Author Interviews, Dermatology, JAMA / 22.07.2016
Kaiser Study Reports Clustering of Basal Cell Skin Cancers in Northern California
MedicalResearch.com Interview with:
G. Thomas (Tom) Ray
Division of Research, Kaiser Permanente
2000 Broadway
Oakland, CA 94612-2304
MedicalResearch.com: What is the background for this study?
[caption id="attachment_18144" align="alignleft" width="158"]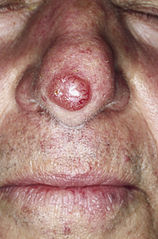 Basal cell skin cancer[/caption]
Response: Basal cell carcinoma (BCC) is the most common cancer in the United States. BCCs tend to develop on sun-exposed areas such as the head and neck and are typically treated with various surgical techniques in an outpatient setting. Although BCCs are rarely fatal, they have been estimated to be among the most costly cancers in the Medicare population due to their high incidence. Yet because these cancers are not tracked by national registries the way, for example, melanoma is, basal cell carcinomas have been difficult to study. Incidence rates in the past have tended to rely on surveys such as those by the National Cancer Institute. And studies using disease codes have, until recently, been difficult because the codes used for basal cell carcinoma and squamous cell carcinoma were the same.
Since 1997, Kaiser Permanente Northern California (KPNC) has had computerized pathology results that allowed us to develop an internal registry of BCC cancers. In addition to having detailed information about basal cell cancer patients, we also had detailed information on the underlying population - KPNC members – which allowed us to determine incidence rates of BCC by age, sex, and most importantly for this study, by geographic location. This is because we know the residential location of all KPNC members at any given time – both those that get basal cell cancer and those who do not. This combination of a validated BCC registry with a well-defined population at-risk gave us the unique ability to investigate the spatial distribution of BCC in Northern California and assess whether there existed geographic clustering of basal cell cancers. Although the investigation of spatial clustering of other cancers is fairly common, no such analyses have been performed for basal cell cancer in the United States.
Basal cell skin cancer[/caption]
Response: Basal cell carcinoma (BCC) is the most common cancer in the United States. BCCs tend to develop on sun-exposed areas such as the head and neck and are typically treated with various surgical techniques in an outpatient setting. Although BCCs are rarely fatal, they have been estimated to be among the most costly cancers in the Medicare population due to their high incidence. Yet because these cancers are not tracked by national registries the way, for example, melanoma is, basal cell carcinomas have been difficult to study. Incidence rates in the past have tended to rely on surveys such as those by the National Cancer Institute. And studies using disease codes have, until recently, been difficult because the codes used for basal cell carcinoma and squamous cell carcinoma were the same.
Since 1997, Kaiser Permanente Northern California (KPNC) has had computerized pathology results that allowed us to develop an internal registry of BCC cancers. In addition to having detailed information about basal cell cancer patients, we also had detailed information on the underlying population - KPNC members – which allowed us to determine incidence rates of BCC by age, sex, and most importantly for this study, by geographic location. This is because we know the residential location of all KPNC members at any given time – both those that get basal cell cancer and those who do not. This combination of a validated BCC registry with a well-defined population at-risk gave us the unique ability to investigate the spatial distribution of BCC in Northern California and assess whether there existed geographic clustering of basal cell cancers. Although the investigation of spatial clustering of other cancers is fairly common, no such analyses have been performed for basal cell cancer in the United States.
 Basal cell skin cancer[/caption]
Response: Basal cell carcinoma (BCC) is the most common cancer in the United States. BCCs tend to develop on sun-exposed areas such as the head and neck and are typically treated with various surgical techniques in an outpatient setting. Although BCCs are rarely fatal, they have been estimated to be among the most costly cancers in the Medicare population due to their high incidence. Yet because these cancers are not tracked by national registries the way, for example, melanoma is, basal cell carcinomas have been difficult to study. Incidence rates in the past have tended to rely on surveys such as those by the National Cancer Institute. And studies using disease codes have, until recently, been difficult because the codes used for basal cell carcinoma and squamous cell carcinoma were the same.
