Allergies, Author Interviews, Dermatology / 20.03.2020
Atopic Dermatitis: Dupilumab Can Rapidly Improve Itch in Moderate to Severe Eczema
MedicalResearch.com Interview with:
[caption id="attachment_53601" align="alignleft" width="144"] Dr. Yosipovitch[/caption]
Gil Yosipovitch, MD, Professor
Miami Itch Center
Lennar Medical Foundation
South Miami Clinic in Coral Gables
University of Miami Health System
MedicalResearch.com: What is the background for this study? How does Dupilumab (Dupixent) differ from other medications for atopic dermatitis/eczema?
Response: Atopic dermatitis (AD) is characterized by intense itch (pruritus) that is one of the most burdensome symptoms; therefore, rapid and sustained improvement in itch is an important marker of treatment benefit. Dupixent® (dupilumab) is approved in the U.S. for adults and adolescents with inadequately-controlled moderate-to-severe Atopic Dermatitis.
Dupilumab remains the first and only biologic medicine for uncontrolled moderate-to-severe atopic dermatitis. Dupilumab is the first and only fully human monoclonal antibody that inhibits the signaling of the interleukin-4 (IL-4) and interleukin-13 (IL-13) proteins. Data from dupilumab clinical trials have shown that IL-4 and IL-13 are key drivers of the type 2 inflammation that plays a major role in atopic dermatitis, asthma and chronic rhinosinusitis with nasal polyps.
Dr. Yosipovitch[/caption]
Gil Yosipovitch, MD, Professor
Miami Itch Center
Lennar Medical Foundation
South Miami Clinic in Coral Gables
University of Miami Health System
MedicalResearch.com: What is the background for this study? How does Dupilumab (Dupixent) differ from other medications for atopic dermatitis/eczema?
Response: Atopic dermatitis (AD) is characterized by intense itch (pruritus) that is one of the most burdensome symptoms; therefore, rapid and sustained improvement in itch is an important marker of treatment benefit. Dupixent® (dupilumab) is approved in the U.S. for adults and adolescents with inadequately-controlled moderate-to-severe Atopic Dermatitis.
Dupilumab remains the first and only biologic medicine for uncontrolled moderate-to-severe atopic dermatitis. Dupilumab is the first and only fully human monoclonal antibody that inhibits the signaling of the interleukin-4 (IL-4) and interleukin-13 (IL-13) proteins. Data from dupilumab clinical trials have shown that IL-4 and IL-13 are key drivers of the type 2 inflammation that plays a major role in atopic dermatitis, asthma and chronic rhinosinusitis with nasal polyps.
 Dr. Yosipovitch[/caption]
Gil Yosipovitch, MD, Professor
Miami Itch Center
Lennar Medical Foundation
South Miami Clinic in Coral Gables
University of Miami Health System
MedicalResearch.com: What is the background for this study? How does Dupilumab (Dupixent) differ from other medications for atopic dermatitis/eczema?
Response: Atopic dermatitis (AD) is characterized by intense itch (pruritus) that is one of the most burdensome symptoms; therefore, rapid and sustained improvement in itch is an important marker of treatment benefit. Dupixent® (dupilumab) is approved in the U.S. for adults and adolescents with inadequately-controlled moderate-to-severe Atopic Dermatitis.
Dupilumab remains the first and only biologic medicine for uncontrolled moderate-to-severe atopic dermatitis. Dupilumab is the first and only fully human monoclonal antibody that inhibits the signaling of the interleukin-4 (IL-4) and interleukin-13 (IL-13) proteins. Data from dupilumab clinical trials have shown that IL-4 and IL-13 are key drivers of the type 2 inflammation that plays a major role in atopic dermatitis, asthma and chronic rhinosinusitis with nasal polyps.
Dr. Yosipovitch[/caption]
Gil Yosipovitch, MD, Professor
Miami Itch Center
Lennar Medical Foundation
South Miami Clinic in Coral Gables
University of Miami Health System
MedicalResearch.com: What is the background for this study? How does Dupilumab (Dupixent) differ from other medications for atopic dermatitis/eczema?
