Author Interviews, Mental Health Research, Psychological Science / 01.12.2020
Mental and Physical Health Suffer In Recently Divorced
MedicalResearch.com Interview with:
Gert Martin Hald, PhD
Head of Section (Environmental Health), Associate Professor
Department of Public Health, University of Copenhagen
Copenhagen, Denmark
MedicalResearch.com: What is the background for this study?
Response: Basically, much of previous research has investigated mental and physical health of divorcees only after extensive separation periods, which is mandatory in most countries before juridical divorce unless infidelity or violence is involved in the divorce. During the time of data collection (2016-2019), Denmark where data was collected did not require separation periods before granting divorce. This means that as a first, we could investigate the mental and physical health of divorcees within days of them filling for divorce and perhaps better and more accurately pick up well-known adverse effects of mental- and physical health states of divorcees at the time of their divorce.



 Dr. Etkin[/caption]
Amit Etkin, MD, PhD
Department of Psychiatry and Behavioral Sciences
Wu Tsai Neurosciences Institute, Stanford Universitu
Stanford, CA
MedicalResearch.com: What is the mission of Cohen Veterans Bioscience - CVB?
Dr. Etkin[/caption]
Amit Etkin, MD, PhD
Department of Psychiatry and Behavioral Sciences
Wu Tsai Neurosciences Institute, Stanford Universitu
Stanford, CA
MedicalResearch.com: What is the mission of Cohen Veterans Bioscience - CVB?
 Response: Cohen Veterans Bioscience (CVB) is a non-profit 501(c)(3) research biotech dedicated to fast-tracking the development of diagnostic tests and personalized therapeutics for the millions of Veterans and civilians who suffer the devastating effects of trauma-related and other brain disorders.
MedicalResearch.com: How can patients with PTSD or MDD benefit from this information?
Response: With the discovery of this new brain imaging biomarker, patients who suffer from PTSD or MDD may be guided towards the most effective treatment without waiting months and months to find a treatment that may work for them.
MedicalResearch.com: What is the background for this study?
Response: This study, which was supported with a grant from Cohen Veterans Bioscience, grants from the National Institute of Mental Health (NIMH and other supporters, derives from our work over the past few years which has pointed to the critical importance of understanding how patients with a variety of psychiatric disorders differ biologically. The shortcomings of our current diagnostic system have become very clear over the past 1-2 decades, but the availability of tools for transcending these limitations on the back of objective biological tests has not kept pace with the need for those tools.
In prior work, we have used a variety of methods, including different types of brain imaging, to identify brain signals that underpin key biological differences within and across traditional psychiatric diagnoses. We have also developed specialized AI tools for decoding complex patterns of brain activity in order to understand and quantify biological heterogeneity in individual patients. These developments have then, in turn, converged with the completion of a number of large brain imaging-coupled clinical trials, which have provided a scale of these types of data not previously available in the field.
Response: Cohen Veterans Bioscience (CVB) is a non-profit 501(c)(3) research biotech dedicated to fast-tracking the development of diagnostic tests and personalized therapeutics for the millions of Veterans and civilians who suffer the devastating effects of trauma-related and other brain disorders.
MedicalResearch.com: How can patients with PTSD or MDD benefit from this information?
Response: With the discovery of this new brain imaging biomarker, patients who suffer from PTSD or MDD may be guided towards the most effective treatment without waiting months and months to find a treatment that may work for them.
MedicalResearch.com: What is the background for this study?
Response: This study, which was supported with a grant from Cohen Veterans Bioscience, grants from the National Institute of Mental Health (NIMH and other supporters, derives from our work over the past few years which has pointed to the critical importance of understanding how patients with a variety of psychiatric disorders differ biologically. The shortcomings of our current diagnostic system have become very clear over the past 1-2 decades, but the availability of tools for transcending these limitations on the back of objective biological tests has not kept pace with the need for those tools.
In prior work, we have used a variety of methods, including different types of brain imaging, to identify brain signals that underpin key biological differences within and across traditional psychiatric diagnoses. We have also developed specialized AI tools for decoding complex patterns of brain activity in order to understand and quantify biological heterogeneity in individual patients. These developments have then, in turn, converged with the completion of a number of large brain imaging-coupled clinical trials, which have provided a scale of these types of data not previously available in the field.










