. A luxury rehab in Hawaii can provide a supportive, serene environment during this challenging phase. Recovery requires patience and self-compassion, with each day of sobriety representing progress towards a healthier, more fulfilling life. Celebrating small victories and staying resilient are key to navigating the path to recovery.
Recovery from drug addiction is often described as a journey rather than a destination. It involves several stages, including:
- Acknowledgment: The first step is recognizing the problem and understanding the impact of addiction on your life and those around you.
- Seeking Help: Many individuals benefit from professional help, which may include therapy, counseling, or rehabilitation programs.
- Detoxification: This process allows the body to rid itself of drugs. It can be physically and emotionally taxing, requiring medical supervision in some cases.
- Rehabilitation: This phase focuses on building coping mechanisms and developing strategies to avoid relapse.
- Aftercare: Maintaining sobriety involves ongoing support and continuous self-improvement.
Editor's note: If you purchase semaglutide or similar medications, be sure to be followed by your health care provider and verify that the supplier is reputable before your purchases.
When it comes to weight loss, it often feels like everyone has an opinion. Some swear by keto, while others say it's all about intermittent fasting. And let’s not forget the ever-popular crash diets that promise instant results but leave you feeling sluggish and starving. With so much conflicting advice, how can you figure out what actually works?
This post attempts to break down the science behind weight loss, cutting through the noise and getting to the core of what really makes a difference in shedding those extra pounds—without the fads.


Calories In, Calories Out: The Basics
At its most fundamental level, weight loss comes down to one basic principle: calories in versus calories out. The idea is simple—if you consume fewer calories than your body needs, you'll lose weight. This is known as creating a calorie deficit. Your body has to find energy somewhere, and when you're not giving it enough through food, it starts to use stored fat. However, it's not always as straightforward as it seems. People have different metabolic rates, meaning some burn calories faster than others. Plus, hormones, genetics, and lifestyle factors can all affect how easy or difficult it is to drop pounds. This is why two people on the same diet might experience different results. Key takeaway: To lose weight, you need to consistently eat fewer calories than you burn. But keep in mind that individual factors can influence how quickly (or slowly) this happens for you. (more…)
Navigating the road to recovery after addiction can be arduous, requiring not only physical detoxification but also mental fortification. Individuals seeking to rebuild their lives must engage in therapies that heal both the mind and body, forging a path to a future free from dependence. Recognizing that addiction is not just a series of poor choices but rather a complex interplay of psychological and physiological factors is essential for compassionate and effective treatment. In this article, readers will unearth the strategies and therapies pivotal in constructing a resilient support system, and they will learn about holistic approaches essential for long-term sobriety. Keep reading to embrace the possibility of transformation and to gather invaluable insights into the journey of rediscovery after addiction.
 Recovery from addiction signifies more than abstinence; it's a comprehensive transformation of mind and body. The initial phase prioritizes physical stabilization, ensuring individuals emerge from the shadow of substance dependence. This first step lays the groundwork for reclaiming control over one’s health and well-being.
(more…)
Recovery from addiction signifies more than abstinence; it's a comprehensive transformation of mind and body. The initial phase prioritizes physical stabilization, ensuring individuals emerge from the shadow of substance dependence. This first step lays the groundwork for reclaiming control over one’s health and well-being.
(more…)
Healing the Mind and Body: The First Steps in Recovery
 Recovery from addiction signifies more than abstinence; it's a comprehensive transformation of mind and body. The initial phase prioritizes physical stabilization, ensuring individuals emerge from the shadow of substance dependence. This first step lays the groundwork for reclaiming control over one’s health and well-being.
(more…)
Recovery from addiction signifies more than abstinence; it's a comprehensive transformation of mind and body. The initial phase prioritizes physical stabilization, ensuring individuals emerge from the shadow of substance dependence. This first step lays the groundwork for reclaiming control over one’s health and well-being.
