MedicalResearch.com Interview with:
[caption id="attachment_71837" align="alignleft" width="150"]

Dr. Holly Kramer[/caption]
Dr. Holly Kramer MD, MPH
Professor of Public Health Sciences and Medicine
Division of Nephrology and Hypertension
Loyola University Chicago
MedicalResearch.com: What is the background for this survey? How is UACR measured? Would you explain the significance of albumin in the urine and what creatinine represents?
Response: Approximately
36 million people live with type 2 diabetes (T2D) in the U.S. today, with cardiovascular disease (CVD) being the number one cause of death for this patient population. About
1 in 3 adults with T2D has UACR
>30 mg/g with prevalence approaching
40% in older patients.
Compared to patients with T2D alone, those with elevated UACR face:
-
- 5-times higher risk of hospitalization for heart failure
- 4-times higher risk of CV mortality
- 3-times higher risk of myocardial infarction
Interestingly, once thought of as a traditional renal biomarker, urine albumin-to-creatinine ratio (UACR)
>30 is also a critical biomarker and urgent signal of cardiovascular (CV) risk.
When checking UACR, we look at two things: the amount of albumin leaking into the urine and the creatinine level. Albumin shouldn’t be getting through the kidneys’ filters at all, so when we see a UACR
>30 mg/g, it’s a sign of systemic vascular endothelial dysfunction. So, if albumin is leaking through the blood vessels inside the kidneys, there’s also damage in the vessels across other organs, like the heart.
UACR is such an important early indicator of CV risk in T2D because even small increases follow a clear ‘rule of three’s’. Healthy kidneys secrete 3 mg/g of albumin to creatinine per day, but when it rises to 30 mg/g, a tenfold increase that signals vascular dysfunction and increasing CV risk. At 300 mg/g, another tenfold increase, the damage is more advanced, and CV risk accelerates.
Patients with eGFR >
60 BUT UACR >30 mg/g can have up to 3.6 times increased risk of CV mortality.
As a nephrologist, I’ve been vocal about the potential for this common urine test that we regularly perform, a UACR test, in helping detect CV risk, not just kidney damage, in more patients.
 Photo by Gustavo Fring[/caption]
Historically, medical and dental care have been treated as separate disciplines in the minds of many patients. Most people associate dental visits primarily with cavity prevention, fresh breath, and achieving a bright, confident smile. However, modern clinical research paints a much broader and more complex picture of why oral hygiene is so critical. The human mouth is a literal gateway to the entire body, and neglecting its care can lead to a cascade of medical issues that extend far beyond tooth decay. Establishing a consistent routine with a reliable local dental spot for preventative screenings and professional cleans is actually one of the most effective ways to protect yourself against long-term, chronic systemic inflammation.
The mechanism behind this whole-body impact comes down to the immune system's biological response to bacterial overgrowth. When plaque is allowed to accumulate and harden into tartar, it creates a highly protected environment where harmful bacteria thrive along and beneath the gumline. This bacterial invasion triggers an immediate immune response, causing localised inflammation known as gingivitis. If left untreated by a professional, this early-stage condition progresses into periodontitis. Periodontitis is a severe infection that breaks down the soft tissue and bone supporting the teeth, creating pockets where even more bacteria can rapidly multiply.
Photo by Gustavo Fring[/caption]
Historically, medical and dental care have been treated as separate disciplines in the minds of many patients. Most people associate dental visits primarily with cavity prevention, fresh breath, and achieving a bright, confident smile. However, modern clinical research paints a much broader and more complex picture of why oral hygiene is so critical. The human mouth is a literal gateway to the entire body, and neglecting its care can lead to a cascade of medical issues that extend far beyond tooth decay. Establishing a consistent routine with a reliable local dental spot for preventative screenings and professional cleans is actually one of the most effective ways to protect yourself against long-term, chronic systemic inflammation.
The mechanism behind this whole-body impact comes down to the immune system's biological response to bacterial overgrowth. When plaque is allowed to accumulate and harden into tartar, it creates a highly protected environment where harmful bacteria thrive along and beneath the gumline. This bacterial invasion triggers an immediate immune response, causing localised inflammation known as gingivitis. If left untreated by a professional, this early-stage condition progresses into periodontitis. Periodontitis is a severe infection that breaks down the soft tissue and bone supporting the teeth, creating pockets where even more bacteria can rapidly multiply.