Since 1997, Kaiser Permanente Northern California (KPNC) has had computerized pathology results that allowed us to develop an internal registry of BCC cancers. In addition to having detailed information about basal cell cancer patients, we also had detailed information on the underlying population - KPNC members – which allowed us to determine incidence rates of BCC by age, sex, and most importantly for this study, by geographic location. This is because we know the residential location of all KPNC members at any given time – both those that get basal cell cancer and those who do not. This combination of a validated BCC registry with a well-defined population at-risk gave us the unique ability to investigate the spatial distribution of BCC in Northern California and assess whether there existed geographic clustering of basal cell cancers. Although the investigation of spatial clustering of other cancers is fairly common, no such analyses have been performed for basal cell cancer in the United States.
Basal cell skin cancer[/caption]
Response: Basal cell carcinoma (BCC) is the most common cancer in the United States. BCCs tend to develop on sun-exposed areas such as the head and neck and are typically treated with various surgical techniques in an outpatient setting. Although BCCs are rarely fatal, they have been estimated to be among the most costly cancers in the Medicare population due to their high incidence. Yet because these cancers are not tracked by national registries the way, for example, melanoma is, basal cell carcinomas have been difficult to study. Incidence rates in the past have tended to rely on surveys such as those by the National Cancer Institute. And studies using disease codes have, until recently, been difficult because the codes used for basal cell carcinoma and squamous cell carcinoma were the same.
Since 1997, Kaiser Permanente Northern California (KPNC) has had computerized pathology results that allowed us to develop an internal registry of BCC cancers. In addition to having detailed information about basal cell cancer patients, we also had detailed information on the underlying population - KPNC members – which allowed us to determine incidence rates of BCC by age, sex, and most importantly for this study, by geographic location. This is because we know the residential location of all KPNC members at any given time – both those that get basal cell cancer and those who do not. This combination of a validated BCC registry with a well-defined population at-risk gave us the unique ability to investigate the spatial distribution of BCC in Northern California and assess whether there existed geographic clustering of basal cell cancers. Although the investigation of spatial clustering of other cancers is fairly common, no such analyses have been performed for basal cell cancer in the United States.






 Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Assistant Professor in Dermatology
Medical Social Sciences and Preventive Medicine
Northwestern University, Chicago, Illinois
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Psoriasis is associated with a number of potential risk factors for developing serious infections, including impaired skin-barrier function, immune dysregulation, use of systemic immunosuppressant and biologic treatments. We hypothesized that adults with psoriasis have higher rates of serious infections.
We examined data from the 2002-2012 National Inpatient Sample, which contains a representative 20% sample of all hospitalizations in the United States. We found that psoriasis was associated with multiple serious infections, including methicillin-resistant Staphylococcus aureus, cellulitis, herpes simplex virus infection, infectious arthritis, osteomyelitis, meningitis, encephalitis and tuberculosis. Rates of serious infections increased over all time.
Significant predictors of serious infections in patients with psoriasis included non-white race, lower estimated income quartile, and Medicaid, Medicare, or self-pay insurance status. These findings suggest that poor access to adequate dermatologic care may be associated with higher rates of infections.
Dr. Jonathan Silverberg[/caption]
Dr. Jonathan L. Silverberg MD PhD MPH
Assistant Professor in Dermatology
Medical Social Sciences and Preventive Medicine
Northwestern University, Chicago, Illinois
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Psoriasis is associated with a number of potential risk factors for developing serious infections, including impaired skin-barrier function, immune dysregulation, use of systemic immunosuppressant and biologic treatments. We hypothesized that adults with psoriasis have higher rates of serious infections.
We examined data from the 2002-2012 National Inpatient Sample, which contains a representative 20% sample of all hospitalizations in the United States. We found that psoriasis was associated with multiple serious infections, including methicillin-resistant Staphylococcus aureus, cellulitis, herpes simplex virus infection, infectious arthritis, osteomyelitis, meningitis, encephalitis and tuberculosis. Rates of serious infections increased over all time.
Significant predictors of serious infections in patients with psoriasis included non-white race, lower estimated income quartile, and Medicaid, Medicare, or self-pay insurance status. These findings suggest that poor access to adequate dermatologic care may be associated with higher rates of infections.
 Dr. Alexander Egeberg[/caption]
Alexander Egeberg, MD PhD
Gentofte Hospital
Department of Dermatology and Allergy
Denmark
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Egeberg: While psoriasis has been associated with an increased risk of cardiovascular disease (CVD), studies have generally neglected to adjust for family history of CVD which is a well-established cardiovascular risk factor.
