The healthcare sector is rapidly evolving with the integration of telehealth technologies. Remote patient monitoring (RPM) is increasingly pivotal in managing chronic conditions, offering real-time insights into patient health. Virtual medical assistants are playing a crucial role in reducing administrative tasks and enhancing care delivery.
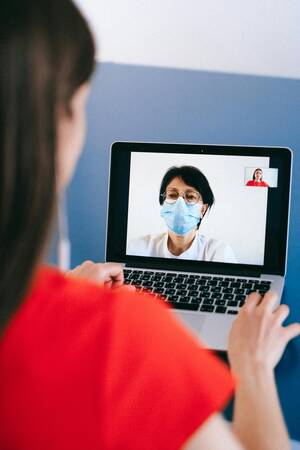
[caption id="attachment_66474" align="aligncenter" width="500"]

Young adult calling doctor on videocall telehealth, talking about healthcare treatment on videoconference and telemedicine. Meeting on remote teleconference call with physician, online appointment.[/caption]
The expansion of telehealth has transformed how patients interact with healthcare providers, particularly in managing chronic diseases. By leveraging RPM, healthcare professionals can monitor patients' health metrics remotely, ensuring timely interventions and improving patient outcomes. The integration of virtual medical assistants, such as those offered by
www.honesttaskers.com, provides a streamlined approach to managing administrative tasks, allowing providers to focus more on patient care.
Key benefits of telehealth and RPM for chronic conditions
One significant advantage of telehealth is the increased accessibility it provides to patients with chronic conditions. This technology reduces the need for frequent in-person visits, saving travel time and costs for patients. With remote monitoring devices, patients can have their vital signs tracked continuously, leading to better adherence to treatment plans and enhanced overall management of their conditions.
The continuous flow of health data from RPM devices enables healthcare teams to detect deviations in patients' health metrics early. Such real-time tracking allows for prompt interventions, potentially preventing complications and hospitalizations. Moreover, this proactive approach facilitates better communication between patients and healthcare providers, fostering a more engaged and informed patient population.
Additionally, telehealth has demonstrated cost-effectiveness for healthcare providers who effectively utilize these platforms. By reducing the need for physical infrastructure and enabling efficient resource allocation, telehealth services help minimize operational costs while maintaining high-quality care delivery. This financial benefit further encourages the adoption of telehealth technologies across various healthcare settings.
 Getting medical help used to take planning, time, and patience. Now things are shifting. With online prescriptions, people can connect with doctors much faster and handle simple health concerns from home. If you want to learn more about how this works, it helps to look at how daily habits are changing. People expect speed and convenience in everything, and healthcare is starting to follow that pattern. This matters because when care is easier to access, people are more likely to act early instead of waiting until problems get worse.
Getting medical help used to take planning, time, and patience. Now things are shifting. With online prescriptions, people can connect with doctors much faster and handle simple health concerns from home. If you want to learn more about how this works, it helps to look at how daily habits are changing. People expect speed and convenience in everything, and healthcare is starting to follow that pattern. This matters because when care is easier to access, people are more likely to act early instead of waiting until problems get worse.
 Getting medical help used to take planning, time, and patience. Now things are shifting. With online prescriptions, people can connect with doctors much faster and handle simple health concerns from home. If you want to learn more about how this works, it helps to look at how daily habits are changing. People expect speed and convenience in everything, and healthcare is starting to follow that pattern. This matters because when care is easier to access, people are more likely to act early instead of waiting until problems get worse.
Getting medical help used to take planning, time, and patience. Now things are shifting. With online prescriptions, people can connect with doctors much faster and handle simple health concerns from home. If you want to learn more about how this works, it helps to look at how daily habits are changing. People expect speed and convenience in everything, and healthcare is starting to follow that pattern. This matters because when care is easier to access, people are more likely to act early instead of waiting until problems get worse.












 Dr. Avinesh Bhar[/caption]
Dr. Avinesh Bhar[/caption]


 Dr. Love you to the moon and back![/caption]
Susan Lu PhD
Gerald Lyles Rising Star Associate Professor of Management
Krannert School of Management
Purdue University
MedicalResearch.com: What is the background for this study?