 Photo by Gustavo Fring[/caption]
Historically, medical and dental care have been treated as separate disciplines in the minds of many patients. Most people associate dental visits primarily with cavity prevention, fresh breath, and achieving a bright, confident smile. However, modern clinical research paints a much broader and more complex picture of why oral hygiene is so critical. The human mouth is a literal gateway to the entire body, and neglecting its care can lead to a cascade of medical issues that extend far beyond tooth decay. Establishing a consistent routine with a reliable local dental spot for preventative screenings and professional cleans is actually one of the most effective ways to protect yourself against long-term, chronic systemic inflammation.
The mechanism behind this whole-body impact comes down to the immune system's biological response to bacterial overgrowth. When plaque is allowed to accumulate and harden into tartar, it creates a highly protected environment where harmful bacteria thrive along and beneath the gumline. This bacterial invasion triggers an immediate immune response, causing localised inflammation known as gingivitis. If left untreated by a professional, this early-stage condition progresses into periodontitis. Periodontitis is a severe infection that breaks down the soft tissue and bone supporting the teeth, creating pockets where even more bacteria can rapidly multiply.
Photo by Gustavo Fring[/caption]
Historically, medical and dental care have been treated as separate disciplines in the minds of many patients. Most people associate dental visits primarily with cavity prevention, fresh breath, and achieving a bright, confident smile. However, modern clinical research paints a much broader and more complex picture of why oral hygiene is so critical. The human mouth is a literal gateway to the entire body, and neglecting its care can lead to a cascade of medical issues that extend far beyond tooth decay. Establishing a consistent routine with a reliable local dental spot for preventative screenings and professional cleans is actually one of the most effective ways to protect yourself against long-term, chronic systemic inflammation.
The mechanism behind this whole-body impact comes down to the immune system's biological response to bacterial overgrowth. When plaque is allowed to accumulate and harden into tartar, it creates a highly protected environment where harmful bacteria thrive along and beneath the gumline. This bacterial invasion triggers an immediate immune response, causing localised inflammation known as gingivitis. If left untreated by a professional, this early-stage condition progresses into periodontitis. Periodontitis is a severe infection that breaks down the soft tissue and bone supporting the teeth, creating pockets where even more bacteria can rapidly multiply.

![Most people only think about their teeth when something hurts. A twinge. A sensitivity. A filling that feels loose. Then the appointment gets booked, the problem gets fixed, and life moves on until the next issue surfaces. It is understandable. But it misses something important. Your mouth is connected to your heart, your lungs, your blood sugar, and your immune response. Researchers have been mapping these connections for decades, yet most people never hear about them in a routine check-up. [ IMAGE 1 ] Your Mouth and Your Heart Have More in Common Than You Think The mouth hosts hundreds of bacterial species. In a healthy mouth, they coexist without causing problems. When the balance shifts, certain bacteria become destructive. They inflame gum tissue — and that inflammation does not stay put. Studies in cardiovascular medicine have found consistent associations between gum disease and elevated heart disease risk. The mechanism is surprisingly direct: bacteria from infected gum tissue enter the bloodstream and travel to arterial walls. Researchers have actually found oral bacteria inside arterial plaque samples. That shifted the conversation from statistical association to something far more specific. Diabetes adds another layer. People with poorly controlled blood sugar tend to have more severe gum disease, and untreated gum disease appears to make blood sugar harder to regulate in return. It runs both ways. Respiratory health is also gaining attention — bacteria from the mouth have been linked to pneumonia and lung infections, particularly in older adults. In pregnancy, gum disease has been associated with preterm birth and low birth weight, and some health systems now recommend dental check-ups as standard prenatal care. The Inflammation Factor Nobody Talks About Short-term inflammation is useful — it is the body defending itself. Chronic, low-grade inflammation that drags on for months or years is something else entirely. It sits at the root of heart disease, type 2 diabetes, certain cancers, autoimmune disorders, and cognitive decline. Advanced gum disease is a chronic inflammatory condition. The gums become a persistent source of immune activation, and the chemicals produced — called cytokines — circulate through the body. This is why dental health is no longer just about avoiding cavities. It is about managing one genuine contributor to body-wide inflammation. Gum disease is largely preventable and responds well to treatment. Adults who have drifted away from regular dental care often find that re-establishing it is one of the more impactful decisions they can make. Finding a dentist in Brighton or a trusted local practice and booking that overdue check-up is a reasonable first step. Not perfection — just professional oversight back in the picture. [ IMAGE 2 ] Why Childhood