Author Interviews, Dermatology, Hair Care, JAMA / 11.10.2025
Alopecia Areata: Switching JAK inhibitors May Achieve Hair Regrowth When Others Fail
[caption id="attachment_70946" align="alignleft" width="200"] Dr. King[/caption]
Brett King, MD, PHD
Dr. King was named an American Academy of Dermatology (AAD) “Patient Care Hero”
for his work treating patients with severe alopecia areata
Dermatology Physicians of Connecticut
Fairfield, Connecticut
MedicalResearch.com: What is the background for this study? Would you briefly explain the condition of Alopecia Areata?
Response: Alopecia Areata (AA), an autoimmune form of hair loss, is common and its treatment has been revolutionized in the past ~3 years with approvals of 3 JAK inhibitors, bariticinib, ritlecitinib and deuruxolitinib. Prior to these approvals, off label treatments included the JAK inhibitors tofacitinib and ruxolitinib.
In a world of multiple treatments, especially when those treatments belong to the same medicine class, the question arises “If patients do not achieve treatment success with one medicine, might they achieve treatment success with another one?”
Dr. King[/caption]
Brett King, MD, PHD
Dr. King was named an American Academy of Dermatology (AAD) “Patient Care Hero”
for his work treating patients with severe alopecia areata
Dermatology Physicians of Connecticut
Fairfield, Connecticut
MedicalResearch.com: What is the background for this study? Would you briefly explain the condition of Alopecia Areata?
Response: Alopecia Areata (AA), an autoimmune form of hair loss, is common and its treatment has been revolutionized in the past ~3 years with approvals of 3 JAK inhibitors, bariticinib, ritlecitinib and deuruxolitinib. Prior to these approvals, off label treatments included the JAK inhibitors tofacitinib and ruxolitinib.
In a world of multiple treatments, especially when those treatments belong to the same medicine class, the question arises “If patients do not achieve treatment success with one medicine, might they achieve treatment success with another one?”
 Dr. King[/caption]
Brett King, MD, PHD
Dr. King was named an American Academy of Dermatology (AAD) “Patient Care Hero”
for his work treating patients with severe alopecia areata
Dermatology Physicians of Connecticut
Fairfield, Connecticut
MedicalResearch.com: What is the background for this study? Would you briefly explain the condition of Alopecia Areata?
Response: Alopecia Areata (AA), an autoimmune form of hair loss, is common and its treatment has been revolutionized in the past ~3 years with approvals of 3 JAK inhibitors, bariticinib, ritlecitinib and deuruxolitinib. Prior to these approvals, off label treatments included the JAK inhibitors tofacitinib and ruxolitinib.
In a world of multiple treatments, especially when those treatments belong to the same medicine class, the question arises “If patients do not achieve treatment success with one medicine, might they achieve treatment success with another one?”
Dr. King[/caption]
Brett King, MD, PHD
Dr. King was named an American Academy of Dermatology (AAD) “Patient Care Hero”
for his work treating patients with severe alopecia areata
Dermatology Physicians of Connecticut
Fairfield, Connecticut
MedicalResearch.com: What is the background for this study? Would you briefly explain the condition of Alopecia Areata?
Response: Alopecia Areata (AA), an autoimmune form of hair loss, is common and its treatment has been revolutionized in the past ~3 years with approvals of 3 JAK inhibitors, bariticinib, ritlecitinib and deuruxolitinib. Prior to these approvals, off label treatments included the JAK inhibitors tofacitinib and ruxolitinib.
In a world of multiple treatments, especially when those treatments belong to the same medicine class, the question arises “If patients do not achieve treatment success with one medicine, might they achieve treatment success with another one?”