Response: We started this project in 2016. Overcrowding in emergency rooms (ERs) is a common yet nagging problem. It not only is costly for hospitals but also compromises care quality and patient experience. Hence, finding effective ways to improve ER care delivery is of great importance. Meanwhile, the advancement of healthcare technologies including electronic medical records, online doctor ratings and 4G mobile network motivates us to think about the impact of telemedicine on ER operations in the near future.
Dr. Love you to the moon and back![/caption]
Susan Lu PhD
Gerald Lyles Rising Star Associate Professor of Management
Krannert School of Management
Purdue University
MedicalResearch.com: What is the background for this study?
Response: We started this project in 2016. Overcrowding in emergency rooms (ERs) is a common yet nagging problem. It not only is costly for hospitals but also compromises care quality and patient experience. Hence, finding effective ways to improve ER care delivery is of great importance. Meanwhile, the advancement of healthcare technologies including electronic medical records, online doctor ratings and 4G mobile network motivates us to think about the impact of telemedicine on ER operations in the near future. 





 Dr. Mima Becevic[/caption]
Mirna Becevic, PhD, MHA
Assistant Research Professor
University of Missouri - Department of Dermatology
Missouri Telehealth Network
MedicalResearch.com: What is the background for this study?
Response: Psychiatry is, by far, the biggest utilizer of telemedicine services on the Missouri Telehealth Network (MTN). MTN supports an average of 4000 tele-psychiatry appointments every month, and 10% of those are provided by the University of Missouri Department of Psychiatry. Since we are all aware of the ever-increasing demand for child and adolescent psychiatry, but also the stigma that goes along with it, we wanted to examine more closely the actual usage of those services at the University of Missouri.
Dr. Mima Becevic[/caption]
Mirna Becevic, PhD, MHA
Assistant Research Professor
University of Missouri - Department of Dermatology
Missouri Telehealth Network
MedicalResearch.com: What is the background for this study?
Response: Psychiatry is, by far, the biggest utilizer of telemedicine services on the Missouri Telehealth Network (MTN). MTN supports an average of 4000 tele-psychiatry appointments every month, and 10% of those are provided by the University of Missouri Department of Psychiatry. Since we are all aware of the ever-increasing demand for child and adolescent psychiatry, but also the stigma that goes along with it, we wanted to examine more closely the actual usage of those services at the University of Missouri.
 Dr. Susan McCurry[/caption]
Dr. Susan McCurry
Principal Investigator
Clinical psychologist and research professor
School of Nursing
University of Washington
MedicalResearch.com: What is the background for this study?
Dr. McCurry: Every woman goes through menopause. Most women experience nighttime hot flashes/sweats and problems sleeping at some point during the menopause transition. Poor sleep leads to daytime fatigue, negative mood, and reduced daytime productivity. When sleep problems become chronic – as they often do – there are also a host of negative physical consequences including increased risk for weight gain, diabetes, and cardiovascular disease. Many women do not want to use sleeping medications or hormonal therapies to treat their sleep problems because of concerns about side effect risks. For these reasons, having effective non-pharmacological options to offer them is important.
Dr. Susan McCurry[/caption]
Dr. Susan McCurry
Principal Investigator
Clinical psychologist and research professor
School of Nursing
University of Washington
MedicalResearch.com: What is the background for this study?
Dr. McCurry: Every woman goes through menopause. Most women experience nighttime hot flashes/sweats and problems sleeping at some point during the menopause transition. Poor sleep leads to daytime fatigue, negative mood, and reduced daytime productivity. When sleep problems become chronic – as they often do – there are also a host of negative physical consequences including increased risk for weight gain, diabetes, and cardiovascular disease. Many women do not want to use sleeping medications or hormonal therapies to treat their sleep problems because of concerns about side effect risks. For these reasons, having effective non-pharmacological options to offer them is important. Dr. Jack Resneck[/caption]
Jack Resneck, Jr, MD
Professor and Vice-Chair of Dermatology
Core Faculty, Philip R. Lee Institute for Health Policy Studies
UCSF School of Medicine
MedicalResearch.com: What is the background for this study?