In a population-based study of young patients with psoriasis, we found an increased risk of CVD only in patients with a positive family history of CVD but not in those patients that did not have a positive family history.
Dr. Alexander Egeberg[/caption]
Alexander Egeberg, MD PhD
Gentofte Hospital
Department of Dermatology and Allergy
Denmark
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Egeberg: While psoriasis has been associated with an increased risk of cardiovascular disease (CVD), studies have generally neglected to adjust for family history of CVD which is a well-established cardiovascular risk factor.
In a population-based study of young patients with psoriasis, we found an increased risk of CVD only in patients with a positive family history of CVD but not in those patients that did not have a positive family history.
 Dr. Laura Ferris[/caption]
MedicalResearch.com Interview with:
Laura Ferris, M.D., Ph.D.
Associate professor, Department of Dermatology
University of Pittsburgh School of Medicine and
Member of the Melanoma Program
University of Pittsburgh Cancer Institute
MedicalResearch.com: What is the background for this study?
Dr. Ferris: Rates of melanoma, the most dangerous form of skin cancer, are on the rise, and skin cancer screenings are one of the most important steps for early detection and treatment. Typically, patients receive skin checks by setting up an appointment with a dermatologist. UPMC instituted a new screening initiative, which was modeled after a promising German program, the goal being to improve the detection of melanomas by making it easier for patients to get screened during routine office visits with their primary care physicians (PCPs). PCPs completed training on how to recognize melanomas and were asked to offer annual screening during office visits to all patients aged 35 and older. In 2014, during the first year of the program, 15 percent of the 333,788 eligible UPMC patients were screened in this fashion.
Dr. Laura Ferris[/caption]
MedicalResearch.com Interview with:
Laura Ferris, M.D., Ph.D.
Associate professor, Department of Dermatology
University of Pittsburgh School of Medicine and
Member of the Melanoma Program
University of Pittsburgh Cancer Institute
MedicalResearch.com: What is the background for this study?
Dr. Ferris: Rates of melanoma, the most dangerous form of skin cancer, are on the rise, and skin cancer screenings are one of the most important steps for early detection and treatment. Typically, patients receive skin checks by setting up an appointment with a dermatologist. UPMC instituted a new screening initiative, which was modeled after a promising German program, the goal being to improve the detection of melanomas by making it easier for patients to get screened during routine office visits with their primary care physicians (PCPs). PCPs completed training on how to recognize melanomas and were asked to offer annual screening during office visits to all patients aged 35 and older. In 2014, during the first year of the program, 15 percent of the 333,788 eligible UPMC patients were screened in this fashion.
 Dr. Benjamin Perry[/caption]
Benjamin M. Perry, DO
Silver Falls Dermatology
Salem, OR 97302
MedicalResearch.com: What is the background for this study?
Dr. Perry: Our interest in this subject developed when a patient came into our clinic with concern of multiple new nevi developing on palmoplantar surfaces following initiation of treatment with Rituximab. We conducted a review of the existing literature and found that this wasn’t a known adverse effect. From that point, we wanted to know the pathogenesis, prognosis, and management for eruptive nevi that developed in the setting of medication use. A collective review had not been previously performed on this subject. In essence, we had questions that were unanswered and set out to find the answers.
Dr. Benjamin Perry[/caption]
Benjamin M. Perry, DO
Silver Falls Dermatology
Salem, OR 97302
MedicalResearch.com: What is the background for this study?
Dr. Perry: Our interest in this subject developed when a patient came into our clinic with concern of multiple new nevi developing on palmoplantar surfaces following initiation of treatment with Rituximab. We conducted a review of the existing literature and found that this wasn’t a known adverse effect. From that point, we wanted to know the pathogenesis, prognosis, and management for eruptive nevi that developed in the setting of medication use. A collective review had not been previously performed on this subject. In essence, we had questions that were unanswered and set out to find the answers.
 Dr. Melissa Wilson[/caption]
Melissa A. Wilson, MD, PhD
Assistant professor of Medical Oncology
NYU Langone Perlmutter Cancer Center
MedicalResearch.com: What are the most common types of skin cancer?
Dr. Wilson: Basal cell carcinoma, squamous cell carcinoma and melanoma. With rare exception, all are related to sun exposure.
MedicalResearch.com: Are some types of skin cancer more serious than others?