 Dr. Ferris[/caption]
Laura Ferris, M.D., Ph.D.
Professor of Dermatology
Director of clinical trials for UPMC Department of Dermatology
University of Pittsburgh School of Medicine
MedicalResearch.com: What is the background for this study?
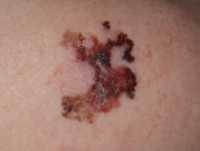
Response: In this quality initiative at UPMC (a large academic and community health system in Western PA and surrounding areas) Primary Care Physicians were trained to perform annual skin cancer screening examinations of their patients who were aged 35 years and older at routine medical visits.
Over a 5-year period more than 595,000 patients who were eligible to be screened were seen by a UPMC PCP and about 24% of them were screened. We compared the number and thickness (an important indicator of prognosis) of the melanomas diagnosed in those patients who were screened to those who were not screened.
Dr. Ferris[/caption]
Laura Ferris, M.D., Ph.D.
Professor of Dermatology
Director of clinical trials for UPMC Department of Dermatology
University of Pittsburgh School of Medicine
MedicalResearch.com: What is the background for this study?
Response: In this quality initiative at UPMC (a large academic and community health system in Western PA and surrounding areas) Primary Care Physicians were trained to perform annual skin cancer screening examinations of their patients who were aged 35 years and older at routine medical visits.
Over a 5-year period more than 595,000 patients who were eligible to be screened were seen by a UPMC PCP and about 24% of them were screened. We compared the number and thickness (an important indicator of prognosis) of the melanomas diagnosed in those patients who were screened to those who were not screened.


 Dr. Albrecht[/caption]
Joerg Albrecht, MD, PhD
Dermatologist, Internist, Clinical Pharmacologist
Division of Dermatology, Department of Medicine
Attending Dermatologist, Chair Division of Dermatology
Chair system-wide Pharmacy & Therapeutics Committee
Cook County Health
Chicago, IL 60612
MedicalResearch.com: What is the background for this study?
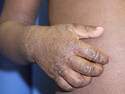
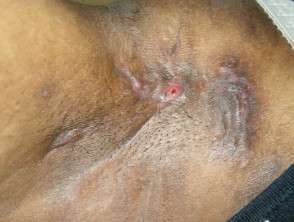
Response: The study was stimulated by data that suggested that an unusually large proportion of inpatient with Hidradenitis suppurativa (HS) were African American. HS is an underdiagnosed disease and the total numbers of inpatients with HS in the year we looked at initially seemed small. So we wanted to test whether this finding held up when the period of observation was extended. Point estimates can be unreliable and we had followed another finding in the data that did not hold up when we looked at other years, so we felt one year was not enough to confirm a trend
Dr. Albrecht[/caption]
Joerg Albrecht, MD, PhD
Dermatologist, Internist, Clinical Pharmacologist
Division of Dermatology, Department of Medicine
Attending Dermatologist, Chair Division of Dermatology
Chair system-wide Pharmacy & Therapeutics Committee
Cook County Health
Chicago, IL 60612
MedicalResearch.com: What is the background for this study?
Response: The study was stimulated by data that suggested that an unusually large proportion of inpatient with Hidradenitis suppurativa (HS) were African American. HS is an underdiagnosed disease and the total numbers of inpatients with HS in the year we looked at initially seemed small. So we wanted to test whether this finding held up when the period of observation was extended. Point estimates can be unreliable and we had followed another finding in the data that did not hold up when we looked at other years, so we felt one year was not enough to confirm a trend

 Dr. Andersson[/caption]
Niklas Worm Andersson, MD
Department of Epidemiology Research
Statens Serum Institut,
Copenhagen Denmark
MedicalResearch.com: What is the background for this study?
Response: "Findings from some previous fetal safety studies on topical corticosteroid use in pregnancy have raised concerns for an increased risk of newborns being small for gestational age or having low birth weight, in particular among pregnancies where larger amounts of potent to very potent agents have been used."
Dr. Andersson[/caption]
Niklas Worm Andersson, MD
Department of Epidemiology Research
Statens Serum Institut,
Copenhagen Denmark
MedicalResearch.com: What is the background for this study?
Response: "Findings from some previous fetal safety studies on topical corticosteroid use in pregnancy have raised concerns for an increased risk of newborns being small for gestational age or having low birth weight, in particular among pregnancies where larger amounts of potent to very potent agents have been used."




