Author Interviews, Dermatology, Technology / 19.09.2018
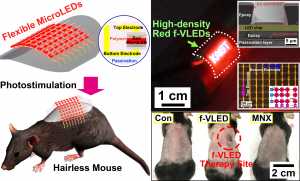
Experimental Cap Regrows Hair Using Photostimulation
MedicalResearch.com Interview with:
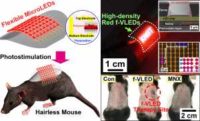 Han Eol Lee Ph.D.
Flexible and Nanobio Device Lab.
Department of Materials Science and Engineering
KAIST
MedicalResearch.com: What is the background for this study?
Response: Numerous people around the world have suffered from alopecia, which leads to aesthetic issues, low self-esteem, and social anxiety. With the population expansion alopecia patients from middle-age down even to the twenties, a depilation treatment is expected to have social and medical impacts on billions of patients. The causes of alopecia are generally known to be heredity, mental stress, aging, and elevated male hormone. Therapeutic techniques such as thermal, electrical, pharmacological, and optical stimulation have been proposed to treat hair problems. Among them, laser stimulation to hair-lost regions is a promising technique, activating the anagen phase and the proliferation of hair follicles without side effects. However, this laser stimulation technique has drawbacks, such as high power consumption, large size, and restrictive use in daily life (e.g., the difficulty of microscale spatial control and the long time exposure of high-energy laser).
Han Eol Lee Ph.D.
Flexible and Nanobio Device Lab.
Department of Materials Science and Engineering
KAIST
MedicalResearch.com: What is the background for this study?
Response: Numerous people around the world have suffered from alopecia, which leads to aesthetic issues, low self-esteem, and social anxiety. With the population expansion alopecia patients from middle-age down even to the twenties, a depilation treatment is expected to have social and medical impacts on billions of patients. The causes of alopecia are generally known to be heredity, mental stress, aging, and elevated male hormone. Therapeutic techniques such as thermal, electrical, pharmacological, and optical stimulation have been proposed to treat hair problems. Among them, laser stimulation to hair-lost regions is a promising technique, activating the anagen phase and the proliferation of hair follicles without side effects. However, this laser stimulation technique has drawbacks, such as high power consumption, large size, and restrictive use in daily life (e.g., the difficulty of microscale spatial control and the long time exposure of high-energy laser).
 Han Eol Lee Ph.D.
Flexible and Nanobio Device Lab.
Department of Materials Science and Engineering
KAIST
MedicalResearch.com: What is the background for this study?
Response: Numerous people around the world have suffered from alopecia, which leads to aesthetic issues, low self-esteem, and social anxiety. With the population expansion alopecia patients from middle-age down even to the twenties, a depilation treatment is expected to have social and medical impacts on billions of patients. The causes of alopecia are generally known to be heredity, mental stress, aging, and elevated male hormone. Therapeutic techniques such as thermal, electrical, pharmacological, and optical stimulation have been proposed to treat hair problems. Among them, laser stimulation to hair-lost regions is a promising technique, activating the anagen phase and the proliferation of hair follicles without side effects. However, this laser stimulation technique has drawbacks, such as high power consumption, large size, and restrictive use in daily life (e.g., the difficulty of microscale spatial control and the long time exposure of high-energy laser).
Han Eol Lee Ph.D.
Flexible and Nanobio Device Lab.
Department of Materials Science and Engineering
KAIST
MedicalResearch.com: What is the background for this study?
Response: Numerous people around the world have suffered from alopecia, which leads to aesthetic issues, low self-esteem, and social anxiety. With the population expansion alopecia patients from middle-age down even to the twenties, a depilation treatment is expected to have social and medical impacts on billions of patients. The causes of alopecia are generally known to be heredity, mental stress, aging, and elevated male hormone. Therapeutic techniques such as thermal, electrical, pharmacological, and optical stimulation have been proposed to treat hair problems. Among them, laser stimulation to hair-lost regions is a promising technique, activating the anagen phase and the proliferation of hair follicles without side effects. However, this laser stimulation technique has drawbacks, such as high power consumption, large size, and restrictive use in daily life (e.g., the difficulty of microscale spatial control and the long time exposure of high-energy laser).