MedicalResearch.com Interview with:
[caption id="attachment_32393" align="alignleft" width="200"]

Dr. David Gaist[/caption]
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The incidence of subdural hematoma (SDH; a bleed located within the skull, but outside the brain) has been reported to be on the increase. Previous studies have shown an association between use of antithrombotic drugs and SDH. However, studies with updated estimates of this risk and with focus on current more complex and aggressive regimens of antithrombotic treatment are scarce.
We therefore performed this study, where we identified 10,010 patients aged 20-89 years that were admitted with SDH in Denmark in 2000 through 2015. Preadmission use of antithrombotic drugs (low-dose aspirin, clopidogrel, vitamin K antagonist, e.g. warfarin, and direct oral anticoagulants) of these cases was compared to that of 400,380 individuals from the general population with no history of SDH (controls).
We found that use of antithrombotic drugs was associated with an increased risk of subdural hematoma . The magnitude of this risk varied by type of antithrombotic, and was, e.g., low for use of low-dose aspirin, and highest for warfarin. Further, with a single exception (low-dose aspirin and dipyridamole), concurrent use of more than one antithrombotic drug was associated with higher risk of SDH, particularly if warfarin was taken along with an antiplatelet drug, e.g., low-dose aspirin or
clopidogrel. Increasing use of antithrombotic drugs was observed in the study period. The incidence of subdural hematomas in the Danish population also increased markedly in the years 2000-2015, particularly among those aged 75+ years. Our study indicates that this increased incidence, can, at least partly, be explained by increased use of antithrombotic drugs.
 Image courtesy of Pexels[/caption]
Image courtesy of Pexels[/caption]





 Dr. Singer[/caption]
Daniel E. Singer, MD
Professor of Medicine, Harvard Medical School
Professor in the Department of Epidemiology
Harvard T.H. Chan School of Public Health
Division of General Internal Medicine
Massachusetts General Hospital
Boston, MA, 02114
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) raises the risk of ischemic stroke 4-5-fold and this risk is largely reversible by oral anticoagulants (OAC). These facts are part of the core knowledge of internal medicine and the basis of multiple guidelines. They are based on studies of patients with persistent or predominantly “heavy burden” paroxysmal AF completed in the 1990s.
More recent studies using cardiac implantable devices (CIEDs: implantable defibrillators, pacemakers, etc) which have the capacity to monitor heart rhythm continuously have found that many older patients have brief, often undiagnosed, episodes of AF. Several of these studies have found that strokes occur during periods of sinus rhythm temporally distant from a preceding episode of AF. This has led to a widespread suspicion that AF is not a direct causal risk factor but a risk “marker” indicating the presence of other truly causal features like a diseased left atrium (atrial myopathy). If the risk marker hypothesis is correct, then long-term anticoagulation is needed even for brief and rare episodes of AF (assuming the patient’ s CHA2DS2-VASc score is high enough). The key problem with prior prospective studies using CIEDs was that only a small number of strokes were observed leading to inadequate statistical power.
Our study addressed this power problem by linking the very large Optum electronic health record database which could identify ischemic strokes with the Medtronic CareLink database of long-term, continuous heart rhythm records of patients with CIEDs. We ended up studying 891 individuals who had an ischemic stroke and had 120 days of continuous heart monitoring prior to the stroke.
Dr. Singer[/caption]
Daniel E. Singer, MD
Professor of Medicine, Harvard Medical School
Professor in the Department of Epidemiology
Harvard T.H. Chan School of Public Health
Division of General Internal Medicine
Massachusetts General Hospital
Boston, MA, 02114
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) raises the risk of ischemic stroke 4-5-fold and this risk is largely reversible by oral anticoagulants (OAC). These facts are part of the core knowledge of internal medicine and the basis of multiple guidelines. They are based on studies of patients with persistent or predominantly “heavy burden” paroxysmal AF completed in the 1990s.
More recent studies using cardiac implantable devices (CIEDs: implantable defibrillators, pacemakers, etc) which have the capacity to monitor heart rhythm continuously have found that many older patients have brief, often undiagnosed, episodes of AF. Several of these studies have found that strokes occur during periods of sinus rhythm temporally distant from a preceding episode of AF. This has led to a widespread suspicion that AF is not a direct causal risk factor but a risk “marker” indicating the presence of other truly causal features like a diseased left atrium (atrial myopathy). If the risk marker hypothesis is correct, then long-term anticoagulation is needed even for brief and rare episodes of AF (assuming the patient’ s CHA2DS2-VASc score is high enough). The key problem with prior prospective studies using CIEDs was that only a small number of strokes were observed leading to inadequate statistical power.
Our study addressed this power problem by linking the very large Optum electronic health record database which could identify ischemic strokes with the Medtronic CareLink database of long-term, continuous heart rhythm records of patients with CIEDs. We ended up studying 891 individuals who had an ischemic stroke and had 120 days of continuous heart monitoring prior to the stroke.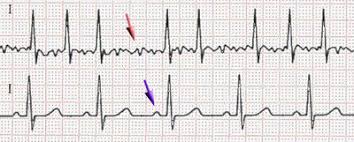
 Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
 Dr. Phelan[/caption]
Dermot Phelan, MD, PhD
Director of the Sports Cardiology Center
Cleveland Clinic in Cleveland, Ohio
MedicalResearch.com: What is the background for this study?
Response: It is well recognized that long-term elite endurance athletes are at higher risk of atrial fibrillation. We wished to evaluate whether this held true for primarily strength-type athletes. We had the opportunity to screen almost 500 former NFL athletes. It became clear that we were seeing more atrial fibrillation than one would expect during the screenings.
Dr. Phelan[/caption]
Dermot Phelan, MD, PhD
Director of the Sports Cardiology Center
Cleveland Clinic in Cleveland, Ohio
MedicalResearch.com: What is the background for this study?
Response: It is well recognized that long-term elite endurance athletes are at higher risk of atrial fibrillation. We wished to evaluate whether this held true for primarily strength-type athletes. We had the opportunity to screen almost 500 former NFL athletes. It became clear that we were seeing more atrial fibrillation than one would expect during the screenings.



 Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
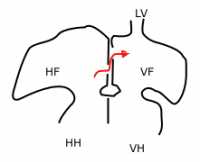
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.
Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.