Dr. Wilson: Melanoma is the most serious form of skin cancer, with the highest risk of developing into metastatic disease. Most basal cell and squamous cell carcinomas are superficial and not as invasive, so removal is the treatment. Rarely, these can cause invasive and metastatic disease, but this occurs infrequently. Melanoma is much more serious. Of course, the earlier melanoma is detected and the earlier stage that it is, is more predictive of a favorable outcome.
MedicalResearch.com: Who is most prone to skin cancer?
Dr. Wilson: Persons with excessive sun exposure, fair skin, light hair and blue eyes - although it can certainly occur in anyone.
Dr. Melissa Wilson[/caption]
Melissa A. Wilson, MD, PhD
Assistant professor of Medical Oncology
NYU Langone Perlmutter Cancer Center
MedicalResearch.com: What are the most common types of skin cancer?
Dr. Wilson: Basal cell carcinoma, squamous cell carcinoma and melanoma. With rare exception, all are related to sun exposure.
MedicalResearch.com: Are some types of skin cancer more serious than others?
Dr. Wilson: Melanoma is the most serious form of skin cancer, with the highest risk of developing into metastatic disease. Most basal cell and squamous cell carcinomas are superficial and not as invasive, so removal is the treatment. Rarely, these can cause invasive and metastatic disease, but this occurs infrequently. Melanoma is much more serious. Of course, the earlier melanoma is detected and the earlier stage that it is, is more predictive of a favorable outcome.
MedicalResearch.com: Who is most prone to skin cancer?
Dr. Wilson: Persons with excessive sun exposure, fair skin, light hair and blue eyes - although it can certainly occur in anyone.
 Dr. Jack Resneck[/caption]
Jack Resneck, Jr, MD
Professor and Vice-Chair of Dermatology
Core Faculty, Philip R. Lee Institute for Health Policy Studies
UCSF School of Medicine
MedicalResearch.com: What is the background for this study?
What are the main findings?
Dr. Resneck: Telemedicine, when done right, can improve access and offer convenience to patients. We have seen proven high-quality care in telemedicine services where patients are using digital platforms to communicate with their existing doctors who know them, and where doctors are getting teleconsultations from other specialists about their patients. But our study shows major quality problems with the rapidly growing corporate direct-to-consumer services where patients send consults via the web or phone apps to clinicians they don’t know.
Most of these sites aren’t giving patients a choice of the clinician who will care for them or disclosing the credentials of those clinicians – patients should know whether their rash is being cared for by a board-certified dermatologist, a pain management specialist, or a nurse practitioner who usually works in an emergency department. Some of these sites are even using doctors who aren’t licensed in the US. We also found that these sites were regularly missing important diagnoses, and prescribing medications without discussing risks and side-effects, putting patients at risk. We observed that if you upload photos of a highly contagious syphilis rash but state that you think you have psoriasis, most clinicians working for these direct-to-consumer sites will just agree with your self-diagnosis and prescribe psoriasis medications, leaving you with a contagious STD.
Perhaps the biggest problem with many of these sites is the lack of coordinating care for patients – most of them didn’t offer to send records to a patient’s existing local doctors. And when patients end up needing in-person care if their condition worsens, or they have a medication side-effect, those distant clinicians often don’t have local contacts, and are unable to facilitate needed appointments.
Dr. Jack Resneck[/caption]
Jack Resneck, Jr, MD
Professor and Vice-Chair of Dermatology
Core Faculty, Philip R. Lee Institute for Health Policy Studies
UCSF School of Medicine
MedicalResearch.com: What is the background for this study?
What are the main findings?
Dr. Resneck: Telemedicine, when done right, can improve access and offer convenience to patients. We have seen proven high-quality care in telemedicine services where patients are using digital platforms to communicate with their existing doctors who know them, and where doctors are getting teleconsultations from other specialists about their patients. But our study shows major quality problems with the rapidly growing corporate direct-to-consumer services where patients send consults via the web or phone apps to clinicians they don’t know.
Most of these sites aren’t giving patients a choice of the clinician who will care for them or disclosing the credentials of those clinicians – patients should know whether their rash is being cared for by a board-certified dermatologist, a pain management specialist, or a nurse practitioner who usually works in an emergency department. Some of these sites are even using doctors who aren’t licensed in the US. We also found that these sites were regularly missing important diagnoses, and prescribing medications without discussing risks and side-effects, putting patients at risk. We observed that if you upload photos of a highly contagious syphilis rash but state that you think you have psoriasis, most clinicians working for these direct-to-consumer sites will just agree with your self-diagnosis and prescribe psoriasis medications, leaving you with a contagious STD.
