MedicalResearch.com Interview with:
[caption id="attachment_32250" align="alignleft" width="142"] Dr. Michael Saladin[/caption]
Michael E. Saladin, Ph.D.
Professor, Department of Health Sciences and Research
College of Health Professions
Medical University of South Carolina
Charleston, SC
MedicalResearch.com: What is the background for this study?
Response: To the extent that learning and memory processes govern all aspects of behavior, they also govern dysregulated or maladaptive behaviors such as addiction and anxiety states. In the former case, stimuli associated with drug administration can acquire the ability to control drug-related motivational states (urges and craving) as well as drug seeking behavior. To illustrate the point, the simple act of observing a person light up a cigarette will cause the typical smoker to desire a cigarette and engage in smoking. A nonsmoker, by contrast, would not be similarly affected because they have no history where stimuli associated with smoking (e.g., sight of a lighter, cigarettes, plumes of smoke) are reliably paired with, or followed by, the rewarding effects of nicotine.
The research we conducted recently was based on neuroscience research showing that retrieved drug-associated memories (prompted with drug-paired cues) can be updated with information that decreases drug craving and/or administration. One such study showed that heroin craving in heroin addicts can be decreased by retrieving memories for heroin use via a brief heroin cue presentation (video of people using heroin) and then, a short time later, presenting an extensive variety of heroin cues (video, pictures and heroin use paraphernalia) over a 1-hour period. The logic of this intervention was that once the heroin memories were prompted into a labile state by the brief video presentation, the extensive heroin cue exposure would serve to update the content of the original memories with new information (i.e., cues are not followed by heroin reward) that is inconsistent with the original cue-drug contingency (i.e., cues are followed with heroin reward). Remarkably, just two sessions of this type of training, which we call retrieval-extinction training, resulted in significant reductions in heroin craving that persisted for six months. This study was done with heroin addicts who were inpatients so there was no way to assess the effects of this treatment on actual heroin use.
Dr. Michael Saladin[/caption]
Michael E. Saladin, Ph.D.
Professor, Department of Health Sciences and Research
College of Health Professions
Medical University of South Carolina
Charleston, SC
MedicalResearch.com: What is the background for this study?
Response: To the extent that learning and memory processes govern all aspects of behavior, they also govern dysregulated or maladaptive behaviors such as addiction and anxiety states. In the former case, stimuli associated with drug administration can acquire the ability to control drug-related motivational states (urges and craving) as well as drug seeking behavior. To illustrate the point, the simple act of observing a person light up a cigarette will cause the typical smoker to desire a cigarette and engage in smoking. A nonsmoker, by contrast, would not be similarly affected because they have no history where stimuli associated with smoking (e.g., sight of a lighter, cigarettes, plumes of smoke) are reliably paired with, or followed by, the rewarding effects of nicotine.
The research we conducted recently was based on neuroscience research showing that retrieved drug-associated memories (prompted with drug-paired cues) can be updated with information that decreases drug craving and/or administration. One such study showed that heroin craving in heroin addicts can be decreased by retrieving memories for heroin use via a brief heroin cue presentation (video of people using heroin) and then, a short time later, presenting an extensive variety of heroin cues (video, pictures and heroin use paraphernalia) over a 1-hour period. The logic of this intervention was that once the heroin memories were prompted into a labile state by the brief video presentation, the extensive heroin cue exposure would serve to update the content of the original memories with new information (i.e., cues are not followed by heroin reward) that is inconsistent with the original cue-drug contingency (i.e., cues are followed with heroin reward). Remarkably, just two sessions of this type of training, which we call retrieval-extinction training, resulted in significant reductions in heroin craving that persisted for six months. This study was done with heroin addicts who were inpatients so there was no way to assess the effects of this treatment on actual heroin use.
 Dr. Michael Saladin[/caption]
Michael E. Saladin, Ph.D.
Professor, Department of Health Sciences and Research
College of Health Professions
Medical University of South Carolina
Charleston, SC
MedicalResearch.com: What is the background for this study?