(more…)
Addiction, addiction-treatment, Alcohol / 17.09.2024
Moving Forward After Overcoming Alcohol Addiction
Overcoming alcohol addiction is both a triumph and a beginning—a launchpad for a new narrative in one’s life. The journey through recovery is often fraught with challenges, but it is also filled with opportunities for personal growth and transformation. Crafting a post-addiction life can be a profound experience that fosters strength, resilience, and joy. Below, we'll explore the key elements that contribute to a successful and fulfilling life beyond alcohol dependency. Keep reading to learn how to embrace this new chapter with confidence and hope.
 Breaking free from alcohol’s hold brings a new sense of freedom, allowing individuals to rediscover old passions and interests. Celebrating every small victory is crucial, as is recognizing the immense effort required to stay sober. Support from loved ones and professionals plays a significant role in this journey, providing essential encouragement and guidance.
Transitioning from a luxury alcohol rehab to daily life involves building a stable routine that supports sobriety. Engaging in regular exercise, exploring creative activities, and maintaining good sleep habits help create a sense of normalcy. As life changes, developing effective coping mechanisms for stress and being patient with oneself are vital for navigating this ongoing journey toward lasting recovery.
(more…)
Breaking free from alcohol’s hold brings a new sense of freedom, allowing individuals to rediscover old passions and interests. Celebrating every small victory is crucial, as is recognizing the immense effort required to stay sober. Support from loved ones and professionals plays a significant role in this journey, providing essential encouragement and guidance.
Transitioning from a luxury alcohol rehab to daily life involves building a stable routine that supports sobriety. Engaging in regular exercise, exploring creative activities, and maintaining good sleep habits help create a sense of normalcy. As life changes, developing effective coping mechanisms for stress and being patient with oneself are vital for navigating this ongoing journey toward lasting recovery.
(more…)
Embracing a New Chapter: The Journey Beyond Alcohol Dependency
 Breaking free from alcohol’s hold brings a new sense of freedom, allowing individuals to rediscover old passions and interests. Celebrating every small victory is crucial, as is recognizing the immense effort required to stay sober. Support from loved ones and professionals plays a significant role in this journey, providing essential encouragement and guidance.
Transitioning from a luxury alcohol rehab to daily life involves building a stable routine that supports sobriety. Engaging in regular exercise, exploring creative activities, and maintaining good sleep habits help create a sense of normalcy. As life changes, developing effective coping mechanisms for stress and being patient with oneself are vital for navigating this ongoing journey toward lasting recovery.
(more…)
Breaking free from alcohol’s hold brings a new sense of freedom, allowing individuals to rediscover old passions and interests. Celebrating every small victory is crucial, as is recognizing the immense effort required to stay sober. Support from loved ones and professionals plays a significant role in this journey, providing essential encouragement and guidance.
Transitioning from a luxury alcohol rehab to daily life involves building a stable routine that supports sobriety. Engaging in regular exercise, exploring creative activities, and maintaining good sleep habits help create a sense of normalcy. As life changes, developing effective coping mechanisms for stress and being patient with oneself are vital for navigating this ongoing journey toward lasting recovery.
(more…)
Legal-Malpractice, Regulations, Technology / 16.09.2024
Key Steps for Ensuring SFDA Compliance for Medical Device Registration
 Manufacturers must comply with the requirements set by Saudi Food and Drug Authority (SFDA) regulations to export into the Saudi market. The SFDA process of registering medical devices is necessary to ensure that the medical devices exported to Saudi Arabia are expected to meet safety and quality standards.
This blog explains how manufacturers can create a step-by-step navigation of the SFDA medical device registration process to ensure compliance and preparation for the market.
(more…)
Manufacturers must comply with the requirements set by Saudi Food and Drug Authority (SFDA) regulations to export into the Saudi market. The SFDA process of registering medical devices is necessary to ensure that the medical devices exported to Saudi Arabia are expected to meet safety and quality standards.
This blog explains how manufacturers can create a step-by-step navigation of the SFDA medical device registration process to ensure compliance and preparation for the market.
(more…)It is important for your recovery to find a physical therapist who understands sciatica and has experience treating it. Look...
It is important to work closely with a doctor to monitor your treatment and adjust it if needed. Not all...