Perhaps the biggest problem with many of these sites is the lack of coordinating care for patients – most of them didn’t offer to send records to a patient’s existing local doctors. And when patients end up needing in-person care if their condition worsens, or they have a medication side-effect, those distant clinicians often don’t have local contacts, and are unable to facilitate needed appointments.
 Dr. Uscher-Pines[/caption]
Lori Uscher-Pines, PhD
RAND Corporation
Arlington, Virginia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Although many communities in the U.S. are underserved by dermatologists, access is particularly limited among Medicaid patients. Teledermatology may be one solution to improve access. Our goal with this study was to assess the effect of a novel teledermatology initiative on access to dermatologists among enrollees in a Medicaid Managed Care Plan in California’s Central Valley.
Among all patients who visited a dermatologist after the introduction of teledermatology from 2012-2014 (n=8614), 49% received care via teledermatology. Among patients newly enrolled in Medicaid following Medicaid expansion in 2014, 76% of those who visited a dermatologist received care via teledermatology. Patients of primary care practices that engaged in teledermatology had a 64% increase in the fraction of patients visiting a dermatologist (vs. 21% in other practices) (p<.01). Compared with in-person dermatology, teledermatology served more patients under age 17, male patients, nonwhite patients, and patients without comorbid conditions. Conditions managed across settings varied; teledermatology physicians were more likely to care for viral skin lesions and acne whereas in-person dermatologists were more likely to care for psoriasis and skin neoplasms.
Dr. Uscher-Pines[/caption]
Lori Uscher-Pines, PhD
RAND Corporation
Arlington, Virginia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Although many communities in the U.S. are underserved by dermatologists, access is particularly limited among Medicaid patients. Teledermatology may be one solution to improve access. Our goal with this study was to assess the effect of a novel teledermatology initiative on access to dermatologists among enrollees in a Medicaid Managed Care Plan in California’s Central Valley.
Among all patients who visited a dermatologist after the introduction of teledermatology from 2012-2014 (n=8614), 49% received care via teledermatology. Among patients newly enrolled in Medicaid following Medicaid expansion in 2014, 76% of those who visited a dermatologist received care via teledermatology. Patients of primary care practices that engaged in teledermatology had a 64% increase in the fraction of patients visiting a dermatologist (vs. 21% in other practices) (p<.01). Compared with in-person dermatology, teledermatology served more patients under age 17, male patients, nonwhite patients, and patients without comorbid conditions. Conditions managed across settings varied; teledermatology physicians were more likely to care for viral skin lesions and acne whereas in-person dermatologists were more likely to care for psoriasis and skin neoplasms.
 Dr. Lihi Eder[/caption]
Lihi Eder, MD, PhD
Assistant Professor of Medicine
University of Toronto
Scientist, Women’s College Research Institute,Room 6326
Women’s College Hospital
Toronto, ON, Canada
MedicalResearch.com: What is the background for this study?
Dr. Eder: Psoriasis is a chronic immune-mediated skin disease affecting 2-3% of the general population. Psoriatic arthritis (PsA) affects 15-30% of patients with psoriasis. Until recently, only few studies assessed the risk of developing cardiovascular events in patients with PsA and while most studies found a higher cardiovascular risk in these patients, others reported cardiovascular rates that were similar to the general population.
Dr. Lihi Eder[/caption]
Lihi Eder, MD, PhD
Assistant Professor of Medicine
University of Toronto
Scientist, Women’s College Research Institute,Room 6326
Women’s College Hospital
Toronto, ON, Canada
MedicalResearch.com: What is the background for this study?
Dr. Eder: Psoriasis is a chronic immune-mediated skin disease affecting 2-3% of the general population. Psoriatic arthritis (PsA) affects 15-30% of patients with psoriasis. Until recently, only few studies assessed the risk of developing cardiovascular events in patients with PsA and while most studies found a higher cardiovascular risk in these patients, others reported cardiovascular rates that were similar to the general population.