What are the main findings?
Dr. Resneck: Telemedicine, when done right, can improve access and offer convenience to patients. We have seen proven high-quality care in telemedicine services where patients are using digital platforms to communicate with their existing doctors who know them, and where doctors are getting teleconsultations from other specialists about their patients. But our study shows major quality problems with the rapidly growing corporate direct-to-consumer services where patients send consults via the web or phone apps to clinicians they don’t know.
Most of these sites aren’t giving patients a choice of the clinician who will care for them or disclosing the credentials of those clinicians – patients should know whether their rash is being cared for by a board-certified dermatologist, a pain management specialist, or a nurse practitioner who usually works in an emergency department. Some of these sites are even using doctors who aren’t licensed in the US. We also found that these sites were regularly missing important diagnoses, and prescribing medications without discussing risks and side-effects, putting patients at risk. We observed that if you upload photos of a highly contagious syphilis rash but state that you think you have psoriasis, most clinicians working for these direct-to-consumer sites will just agree with your self-diagnosis and prescribe psoriasis medications, leaving you with a contagious STD.
Perhaps the biggest problem with many of these sites is the lack of coordinating care for patients – most of them didn’t offer to send records to a patient’s existing local doctors. And when patients end up needing in-person care if their condition worsens, or they have a medication side-effect, those distant clinicians often don’t have local contacts, and are unable to facilitate needed appointments.
Dr. Jack Resneck[/caption]
Jack Resneck, Jr, MD
Professor and Vice-Chair of Dermatology
Core Faculty, Philip R. Lee Institute for Health Policy Studies
UCSF School of Medicine
MedicalResearch.com: What is the background for this study?
What are the main findings?
Dr. Resneck: Telemedicine, when done right, can improve access and offer convenience to patients. We have seen proven high-quality care in telemedicine services where patients are using digital platforms to communicate with their existing doctors who know them, and where doctors are getting teleconsultations from other specialists about their patients. But our study shows major quality problems with the rapidly growing corporate direct-to-consumer services where patients send consults via the web or phone apps to clinicians they don’t know.
Most of these sites aren’t giving patients a choice of the clinician who will care for them or disclosing the credentials of those clinicians – patients should know whether their rash is being cared for by a board-certified dermatologist, a pain management specialist, or a nurse practitioner who usually works in an emergency department. Some of these sites are even using doctors who aren’t licensed in the US. We also found that these sites were regularly missing important diagnoses, and prescribing medications without discussing risks and side-effects, putting patients at risk. We observed that if you upload photos of a highly contagious syphilis rash but state that you think you have psoriasis, most clinicians working for these direct-to-consumer sites will just agree with your self-diagnosis and prescribe psoriasis medications, leaving you with a contagious STD.
Perhaps the biggest problem with many of these sites is the lack of coordinating care for patients – most of them didn’t offer to send records to a patient’s existing local doctors. And when patients end up needing in-person care if their condition worsens, or they have a medication side-effect, those distant clinicians often don’t have local contacts, and are unable to facilitate needed appointments.
 Dr. Uscher-Pines[/caption]
Lori Uscher-Pines, PhD
RAND Corporation
Arlington, Virginia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Although many communities in the U.S. are underserved by dermatologists, access is particularly limited among Medicaid patients. Teledermatology may be one solution to improve access. Our goal with this study was to assess the effect of a novel teledermatology initiative on access to dermatologists among enrollees in a Medicaid Managed Care Plan in California’s Central Valley.
Among all patients who visited a dermatologist after the introduction of teledermatology from 2012-2014 (n=8614), 49% received care via teledermatology. Among patients newly enrolled in Medicaid following Medicaid expansion in 2014, 76% of those who visited a dermatologist received care via teledermatology. Patients of primary care practices that engaged in teledermatology had a 64% increase in the fraction of patients visiting a dermatologist (vs. 21% in other practices) (p<.01). Compared with in-person dermatology, teledermatology served more patients under age 17, male patients, nonwhite patients, and patients without comorbid conditions. Conditions managed across settings varied; teledermatology physicians were more likely to care for viral skin lesions and acne whereas in-person dermatologists were more likely to care for psoriasis and skin neoplasms.