Introduction
Shoulder tendonitis is a common problem that causes pain and stiffness in the shoulder. It often happens when the tendons in your shoulder get overused or irritated. Everyday activities like lifting, reaching, or playing sports can lead to tendonitis. If left untreated, it can get worse over time and limit your ability to move your arm. Physical therapy is one of the best ways to heal shoulder tendonitis. It helps reduce pain, improve movement, and strengthen the muscles around the shoulder. With the right exercises and treatment, physical therapy can speed up recovery and prevent the problem from coming back. In this guide, we’ll explain how physical therapy for shoulder tendonitis can help and what you can expect from treatment. (more…)
Aging, Nursing / 14.09.2024
Resources for Caring for an Elderly Family Member
Legal planning is an essential aspect of long-term care for elderly family members. Establishing power of attorney, creating living wills,...
Choosing the right nursing care facility for a loved one is an important decision that requires thorough evaluation and thoughtful planning. Whether for short-term rehabilitation or long-term care, finding a facility that meets both medical needs and emotional well-being is crucial. Here are some key steps to help guide your decision-making process.
Determine Your Loved One’s Care Requirements
Start by identifying the specific needs of your loved one. This includes their current medical conditions, level of mobility, dietary preferences, and any special needs like regular medication or therapeutic support. Having a clear picture of these requirements will help you identify the most suitable care setting. When evaluating potential facilities, you can find detailed information and compare different options for nursing care services with careforfamily.com.au to help guide your decision. (more…)
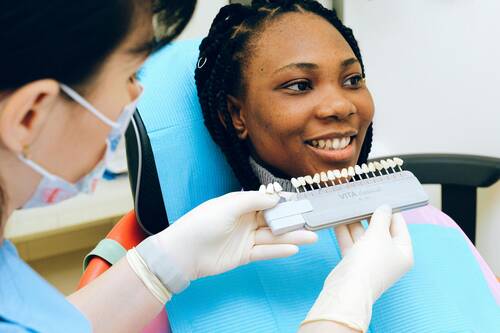
A great smile can boost your confidence, help you feel more comfortable in social situations, and even make a lasting first impression. Thanks to advancements in cosmetic dentistry, transforming your smile has never been easier. But with so many options available, how do you know which procedure is right for you? Let’s break down five popular cosmetic dental treatments that can give you a smile makeover.
1. Teeth Whitening – A Quick Brightness Boost
When it comes to brightening your smile, teeth whitening is hands-down one of the most popular treatments from a cosmetic dentist. Whether you're dealing with coffee stains, years of wear and tear, or just want to amp up the brightness, teeth whitening offers a simple solution. Professional teeth whitening is far more effective than over-the-counter treatments. It’s quick, relatively inexpensive, and can brighten your teeth by several shades in just one session. Many people love how easy it is to transform their smile with such minimal effort. While results are immediate, they can last a long time with proper care—just avoid too much coffee or red wine afterward! (more…)Disclaimer: Encer is a homeopathic product has not been evaluated by the Food and Drug Administration for safety or efficacy. FDA is not aware of scientific evidence to support homeopathy as effective.
In the diverse and evolving field of complementary and alternative medicine, homeopathy has established a distinct presence. Encer - a homeopathic medicine used for its potential in managing cancer-related fatigue (CRF), a prevalent and debilitating symptom affecting individuals diagnosed with cancer.What is Encer
Encer is a homeopathic remedy designed with a blend of highly diluted natural substances. Following the homeopathic principle of "like cures like," it is formulated to stimulate the body's self-healing mechanisms. Despite the absence of Encer in mainstream pharmacological references, as it's a concept perhaps more familiar within homeopathic circles, its use is aimed at providing a non-toxic, gentle treatment option for managing the symptoms of cancer and its treatment, including CRF. (more…)
Editor's note: Remember to follow your health care providers' instructions regarding regular breast examinations and mammograms. Don't wait for a sign or symptom of breast cancer to get screened.
Breast cancer is one of the most prevalent cancers affecting women worldwide. While it can be a frightening diagnosis, early detection significantly improves treatment outcomes and survival rates. By being aware of the symptoms of breast cancer, individuals can take proactive steps to seek medical attention, ensuring the best possible chance for early intervention. In this article, we’ll walk through the key signs to watch for and the importance of understanding your body.