 Dr. Kendall[/caption]
Dr Kimberley Kendall MBBCh
Wellcome Trust Clinical Research Fellow
[caption id="attachment_48630" align="alignleft" width="150"]
Dr. Kendall[/caption]
Dr Kimberley Kendall MBBCh
Wellcome Trust Clinical Research Fellow
[caption id="attachment_48630" align="alignleft" width="150"]





 Dr. Vallerand[/caption]
Isabelle Vallerand, PhD
Epidemiologist, MD Student
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study? What are the main findings?
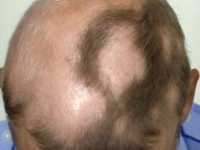
Response: It is well known that patients with alopecia areata, a form of autoimmune hair loss, are at a higher risk of suffering from depression than the general population. But in practice, we often hear patients tell us that they believe their hair loss developed as a result of stress or problems with mental health – certainly the phrase “so stressed your hair is falling out” is something most people have heard of. Despite this, there has actually been very little research investigating the role that mental health may have on development of alopecia areata.
Interestingly, depression has recently been associated with increased systemic inflammatory markers, so there is biologic plausibility that depression could increase the risk of alopecia areata. Our group was interested in addressing this question, and used a large population-level health records database with up to 26 years of follow-up to study it. We ultimately found that not only does depression increase one’s risk of alopecia areata, but that it increases their risk by nearly 90% compared to people who have never had depression. We also found that using antidepressants can significantly decrease the risk of developing alopecia areata in patients with depression. So there appears to be an important link between mental health and development of hair loss from alopecia areata.
Dr. Vallerand[/caption]
Isabelle Vallerand, PhD
Epidemiologist, MD Student
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: It is well known that patients with alopecia areata, a form of autoimmune hair loss, are at a higher risk of suffering from depression than the general population. But in practice, we often hear patients tell us that they believe their hair loss developed as a result of stress or problems with mental health – certainly the phrase “so stressed your hair is falling out” is something most people have heard of. Despite this, there has actually been very little research investigating the role that mental health may have on development of alopecia areata.
Interestingly, depression has recently been associated with increased systemic inflammatory markers, so there is biologic plausibility that depression could increase the risk of alopecia areata. Our group was interested in addressing this question, and used a large population-level health records database with up to 26 years of follow-up to study it. We ultimately found that not only does depression increase one’s risk of alopecia areata, but that it increases their risk by nearly 90% compared to people who have never had depression. We also found that using antidepressants can significantly decrease the risk of developing alopecia areata in patients with depression. So there appears to be an important link between mental health and development of hair loss from alopecia areata.







 Dr Sarah Myers PhD
Honorary Research Associate
UCL Department of Anthropology
MedicalResearch.com: What is the background for this study?
Response: Postnatal or postpartum depression is unfortunately common after giving birth; a figure often quoted is 15%, but some studies have found much higher numbers. Postnatal depression is associated with a range of poorer outcomes for mothers and their infants, and the financial costs of treating maternal mental ill health put health services under considerable strain. Studies have found that providing additional emotional support to at risk mothers, for instance via peer support programmes or regular phone calls with health visitors, can reduce the likelihood of them developing the condition. Therefore, it is really important that we understand the full range of risk factors that put women at greater risk of becoming depressed after giving birth.
There is increasing evidence for a link between inflammation and depression, with factors that trigger an inflammatory immune response also increasing the likelihood of depressive symptoms. The opens up the possibility of finding new risk factors for postnatal depression based on known associations with inflammation.
Dr Sarah Myers PhD
Honorary Research Associate
UCL Department of Anthropology
MedicalResearch.com: What is the background for this study?
Response: Postnatal or postpartum depression is unfortunately common after giving birth; a figure often quoted is 15%, but some studies have found much higher numbers. Postnatal depression is associated with a range of poorer outcomes for mothers and their infants, and the financial costs of treating maternal mental ill health put health services under considerable strain. Studies have found that providing additional emotional support to at risk mothers, for instance via peer support programmes or regular phone calls with health visitors, can reduce the likelihood of them developing the condition. Therefore, it is really important that we understand the full range of risk factors that put women at greater risk of becoming depressed after giving birth.
There is increasing evidence for a link between inflammation and depression, with factors that trigger an inflammatory immune response also increasing the likelihood of depressive symptoms. The opens up the possibility of finding new risk factors for postnatal depression based on known associations with inflammation.