 MedicalResearch.com: What is the background for this study?
Response: A prior pilot
MedicalResearch.com: What is the background for this study?
Response: A prior pilot 


 Dr. Helen Marsden PhD
Skin Analytics Limited
London, United Kingdom
MedicalResearch.com: What is the background for this study?
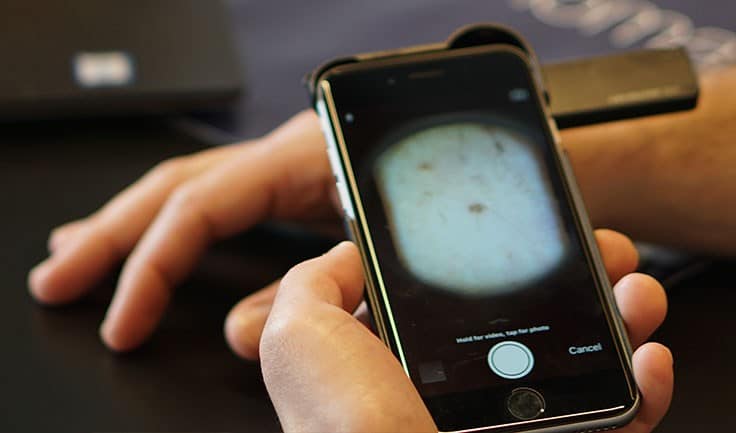
Response: In this technology age, with the explosion of interest and applications using Artificial Intelligence, it is easy to accept the output of a technology-based test - such as a smartphone app designed to identify skin cancer - without thinking too much about it. In reality, technology is only as good as the way it has been developed, tested and validated. In particular, AI algorithms are prone to a lack of “generalisation” - i.e. their performance drops when presented with data it has not seen before. In the medical field, and particularly in areas where AI is being developed to direct a patient’s diagnosis or care, this is particularly problematic. Inappropriate diagnosis or advice to patients can lead to false reassurance, heightened concern and pressure on NHS services, or worse. It is concerning, therefore, that there are a large number of smartphone apps available that provide an assessment of skin lesions, including some that provide an estimate of the probability of malignancy, that have not been assessed for diagnostic accuracy.
Skin Analytics has developed an AI-based algorithm, named: Deep Ensemble for Recognition of Malignancy (DERM), for use as a decision support tool for healthcare providers. DERM determines the likelihood of skin cancer from dermoscopic images of skin lesions. It was developed using deep learning techniques that identify and assess features of these lesions which are associated with melanoma, using over 7,000 archived dermoscopic images. Using these images, it was shown to identify melanoma with similar accuracy to specialist physicians. However, to prove the algorithm could be used in a real life clinical setting, Skin Analytics set out to conduct a clinical validation study.
Dr. Helen Marsden PhD
Skin Analytics Limited
London, United Kingdom
MedicalResearch.com: What is the background for this study?
Response: In this technology age, with the explosion of interest and applications using Artificial Intelligence, it is easy to accept the output of a technology-based test - such as a smartphone app designed to identify skin cancer - without thinking too much about it. In reality, technology is only as good as the way it has been developed, tested and validated. In particular, AI algorithms are prone to a lack of “generalisation” - i.e. their performance drops when presented with data it has not seen before. In the medical field, and particularly in areas where AI is being developed to direct a patient’s diagnosis or care, this is particularly problematic. Inappropriate diagnosis or advice to patients can lead to false reassurance, heightened concern and pressure on NHS services, or worse. It is concerning, therefore, that there are a large number of smartphone apps available that provide an assessment of skin lesions, including some that provide an estimate of the probability of malignancy, that have not been assessed for diagnostic accuracy.
Skin Analytics has developed an AI-based algorithm, named: Deep Ensemble for Recognition of Malignancy (DERM), for use as a decision support tool for healthcare providers. DERM determines the likelihood of skin cancer from dermoscopic images of skin lesions. It was developed using deep learning techniques that identify and assess features of these lesions which are associated with melanoma, using over 7,000 archived dermoscopic images. Using these images, it was shown to identify melanoma with similar accuracy to specialist physicians. However, to prove the algorithm could be used in a real life clinical setting, Skin Analytics set out to conduct a clinical validation study.