Response: To the extent that learning and memory processes govern all aspects of behavior, they also govern dysregulated or maladaptive behaviors such as addiction and anxiety states. In the former case, stimuli associated with drug administration can acquire the ability to control drug-related motivational states (urges and craving) as well as drug seeking behavior. To illustrate the point, the simple act of observing a person light up a cigarette will cause the typical smoker to desire a cigarette and engage in smoking. A nonsmoker, by contrast, would not be similarly affected because they have no history where stimuli associated with smoking (e.g., sight of a lighter, cigarettes, plumes of smoke) are reliably paired with, or followed by, the rewarding effects of nicotine.
The research we conducted recently was based on neuroscience research showing that retrieved drug-associated memories (prompted with drug-paired cues) can be updated with information that decreases drug craving and/or administration. One such study showed that heroin craving in heroin addicts can be decreased by retrieving memories for heroin use via a brief heroin cue presentation (video of people using heroin) and then, a short time later, presenting an extensive variety of heroin cues (video, pictures and heroin use paraphernalia) over a 1-hour period. The logic of this intervention was that once the heroin memories were prompted into a labile state by the brief video presentation, the extensive heroin cue exposure would serve to update the content of the original memories with new information (i.e., cues are not followed by heroin reward) that is inconsistent with the original cue-drug contingency (i.e., cues are followed with heroin reward). Remarkably, just two sessions of this type of training, which we call retrieval-extinction training, resulted in significant reductions in heroin craving that persisted for six months. This study was done with heroin addicts who were inpatients so there was no way to assess the effects of this treatment on actual heroin use.
Dr. Michael Saladin[/caption]
Michael E. Saladin, Ph.D.
Professor, Department of Health Sciences and Research
College of Health Professions
Medical University of South Carolina
Charleston, SC
MedicalResearch.com: What is the background for this study?
Response: To the extent that learning and memory processes govern all aspects of behavior, they also govern dysregulated or maladaptive behaviors such as addiction and anxiety states. In the former case, stimuli associated with drug administration can acquire the ability to control drug-related motivational states (urges and craving) as well as drug seeking behavior. To illustrate the point, the simple act of observing a person light up a cigarette will cause the typical smoker to desire a cigarette and engage in smoking. A nonsmoker, by contrast, would not be similarly affected because they have no history where stimuli associated with smoking (e.g., sight of a lighter, cigarettes, plumes of smoke) are reliably paired with, or followed by, the rewarding effects of nicotine.
The research we conducted recently was based on neuroscience research showing that retrieved drug-associated memories (prompted with drug-paired cues) can be updated with information that decreases drug craving and/or administration. One such study showed that heroin craving in heroin addicts can be decreased by retrieving memories for heroin use via a brief heroin cue presentation (video of people using heroin) and then, a short time later, presenting an extensive variety of heroin cues (video, pictures and heroin use paraphernalia) over a 1-hour period. The logic of this intervention was that once the heroin memories were prompted into a labile state by the brief video presentation, the extensive heroin cue exposure would serve to update the content of the original memories with new information (i.e., cues are not followed by heroin reward) that is inconsistent with the original cue-drug contingency (i.e., cues are followed with heroin reward). Remarkably, just two sessions of this type of training, which we call retrieval-extinction training, resulted in significant reductions in heroin craving that persisted for six months. This study was done with heroin addicts who were inpatients so there was no way to assess the effects of this treatment on actual heroin use.







 Marissa Hall[/caption]
Marissa G. Hall, MSPH
Doctoral Candidate, Department of Health Behavior
Gillings School of Global Public Health
University of North Carolina at Chapel Hill
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The US Food and Drug Administration (FDA) requires pictorial warnings on cigarette packs, but implementation was stalled by a 2012 lawsuit by the tobacco industry. The US Court of Appeals for the DC Circuit ruled against pictorial warnings, saying that FDA had “not provided a shred of evidence” that the pictorial warnings reduce smoking. To address this critique, our randomized trial examined the impact on smoking behavior of adding pictorial warnings to the front and back of cigarette packs. We found that smokers with pictorial warnings on their packs were more likely to attempt to quit and to successfully quit than those whose packs had text-only warnings.
Marissa Hall[/caption]
Marissa G. Hall, MSPH
Doctoral Candidate, Department of Health Behavior
Gillings School of Global Public Health
University of North Carolina at Chapel Hill
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The US Food and Drug Administration (FDA) requires pictorial warnings on cigarette packs, but implementation was stalled by a 2012 lawsuit by the tobacco industry. The US Court of Appeals for the DC Circuit ruled against pictorial warnings, saying that FDA had “not provided a shred of evidence” that the pictorial warnings reduce smoking. To address this critique, our randomized trial examined the impact on smoking behavior of adding pictorial warnings to the front and back of cigarette packs. We found that smokers with pictorial warnings on their packs were more likely to attempt to quit and to successfully quit than those whose packs had text-only warnings.
