Author Interviews, Cancer Research, Dental Research, Opiods / 23.07.2019
Phototherapy Improves Oral Side Effects of Cancer Treatment
MedicalResearch.com Interview with:
[caption id="attachment_50367" align="alignleft" width="200"] Dr. Arany[/caption]
Praveen Arany, DDS, PhD
Department of Oral Biology
School of Dental Medicine
University of Buffalo
MedicalResearch.com: What is the background for this study? How is the light treatment delivered?
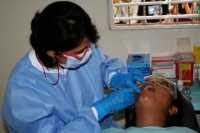
Response: Cancers are usually treated with chemotherapy and/or radiation to destroy the tumor cells. However, an unfortunate side-effect of these treatments is pain and ulcers in the mouth due to breakdown of normal protective responses.
Light has various applications in human health and normal physiology. Two good examples are vision and sunlight-Vitamin D for bone and health. The use of low dose light to alleviate pain or inflammation and promote tissue healing is termed Photobiomodulation (PBM) Therapy.
This treatment can be provided with lasers or LED devices at specific wavelength (color) and dose (power). This treatment is currently being provided by a health care provider - usually a laser - either nurse or dentist prior or during the cancer treatments. There are several exciting innovation where take-home, self-use devices are becoming available.
Dr. Arany[/caption]
Praveen Arany, DDS, PhD
Department of Oral Biology
School of Dental Medicine
University of Buffalo
MedicalResearch.com: What is the background for this study? How is the light treatment delivered?
Response: Cancers are usually treated with chemotherapy and/or radiation to destroy the tumor cells. However, an unfortunate side-effect of these treatments is pain and ulcers in the mouth due to breakdown of normal protective responses.
Light has various applications in human health and normal physiology. Two good examples are vision and sunlight-Vitamin D for bone and health. The use of low dose light to alleviate pain or inflammation and promote tissue healing is termed Photobiomodulation (PBM) Therapy.
This treatment can be provided with lasers or LED devices at specific wavelength (color) and dose (power). This treatment is currently being provided by a health care provider - usually a laser - either nurse or dentist prior or during the cancer treatments. There are several exciting innovation where take-home, self-use devices are becoming available.
 Dr. Arany[/caption]
Praveen Arany, DDS, PhD
Department of Oral Biology
School of Dental Medicine
University of Buffalo
MedicalResearch.com: What is the background for this study? How is the light treatment delivered?
Response: Cancers are usually treated with chemotherapy and/or radiation to destroy the tumor cells. However, an unfortunate side-effect of these treatments is pain and ulcers in the mouth due to breakdown of normal protective responses.
Light has various applications in human health and normal physiology. Two good examples are vision and sunlight-Vitamin D for bone and health. The use of low dose light to alleviate pain or inflammation and promote tissue healing is termed Photobiomodulation (PBM) Therapy.
This treatment can be provided with lasers or LED devices at specific wavelength (color) and dose (power). This treatment is currently being provided by a health care provider - usually a laser - either nurse or dentist prior or during the cancer treatments. There are several exciting innovation where take-home, self-use devices are becoming available.
Dr. Arany[/caption]
Praveen Arany, DDS, PhD
Department of Oral Biology
School of Dental Medicine
University of Buffalo
MedicalResearch.com: What is the background for this study? How is the light treatment delivered?
Response: Cancers are usually treated with chemotherapy and/or radiation to destroy the tumor cells. However, an unfortunate side-effect of these treatments is pain and ulcers in the mouth due to breakdown of normal protective responses.
Light has various applications in human health and normal physiology. Two good examples are vision and sunlight-Vitamin D for bone and health. The use of low dose light to alleviate pain or inflammation and promote tissue healing is termed Photobiomodulation (PBM) Therapy.
This treatment can be provided with lasers or LED devices at specific wavelength (color) and dose (power). This treatment is currently being provided by a health care provider - usually a laser - either nurse or dentist prior or during the cancer treatments. There are several exciting innovation where take-home, self-use devices are becoming available.

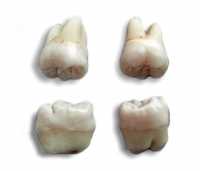



 It was noted that the differentiation of the structures of the developing jaws is ahead of other divisions. The presence of chromophobic spindle-shaped cells migrating in the direction of the tooth rudiments and their location in the region surrounding the enamel organ indicates intercellular interactions in the development of teeth in humans that differ from these processes in lower vertebrates. At the present stage, it is known that ectomesenchyme is involved in cell assemblies participating in the development of dentin.
It was noted that the differentiation of the structures of the developing jaws is ahead of other divisions. The presence of chromophobic spindle-shaped cells migrating in the direction of the tooth rudiments and their location in the region surrounding the enamel organ indicates intercellular interactions in the development of teeth in humans that differ from these processes in lower vertebrates. At the present stage, it is known that ectomesenchyme is involved in cell assemblies participating in the development of dentin.