Response: Atopic dermatitis (AD) is characterized by intense itch (pruritus) that is one of the most burdensome symptoms; therefore, rapid and sustained improvement in itch is an important marker of treatment benefit. Dupixent® (dupilumab) is approved in the U.S. for adults and adolescents with inadequately-controlled moderate-to-severe Atopic Dermatitis.
Dupilumab remains the first and only biologic medicine for uncontrolled moderate-to-severe atopic dermatitis. Dupilumab is the first and only fully human monoclonal antibody that inhibits the signaling of the interleukin-4 (IL-4) and interleukin-13 (IL-13) proteins. Data from dupilumab clinical trials have shown that IL-4 and IL-13 are key drivers of the type 2 inflammation that plays a major role in atopic dermatitis, asthma and chronic rhinosinusitis with nasal polyps. 
 Adawiyah Jami[/caption]
Adawiyah Jamil, AdvMDerm
Associate Professor at Department of Medicine
University Kebangsaan Malaysia Medical Center
Kuala Lumpur, Malaysia
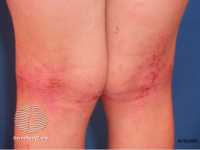
MedicalResearch.com: What is the background for this study?
Response: We commonly observed poor dietary pattern and multiple food restrictions imposed on atopic dermatitis (AD) children by their parents in our daily clinical practice. Food allergy is often associated with AD, however excessive and medically unsubstantiated restriction may lead to various health issues. AD is a chronic skin disease, like any other chronic diseases it affects an individual’s general health. Growth and development are key measures of health in children. We embarked on this study as we were very worried of the consequences of medically unsupervised food restriction, especially those with severe disease. We were concerned about how our atopic dermatitis children are eating and how to help them.
Adawiyah Jami[/caption]
Adawiyah Jamil, AdvMDerm
Associate Professor at Department of Medicine
University Kebangsaan Malaysia Medical Center
Kuala Lumpur, Malaysia
MedicalResearch.com: What is the background for this study?
Response: We commonly observed poor dietary pattern and multiple food restrictions imposed on atopic dermatitis (AD) children by their parents in our daily clinical practice. Food allergy is often associated with AD, however excessive and medically unsubstantiated restriction may lead to various health issues. AD is a chronic skin disease, like any other chronic diseases it affects an individual’s general health. Growth and development are key measures of health in children. We embarked on this study as we were very worried of the consequences of medically unsupervised food restriction, especially those with severe disease. We were concerned about how our atopic dermatitis children are eating and how to help them.


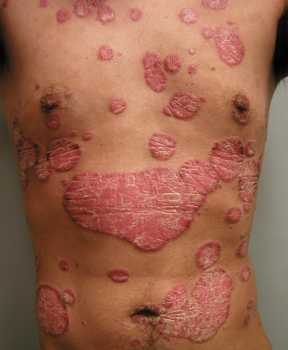




 MedicalResearch.com: What is the background for this study?
Response: A prior pilot
MedicalResearch.com: What is the background for this study?
Response: A prior pilot 
 Dr. Diaz[/caption]
Lucia Diaz, M.D., is chief of pediatric dermatology, dermatology residency associate program director and assistant professor of medicine and pediatrics at Dell Medical School. She is also co-director of the dermatology-rheumatology combined clinic at Dell Children’s Medical Center.
[caption id="attachment_52796" align="alignleft" width="150"]
Dr. Diaz[/caption]
Lucia Diaz, M.D., is chief of pediatric dermatology, dermatology residency associate program director and assistant professor of medicine and pediatrics at Dell Medical School. She is also co-director of the dermatology-rheumatology combined clinic at Dell Children’s Medical Center.
[caption id="attachment_52796" align="alignleft" width="150"] Dr. Jaquez[/caption]
Sasha Jaquez, Ph.D. is a pediatric psychologist at Dell Children's Medical School/Dell Children's Medical Center and specializes in seeing children with chronic medical illness, including skin disorders.
[caption id="attachment_52791" align="alignleft" width="294"]
Dr. Jaquez[/caption]
Sasha Jaquez, Ph.D. is a pediatric psychologist at Dell Children's Medical School/Dell Children's Medical Center and specializes in seeing children with chronic medical illness, including skin disorders.