 Dr. Alan Brown[/caption]
Alan S. Brown, M.D., M.P.H.
Professor of Psychiatry and Epidemiology
Columbia University Medical Center
Director, Program in Birth Cohort Studies, Division of Epidemiology
New York State Psychiatric Institute
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Brown: Smoking during pregnancy is a risk factor for several pregnancy-related outcomes including low birthweight and preterm birth. Evidence for a link with schizophrenia is scant. We analyzed a maternal biomarker of smoking called cotinine, a nicotine metabolite, in mothers of nearly 1,000 schizophrenia cases and 1,000 controls in a national birth cohort in Finland. We found that heavy smoking in pregnancy was related to a 38% increase in schizophrenia risk in offspring and that as cotinine levels increased even in the more moderate smokers risk of schizophrenia also increased.
Dr. Alan Brown[/caption]
Alan S. Brown, M.D., M.P.H.
Professor of Psychiatry and Epidemiology
Columbia University Medical Center
Director, Program in Birth Cohort Studies, Division of Epidemiology
New York State Psychiatric Institute
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Brown: Smoking during pregnancy is a risk factor for several pregnancy-related outcomes including low birthweight and preterm birth. Evidence for a link with schizophrenia is scant. We analyzed a maternal biomarker of smoking called cotinine, a nicotine metabolite, in mothers of nearly 1,000 schizophrenia cases and 1,000 controls in a national birth cohort in Finland. We found that heavy smoking in pregnancy was related to a 38% increase in schizophrenia risk in offspring and that as cotinine levels increased even in the more moderate smokers risk of schizophrenia also increased.
 Dr. Tanush Gupta[/caption]
Tanush Gupta, MD
Chief Resident & Instructor of Medicine
Department of Medicine
New York Medical College & Westchester Medical Center
Valhalla, NY
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Gupta: Cigarette smoking is the leading preventable cause of premature death in the United States (U.S.). Approximately one-third of all coronary artery disease related deaths in the U.S. annually can be attributed to cigarette smoking. However, studies from the pre-thrombolytic and thrombolytic eras have shown that mortality in smokers with ST-segment elevation myocardial infarction (STEMI) may be lower than in nonsmokers, a phenomenon called the “smoker’s paradox.”
The majority of STEMI patients in contemporary practice are treated with primary percutaneous coronary intervention (pPCI). Data on the association of smoking with outcomes in STEMI patients undergoing pPCI are limited and also conflicting as to whether the smoker’s paradox exists in this population. Hence, the purpose of our study was to examine the association of smoking status with in-hospital outcomes in a nationwide cohort of STEMI patients undergoing pPCI, included in the U.S. National Inpatient Sample, over a 10-year time period from 2003 to 2012. Our primary outcome of interest was in-hospital mortality and secondary outcomes were post-procedure hemorrhage, in-hospital cardiac arrest, and average length of stay.
Of 985,174 STEMI patients who underwent pPCI in the U.S. over this time period, 438,954 (44.6%) were smokers. Smokers were on an average 8 years younger than nonsmokers and had lower prevalence of most cardiovascular comorbidities. Smoking status was associated with lower risk-adjusted in-hospital mortality (2.0% vs. 5.9%, adjusted OR 0.60, p<0.001), lower incidence of post-procedure hemorrhage (4.2% vs. 6.1%, adjusted OR 0.81, p<0.001) and in-hospital cardiac arrest (1.3% vs. 2.1%, adjusted OR 0.78, p<0.001), and shorter average length of stay (3.5 days vs. 4.5 days, p<0.001). To assess whether younger age of smokers was influencing the association with in-hospital mortality, we also performed an age-stratified analyses in different age groups. The smoker’s paradox largely persisted in age-stratified analyses suggesting that younger age of smokers was not the sole explanation for this paradox.
