Author Interviews, Heart Disease, JACC, Pediatrics, Surgical Research, UCSD / 04.01.2018
Children with Heart Failure from Dilated Cardiomyopathy are Surviving Longer in the Most Recent Era
[caption id="attachment_39174" align="alignleft" width="300"]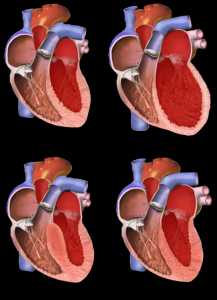 Structural categories of cardiomyopathy Wikipedia image[/caption]
MedicalResearch.com Interview with:
Rakesh K. Singh MD, MS
Department of Pediatrics, University of California–San Diego and
Rady Children’s Hospital
San Diego, California
Steven E. Lipshultz MD
Department of Pediatrics
Wayne State University School of Medicine and
Children’s Hospital of Michigan
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Dilated cardiomyopathy (DCM) is a disease characterized by dilation and dysfunction of the left ventricle of the heart. While DCM is a relatively rare disease in children, nearly 40% of children with DCM require a heart transplant or die within 2 years of diagnosis. Heart transplantation has improved the outcomes of children with DCM over the last 3 decades, but is limited by donor heart availability. Newer therapies, including advanced ICU care and artificial heart machines, are now being used to treat children with DCM.
This study published in the November 28, 2017 issue of the Journal of American College of Cardiology (JACC) sought to determine whether more children with DCM were surviving longer in the more recent era. Specifically, it investigated whether children with DCM were surviving longer without the need for heart transplantation. Rakesh Singh, MD is the first author and an Associate Professor of Pediatrics at UC San Diego/Rady Children’s Hospital, while the senior author is Steven Lipshultz, MD, Professor at Wayne State University School of Medicine/Detroit Medical Center’s Children’s Hospital of Michigan and Director of Children’s Research Center of Michigan.
The Pediatric Cardiomyopathy Registry (PCMR) is a National Heart, Lung, and Blood Institute (NHLBI) sponsored registry from 98 pediatric centers in United States and Canada created to study the outcomes of children with various heart muscle disorders known as cardiomyopathies. For this study, outcomes of 1,199 children diagnosed with DCM from 1990-1999 were compared with 754 children diagnosed with DCM from 2000-2009.
Structural categories of cardiomyopathy Wikipedia image[/caption]
MedicalResearch.com Interview with:
Rakesh K. Singh MD, MS
Department of Pediatrics, University of California–San Diego and
Rady Children’s Hospital
San Diego, California
Steven E. Lipshultz MD
Department of Pediatrics
Wayne State University School of Medicine and
Children’s Hospital of Michigan
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Dilated cardiomyopathy (DCM) is a disease characterized by dilation and dysfunction of the left ventricle of the heart. While DCM is a relatively rare disease in children, nearly 40% of children with DCM require a heart transplant or die within 2 years of diagnosis. Heart transplantation has improved the outcomes of children with DCM over the last 3 decades, but is limited by donor heart availability. Newer therapies, including advanced ICU care and artificial heart machines, are now being used to treat children with DCM.
This study published in the November 28, 2017 issue of the Journal of American College of Cardiology (JACC) sought to determine whether more children with DCM were surviving longer in the more recent era. Specifically, it investigated whether children with DCM were surviving longer without the need for heart transplantation. Rakesh Singh, MD is the first author and an Associate Professor of Pediatrics at UC San Diego/Rady Children’s Hospital, while the senior author is Steven Lipshultz, MD, Professor at Wayne State University School of Medicine/Detroit Medical Center’s Children’s Hospital of Michigan and Director of Children’s Research Center of Michigan.
The Pediatric Cardiomyopathy Registry (PCMR) is a National Heart, Lung, and Blood Institute (NHLBI) sponsored registry from 98 pediatric centers in United States and Canada created to study the outcomes of children with various heart muscle disorders known as cardiomyopathies. For this study, outcomes of 1,199 children diagnosed with DCM from 1990-1999 were compared with 754 children diagnosed with DCM from 2000-2009.
 Structural categories of cardiomyopathy Wikipedia image[/caption]
MedicalResearch.com Interview with:
Rakesh K. Singh MD, MS
Department of Pediatrics, University of California–San Diego and
Rady Children’s Hospital
San Diego, California
Steven E. Lipshultz MD
Department of Pediatrics
Wayne State University School of Medicine and
Children’s Hospital of Michigan
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Dilated cardiomyopathy (DCM) is a disease characterized by dilation and dysfunction of the left ventricle of the heart. While DCM is a relatively rare disease in children, nearly 40% of children with DCM require a heart transplant or die within 2 years of diagnosis. Heart transplantation has improved the outcomes of children with DCM over the last 3 decades, but is limited by donor heart availability. Newer therapies, including advanced ICU care and artificial heart machines, are now being used to treat children with DCM.
This study published in the November 28, 2017 issue of the Journal of American College of Cardiology (JACC) sought to determine whether more children with DCM were surviving longer in the more recent era. Specifically, it investigated whether children with DCM were surviving longer without the need for heart transplantation. Rakesh Singh, MD is the first author and an Associate Professor of Pediatrics at UC San Diego/Rady Children’s Hospital, while the senior author is Steven Lipshultz, MD, Professor at Wayne State University School of Medicine/Detroit Medical Center’s Children’s Hospital of Michigan and Director of Children’s Research Center of Michigan.