 Prof. Thornhill[/caption]
Martin H. Thornhill MBBS, BDS, PhD, MSc, FDSRCS(Edin), FDSRCSI, FDSRCS(Eng)
Professor of Translational Research in Dentistry
Academic Unit of Oral & Maxillofacial Medicine Surgery & Pathology,
University of Sheffield School of Clinical Dentistry
MedicalResearch.com: What is the background for this study?
Response: Infective endocarditis is an infection of the heart valves that has a high death rate (around 30% in the first year). It requires intensive treatment often involving replacement of affected heart valves and frequently results in serious long-term illness and disability in those who survive as well as an increased risk of re-infection and high healthcare costs.
In ~40% of cases, bacteria from the mouth are implicated as the causal organism. Because of this, guideline committees around the world recommended that all those at risk of infective endocarditis should receive antibiotic prophylaxis before undergoing invasive dental procedures. Due to a lack of evidence for efficacy, however, guideline committees started to limit the use of antibiotic prophylaxis. And in 2007, the American Heart Association (AHA) guideline committee recommended that antibiotic prophylaxis should continue for those at high-risk but should cease for those at moderate risk of endocarditis. Most guideline countries around the world followed suite. Except in the UK, where the National Institute for Health and Care Excellence (NICE) recommended that the use of antibiotic prophylaxis should completely stop in 2008.
Prof. Thornhill[/caption]
Martin H. Thornhill MBBS, BDS, PhD, MSc, FDSRCS(Edin), FDSRCSI, FDSRCS(Eng)
Professor of Translational Research in Dentistry
Academic Unit of Oral & Maxillofacial Medicine Surgery & Pathology,
University of Sheffield School of Clinical Dentistry
MedicalResearch.com: What is the background for this study?
Response: Infective endocarditis is an infection of the heart valves that has a high death rate (around 30% in the first year). It requires intensive treatment often involving replacement of affected heart valves and frequently results in serious long-term illness and disability in those who survive as well as an increased risk of re-infection and high healthcare costs.
In ~40% of cases, bacteria from the mouth are implicated as the causal organism. Because of this, guideline committees around the world recommended that all those at risk of infective endocarditis should receive antibiotic prophylaxis before undergoing invasive dental procedures. Due to a lack of evidence for efficacy, however, guideline committees started to limit the use of antibiotic prophylaxis. And in 2007, the American Heart Association (AHA) guideline committee recommended that antibiotic prophylaxis should continue for those at high-risk but should cease for those at moderate risk of endocarditis. Most guideline countries around the world followed suite. Except in the UK, where the National Institute for Health and Care Excellence (NICE) recommended that the use of antibiotic prophylaxis should completely stop in 2008.







 Dr. Wactawski-Wende[/caption]
Jean Wactawski-Wende, PhD
Dean, SUNY Distinguished Professor
Professor, Department of Epidemiology and Environmental Health
School of Public Health and Health Professions
University of Buffalo
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There has been a growing interest in the role of periodontal disease in system chronic diseases, including cancer. We explored the association of periodontal disease history and incident cancer in the women's health initiative study of postmenopausal women. We found that women reporting periodontal disease history were at increased risk of developing cancer overall. In addition they were found to have significant increased risk of specific cancers including cancers of the lung, breast, esophagus, gallbladder and melanoma. The risk persisted after control for many other factors. In addition, the risk was seen in women regardless of their smoking history. Both ever smokers and never smokers were found to have increased risk of cancer associated with periodontal disease history.
Dr. Wactawski-Wende[/caption]
Jean Wactawski-Wende, PhD
Dean, SUNY Distinguished Professor
Professor, Department of Epidemiology and Environmental Health
School of Public Health and Health Professions
University of Buffalo
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There has been a growing interest in the role of periodontal disease in system chronic diseases, including cancer. We explored the association of periodontal disease history and incident cancer in the women's health initiative study of postmenopausal women. We found that women reporting periodontal disease history were at increased risk of developing cancer overall. In addition they were found to have significant increased risk of specific cancers including cancers of the lung, breast, esophagus, gallbladder and melanoma. The risk persisted after control for many other factors. In addition, the risk was seen in women regardless of their smoking history. Both ever smokers and never smokers were found to have increased risk of cancer associated with periodontal disease history.