We performed additional assessment for confounding to explore whether the paradoxically lower risk-adjusted in-hospital mortality in smokers with STEMI was driven by differences in baseline demographics and comorbidities between hospitalized smokers and nonsmokers in general. To test for such confounding, we examined the association of smoking with in-hospital mortality in 2 conditions in which this association has not been previously studied – hip fractures and severe sepsis – using similar statistical regression models. In both these study populations, smokers were on average younger than nonsmokers and had lower risk-adjusted in-hospital mortality, but, the paradoxical association in both these conditions was weaker in magnitude than in STEMI patients. Since there is no cogent biological hypothesis to explain the lower mortality in smokers with sepsis or hip fractures, it is likely that the smoker’s paradox in STEMI is also at least partly driven by residual confounding due to inadequate adjustment for the biological effects of age. However, as this paradox was stronger in STEMI patients than in patients with hip fractures or severe sepsis, we believe that additional true biological differences between smokers and nonsmokers with STEMI also contribute to the paradoxically lower in-hospital mortality.
Dr. Tanush Gupta[/caption]
Tanush Gupta, MD
Chief Resident & Instructor of Medicine
Department of Medicine
New York Medical College & Westchester Medical Center
Valhalla, NY
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Gupta: Cigarette smoking is the leading preventable cause of premature death in the United States (U.S.). Approximately one-third of all coronary artery disease related deaths in the U.S. annually can be attributed to cigarette smoking. However, studies from the pre-thrombolytic and thrombolytic eras have shown that mortality in smokers with ST-segment elevation myocardial infarction (STEMI) may be lower than in nonsmokers, a phenomenon called the “smoker’s paradox.”
The majority of STEMI patients in contemporary practice are treated with primary percutaneous coronary intervention (pPCI). Data on the association of smoking with outcomes in STEMI patients undergoing pPCI are limited and also conflicting as to whether the smoker’s paradox exists in this population. Hence, the purpose of our study was to examine the association of smoking status with in-hospital outcomes in a nationwide cohort of STEMI patients undergoing pPCI, included in the U.S. National Inpatient Sample, over a 10-year time period from 2003 to 2012. Our primary outcome of interest was in-hospital mortality and secondary outcomes were post-procedure hemorrhage, in-hospital cardiac arrest, and average length of stay.
Of 985,174 STEMI patients who underwent pPCI in the U.S. over this time period, 438,954 (44.6%) were smokers. Smokers were on an average 8 years younger than nonsmokers and had lower prevalence of most cardiovascular comorbidities. Smoking status was associated with lower risk-adjusted in-hospital mortality (2.0% vs. 5.9%, adjusted OR 0.60, p<0.001), lower incidence of post-procedure hemorrhage (4.2% vs. 6.1%, adjusted OR 0.81, p<0.001) and in-hospital cardiac arrest (1.3% vs. 2.1%, adjusted OR 0.78, p<0.001), and shorter average length of stay (3.5 days vs. 4.5 days, p<0.001). To assess whether younger age of smokers was influencing the association with in-hospital mortality, we also performed an age-stratified analyses in different age groups. The smoker’s paradox largely persisted in age-stratified analyses suggesting that younger age of smokers was not the sole explanation for this paradox.
We performed additional assessment for confounding to explore whether the paradoxically lower risk-adjusted in-hospital mortality in smokers with STEMI was driven by differences in baseline demographics and comorbidities between hospitalized smokers and nonsmokers in general. To test for such confounding, we examined the association of smoking with in-hospital mortality in 2 conditions in which this association has not been previously studied – hip fractures and severe sepsis – using similar statistical regression models. In both these study populations, smokers were on average younger than nonsmokers and had lower risk-adjusted in-hospital mortality, but, the paradoxical association in both these conditions was weaker in magnitude than in STEMI patients. Since there is no cogent biological hypothesis to explain the lower mortality in smokers with sepsis or hip fractures, it is likely that the smoker’s paradox in STEMI is also at least partly driven by residual confounding due to inadequate adjustment for the biological effects of age. However, as this paradox was stronger in STEMI patients than in patients with hip fractures or severe sepsis, we believe that additional true biological differences between smokers and nonsmokers with STEMI also contribute to the paradoxically lower in-hospital mortality.


 Dr. Jo Freudenheim[/caption]
MedicalResearch.com Interview with:
Jo Freudenheim, PhD
UB Distinguished Professor and Interim Chair
Department of Epidemiology and Environmental Health
School of Public Health and Health Professions
University at Buffalo
Buffalo, NY
Medical Research: What is the background for this study? What are the main findings?