 Dr. Orit Markowitz[/caption]
Orit Markowitz, MD, FAAD
Director of Pigmented Lesions and Skin Cancer
Assistant Professor of Dermatology
Mount Sinai Medical Center, NY, NY
Director of Pigmented lesions clinic
Brooklyn VA, Brooklyn, NY
Adjunct Professor, Dermatology
SUNY Downstate Medical Center, Brooklyn, NY
Chief of Dermatology
Queens General Hospital, Jamaica, NY
MedicalResearch.com: How common is skin cancer? Is the incidence rising in US adults? Who is most at risk?
Dr. Markowitz: The annual incidence of skin cancer is more than breast, colon, lung, and prostate cancer combined. Of the 7 most common skin cancers in the US melanoma is the only one whose incidence is increasing. The highest risk group for skin cancer are fair skin, adults with a history of sun exposure.
Dr. Orit Markowitz[/caption]
Orit Markowitz, MD, FAAD
Director of Pigmented Lesions and Skin Cancer
Assistant Professor of Dermatology
Mount Sinai Medical Center, NY, NY
Director of Pigmented lesions clinic
Brooklyn VA, Brooklyn, NY
Adjunct Professor, Dermatology
SUNY Downstate Medical Center, Brooklyn, NY
Chief of Dermatology
Queens General Hospital, Jamaica, NY
MedicalResearch.com: How common is skin cancer? Is the incidence rising in US adults? Who is most at risk?
Dr. Markowitz: The annual incidence of skin cancer is more than breast, colon, lung, and prostate cancer combined. Of the 7 most common skin cancers in the US melanoma is the only one whose incidence is increasing. The highest risk group for skin cancer are fair skin, adults with a history of sun exposure.
 Prof. Rudi Beyaert[/caption]
Professor Rudi Beyaert
VIB - Inflammation Research Center Ghent University
Department for Biomedical Molecular Biology Unit of Molecular Signal Transduction in Inflammation
Technologiepark Ghent) Belgium
MedicalResearch.com: What is the background for this study? What are the main findings?
Prof. Beyaert: The interest of my laboratory is in understanding the molecular mechanisms that are responsible for the development of inflammatory diseases such as Crohn's disease, multiple sclerosis, rheumatoid arthritis and also psoriasis, which is the topic of the published study. We already know that genetic factors can determine the onset of these inflammatory diseases, but how these genetic factors drive an inflammatory response is still largely unclear. We were specifically interested in the CARD14 gene, because patients with mutations in CARD14 have a very high chance to develop psoriasis. Psoriasis-associated mutations in CARD14 trigger specific skin cells (keratinocytes) to produce and release large amounts of other proteins that recruit and activate specific white blood cells driving an inflammatory response. We now discovered that this effect is dependent on the physical interaction of CARD14 with the protease MALT1 in keratinocytes, leading to the activation of its enzymatic activity and the MALT1-mediated cleavage and inactivation of a number of cellular proteins that normally keep our immune system in check. Treatment of skin cells with small compound MALT1 inhibitors prevents the CARD14-induced production of several pro-inflammatory mediators.
Prof. Rudi Beyaert[/caption]
Professor Rudi Beyaert
VIB - Inflammation Research Center Ghent University
Department for Biomedical Molecular Biology Unit of Molecular Signal Transduction in Inflammation
Technologiepark Ghent) Belgium
MedicalResearch.com: What is the background for this study? What are the main findings?
Prof. Beyaert: The interest of my laboratory is in understanding the molecular mechanisms that are responsible for the development of inflammatory diseases such as Crohn's disease, multiple sclerosis, rheumatoid arthritis and also psoriasis, which is the topic of the published study. We already know that genetic factors can determine the onset of these inflammatory diseases, but how these genetic factors drive an inflammatory response is still largely unclear. We were specifically interested in the CARD14 gene, because patients with mutations in CARD14 have a very high chance to develop psoriasis. Psoriasis-associated mutations in CARD14 trigger specific skin cells (keratinocytes) to produce and release large amounts of other proteins that recruit and activate specific white blood cells driving an inflammatory response. We now discovered that this effect is dependent on the physical interaction of CARD14 with the protease MALT1 in keratinocytes, leading to the activation of its enzymatic activity and the MALT1-mediated cleavage and inactivation of a number of cellular proteins that normally keep our immune system in check. Treatment of skin cells with small compound MALT1 inhibitors prevents the CARD14-induced production of several pro-inflammatory mediators.






