Author Interviews, Dermatology, Immunotherapy / 29.03.2017
Safer Immunotherapy Dupilumab (Dupixent) FDA Approved For Atopic Dermatitis
MedicalResearch.com Interview with:
[caption id="attachment_33490" align="alignleft" width="130"] Dr. Guttman[/caption]
Emma Guttman, MD, PhD
Professor, Dermatology, Medicine and Clinical Immunology
Vice Chair of Research in the Dermatology Department
Director of the center for Excellence
Eczema in the Occupational/Contact Dermatitis clinic
Director of the Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai Medical Center
New York
MedicalResearch.com: Would you briefly explain what is meant by atopic dermatitis? How many people are affected by this disorder?
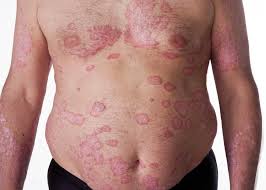
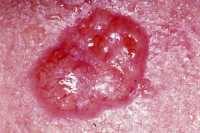
Response: Atopic dermatitis or eczema as most people know it is an itchy red scaly skin disorder characterized by a very severe itch, that disrupts daily activities, and sleep and severely impairs the quality of life of patients. In the US 30 million people are affected by it, and 1/3 of these we expect to be moderate to severe.
MedicalResearch.com: What is the background for Dupilumab therapy? How does it differ from emollients, steroids or topical immunomodulator treatments for eczema ie Protopic?
Response: The background is that we currently do not have good treatments for long term use for our moderate to severe patients. The only approved drug by the FDA for atopic dermatitis in the US is oral prednisone, that has many long term side effects and causes disease rebound upon discontinuation. Other treatments with many side effects
are broad immune suppressants--Cyclopsorin A, Mycophenolate mofetyl and phototherapy that is not feasible for most patients.
Thus there is a large unmet need for safer and better treatments for moderate to severe atopic dermatitis patients.
Dupilumab is different since it only targets one immune axis--Th2 axis, providing a safer alternative, with high efficacy, that is equal or even better than cyclosporin A, that is the current gold standard immune suppressant, and harbors many side effects including permanent effects on the kidneys after long term use. Topical treatments, while useful for mild patients, are often not adequate or sufficient to control moderate to severe patients that usually have more than 10% body surface area involved and need a systemic treatment.
Dr. Guttman[/caption]
Emma Guttman, MD, PhD
Professor, Dermatology, Medicine and Clinical Immunology
Vice Chair of Research in the Dermatology Department
Director of the center for Excellence
Eczema in the Occupational/Contact Dermatitis clinic
Director of the Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai Medical Center
New York
MedicalResearch.com: Would you briefly explain what is meant by atopic dermatitis? How many people are affected by this disorder?
Response: Atopic dermatitis or eczema as most people know it is an itchy red scaly skin disorder characterized by a very severe itch, that disrupts daily activities, and sleep and severely impairs the quality of life of patients. In the US 30 million people are affected by it, and 1/3 of these we expect to be moderate to severe.
MedicalResearch.com: What is the background for Dupilumab therapy? How does it differ from emollients, steroids or topical immunomodulator treatments for eczema ie Protopic?
Response: The background is that we currently do not have good treatments for long term use for our moderate to severe patients. The only approved drug by the FDA for atopic dermatitis in the US is oral prednisone, that has many long term side effects and causes disease rebound upon discontinuation. Other treatments with many side effects
are broad immune suppressants--Cyclopsorin A, Mycophenolate mofetyl and phototherapy that is not feasible for most patients.
Thus there is a large unmet need for safer and better treatments for moderate to severe atopic dermatitis patients.
Dupilumab is different since it only targets one immune axis--Th2 axis, providing a safer alternative, with high efficacy, that is equal or even better than cyclosporin A, that is the current gold standard immune suppressant, and harbors many side effects including permanent effects on the kidneys after long term use. Topical treatments, while useful for mild patients, are often not adequate or sufficient to control moderate to severe patients that usually have more than 10% body surface area involved and need a systemic treatment.