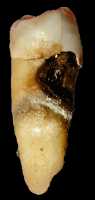
Dr. Freudenheim: There have been a number of studies that have shown an association between periodontal disease and chronic diseases, particularly stroke and heart attacks. There is also some newer evidence that periodontal disease is associated with cancer, particularly cancers of the gastrointestinal tract. Ours is the first large prospective study of periodontal disease and breast cancer.
This was part of a study of more than 70,000 postmenopausal women from throughout the United States, the Women’s Health Initiative. Women provided information about their health and other related factors and then those women were followed to see who developed certain diseases.
We found that women who had been told that they had periodontal disease were more likely to develop breast cancer. In particular, women who were former smokers (quit within the last 20 years) and who had periodontal disease were at increased breast cancer risk. There was a similar increase in risk for current smokers with periodontal disease but it was not statistically significant. (There was a relatively small number of current smokers in the WHI study.)
Dr. Jo Freudenheim[/caption]
MedicalResearch.com Interview with:
Jo Freudenheim, PhD
UB Distinguished Professor and Interim Chair
Department of Epidemiology and Environmental Health
School of Public Health and Health Professions
University at Buffalo
Buffalo, NY
Medical Research: What is the background for this study? What are the main findings?
Dr. Freudenheim: There have been a number of studies that have shown an association between periodontal disease and chronic diseases, particularly stroke and heart attacks. There is also some newer evidence that periodontal disease is associated with cancer, particularly cancers of the gastrointestinal tract. Ours is the first large prospective study of periodontal disease and breast cancer.
This was part of a study of more than 70,000 postmenopausal women from throughout the United States, the Women’s Health Initiative. Women provided information about their health and other related factors and then those women were followed to see who developed certain diseases.
We found that women who had been told that they had periodontal disease were more likely to develop breast cancer. In particular, women who were former smokers (quit within the last 20 years) and who had periodontal disease were at increased breast cancer risk. There was a similar increase in risk for current smokers with periodontal disease but it was not statistically significant. (There was a relatively small number of current smokers in the WHI study.)
 Dr. Villanti[/caption]
MedicalResearch.com Interview with:
Dr. Andrea C. Villanti PhD, MPH
Director, Regulatory Science and Policy Schroeder Institute for Tobacco Research and Policy Studies at Truth Initiative
Washington, DC 20001
Medical Research: What is the background for this study? What are the main findings?
Dr. Villanti: Awareness, interest, and use of electronic cigarettes (e-cigarettes) have increased since the products were introduced in the U.S. in 2006. Between 2012 and 2013, 8.3% of young adults reported current e-cigarette use compared to 4.2% of adults overall. One factor likely driving
Dr. Villanti[/caption]
MedicalResearch.com Interview with:
Dr. Andrea C. Villanti PhD, MPH
Director, Regulatory Science and Policy Schroeder Institute for Tobacco Research and Policy Studies at Truth Initiative
Washington, DC 20001
Medical Research: What is the background for this study? What are the main findings?
Dr. Villanti: Awareness, interest, and use of electronic cigarettes (e-cigarettes) have increased since the products were introduced in the U.S. in 2006. Between 2012 and 2013, 8.3% of young adults reported current e-cigarette use compared to 4.2% of adults overall. One factor likely driving  Dr. Delnevo[/caption]
MedicalResearch.com Interview with:
Cristine D. Delnevo, PhD, MPH
Chair, Professor, and Director, Center for Tobacco Studies
Rutgers School of Public Health
Medical Research: What is the background for this study? What are the main findings?
Dr. Delnevo: We analyzed data from the 2014 National Health Interview Survey (NHIS) to examine how e-cigarette use differs by demographic subgroups and smoking status. We found that daily e-cigarette use is highest among
Dr. Delnevo[/caption]
MedicalResearch.com Interview with:
Cristine D. Delnevo, PhD, MPH
Chair, Professor, and Director, Center for Tobacco Studies
Rutgers School of Public Health
Medical Research: What is the background for this study? What are the main findings?
Dr. Delnevo: We analyzed data from the 2014 National Health Interview Survey (NHIS) to examine how e-cigarette use differs by demographic subgroups and smoking status. We found that daily e-cigarette use is highest among