MedicalResearch.com Interview with:
[caption id="attachment_36710" align="alignleft" width="179"]

Dr. Rish[/caption]
Irina Rish PhD
IBM T.J. Watson Research Center
Yorktown Heights, NY 10598
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Schizophrenia is a chronic and severe psychiatric disorder that affects roughly about 1% of population. Although it is not as common as other mental disorders, such as depression, anxiety, and attention deficit disorder (ADD), and so on, schizophrenia is perhaps one of the most debilitating psychiatric disorders, preventing people from normal functioning in daily life. It is characterized primarily by a range of psychotic symptoms, including hallucinations (false auditory, visual or tactile perceptions detached from reality), as well as delusions, disorganized thoughts, speech and behavior, and multiple other symptoms including difficulty showing (and recognizing) emotions, poor executive functioning, inattentiveness, problems with working memory, and so one. Overall, schizophrenia has a devastating impact not only on patients and their families, but on the economy, as it was estimated to cost the US about 2% off gross national product in treatment costs, missed work, etc.
Thus, taking steps towards better understanding of the disease can potentially lead to more accurate early diagnosis and better treatments.
In this work, the objective was to identify "statistical biomarkers' of schizophrenia from brain imaging data (specifically, functional MRI), i.e. brain activity patterns that would be capable of accurately discriminating between schizophrenic patients and controls, and reproducible (stable) across multiple datasets. The focus on both predictive accuracy (generalization to previously unseen subjects) as well as on stability (reproducibility) across multiple datsets differentiates our work from majority of similar studies in neuroimaging field that tend to focus only on statistically significant differences between such patterns on a fixed dataset, and may not reliably generalize to new data.
Our prior work on neuroimaging-based analysis of schizoprenia
http://journals.plos.org/plosone/article/related?id=10.1371/journal.pone.0050625, as well as other research in the field, suggest that disrupted functional connectivity can be a much more informative source of discriminative patterns than local changes in brain activations, since schizophrenia is well known to be a "network disease", rather than a localized one.
 Pexels Photo by MART PRODUCTION[/caption]
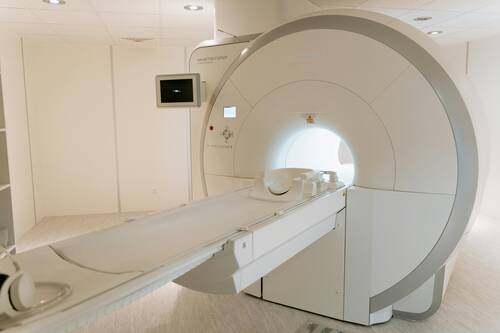
MRI (Magnetic Resonance Imaging) machines are complex and rely on a range of parts working together to deliver clear imaging. Due to their heavy daily use in hospitals and clinics, some parts undergo more wear and tear than others. Replacing these components on time is crucial for ensuring accurate diagnostics and patient safety. Below, we’ll explore the MRI parts that most often require replacement and offer tips on how to find quality MRI spare parts.
Pexels Photo by MART PRODUCTION[/caption]
MRI (Magnetic Resonance Imaging) machines are complex and rely on a range of parts working together to deliver clear imaging. Due to their heavy daily use in hospitals and clinics, some parts undergo more wear and tear than others. Replacing these components on time is crucial for ensuring accurate diagnostics and patient safety. Below, we’ll explore the MRI parts that most often require replacement and offer tips on how to find quality MRI spare parts.
 Pexels Photo by MART PRODUCTION[/caption]
MRI (Magnetic Resonance Imaging) machines are complex and rely on a range of parts working together to deliver clear imaging. Due to their heavy daily use in hospitals and clinics, some parts undergo more wear and tear than others. Replacing these components on time is crucial for ensuring accurate diagnostics and patient safety. Below, we’ll explore the MRI parts that most often require replacement and offer tips on how to find quality MRI spare parts.
Pexels Photo by MART PRODUCTION[/caption]
MRI (Magnetic Resonance Imaging) machines are complex and rely on a range of parts working together to deliver clear imaging. Due to their heavy daily use in hospitals and clinics, some parts undergo more wear and tear than others. Replacing these components on time is crucial for ensuring accurate diagnostics and patient safety. Below, we’ll explore the MRI parts that most often require replacement and offer tips on how to find quality MRI spare parts.