 Dr. Vallerand[/caption]
Isabelle Vallerand, PhD
Epidemiologist, MD Student
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study? What are the main findings?
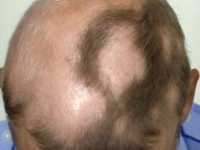
Response: It is well known that patients with alopecia areata, a form of autoimmune hair loss, are at a higher risk of suffering from depression than the general population. But in practice, we often hear patients tell us that they believe their hair loss developed as a result of stress or problems with mental health – certainly the phrase “so stressed your hair is falling out” is something most people have heard of. Despite this, there has actually been very little research investigating the role that mental health may have on development of alopecia areata.
Interestingly, depression has recently been associated with increased systemic inflammatory markers, so there is biologic plausibility that depression could increase the risk of alopecia areata. Our group was interested in addressing this question, and used a large population-level health records database with up to 26 years of follow-up to study it. We ultimately found that not only does depression increase one’s risk of alopecia areata, but that it increases their risk by nearly 90% compared to people who have never had depression. We also found that using antidepressants can significantly decrease the risk of developing alopecia areata in patients with depression. So there appears to be an important link between mental health and development of hair loss from alopecia areata.
Dr. Vallerand[/caption]
Isabelle Vallerand, PhD
Epidemiologist, MD Student
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: It is well known that patients with alopecia areata, a form of autoimmune hair loss, are at a higher risk of suffering from depression than the general population. But in practice, we often hear patients tell us that they believe their hair loss developed as a result of stress or problems with mental health – certainly the phrase “so stressed your hair is falling out” is something most people have heard of. Despite this, there has actually been very little research investigating the role that mental health may have on development of alopecia areata.
Interestingly, depression has recently been associated with increased systemic inflammatory markers, so there is biologic plausibility that depression could increase the risk of alopecia areata. Our group was interested in addressing this question, and used a large population-level health records database with up to 26 years of follow-up to study it. We ultimately found that not only does depression increase one’s risk of alopecia areata, but that it increases their risk by nearly 90% compared to people who have never had depression. We also found that using antidepressants can significantly decrease the risk of developing alopecia areata in patients with depression. So there appears to be an important link between mental health and development of hair loss from alopecia areata.
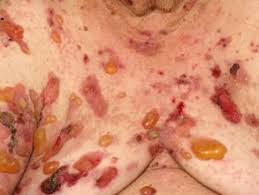

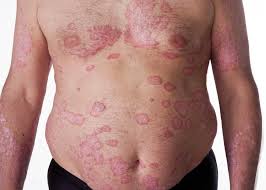 Psoriasis[/caption]
Prof Ching-Chi Chi, MD, MMS, DPhil
Department of Dermatology
Chang Gung Memorial Hospital, Linkou
Guishan Dist, Taoyuan
MedicalResearch.com: What is the background for this study? What are the main findings?
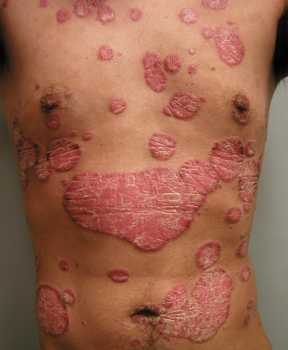
Response: Previous studies have shown common genotypes, clinical course, and immunological features shared by psoriasis and inflammatory bowel disease.
However, the relationship between psoriasis and inflammatory bowel disease was largely unclear.
In this study, we found when compared to the general population, psoriatic patients are more likely to have concomitant inflammatory bowel disease.
Psoriasis[/caption]
Prof Ching-Chi Chi, MD, MMS, DPhil
Department of Dermatology
Chang Gung Memorial Hospital, Linkou
Guishan Dist, Taoyuan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Previous studies have shown common genotypes, clinical course, and immunological features shared by psoriasis and inflammatory bowel disease.
However, the relationship between psoriasis and inflammatory bowel disease was largely unclear.
In this study, we found when compared to the general population, psoriatic patients are more likely to have concomitant inflammatory bowel disease. 