Dr. Uscher-Pines[/caption]
Lori Uscher-Pines, PhD
RAND Corporation
Arlington, Virginia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Although many communities in the U.S. are underserved by dermatologists, access is particularly limited among Medicaid patients. Teledermatology may be one solution to improve access. Our goal with this study was to assess the effect of a novel teledermatology initiative on access to dermatologists among enrollees in a Medicaid Managed Care Plan in California’s Central Valley.
Among all patients who visited a dermatologist after the introduction of teledermatology from 2012-2014 (n=8614), 49% received care via teledermatology. Among patients newly enrolled in Medicaid following Medicaid expansion in 2014, 76% of those who visited a dermatologist received care via teledermatology. Patients of primary care practices that engaged in teledermatology had a 64% increase in the fraction of patients visiting a dermatologist (vs. 21% in other practices) (p<.01). Compared with in-person dermatology, teledermatology served more patients under age 17, male patients, nonwhite patients, and patients without comorbid conditions. Conditions managed across settings varied; teledermatology physicians were more likely to care for viral skin lesions and acne whereas in-person dermatologists were more likely to care for psoriasis and skin neoplasms.
 Dr. Becevic[/caption]
MedicalResearch.com Interview with:
Mirna Becevic, PhD, MHA
Assistant Research Professor of Telemedicine
University of Missouri - Department of Dermatology
Missouri Telehealth Network
Medical Research: What is the background for this study? What are the main findings?
Dr. Becevic: The Missouri Telehealth Network (MTN) at the University of Missouri has been providing outpatient clinical services to rural Missourians since 1995. Over 29 specialties and subspecialties have been utilized to assist patients in 69 counties. We have learned a lot along the way, what works well and what does not, in terms of telehealth protocols, trainings, best practices, etc.
The MTN holds bi-annual two day training conference for new sites to share these experiences and provide hands-on training in telemedicine. Our main goal with this study was to reach all telehealth users on the Missouri Telehealth Network (patients, providers, and telehealth coordinators-patient presenters) and learn about their perceptions of and opinions regarding this form of health care delivery. We also wanted to evaluate the overall accessibility and discernment of the MTN by telehealth coordinators, since we felt that they might need to have continuous support in order to successfully manage their telehealth programs.
Our main findings indicated that all three surveyed groups had high satisfaction with telemedicine. Patients were confident in their doctors’ medical skills, and lack of physical contact was not viewed as a barrier. Telehealth providers thought telehealth was an effective tool for providing care at a distance, but indicated that they did not prefer telehealth over in-person visits.
Dr. Becevic[/caption]
MedicalResearch.com Interview with:
Mirna Becevic, PhD, MHA
Assistant Research Professor of Telemedicine
University of Missouri - Department of Dermatology
Missouri Telehealth Network
Medical Research: What is the background for this study? What are the main findings?
Dr. Becevic: The Missouri Telehealth Network (MTN) at the University of Missouri has been providing outpatient clinical services to rural Missourians since 1995. Over 29 specialties and subspecialties have been utilized to assist patients in 69 counties. We have learned a lot along the way, what works well and what does not, in terms of telehealth protocols, trainings, best practices, etc.
The MTN holds bi-annual two day training conference for new sites to share these experiences and provide hands-on training in telemedicine. Our main goal with this study was to reach all telehealth users on the Missouri Telehealth Network (patients, providers, and telehealth coordinators-patient presenters) and learn about their perceptions of and opinions regarding this form of health care delivery. We also wanted to evaluate the overall accessibility and discernment of the MTN by telehealth coordinators, since we felt that they might need to have continuous support in order to successfully manage their telehealth programs.
Our main findings indicated that all three surveyed groups had high satisfaction with telemedicine. Patients were confident in their doctors’ medical skills, and lack of physical contact was not viewed as a barrier. Telehealth providers thought telehealth was an effective tool for providing care at a distance, but indicated that they did not prefer telehealth over in-person visits.