Sets the Trajectory There is a concept in medicine called the critical window — a period in development when habits and exposures have an outsized effect on long-term outcomes. For oral health, that window opens early. Children who see a dentist regularly from a young age get more than clean teeth. They get comfortable with the environment, and that matters more than most parents realise. Dental anxiety stops many adults from seeking timely care, and a significant amount of that anxiety traces back to early experiences. Primary teeth matter too. They hold space in the jaw for permanent teeth, support speech development, and allow children to eat without pain. When lost too early through decay or infection, they disrupt everything that follows. There is a social dimension as well. Children with visible decay or dental pain often hold back — they avoid smiling, eat less comfortably at school, and stay quiet in class. Getting children into a supportive, child-focused environment early makes a genuine difference. Families who want that specialist approach will find that a dedicated kids dentist Newtown or a similarly focused local practice offers both clinical expertise and the patient manner that makes dental visits manageable rather than dreaded. [ IMAGE 3 ] What Good Daily Habits Actually Look Like Brushing twice a day with fluoride toothpaste is still the foundation. Two minutes is the clinical recommendation — most people do around 45 seconds. A simple phone timer changes this more than any gadget will. Electric toothbrushes consistently outperform manual ones in the research, particularly along the gumline. Flossing clears the contact points between teeth that bristles cannot reach — precisely where decay and gum disease most often begin. If flossing feels awkward, interdental brushes are easier and equally effective. Diet matters more than most people expect, but perhaps not in the way they think. Frequency of sugar exposure is more damaging than total intake. Each sugary encounter triggers an acid attack on enamel lasting around 20 minutes — sipping a soft drink across three hours is far harder on teeth than something sweet eaten once with a meal. Stress is the overlooked factor. It contributes to grinding and clenching during sleep, which wears enamel and can fracture teeth over time. A dentist can spot the signs early and recommend a night guard before real damage accumulates. Why Waiting Almost Always Costs More A small cavity caught early takes minutes to treat. Left alone, it reaches the nerve — meaning root canal treatment. Left longer still, the tooth may not be salvageable at all. Then comes the extraction, the bone loss, the shifting of adjacent teeth, and eventually the conversation about implants or bridges. At every stage the cost increases. The treatment that costs least and causes least discomfort is always the earliest one. Gum disease follows the same pattern. Early-stage gingivitis reverses with a professional clean and better home care. Advanced periodontitis involves bone loss that cannot be restored, only managed. The only thing separating those two outcomes is usually how long treatment was delayed. Rethinking What Dental Care Is Actually For Your mouth is not separate from your health — it is part of it. Treating dental care as optional, or as something to deal with only when things go wrong, ignores what the evidence has been building toward for years. For adults, that means a regular check-up rhythm with a practice you trust. For parents, it means introducing dental visits early, keeping them calm and low-key, and not letting your own anxieties pass to your children. The research keeps deepening and the connections between oral health and the rest of the body keep getting clearer. Taking care of your mouth is, increasingly, one of the more straightforward things you can do for your overall health. Disclaimer: The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Some links are sponsored. Products, services and providers are not warranted or endorsed by MedicalResearch.com or Eminent Domains Inc. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/2026/05/oral-health-and-bodys-well-being.png)





 Dr. Bell[/caption]
Dr. Jack Bell
Liverpool Heart and Chest Hospital
Liverpool, UK
MedicalResearch.com: What is the background for this study?
Response: Coronary computed tomography angiography (CCTA) is a non-invasive heart scan used in the first-line investigation of patients with suspected stable coronary artery disease (CAD). While CCTA clearly shows blockages in coronary arteries, it is limited in its ability to estimate reduced blood flow, which is necessary to diagnose angina.
An artificial intelligence-based tool (Heartflow) has been developed that analyses CCTA images and provides an estimate of blood flow: CT-derived fractional flow reserve (FFR-CT). The real-world, retrospective English FISH&CHIPS study demonstrated that including FFR-CT as a decision-making tool in the diagnosis of stable CAD reduces the number of subsequent invasive and non-invasive tests performed.
Whether FFR-CT could also be used prognostically, to predict future major cardiovascular events, was not fully understood. Previous studies have had small patient numbers, short follow-up and investigated combined cardiovascular outcomes. We performed an analysis on the national FISH&CHIPS population, which was large enough to determine if FFR-CT adds incremental value to traditional cardiovascular risk factors in predicting cardiovascular outcomes and death.
Dr. Bell[/caption]
Dr. Jack Bell
Liverpool Heart and Chest Hospital
Liverpool, UK
MedicalResearch.com: What is the background for this study?