The Pediatric Cardiomyopathy Registry (PCMR) is a National Heart, Lung, and Blood Institute (NHLBI) sponsored registry from 98 pediatric centers in United States and Canada created to study the outcomes of children with various heart muscle disorders known as cardiomyopathies. For this study, outcomes of 1,199 children diagnosed with DCM from 1990-1999 were compared with 754 children diagnosed with DCM from 2000-2009.
Structural categories of cardiomyopathy Wikipedia image[/caption]
MedicalResearch.com Interview with:
Rakesh K. Singh MD, MS
Department of Pediatrics, University of California–San Diego and
Rady Children’s Hospital
San Diego, California
Steven E. Lipshultz MD
Department of Pediatrics
Wayne State University School of Medicine and
Children’s Hospital of Michigan
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Dilated cardiomyopathy (DCM) is a disease characterized by dilation and dysfunction of the left ventricle of the heart. While DCM is a relatively rare disease in children, nearly 40% of children with DCM require a heart transplant or die within 2 years of diagnosis. Heart transplantation has improved the outcomes of children with DCM over the last 3 decades, but is limited by donor heart availability. Newer therapies, including advanced ICU care and artificial heart machines, are now being used to treat children with DCM.
This study published in the November 28, 2017 issue of the Journal of American College of Cardiology (JACC) sought to determine whether more children with DCM were surviving longer in the more recent era. Specifically, it investigated whether children with DCM were surviving longer without the need for heart transplantation. Rakesh Singh, MD is the first author and an Associate Professor of Pediatrics at UC San Diego/Rady Children’s Hospital, while the senior author is Steven Lipshultz, MD, Professor at Wayne State University School of Medicine/Detroit Medical Center’s Children’s Hospital of Michigan and Director of Children’s Research Center of Michigan.
The Pediatric Cardiomyopathy Registry (PCMR) is a National Heart, Lung, and Blood Institute (NHLBI) sponsored registry from 98 pediatric centers in United States and Canada created to study the outcomes of children with various heart muscle disorders known as cardiomyopathies. For this study, outcomes of 1,199 children diagnosed with DCM from 1990-1999 were compared with 754 children diagnosed with DCM from 2000-2009.












 Dr. Steven Kyle Grinspoon[/caption]
Steven Grinspoon, MD
Professor of Medicine, Harvard Medical School
MGH Endowed Chair in Neuroendocrinology and Metabolism
Director, MGH Program in Nutritional Metabolism
and Nutrition Obesity Research Center at Harvard
MGH
Boston, MA 02114
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Grinspoon: Numerous epidemiologic studies have shown that people living with HIV face a 1.5 to 2-fold increased risk of heart attack, or myocardial infarction, as compared to individuals without the virus. Mechanisms underlying the increased risk of myocardial infarction in HIV are incompletely understood. It is possible that among people living with HIV, increased systemic immune activation fuels arterial inflammation. Arterial inflammation may, in turn, promote the development of high-risk morphology coronary atherosclerotic plaque, which is liable to rupture and result in myocardial infarction.
For people diagnosed with HIV, the overall health benefits of immediate antiretroviral therapy (ART) are clear. However, the effects of newly-initiated antiretroviral therapy on arterial inflammation have not previously been studied. In this study, we set out to assess among a cohort of treatment-naive HIV-infected subjects, the effects of newly-initiated ART with a contemporary regimen on both immune function and arterial inflammation. We found that among treatment-naive HIV-infected individuals without clinical cardiovascular disease, newly initiated combined antiretroviral therapy has discordant effects to restore immune function without reducing the degree of arterial inflammation.
Dr. Steven Kyle Grinspoon[/caption]
Steven Grinspoon, MD
Professor of Medicine, Harvard Medical School
MGH Endowed Chair in Neuroendocrinology and Metabolism
Director, MGH Program in Nutritional Metabolism
and Nutrition Obesity Research Center at Harvard
MGH
Boston, MA 02114
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Grinspoon: Numerous epidemiologic studies have shown that people living with HIV face a 1.5 to 2-fold increased risk of heart attack, or myocardial infarction, as compared to individuals without the virus. Mechanisms underlying the increased risk of myocardial infarction in HIV are incompletely understood. It is possible that among people living with HIV, increased systemic immune activation fuels arterial inflammation. Arterial inflammation may, in turn, promote the development of high-risk morphology coronary atherosclerotic plaque, which is liable to rupture and result in myocardial infarction.
For people diagnosed with HIV, the overall health benefits of immediate antiretroviral therapy (ART) are clear. However, the effects of newly-initiated antiretroviral therapy on arterial inflammation have not previously been studied. In this study, we set out to assess among a cohort of treatment-naive HIV-infected subjects, the effects of newly-initiated ART with a contemporary regimen on both immune function and arterial inflammation. We found that among treatment-naive HIV-infected individuals without clinical cardiovascular disease, newly initiated combined antiretroviral therapy has discordant effects to restore immune function without reducing the degree of arterial inflammation.