[caption id="attachment_52791" align="alignleft" width="294"]







 Dr. Helen Marsden PhD
Skin Analytics Limited
London, United Kingdom
MedicalResearch.com: What is the background for this study?
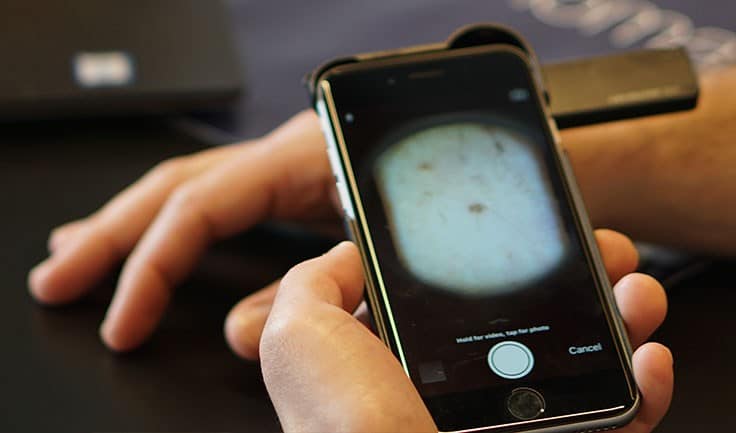
Response: In this technology age, with the explosion of interest and applications using Artificial Intelligence, it is easy to accept the output of a technology-based test - such as a smartphone app designed to identify skin cancer - without thinking too much about it. In reality, technology is only as good as the way it has been developed, tested and validated. In particular, AI algorithms are prone to a lack of “generalisation” - i.e. their performance drops when presented with data it has not seen before. In the medical field, and particularly in areas where AI is being developed to direct a patient’s diagnosis or care, this is particularly problematic. Inappropriate diagnosis or advice to patients can lead to false reassurance, heightened concern and pressure on NHS services, or worse. It is concerning, therefore, that there are a large number of smartphone apps available that provide an assessment of skin lesions, including some that provide an estimate of the probability of malignancy, that have not been assessed for diagnostic accuracy.
Skin Analytics has developed an AI-based algorithm, named: Deep Ensemble for Recognition of Malignancy (DERM), for use as a decision support tool for healthcare providers. DERM determines the likelihood of skin cancer from dermoscopic images of skin lesions. It was developed using deep learning techniques that identify and assess features of these lesions which are associated with melanoma, using over 7,000 archived dermoscopic images. Using these images, it was shown to identify melanoma with similar accuracy to specialist physicians. However, to prove the algorithm could be used in a real life clinical setting, Skin Analytics set out to conduct a clinical validation study.
Dr. Helen Marsden PhD
Skin Analytics Limited
London, United Kingdom
MedicalResearch.com: What is the background for this study?
Response: In this technology age, with the explosion of interest and applications using Artificial Intelligence, it is easy to accept the output of a technology-based test - such as a smartphone app designed to identify skin cancer - without thinking too much about it. In reality, technology is only as good as the way it has been developed, tested and validated. In particular, AI algorithms are prone to a lack of “generalisation” - i.e. their performance drops when presented with data it has not seen before. In the medical field, and particularly in areas where AI is being developed to direct a patient’s diagnosis or care, this is particularly problematic. Inappropriate diagnosis or advice to patients can lead to false reassurance, heightened concern and pressure on NHS services, or worse. It is concerning, therefore, that there are a large number of smartphone apps available that provide an assessment of skin lesions, including some that provide an estimate of the probability of malignancy, that have not been assessed for diagnostic accuracy.
Skin Analytics has developed an AI-based algorithm, named: Deep Ensemble for Recognition of Malignancy (DERM), for use as a decision support tool for healthcare providers. DERM determines the likelihood of skin cancer from dermoscopic images of skin lesions. It was developed using deep learning techniques that identify and assess features of these lesions which are associated with melanoma, using over 7,000 archived dermoscopic images. Using these images, it was shown to identify melanoma with similar accuracy to specialist physicians. However, to prove the algorithm could be used in a real life clinical setting, Skin Analytics set out to conduct a clinical validation study.