Response: Coronary computed tomography angiography (CCTA) is a non-invasive heart scan used in the first-line investigation of patients with suspected stable coronary artery disease (CAD). While CCTA clearly shows blockages in coronary arteries, it is limited in its ability to estimate reduced blood flow, which is necessary to diagnose angina.
An artificial intelligence-based tool (Heartflow) has been developed that analyses CCTA images and provides an estimate of blood flow: CT-derived fractional flow reserve (FFR-CT). The real-world, retrospective English FISH&CHIPS study demonstrated that including FFR-CT as a decision-making tool in the diagnosis of stable CAD reduces the number of subsequent invasive and non-invasive tests performed.
Whether FFR-CT could also be used prognostically, to predict future major cardiovascular events, was not fully understood. Previous studies have had small patient numbers, short follow-up and investigated combined cardiovascular outcomes. We performed an analysis on the national FISH&CHIPS population, which was large enough to determine if FFR-CT adds incremental value to traditional cardiovascular risk factors in predicting cardiovascular outcomes and death.




 Dr. Hazen[/caption]
Stanley Hazen, MD, PhD
Chair, Cardiovascular & Metabolic Sciences
Lerner Research Institute
CoSection head, Preventive Cardiology & Cardiovascular Rehabilitation
Heart, Vascular and Thoracic Institute
Cleveland Clinic
MedicalResearch.com: What is the background for this study?
Response: One of the unique features of COVID is that in some subjects, there unfortunately appear to be long term adverse effects that can occur following resolution of the acute infection. These studies add to the growing body of data showing that COVID-19 infection can enhance risk for experiencing adverse cardiac events (heart attack, stroke, and death) over time.
Dr. Hazen[/caption]
Stanley Hazen, MD, PhD
Chair, Cardiovascular & Metabolic Sciences
Lerner Research Institute
CoSection head, Preventive Cardiology & Cardiovascular Rehabilitation
Heart, Vascular and Thoracic Institute
Cleveland Clinic
MedicalResearch.com: What is the background for this study?
Response: One of the unique features of COVID is that in some subjects, there unfortunately appear to be long term adverse effects that can occur following resolution of the acute infection. These studies add to the growing body of data showing that COVID-19 infection can enhance risk for experiencing adverse cardiac events (heart attack, stroke, and death) over time.











 Dr. Simin Liu[/caption]
Simin Liu MD MPH ScD
Professor of Epidemiology at the School of Public Health,
Professor of Medicine (Endocrinology) and
Professor of Surgery at the Alpert School of Medicine
Brown University
MedicalResearch.com: What is the background for this study?
Response: Our research team has been researching the roles of environmental and genetic determinants of chronic diseases for nearly three decades, with special emphasis on evaluating micronutrients, minerals, and trace elements in relation to cardiometabolic outcomes, and findings of which have contributed to the design of several large, randomized trials of dietary supplements in the US (Liu JAMA 1999; 2011; Diabetes Care 2005a,b; Diabetes 2006). Several large intervention trials have consistently shown beneficial effects on clinical cardiometabolic outcomes of a diet pattern rich in micronutrients, although research on micronutrient supplementation has mainly focused on the health effects of a single or a few vitamins and minerals.
We decided to take a comprehensive and systematic approach to evaluate all the publicly available/accessible studies reporting all micronutrients including phytochemicals and antioxidant supplements and their effects on cardiovascular risk factors as well as multiple CVDs.
Dr. Simin Liu[/caption]
Simin Liu MD MPH ScD
Professor of Epidemiology at the School of Public Health,
Professor of Medicine (Endocrinology) and
Professor of Surgery at the Alpert School of Medicine
Brown University
MedicalResearch.com: What is the background for this study?
Response: Our research team has been researching the roles of environmental and genetic determinants of chronic diseases for nearly three decades, with special emphasis on evaluating micronutrients, minerals, and trace elements in relation to cardiometabolic outcomes, and findings of which have contributed to the design of several large, randomized trials of dietary supplements in the US (Liu JAMA 1999; 2011; Diabetes Care 2005a,b; Diabetes 2006). Several large intervention trials have consistently shown beneficial effects on clinical cardiometabolic outcomes of a diet pattern rich in micronutrients, although research on micronutrient supplementation has mainly focused on the health effects of a single or a few vitamins and minerals.
We decided to take a comprehensive and systematic approach to evaluate all the publicly available/accessible studies reporting all micronutrients including phytochemicals and antioxidant supplements and their effects on cardiovascular risk factors as well as multiple CVDs.
 Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
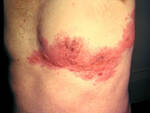
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.



