Alzheimer's - Dementia, Author Interviews, JAMA / 22.06.2024
Alzheimer’s Patients: Elevated Amyloid Detected on PET Scans of Family Members
MedicalResearch.com Interview with:
[caption id="attachment_62050" align="alignleft" width="150"] Dr. Seto[/caption]
Mabel Seto, PhD
Harvard Aging Brain Study, Department of Neurology
Massachusetts General Hospital, Center for Alzheimer Research and Treatment
Department of Neurology
Brigham and Women’s Hospital
Harvard Medical School, Boston, Massachusetts
Vanderbilt Memory and Alzheimer’s Center
Vanderbilt University Medical Center
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: The background for this study is that individuals with a family history of Alzheimer’s disease (i.e., one or more first-degree relatives) have a higher risk for the disease than individuals that don’t have a family history. Previous studies suggested a preferential maternal inheritance of AD, though they were limited in sample size and statistical power.
In our study, we wanted to focus on a larger, cognitively unimpaired sample. Using data from the Anti-Amyloid Treatment in Asymptomatic Alzheimer’s (A4) study, a randomized clinical trial aimed at AD prevention, we examined the relationship between a parental history of significant memory impairment as a proxy for AD (as some individuals may not have pursued formal diagnosis) and amyloid-beta burden in the offspring.
Dr. Seto[/caption]
Mabel Seto, PhD
Harvard Aging Brain Study, Department of Neurology
Massachusetts General Hospital, Center for Alzheimer Research and Treatment
Department of Neurology
Brigham and Women’s Hospital
Harvard Medical School, Boston, Massachusetts
Vanderbilt Memory and Alzheimer’s Center
Vanderbilt University Medical Center
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: The background for this study is that individuals with a family history of Alzheimer’s disease (i.e., one or more first-degree relatives) have a higher risk for the disease than individuals that don’t have a family history. Previous studies suggested a preferential maternal inheritance of AD, though they were limited in sample size and statistical power.
In our study, we wanted to focus on a larger, cognitively unimpaired sample. Using data from the Anti-Amyloid Treatment in Asymptomatic Alzheimer’s (A4) study, a randomized clinical trial aimed at AD prevention, we examined the relationship between a parental history of significant memory impairment as a proxy for AD (as some individuals may not have pursued formal diagnosis) and amyloid-beta burden in the offspring.
 Dr. Seto[/caption]
Mabel Seto, PhD
Harvard Aging Brain Study, Department of Neurology
Massachusetts General Hospital, Center for Alzheimer Research and Treatment
Department of Neurology
Brigham and Women’s Hospital
Harvard Medical School, Boston, Massachusetts
Vanderbilt Memory and Alzheimer’s Center
Vanderbilt University Medical Center
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: The background for this study is that individuals with a family history of Alzheimer’s disease (i.e., one or more first-degree relatives) have a higher risk for the disease than individuals that don’t have a family history. Previous studies suggested a preferential maternal inheritance of AD, though they were limited in sample size and statistical power.
In our study, we wanted to focus on a larger, cognitively unimpaired sample. Using data from the Anti-Amyloid Treatment in Asymptomatic Alzheimer’s (A4) study, a randomized clinical trial aimed at AD prevention, we examined the relationship between a parental history of significant memory impairment as a proxy for AD (as some individuals may not have pursued formal diagnosis) and amyloid-beta burden in the offspring.
Dr. Seto[/caption]
Mabel Seto, PhD
Harvard Aging Brain Study, Department of Neurology
Massachusetts General Hospital, Center for Alzheimer Research and Treatment
Department of Neurology
Brigham and Women’s Hospital
Harvard Medical School, Boston, Massachusetts
Vanderbilt Memory and Alzheimer’s Center
Vanderbilt University Medical Center
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: The background for this study is that individuals with a family history of Alzheimer’s disease (i.e., one or more first-degree relatives) have a higher risk for the disease than individuals that don’t have a family history. Previous studies suggested a preferential maternal inheritance of AD, though they were limited in sample size and statistical power.
In our study, we wanted to focus on a larger, cognitively unimpaired sample. Using data from the Anti-Amyloid Treatment in Asymptomatic Alzheimer’s (A4) study, a randomized clinical trial aimed at AD prevention, we examined the relationship between a parental history of significant memory impairment as a proxy for AD (as some individuals may not have pursued formal diagnosis) and amyloid-beta burden in the offspring.