 Dr. Guttman[/caption]
Emma Guttman, MD, PhD
Professor, Dermatology, Medicine and Clinical Immunology
Vice Chair of Research in the Dermatology Department
Director of the center for Excellence
Eczema in the Occupational/Contact Dermatitis clinic
Director of the Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai Medical Center
New York
MedicalResearch.com: Would you briefly explain what is meant by atopic dermatitis? How many people are affected by this disorder?
Response: Atopic dermatitis or eczema as most people know it is an itchy red scaly skin disorder characterized by a very severe itch, that disrupts daily activities, and sleep and severely impairs the quality of life of patients. In the US 30 million people are affected by it, and 1/3 of these we expect to be moderate to severe.
MedicalResearch.com: What is the background for Dupilumab therapy? How does it differ from emollients, steroids or topical immunomodulator treatments for eczema ie Protopic?
Response: The background is that we currently do not have good treatments for long term use for our moderate to severe patients. The only approved drug by the FDA for atopic dermatitis in the US is oral prednisone, that has many long term side effects and causes disease rebound upon discontinuation. Other treatments with many side effects
are broad immune suppressants--Cyclopsorin A, Mycophenolate mofetyl and phototherapy that is not feasible for most patients.
Thus there is a large unmet need for safer and better treatments for moderate to severe atopic dermatitis patients.
Dupilumab is different since it only targets one immune axis--Th2 axis, providing a safer alternative, with high efficacy, that is equal or even better than cyclosporin A, that is the current gold standard immune suppressant, and harbors many side effects including permanent effects on the kidneys after long term use. Topical treatments, while useful for mild patients, are often not adequate or sufficient to control moderate to severe patients that usually have more than 10% body surface area involved and need a systemic treatment.
Dr. Guttman[/caption]
Emma Guttman, MD, PhD
Professor, Dermatology, Medicine and Clinical Immunology
Vice Chair of Research in the Dermatology Department
Director of the center for Excellence
Eczema in the Occupational/Contact Dermatitis clinic
Director of the Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai Medical Center
New York
MedicalResearch.com: Would you briefly explain what is meant by atopic dermatitis? How many people are affected by this disorder?
Response: Atopic dermatitis or eczema as most people know it is an itchy red scaly skin disorder characterized by a very severe itch, that disrupts daily activities, and sleep and severely impairs the quality of life of patients. In the US 30 million people are affected by it, and 1/3 of these we expect to be moderate to severe.
MedicalResearch.com: What is the background for Dupilumab therapy? How does it differ from emollients, steroids or topical immunomodulator treatments for eczema ie Protopic?
Response: The background is that we currently do not have good treatments for long term use for our moderate to severe patients. The only approved drug by the FDA for atopic dermatitis in the US is oral prednisone, that has many long term side effects and causes disease rebound upon discontinuation. Other treatments with many side effects
are broad immune suppressants--Cyclopsorin A, Mycophenolate mofetyl and phototherapy that is not feasible for most patients.
Thus there is a large unmet need for safer and better treatments for moderate to severe atopic dermatitis patients.
Dupilumab is different since it only targets one immune axis--Th2 axis, providing a safer alternative, with high efficacy, that is equal or even better than cyclosporin A, that is the current gold standard immune suppressant, and harbors many side effects including permanent effects on the kidneys after long term use. Topical treatments, while useful for mild patients, are often not adequate or sufficient to control moderate to severe patients that usually have more than 10% body surface area involved and need a systemic treatment.



![Prof. Dr. Kristian Reich, Dermatologikum Hamburg, Hamburg 07.04.2009 | Prof. Dr. Kristian Reich, Dermatologikum Hamburg, Hamburg, Germany, 07.04.2009 | [© (c) Martin Zitzlaff, Emilienstr.78, 20259 Hamburg, Germany, Tel. +491711940261, http://www.zitzlaff.com, martin@zitzlaff.com, Postbank Hamburg BLZ 20010020 Kto.-Nr. 10204204, MwSt. 7%, Veroeffentlichung nur gegen Honorar (MFM) und Belegexemplar, mit Namensnennung]](https://medicalresearch.com/wp-content/uploads/Professor-Reich.jpg)