 Dr. Schreiber[/caption]
Darren Schreiber JD PhD
Senior Lecturer
Exeter
MedicalResearch.com: What is the background for this study?
Response: My co-authors and I saw an opportunity to match existing functional brain imaging data with publicly available voter registration data so that we could look for patterns that distinguish brain activity in nonpartisans from partisans. While a number of studies have found differences in both brain structure and function between partisans on the left and right and there is a massive amount of scholarship in political science on partisans and polarization, no brain imaging work had focused on nonpartisans. Around 40% of Americans do not affiliate with a political party and one important campaign strategy has been to persuade these voters to support party candidates. However many political scientists are skeptical about voters claims to be nonpartisans and will instead treat them as if they were merely covert partisans.
Dr. Schreiber[/caption]
Darren Schreiber JD PhD
Senior Lecturer
Exeter
MedicalResearch.com: What is the background for this study?
Response: My co-authors and I saw an opportunity to match existing functional brain imaging data with publicly available voter registration data so that we could look for patterns that distinguish brain activity in nonpartisans from partisans. While a number of studies have found differences in both brain structure and function between partisans on the left and right and there is a massive amount of scholarship in political science on partisans and polarization, no brain imaging work had focused on nonpartisans. Around 40% of Americans do not affiliate with a political party and one important campaign strategy has been to persuade these voters to support party candidates. However many political scientists are skeptical about voters claims to be nonpartisans and will instead treat them as if they were merely covert partisans.
 Dr. Kooraki[/caption]
Soheil Kooraki MSR MS, MD
on behalf of Dr. Ali Gholamrezanezhad MD and co-authors
Department of Radiological Sciences,
David Geffen School of Medicine, University of California at Los Angeles
Los Angeles, California
MedicalResearch.com: What is the background for this study? What are the main findings?
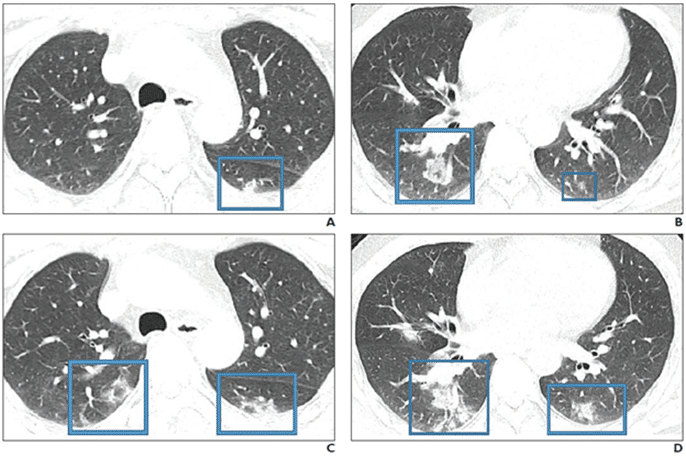
Response: COVID19 is a novel strain of the coronavirus family causing pneumonia. Two similar strains were discovered in 2003 and 2012 to cause the so-called SARS and MERS outbreaks, respectively. Radiologists need to be prepared for the escalating incidence of COVID-19. We reviewed the literature to extract the epidemiologic and imaging features of SARS and MERS in comparison with known imaging features of COVID-19 pneumonia to have a better understanding of the imaging features of the COVID19 pneumonia in acute and post-recovery stages.
Dr. Kooraki[/caption]
Soheil Kooraki MSR MS, MD
on behalf of Dr. Ali Gholamrezanezhad MD and co-authors
Department of Radiological Sciences,
David Geffen School of Medicine, University of California at Los Angeles
Los Angeles, California
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: COVID19 is a novel strain of the coronavirus family causing pneumonia. Two similar strains were discovered in 2003 and 2012 to cause the so-called SARS and MERS outbreaks, respectively. Radiologists need to be prepared for the escalating incidence of COVID-19. We reviewed the literature to extract the epidemiologic and imaging features of SARS and MERS in comparison with known imaging features of COVID-19 pneumonia to have a better understanding of the imaging features of the COVID19 pneumonia in acute and post-recovery stages.