 Dr. Traverso[/caption]
Giovanni Traverso MD PhD
Karl Van Tassel (1925) Career Development Professor
Department of Mechanical Engineering
Koch Institute of Integrative Cancer Research
Division of Gastroenterology
Brigham and Women’s Hospital
Harvard Medical School, Boston, MA, USA
MedicalResearch.com: What is the background for this study?
Response: I think its always important to acknowledge that this is a big team effort. We have the teams from MIT, Celero Systems, West Virgnia University (WVU) and Brigham and Women’s Hospital (BWH) all working together on this. For this study, Celero prototyped the devices that we tested in pre-clinical (Swine) models and in a first-in-human study with the team at WVU.
Our lab focuses on the development of ingestible devices for drug delivery and sensing and these have informed the development of these efforts as you can see.
Dr. Traverso[/caption]
Giovanni Traverso MD PhD
Karl Van Tassel (1925) Career Development Professor
Department of Mechanical Engineering
Koch Institute of Integrative Cancer Research
Division of Gastroenterology
Brigham and Women’s Hospital
Harvard Medical School, Boston, MA, USA
MedicalResearch.com: What is the background for this study?
Response: I think its always important to acknowledge that this is a big team effort. We have the teams from MIT, Celero Systems, West Virgnia University (WVU) and Brigham and Women’s Hospital (BWH) all working together on this. For this study, Celero prototyped the devices that we tested in pre-clinical (Swine) models and in a first-in-human study with the team at WVU.
Our lab focuses on the development of ingestible devices for drug delivery and sensing and these have informed the development of these efforts as you can see.

 Dr. Gaba[/caption]
Prakriti Gaba, MD
Cardiovascular Medicine Fellow
Brigham and Women's Hospital
[caption id="attachment_31114" align="alignleft" width="120"]
Dr. Gaba[/caption]
Prakriti Gaba, MD
Cardiovascular Medicine Fellow
Brigham and Women's Hospital
[caption id="attachment_31114" align="alignleft" width="120"] Dr. Deepak Bhatt[/caption]
Deepak L. Bhatt MD MPH
Director of Mount Sinai Fuster Heart Hospital
Dr. Valentin Fuster Professor of Cardiovascular Medicine
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: Accurate classification of acute myocardial infarction is instrumental for the appropriate diagnosis and effective management of patients suffering from this widely prevalent cardiovascular condition.
In the past, there have been a variety of clinical scores published to advise clinicians on the best classifications schemes for patients with acute MI. These have included the Thrombolysis in Myocardial Infarction (TIMI) risk score, the HEART score, and the Killip classification. The strength of these traditional scores includes their practicality, as they can be implemented at the bedside to rapidly assist with prognostication. Nonetheless, as technologic advancements have made imaging and tissue identification more accessible, national and international committees are looking to revise traditional classification schemes of acute MI with novel ones leveraging multimodal approaches.
Dr. Deepak Bhatt[/caption]
Deepak L. Bhatt MD MPH
Director of Mount Sinai Fuster Heart Hospital
Dr. Valentin Fuster Professor of Cardiovascular Medicine
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: Accurate classification of acute myocardial infarction is instrumental for the appropriate diagnosis and effective management of patients suffering from this widely prevalent cardiovascular condition.
In the past, there have been a variety of clinical scores published to advise clinicians on the best classifications schemes for patients with acute MI. These have included the Thrombolysis in Myocardial Infarction (TIMI) risk score, the HEART score, and the Killip classification. The strength of these traditional scores includes their practicality, as they can be implemented at the bedside to rapidly assist with prognostication. Nonetheless, as technologic advancements have made imaging and tissue identification more accessible, national and international committees are looking to revise traditional classification schemes of acute MI with novel ones leveraging multimodal approaches.

 Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
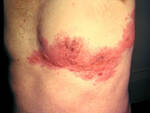
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.


 Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.
Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.
 Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.
Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.




 Dr. LeBoff[/caption]
Meryl S. LeBoff, MD
Dr. LeBoff[/caption]
Meryl S. LeBoff, MD
 Dr. Manson[/caption]
JoAnn E. Manson, MD, DrPH
Professor, Epidemiology, Harvard T.H. Chan School Of Public Health
Michael and Lee Bell Professor of Women's Health, Medicine, Harvard Medical School
Chief, Preventive Medicine, Brigham And Women's Hospital
Co-Director, Womens Health, Brigham And Women's Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Osteoporosis is a major public health problem. Although supplemental vitamin D has been widely used to reduce the risk of fractures in the general population, studies of the effects of vitamin D on fractures, the most important bone health outcome, have been conflicting.
Randomized controlled trials, the highest quality studies, from around the world have shown benefit, no effect, or even harm of supplemental vitamin D on risk of fractures. Some of the trials used bolus dosing, had small samples sizes or short study duration, and co-administered calcium. No large RCTS of this scale tested whether daily supplemental vitamin D (without co-administration with calcium) prevented fractures in the US population.
To fill these knowledge gaps, we tested the hypothesis in this ancillary study to VITAL, whether daily supplemental vitamin D3 reduced the risk of incident total, non-spine and hip fractures in women and men in the US.
Dr. Manson[/caption]
JoAnn E. Manson, MD, DrPH
Professor, Epidemiology, Harvard T.H. Chan School Of Public Health
Michael and Lee Bell Professor of Women's Health, Medicine, Harvard Medical School
Chief, Preventive Medicine, Brigham And Women's Hospital
Co-Director, Womens Health, Brigham And Women's Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Osteoporosis is a major public health problem. Although supplemental vitamin D has been widely used to reduce the risk of fractures in the general population, studies of the effects of vitamin D on fractures, the most important bone health outcome, have been conflicting.
Randomized controlled trials, the highest quality studies, from around the world have shown benefit, no effect, or even harm of supplemental vitamin D on risk of fractures. Some of the trials used bolus dosing, had small samples sizes or short study duration, and co-administered calcium. No large RCTS of this scale tested whether daily supplemental vitamin D (without co-administration with calcium) prevented fractures in the US population.
To fill these knowledge gaps, we tested the hypothesis in this ancillary study to VITAL, whether daily supplemental vitamin D3 reduced the risk of incident total, non-spine and hip fractures in women and men in the US.






 Dr, Ferguson[/caption]
Michael Ferguson, PhD
Instructor in Neurology | Harvard Medical School
Lecturer on Neurospirituality | Harvard Divinity School
Center for Brain Circuit Therapeutics
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
Response: Over 80% of the global population consider themselves religious with even more identifying as spiritual, but the neural substrates of spirituality and religiosity remain unresolved.
MedicalResearch.com: What are the main findings? Where is this circuit located in the brain? What other effects does this circuit control or influence?
Response: We found that brain lesions associated with self-reported spirituality map to a human brain circuit centered on the periaqueductal grey.
Dr, Ferguson[/caption]
Michael Ferguson, PhD
Instructor in Neurology | Harvard Medical School
Lecturer on Neurospirituality | Harvard Divinity School
Center for Brain Circuit Therapeutics
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
Response: Over 80% of the global population consider themselves religious with even more identifying as spiritual, but the neural substrates of spirituality and religiosity remain unresolved.
MedicalResearch.com: What are the main findings? Where is this circuit located in the brain? What other effects does this circuit control or influence?
Response: We found that brain lesions associated with self-reported spirituality map to a human brain circuit centered on the periaqueductal grey.
